Abstract
Introduction
Pelvic Organ Prolapse Quantification (POP-Q) system, measured in centimetres using a ruler (e.g. POPstix®), is recommended to quantify prolapse severity. POPstix® are costly (US $1/ruler). Home-made devices are used instead, but these have not been shown to be reproducible.
Hypothesis
Digitally assessed POP-Q (DPOP-Q) is as reliable, reproducible and acceptable as POP-Q assessed using POPstix®.
Methods
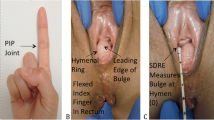
In this randomised crossover diagnostic agreement trial, each assessor measured the index finger of their dominant hand using a ruler. At visit one, patients were randomised to either POPstix® POP-Q assessment in a modified lithotomy position or DPOP-Q in both modified a lithotomy and a standing position. After the first clinician conducted this assessment, a second blinded clinician then carried out the remaining assessment on the same patient. For each examination, duration was recorded, along with a patient-completed discomfort score. Twenty-five women were invited for visit two, at which DPOP-Q was recorded by the same clinician who undertook DPOP-Q at the first visit. This allowed evaluation of inter- and intraobserver agreement together with examination acceptability.
Results
One hundred and nine women were recruited [median age 55 years, parity 2, body mass index (BMI) 27.1]. Of the 25 patients invited, 23 returned for visit two. DPOP-Q had high interobserver reliability [κ = 0.94, 95 % confidence interval (CI) 0.878–0.996] and intraobserver reliability (α = 0.96) with POPstix®. DPOP-Q was significantly quicker (p = 0.02) and less uncomfortable (p < 0.01) than POPstix® POP-Q.
Conclusion
DPOP-Q is reliable, acceptable and cost effective.




Similar content being viewed by others
References
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89(4):501–506
Porges RF (1963) A practical system of diagnosis and classification of pelvic relaxations. Surg Gynecol Obstet 117:769–773
Baden WF, Walker TA (1972) Genesis of the vaginal profile: a correlated classification of vaginal relaxation. Clin Obstet Gynecol 15(4):1048–1054
Bump RC, Mattiasson A, Bø K, Brubaker LP, DeLancey JO, Klarskov P, Shull BL, Smith AR (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175(1):10–17
Auwad W, Freeman RM, Swift S (2004) Is the pelvic organ prolapse quantification system (POPQ) being used? A survey of members of the International Continence Society (ICS) and the American Urogynecologic Society (AUGS). Int Urogynecol J Pelvic Floor Dysfunct 15(5):324–327
Treszezamsky AD, Rascoff L, Shahryarinejad A et al (2010) Use of pelvic organ prolapse staging systems in published articles of selected specialized journals. Int Urogynecol J Pelvic Floor Dysfunct 21(3):359–363
Treszezamsky AD, Filmar G, Panagopoulos G, Vardy MD, Ascher-Walsh CJ (2012) Teaching of pelvic organ prolapse quantification system among obstetrics/gynecology and urology residents in the United States. Female Pelvic Med Reconstr Surg 18(1):37–40
Hayward L, Wong V, Tomlinson L, Smalldridge J (2009) A prospective interobserver study using the POPstix device, a measuring tool to simplify POPQ measurement. ICS 2009 San Francisco Abstract
Cheng WC, Ng FC et al (2004) Interobserver variation of prostatic volume estimation with digital rectal examination by urological staffs with different experiences. Int Braz J Urol 30(6):466–471
Reis LO, Simao AFL et al (2013) Digital rectal examination standardization for inexperienced hands: teaching medical students. Adv Urol 2013:797096
Silva WA, Kleeman S, Segal J et al (2004) Effects of a full bladder and patient positioning on pelvic organ prolapse assessment. Obstet Gynecol 104(1):37–41
Julious SA (2005) Sample size of 12 per group rule of thumb for a pilot study. Pharm Stat 4:287–291
Lloyd J, Crouch NS, Minto CL, Liao LM, Creighton SM (2005) Female genital appearance: “normality” unfolds. BJOG 112(5):643–646
Conflict of interest
G Thiagamoorthy has received funding from Astellas and Johnson & Johnson to attend conferences; also received an IUGA FRN grant to set up a multicentre research project. M Zacchè has received funding from Astellas to attend conferences. L Cardozo received funding for research, lecturing and/or advice/consultancies from Allergan, Astellas & Pfizer. M Naidu has received funding from Astellas to attend conferences. I Giarenis has received funding from Astellas and Johnson & Johnson to attend conferences. R Flint has no conflicts. S Srikrishna has received funding for lecturing and/or advice/consultancies from Astellas. D Robinson has received funding for research, lecturing and/or advice/consultancies from Allergan, Astellas, Ferring & Pfizer.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thiagamoorthy, G., Zacchè, M., Cardozo, L. et al. Digital assessment and quantification of pelvic organ prolapse (DPOP-Q): a randomised cross-over diagnostic agreement trial. Int Urogynecol J 27, 433–437 (2016). https://doi.org/10.1007/s00192-015-2841-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-015-2841-3