Abstract
Introduction and hypothesis
The objective was to assess the safety and feasibility of using a pelvic floor dilator during active labor to prevent injuries to the levator ani muscle (LAM) and perineum.
Methods
In a prospective pilot study, a pelvic floor dilator using soft pads was introduced into the vaginal canal to gradually expand the vagina, in 30 nulliparous women and in 10 controls. The primary outcomes were adverse events related to the device. Secondary outcomes were perineal lacerations after delivery, sonographically defined levator ani injury, hiatal area dimensions, and anal sphincter disruption, all at 12–20 weeks postpartum, and maximum pelvic floor dilation, time to achieve maximum dilation, and device retention rate.
Results
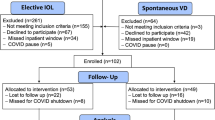
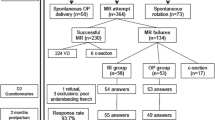
From October 2014 through November 2016, a total of 494 women were screened, and 61 consented to the study. Thirty women used the device and 27 returned for follow-up. No maternal or neonatal injuries were related to use of the dilator. The average maximum dilation of the vaginal canal was 7.4 cm (SD 0.7, range 5.5–8.0). Dilation time averaged 27 min (SD 13, range 5–60). Device insertion adjustment was needed in 13 out of 30 cases (43%). Similar rates of 3th–4th degree perineal lacerations were seen in both groups. Levator ani avulsion was diagnosed in 2 out of 27 (7%) in the device group and in 1 out of 9 (11%) in the control group (p = 0.2). The rate of partial injury in the device group was 2 out of 27 (7%) vs 2 out of 9 (22%) in the comparison group (p = 0.2).
Conclusion
The use of the pelvic floor dilator during active labor is feasible. No safety issues were identified.




Similar content being viewed by others
References
Gyhagen M, Bullarbo M, Nielsen TF, Milsom I. Prevalence and risk factors for pelvic organ prolapse 20 years after childbirth: a national cohort study in singleton primiparae after vaginal or caesarean delivery. BJOG. 2013;120(2):152–60. https://doi.org/10.1111/1471-0528.12020.
Goldberg J, Hyslop T, Tolosa JE, Sultana C. Racial differences in severe perineal lacerations after vaginal delivery. Am J Obstet Gynecol. 2003;188(4):1063–7.
Dietz HP. Pelvic floor trauma following vaginal delivery. Curr Opin Obstet Gynecol. 2006;18(5):528–37. https://doi.org/10.1097/01.gco.0000242956.40491.1e.
Handa VL, Blomquist JL, Knoepp LR, Hoskey KA, McDermott KC, Munoz A. Pelvic floor disorders 5–10 years after vaginal or cesarean childbirth. Obstet Gynecol. 2011;118(4):777–84. https://doi.org/10.1097/AOG.0b013e3182267f2f.
Nygaard I, Barber MD, Burgio KL, Kenton K, Meikle S, Schaffer J, et al. Prevalence of symptomatic pelvic floor disorders in US women. JAMA. 2008;300(11):1311–6. https://doi.org/10.1001/jama.300.11.1311.
Wu JM, Matthews CA, Conover MM, Pate V, Jonsson FM. Lifetime risk of stress urinary incontinence or pelvic organ prolapse surgery. Obstet Gynecol. 2014;123(6):1201–6. https://doi.org/10.1097/aog.0000000000000286.
Dudding TC, Vaizey CJ, Kamm MA. Obstetric anal sphincter injury: incidence, risk factors, and management. Ann Surg. 2008;247(2):224–37. https://doi.org/10.1097/SLA.0b013e318142cdf4.
Riskin-Mashiah S, O'Brian Smith E, Wilkins IA. Risk factors for severe perineal tear: can we do better? Am J Perinatol. 2002;19(5):225–34. https://doi.org/10.1055/s-2002-33088.
LaCross A, Groff M, Smaldone A. Obstetric anal sphincter injury and anal incontinence following vaginal birth: a systematic review and meta-analysis. J Midwifery Womens Health. 2015;60(1):37–47. https://doi.org/10.1111/jmwh.12283.
DeLancey JO, Kearney R, Chou Q, Speights S, Binno S. The appearance of levator ani muscle abnormalities in magnetic resonance images after vaginal delivery. Obstet Gynecol. 2003;101(1):46–53.
Dietz HP, Lanzarone V. Levator trauma after vaginal delivery. Obstet Gynecol. 2005;106(4):707–12. https://doi.org/10.1097/01.aog.0000178779.62181.01.
