Abstract
Introduction and hypothesis
There is a difference of opinion in the literature as to whether pelvic organ prolapse (POP) is a direct cause of female sexual dysfunction (FSD). Sexual function in women is negatively impacted by the presence of urinary symptoms. Thus, sexual dysfunction (SD) might be improved, unchanged, or worsened by pelvic floor surgery.
Methods
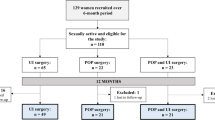
In this study, we observed SD and impact of surgical intervention on female sexual function (FSF) using a validated Prolapse/Urinary Incontinence Sexual Questionnaire Short Form (PISQ-12) in women undergoing surgery for POP with or without urinary incontinence. Two hundred women were recruited and followed up at 6 and 12 months postoperatively.
Results
Sexual function (SF) as measured by the PISQ-12 improved after surgery irrespective of the nature of surgery or the patient’s past gynaecology history. Improvement in SF was seen by 6 months (97 patients) postsurgery (P < 0.05), after which (at 12 months; 80 patients) no further change was observed. Improved SF was associated with better patient satisfaction postoperatively.
Conclusions
Sexual function improved in women following surgery for POP with or withour urinary incontinence, irrespective of the nature of surgery and the patient’s past gynecologic history. Results of this study will assist when counselling women with POP with or without urinary incontinence regarding treatment options.

Similar content being viewed by others
References
Laumann EO, Paik A, Rosen RC. Sexual dysfunction in the United States: prevalence and predictors. JAMA. 1999;281:537–44. https://doi.org/10.1001/jama.281.6.537.
Raina R, Pahlajani G, Khan S, Gupta S, Agarwal A, Zippe CD. Female sexual dysfunction: classification,pathophysiology, and management. Fertil Steril. 2007;88(5).
Swift SE. Distribution of pelvic organ support in a population of female subjects seen for routine gynaecological health care. Am J Obstet Gynecol. 2000;183(2):277–85.
Swift S, Woodman P, O'Boyle A, Kahn M, Valley M, Bland D, et al. Pelvic organ support study (POSST): the distribution, clinical definition, and epidemiologic condition of pelvic organ support defects. Am J Obstet Gynecol. 2005;192(3):795–806.
Jolleys JV. Reported prevalence of urinary incontinence in women in a general practice. Br Med J (Clin Res Ed). 1988;296(6632):1300–2.
Fialkow MF, Newton KM, Lentz GM, Weiss NS. Lifetime risk of surgical management for pelvic organ prolapse or urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19(3):437–40.
Barber MD, Visco AG, Wyman JF, Fantl JA, Bump RC, Continence Program for Women Research Group. Sexual function in women with urinary incontinence and pelvic organ prolapse. Obstet Gynecol. 2002;99(2):281–9.
Pauls RN, Silva WA, Rooney CM, Siddighi S, Kleeman SD, Dryfhout V, et al. Sexual function after vaginal surgery for pelvic organ prolapse and urinary incontinence. Am J Obstet Gynecol. 2007;197(6):622.e1–7.
Salonia A, Zanni G, Nappi RE, Briganti A, Dehò F, Fabbri F, et al. Sexual dysfunction is common in women with lower urinary tract symptoms and urinary incontinence: results of a cross-sectional study. Eur Urol. 2004;45(5):642–8. discussion 648
Rogers RG, Kammerer-Doak D, Villarreal A, et al. A new instrument to measure sexual function in women with urinary incontinence or pelvic organ prolapse. Am J Obstet Gynecol. 2001;184:552.
Handa VL, Cundiff G, Chang HH, Helzlsouer KJ. Female sexual function and pelvic floor disorders. Obstet Gynecol. 2008;111(5):1045–52. https://doi.org/10.1097/AOG.0b013e31816bbe85.
Nappi R, Salonia A, Traish AM, van Lunsen RH, Vardi Y, Kodiglu A, et al. Clinical biologic pathophysiologies of women's sexual dysfunction. J Sex Med. 2005;2(1):4–25.
Althof SE, Dean J, Derogatis LR, Rosen RC, Sisson M. Current perspectives on the clinical assessment and diagnosis of female sexual dysfunction and clinical studies of potential therapies: a statement of concern. J Sex Med. 2005;48:642–9.
