Abstract
Introduction and hypothesis
The aim of the study was to describe effectiveness and safety of percutaneous tibial nerve stimulation (PTNS) at 2 years in women with overactive bladder (OAB) syndrome unresponsive to pharmacotherapy.
Methods
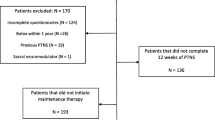
Of 30 women who had initial positive response to PTNS, 23 continued to receive maintenance treatment and were reassessed at 2 years using bladder symptom diaries and the Incontinence Impact Questionnaire (IIQ-7). They were also questioned on acceptability and any adverse effects of long-term peripheral neuromodulative treatment.
Results
Data from 23 women were available and 7 had been lost to follow-up. With maintenance treatment, the median nocturnal frequency at 2 years had decreased by 57 % (3.5 to 1.5 times/night), while the median IIQ-7 had reduced from 30.4 to 21.5 (both p < 0.01) compared to pre-treatment baseline. Median nocturnal frequency and IIQ-7 scores at 2 years were comparable to those documented after initial response to treatment at 6 weeks, suggesting that maintenance therapy continued to suppress OAB symptoms. Daytime frequency and daily urgency incontinence episodes at 2 years were statistically similar to those documented at 6 weeks and remained lower than pre-treatment baseline (6.5 vs 11.8 and 2.0 vs 3.5, respectively, p < 0.05). The women received a median of 8.42 treatments per year and the median length between treatments was 64.3 days. Apart from hypaesthesia in the toe of one responder lasting for 4 months, there were no reported side effects.
Conclusions
Women receiving PTNS for intractable OAB syndrome reported significant symptom relief at 2 years. This remains a safe mode of second-line treatment with excellent durability.


Similar content being viewed by others
References
McGuire E, Zhang S, Horwinski E, Lytton B (1983) Treatment of motor and sensory detrusor instability by electrical stimulation. J Urol 129(1):78–79
van Balken MR, Vandoninck V, Gisolf KW et al (2001) Posterior tibial nerve stimulation as neuromodulative treatment of lower urinary tract dysfunction. J Urol 166:914–918
Vandoninck V, van Balken MR, Finazzi Agró E et al (2003) Posterior tibial nerve stimulation in the treatment of urge incontinence. Neurourol Urodyn 22:17–23
Yoong W, Ridout AE, Damodaram M, Dadswell R (2010) Neuromodulative treatment with percutaneous tibial nerve stimulation for intractable detrusor instability: outcomes following a shortened 6-week protocol. BJU Int 106(11):1673–1676
Peters KM, Macdiarmid SA, Wooldridge LS et al (2009) Randomised trial of percutaneous tibial nerve stimulation versus extended-release tolterodine: results from the overactive bladder innovative therapy trial. J Urol 182(3):1055–1061
National Institute for Health and Clinical Excellence (2010) Percutaneous posterior tibial nerve stimulation for overactive bladder syndrome. NICE interventional procedure guidance 362
MacDiarmid SA, Peters KM, Shobeiri SA et al (2010) Long-term durability of percutaneous tibial nerve stimulation for the treatment of overactive bladder. J Urol 183(1):234–240
Capitanucci ML, Camanni D, Demelas F et al (2009) Long-term efficacy of percutaneous tibial nerve stimulation for different types of lower urinary tract dysfunction in children. J Urol 182(4 Suppl):2056–2061
Govier FE, Litwiller S, Nitti V, Kreder KJ Jr, Rosenblatt P (2001) Percutaneous afferent neuromodulation for the refractory overactive bladder: results of a multicenter study. J Urol 165:1193–1198
Stoller M (1999) Afferent nerve stimulation for pelvic floor dysfunction. Eur Urol 35(Suppl 2):16
Schäfer W, Abrams P, Liao L et al (2002) Good urodynamic practices: uroflowmetry, filling cystometry, and pressure-flow studies. Neurourol Urodyn 21:261–274
Haylen BT, de Ridder D, Freeman RM, Swift SE et al (2010) An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J 21(1):5–26
Klingler HC, Pycha A, Schmidbauer J, Marberger M (2000) Use of peripheral neuromodulation of the S3 region for treatment of detrusor overactivity: a urodynamic-based study. Urology 56(5):766–771
Karademir K, Baykal K, Sen B, Senkul T, Iseri C, Erden D (2005) A peripheric neuromodulation technique for curing detrusor overactivity: Stoller afferent neurostimulation. Scand J Urol Nephrol 39:230–233
van der Pal F, van Balken MR, Heesakkers JPFA, Debruyne FMJ, Bemelmans BLH (2006) Percutaneous tibial nerve stimulation in the treatment of refractory overactive bladder syndrome: is maintenance treatment necessary? BJU Int 97:547–590
Wooldridge LS (2009) Percutaneous tibial nerve stimulation for the treatment of urinary frequency, urinary urgency, and urge incontinence: results from a community-based clinic. Urol Nurs 29(3):177–185
Padmanabhan P, Scarpero HM, Milam DF, Dmochowski RR, Penson DF (2011) Five-year cost analysis of intra-detrusor botulinum toxin type A and augmentation cystoplasty for refractory neurogenic detrusor overactivity. World J Urol 29(1):51–57
Robinson D, Jacklin P, Cardozo L (2010) What’s needling us about the management of refractory overactive bladder? An economic analysis of the use of percutaneous nerve stimulation and botulinum toxin. Neurourol Urodyn 29(6):805–1255
Govaert B, Pares D, Delgado-Aros S, La Torre F, van Gemert WG, Baeten CG (2010) A prospective multicenter study to investigate percutaneous tibial nerve stimulation for the treatment of faecal incontinence. Colorectal Dis 12(12):1236–1241
Acknowledgements
We would like to thank Dr. Alexandra Ridout and Mr. Derek Graham for helping with data collection.
Conflicts of interest
None.
Ethics approval
None required as observational data and this has been discussed with Hospital Ethics Committee.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yoong, W., Shah, P., Dadswell, R. et al. Sustained effectiveness of percutaneous tibial nerve stimulation for overactive bladder syndrome: 2-year follow-up of positive responders. Int Urogynecol J 24, 795–799 (2013). https://doi.org/10.1007/s00192-012-1936-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1936-3