Schwertner-Tiepelmann N, Thakar R, Sultan AH, Tunn R. Obstetric levator ani muscle injuries: current status. Ultrasound Obstet Gynecol. 2012;39(4):372–83. https://doi.org/10.1002/uog.11080.
Lien KC, Mooney B, DeLancey JO, Ashton-Miller JA. Levator ani muscle stretch induced by simulated vaginal birth. Obstet Gynecol. 2004;103(1):31–40. https://doi.org/10.1097/01.aog.0000109207.22354.65.
Ashton-Miller JA, Delancey JO. On the biomechanics of vaginal birth and common sequelae. Annu Rev Biomed Eng. 2009;11:163–76. https://doi.org/10.1146/annurev-bioeng-061008-124823.
Svabik K, Shek KL, Dietz HP. How much does the levator hiatus have to stretch during childbirth? BJOG. 2009;116(12):1657–62. https://doi.org/10.1111/j.1471-0528.2009.02321.x.
Kamisan Atan I, Shek KL, Langer S, Guzman Rojas R, Caudwell-Hall J, Daly JO, et al. Does the Epi-No® birth trainer prevent vaginal birth-related pelvic floor trauma? A multicentre prospective randomised controlled trial. BJOG. 2016;123(6):995–1003. https://doi.org/10.1111/1471-0528.13924.
Beckmann MM, Stock OM. Antenatal perineal massage for reducing perineal trauma. Cochrane Database Syst Rev 2013;(4):CD005123. https://doi.org/10.1002/14651858.CD005123.pub3.
Aasheim V, Nilsen AB, Lukasse M, Reinar LM. Perineal techniques during the second stage of labour for reducing perineal trauma. Cochrane Database Syst Rev 2011;(12):CD006672. https://doi.org/10.1002/14651858.CD006672.pub2.
Bazi T, Takahashi S, Ismail S, Bo K, Ruiz-Zapata AM, Duckett J, et al. Prevention of pelvic floor disorders: International Urogynecological Association research and development committee opinion. Int Urogynecol J. 2016;27(12):1785–95. https://doi.org/10.1007/s00192-016-2993-9.
Practice Bulletin No. 165: Prevention and management of obstetric lacerations at vaginal delivery. Obstet Gynecol. 2016;128(1):e1–15. https://doi.org/10.1097/aog.0000000000001523.
Dietz HP, Shek KL. Tomographic ultrasound imaging of the pelvic floor: which levels matter most? Ultrasound Obstet Gynecol. 2009;33(6):698–703. https://doi.org/10.1002/uog.6403.
Dietz HP, Haylen BT, Broome J. Ultrasound in the quantification of female pelvic organ prolapse. Ultrasound Obstet Gynecol. 2001;18(5):511–4. https://doi.org/10.1046/j.0960-7692.2001.00494.x.
Guzman Rojas RA, Kamisan Atan I, Shek KL, Dietz HP. Anal sphincter trauma and anal incontinence in urogynecological patients. Ultrasound Obstet Gynecol. 2015;46(3):363–6. https://doi.org/10.1002/uog.14845.
Kearney R, Miller JM, Ashton-Miller JA, DeLancey JO. Obstetric factors associated with levator ani muscle injury after vaginal birth. Obstet Gynecol. 2006;107(1):144–9. https://doi.org/10.1097/01.AOG.0000194063.63206.1c.
Caudwell-Hall J, Kamisan Atan I, Martin A, Guzman Rojas R, Langer S, Shek K, et al. Intrapartum predictors of maternal levator ani injury. Acta Obstet Gynecol Scand. 2017;96(4):426–31. https://doi.org/10.1111/aogs.13103.
Funding
Materna Medical Inc., Mountain View, CA, USA (salaries and supplies).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
FJ Orejuela and SM Ramin received salary support from Materna Medical Inc.
HP Dietz receives unrestricted educational grant support from GE.
None of the other authors has any conflicts of interest to disclose.
Additional information
Clinical trial registration
ClinicalTrials.gov, NCT02332759
Electronic supplementary material
ESM 1
(MOV 110808 kb)
Rights and permissions
About this article
Cite this article
Orejuela, F.J., Gandhi, R., Mack, L. et al. Prospective evaluation of the safety and feasibility of a pelvic floor dilator during active labor. Int Urogynecol J 29, 1485–1492 (2018). https://doi.org/10.1007/s00192-018-3555-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-018-3555-0