Abstract
Introduction and hypothesis
The aim of this study was to evaluate pelvic floor dysfunction and anatomical signs of pelvic organ prolapse (POP) in patients with levator ani muscle (LAM) trauma compared with patients with an intact LAM 1 year postpartum.
Methods
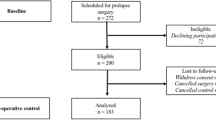
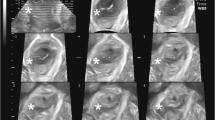
In a prospective case–control study, primiparous women after vaginal delivery, with LAM trauma diagnosed on 3D ultrasound, were included in the case group. Controls consisted of patients who fulfilled the same inclusion criteria but had an intact levator. All women were investigated 1 year postpartum in respect of bladder, bowel, prolapse, and sexual function using the Australian Pelvic Floor Questionnaire. POP was assessed according to the Pelvic Organ Prolapse Quantification (POP-Q) system and pelvic floor muscle strength using the Oxford Grading Scale.
Results
Forty patients were included: 20 with and 20 without levator trauma. Urinary symptoms were significantly more frequent in women with LAM trauma compared with controls (p = 0.01). The two groups were comparable in respect of bowel, sexual, and prolapse symptoms (p = 0.24, p = 0.60, p = 0.99 respectively). Unlike POP stages II and III, POP stage I was significantly more common in LAM trauma patients (n = 19, 95 %) than in controls (n = 10, 50 %) (p =0.003). A positive association was noted between POP stage I and LAM trauma (RR = 7.2). The involvement of multiple compartments was significantly more frequent in cases than in controls (p = 0.003).
Conclusions
Except for urinary symptoms, LAM trauma was asymptomatic in nearly all patients 1 year postpartum. However, POP stage I involving multiple compartments occurred more frequently in LAM trauma patients than in controls.


Similar content being viewed by others
Abbreviations
- LAM:
-
Levator ani muscle
- POP:
-
Pelvic organ prolapse
- POP-Q:
-
Pelvic organ prolapse quantification
- TUI:
-
Tomographic ultrasound imaging
References
Sultan AH et al (1993) Anal-sphincter disruption during vaginal delivery. N Engl J Med 329(26):1905–1911
Sultan AH, Monga AK (1997) Anal and urinary incontinence in women with obstetric anal sphincter rupture. Br J Obstet Gynaecol 104(6):754–755
Scheer I et al (2008) Urinary incontinence after obstetric anal sphincter injuries (OASIS)—is there a relationship? Int Urogynecol J Pelvic Floor Dysfunct 19(2):179–183
Dietz HP, Lanzarone V (2005) Levator trauma after vaginal delivery. Obstet Gynecol 106(4):707–712
Kearney R et al (2006) Obstetric factors associated with levator ani muscle injury after vaginal birth. Obstet Gynecol 107(1):144–149
Valsky DV et al (2009) Fetal head circumference and length of second stage of labor are risk factors for levator ani muscle injury, diagnosed by 3-dimensional transperineal ultrasound in primiparous women. Am J Obstet Gynecol 201(1):91.e1–7
Delancey JO, Hurd WW (1998) Size of the urogenital hiatus in the levator ani muscles in normal women and women with pelvic organ prolapse. Obstet Gynecol 91(3):364–368
Dietz HP, Simpson JM (2008) Levator trauma is associated with pelvic organ prolapse. BJOG 115(8):979–884
Chen L et al (2006) Interaction among apical support, levator ani impairment, and anterior vaginal wall prolapse. Obstet Gynecol 108(2):324–332
Rostaminia G et al (2013) Levator ani deficiency and pelvic organ prolapse severity. Obstet Gynecol 121(5):1017–1024
Dietz HP (2010) Pelvic floor ultrasound: a review. Am J Obstet Gynecol 202(4):321–334
Dietz HP, Shek C, Clarke B (2005) Biometry of the pubovisceral muscle and levator hiatus by three-dimensional pelvic floor ultrasound. Ultrasound Obstet Gynecol 25(6):580–585
Dietz HP, Shek KL (2009) Tomographic ultrasound imaging of the pelvic floor: which levels matter most? Ultrasound Obstet Gynecol 33(6):698–703
Dietz HP, Abbu A, Shek KL (2008) The levator-urethra gap measurement: a more objective means of determining levator avulsion? Ultrasound Obstet Gynecol 32(7):941–945
Baessler K et al (2009) Australian pelvic floor questionnaire: a validated interviewer-administered pelvic floor questionnaire for routine clinic and research. Int Urogynecol J Pelvic Floor Dysfunct 20(2):149–158
Baessler K (2009) Validierung eines umfassenden Beckenboden-Fragebogens für Klinik, Praxis und Forschung. Gynakol Geburtshilfliche Rundsch 49:299–307
Bump RC et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175(1):10–17
Haylen BT et al (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J 21(1):5–26
Orno AK, Dietz HP (2007) Levator co-activation is a significant confounder of pelvic organ descent on Valsalva maneuver. Ultrasound Obstet Gynecol 30(3):346–350
Laycock J (1994) Clinical evaluation of the pelvic floor. In: Schussler B, Laycock J, Norton P, Stanton SL (eds) Pelvic floor reeducation, principles, and practice. Springer, London, pp 39–51
Von Elm E et al (2007) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 370(9596):1453–1457
Albrich SB et al (2012) Impact of mode of delivery on levator morphology: a prospective observational study with three-dimensional ultrasound early in the postpartum period. BJOG 119(1):51–60
Guzman Rojas R et al (2014) Impact of levator trauma on pelvic floor muscle function. Int Urogynecol J 25(3):375–380
Shek KL, Dietz HP (2009) The effect of childbirth on hiatal dimensions. Obstet Gynecol 113(6):1272–1278
Morgan DM et al (2010) Levator ani defect status and lower urinary tract symptoms in women with pelvic organ prolapse. Int Urogynecol J 21(1):47–52
Dietz HP et al (2009) Does avulsion of the puborectalis muscle affect bladder function? Int Urogynecol J Pelvic Floor Dysfunct 20(8):967–972
Heilbrun ME et al (2010) Correlation between levator ani muscle injuries on magnetic resonance imaging and fecal incontinence, pelvic organ prolapse, and urinary incontinence in primiparous women. Am J Obstet Gynecol 202(5):488.e1–6
Tumbarello JA et al (2010) Do repetitive Valsalva maneuvers change maximum prolapse on dynamic MRI? Int Urogynecol J 21(10):1247–1251
Orejuela FJ, Shek KL, Dietz HP (2012) The time factor in the assessment of prolapse and levator ballooning. Int Urogynecol J 23(2):175–178
Conflict of interest
None related to this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Laterza, R.M., Schrutka, L., Umek, W. et al. Pelvic floor dysfunction after levator trauma 1-year postpartum: a prospective case–control study. Int Urogynecol J 26, 41–47 (2015). https://doi.org/10.1007/s00192-014-2456-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-014-2456-0