Su TH, Lau HH, Huang WC, Chen SS, Lin TY, Hsieh CH, et al. Short term impact on female sexual function of pelvic floor reconstruction with the Prolift procedure. J Sex Med. 2009;6(11):3201–7. https://doi.org/10.1111/j.1743-6109.2009.01399.x.
Rogers RG, Kammerer-Doak D, Darrow A, Murray K, Qualls C, Olsen A, et al. Does sexual function change after surgery for stress urinary incontinence and/or pelvic organ prolapse? A multicenter prospective study. Am J Obstet Gynecol. 2006;195(5):e1–4.
Thakar R, Chawla S, Scheer I, et al. Sexual function following pelvic floor surgery. Int J Gynaecol Obstet. 2008;102:110.
Srikrishna S, Robinson D, Cardozo L, Gonzalez J. Can sex survive pelvic floor surgery? Int Urogynecol J. 2010;21(11):1313–9. https://doi.org/10.1007/s00192-010-1198-x.
Occhino JA, Trabuco EC, Heisler CA, Klingele CJ, Gebhart JB. Changes in vaginal anatomy and sexual function after vaginal surgery. Int Urogynecol J. 2011;22(7):799–804. https://doi.org/10.1007/s00192-011-1386-3.
Helström L, Nilsson B. Impact of vaginal surgery on sexuality and quality of life in women with urinary incontinence or genital descensus. Acta Obstet Gynecol Scand. 2005;84(1):79–84.
Hasse P, Skidstead L. Influence of operations for stress incontinence and/or genital descensus on sexual life. Acta Obstet Gynecol Scand. 1988;67(7):659–61.
Lemack GE, Zimmern PE. Sexual function after vaginal surgery for stress incontinence: results of a mailed questionnaire. Urology. 2000;56:223.
Neill C, Abdel-Fattah M, Ramsay IN. Sexual function and vaginal surgery. Obstet Gynaecol. 2009;11:193–8. https://doi.org/10.1576/toag.11.3.193.27504.
Roos AM, Thakar R, Sultan AH, de Leeuw JW, Paulus AT. The impact of pelvic floor surgery on female sexual function: a mixed quantitative and qualitative study. BJOG. 2014;121(1):92–100. https://doi.org/10.1111/1471-0528.12412.
Weber AM, Walters MD, Schover LR, Mitchinson A. Sexual function in women with uterovaginal prolapse and urinary incontinence. Obstet Gynecol. 1995;85:483.
Brubaker L, Chiang S, Zyczynski H, Norton P, Kalinoski DL, Stoddard A, et al. The impact of stress incontinence surgery on female sexual function. Am J Obstet Gynecol. 2009;200(5):562.e1–7. https://doi.org/10.1016/j.ajog.2008.11.017.
Glavind K. Sexual function in women before and after surgery for pelvic organ prolapse. AOGS. 2015;94:80–5.
Lindquist AS, Glavind K. Long-term follow-up of sexual function in women before and after tension-free vaginal tape operation for stress urinary incontinence. IUJ. 2016;27(10):1571–6. https://doi.org/10.1007/s00192-016-3004-x.
Sloan J, Symonds T, Vargas-Chanes D, Fridley B. Practical guidelines for assessing the clinical significance of health-related quality of life changes within clinical trials. Drug Inf J. 2003;37(1):23–31.
Tok EC, Yasa O, Ertunc D, Savas A, Durukan H, Kanik A. The effect of pelvic organ prolapse on sexual function in a general cohort of women. J Sex Med. 2010;7(12):3957–62. https://doi.org/10.1111/j.1743-6109.2010.01940.x.
Lowenstein L, Gamble T, Sanses TV, et al. Changes in sexual function after treatment for prolapse are related to the improvement in body image perception. J Sex Med. 2010;7:1023.
Funding
Project was funded by the Department of Urogynaecology, South Glasgow University Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Appendix 1
Appendix 1

Rights and permissions
About this article
Cite this article
Tyagi, V., Perera, M., Guerrero, K. et al. Prospective observational study of the impact of vaginal surgery (pelvic organ prolapse with or without urinary incontinence) on female sexual function. Int Urogynecol J 29, 837–845 (2018). https://doi.org/10.1007/s00192-017-3500-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-017-3500-7