Abstract
Introduction and hypothesis
Obstetric anal sphincter injury (OASIS) following birth may have serious, long-term effects on affected women, including fecal incontinence, despite primary repair.
Methods
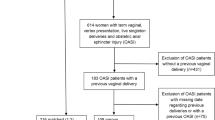
This was a retrospective population-based register study. Women with OASIS grouped by order of vaginal delivery and prior cesarean section (CS) were compared separately with women without OASIS using logistic regression analysis. The aim was to assess an association between prior CS and incidence of OASIS across groups of women categorized according to singleton first, second, and third vaginal deliveries between 1997 and 2007 in Finland.
Results
The incidence of OASIS was 1.8 % at a first vaginal delivery after a prior CS compared with 1.0 % at a first vaginal delivery without prior CS. After adjustment prior CS was associated with a 1.42-fold risk of OASIS only at the first vaginal delivery, with no further significant risk after one or two previous vaginal deliveries. One centimeter increase in maternal height was associated with a 2 % decrease in OASIS incidence at the first vaginal delivery.
Conclusions
Prior CS is a significant risk factor for OASIS at the first vaginal delivery. This suggests that relative fetopelvic disproportion leading to CS for a first delivery also predisposes to OASIS at a first vaginal delivery since 40 % of the increased incidence of OASIS risk was explained by birthweight and 4 % by maternal height.
Similar content being viewed by others
References
Dudding TC, Vaizey CJ, Kamm MA (2008) Obstetric anal sphincter injury: incidence, risk factors, and management. Ann Surg 247:224–237
EURO-PERISTAT project (2008) European Perinatal Health Report. Available via http://www.europeristat.com/. Accessed 10 Aug 2012
Handa VL, Danielsen BH, Gilbert WM (2001) Obstetric anal sphincter lacerations. Obstet Gynecol 98:225–230
Frankman EA, Wang L, Bunker CH, Lowder JL (2009) Episiotomy in the United States: has anything changed? Am J Obstet Gynecol 200:573.e1–573.e7
Laine K, Gissler M, Pirhonen J (2009) Changing incidence of anal sphincter tears in four Nordic countries through the last decades. Eur J Obstet Gynecol Reprod Biol 146:71–75
Andrews V, Sultan AH, Thakar R, Jones PW (2006) Occult anal sphincter injuries–myth or reality? BJOG 113:195–200
Baghestan E, Irgens LM, Bordahl PE, Rasmussen S (2010) Trends in risk factors for obstetric anal sphincter injuries in Norway. Obstet Gynecol 116:25–34
Räisänen SH, Vehviläinen-Julkunen K, Gissler M, Heinonen S (2009) Lateral episiotomy protects primiparous but not multiparous women from obstetric anal sphincter rupture. Acta Obstet Gynecol Scand 88:1365–1372
Revicky V, Nirmal D, Mukhopadhyay S, Morris EP, Nieto JJ (2010) Could a mediolateral episiotomy prevent obstetric anal sphincter injury? Eur J Obstet Gynecol Reprod Biol 150:142–146
de Leeuw JW, Struijk PC, Vierhout ME, Wallenburg HC (2001) Risk factors for third degree perineal ruptures during delivery. BJOG 108:383–387
Fitzgerald MP, Weber AM, Howden N, Cundiff GW, Brown MB et al (2007) Risk factors for anal sphincter tear during vaginal delivery. Obstet Gynecol 109:29–34
Dandolu V, Chatwani A, Harmanli O, Floro C, Gaughan JP, Hernandez E (2005) Risk factors for obstetrical anal sphincter lacerations. Int Urogynecol J Pelvic Floor Dysfunct 16:304–307
de Leeuw JW, de Wit C, Kuijken JP, Bruinse HW (2008) Mediolateral episiotomy reduces the risk for anal sphincter injury during operative vaginal delivery. BJOG 115:104–108
Kalis V, Laine K, de Leeuw J, Ismail K, Tincello D (2012) Classification of episiotomy: towards a standardisation of terminology. BJOG 119:522–526
Lowder JL, Burrows LJ, Krohn, Weber AM (2007) Risk factors for primary and subsequent anal sphincter lacerations: a comparison of cohorts by parity and prior mode of delivery. Am J Obstet Gynecol 196:344–345
Richter HE, Brumfield CG, Cliver SP, Burgio KL, Neely CL, Varner RE (2002) Risk factors associated with anal sphincter tear: a comparison of primiparous patients, vaginal births after cesarean deliveries, and patients with previous vaginal delivery. Am J Obstet Gynecol 187:1194–1198
Belsley DA, Kuh E, Welsch RE (1980) Regression diagnostics: identifying influential data and sources of collinearity. Wiley, New York
Van de Mheen H, Stronks K, Van den Bos J, Mackenbach JP (1997) The contribution of childhood environment to the explanation of socio-economic inequalities in health in adult life: a retrospective study. Soc Sci Med 44:13–24
Sultan A (1999) Obstetric perineal injury and anal incontinence. Clin Risk 5:193–196
Gissler M, Teperi J, Hemminki E, Meriläinen J (1995) Data quality after restructuring a national medical registry. Scand J Soc Med 23:75–80
Martin JA, Hamilton BE, Ventura SJ, Osterman MJ, Kirmeyer S, Mathews TJ et al (2011) Births: final data for 2009. Natl Vital Stat Rep 60:1–70
Rozenholc AT, Ako SN, Leke RJ, Boulvain M (2007) The diagnostic accuracy of external pelvimetry and maternal height to predict dystocia in nulliparous women: a study in Cameroon. BJOG 114:630–635
van Roosmalen J, Brand R (1992) Maternal height and the outcome of labor in rural Tanzania. Int J Gynaecol Obstet 37:169–177
Liselele HB, Boulvain M, Tshibangu KC, Meuris S (2000) Maternal height and external pelvimetry to predict cephalopelvic disproportion in nulliparous African women: a cohort study. BJOG 107:947–952
Merchant KM, Villar J, Kestler E (2001) Maternal height and newborn size relative to risk of intrapartum caesarean delivery and perinatal distress. BJOG 108:689–696
Benjamin SJ, Daniel AB, Kamath A, Ramkumar V (2012) Anthropometric measurements as predictors of cephalopelvic disproportion: can the diagnostic accuracy be improved? Acta Obstet Gynecol Scand 91:122–127
Maharaj D (2010) Assessing cephalopelvic disproportion: back to the basics. Obstet Gynecol Surv 65:387–395
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Räisänen, S., Vehviläinen-Julkunen, K., Cartwright, R. et al. A prior cesarean section and incidence of obstetric anal sphincter injury. Int Urogynecol J 24, 1331–1339 (2013). https://doi.org/10.1007/s00192-012-2006-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-2006-6