Abstract
Introduction and hypothesis
Overactive bladder (OAB) is a symptom-based condition consisting of urgency, with or without incontinence, usually with frequency and nocturia. There are many potential causes of OAB, yet many patients are prescribed anticholinergic medications empirically. This study aimed to determine what proportion of patients presenting for urogynecologic assessment with symptoms of OAB had urodynamic detrusor overactivity (DO).
Methods
Retrospective chart review was performed for 220 consecutive patient referrals. Demographic data, physical exam information, and urodynamic results were collected. The t test and Fisher’s exact test were used for statistical analyses.
Results
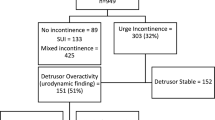
The prevalence of DO was 11.8 % in this population. Urogenital atrophy and incomplete emptying were more common. Patients with DO were older and more often menopausal than those without DO. Significant prolapse was a common finding amongst patients with OAB symptoms.
Conclusions
Patients with symptoms of OAB should undergo pelvic examination and assessment of post-void residuals before being initiated on anticholinergic medication.

Similar content being viewed by others
References
Abrams P, Cardozo L, Fall M et al (2002) The standardisation of terminology of lower urinary tract function: report from the Standarisation Sub-committee of the International Continence Society. Neurourol Urodyn 21(2):167–178
Irwin D, Milsom I, Hunskaar S et al (2006) Population-based survey of urinary incontinence, overactive bladder, and other lower urinary tract symptoms in five countries: results of the EPIC study. Eur Urol 50:1306–1315
Milsom I, Abrams P, Cardozo L, Roberts RG, Thüroff J, Wein AJ (2001) How widespread are the symptoms of an overactive bladder and how are they managed? A population-based prevalence study. BJU Int 87:760–766
Stewart WF, Van Rooyen JB, Cundiff GW et al (2003) Prevalence and burden of overactive bladder in the United States. World J Urol 20:327–336
Wan H, Sengupta M, Velkoff VA, DeBarros KA (2005) 65+ in the United States. U.S. Census Bureau, Current Population Reports. U.S. Government Printing Office, Washington, DC, pp 23-209
Irwin DE, Mungapen L, Milsom I et al (2009) The economic impact of overactive bladder syndrome in six Western countries. BJU Int 103:202–209
Resnick NM, Yalla SV, Laurino E (1989) The pathophysiology of urinary incontinence among institutionalized elderly persons. N Engl J Med 320(1):1–7
Drutz HP (2011) Overactive bladder: the importance of tailoring treatment to the individual patient. J Multidiscip Healthc 4:233–237
Ashok K, Wang A (2010) Detrusor overactivity: an overview. Arch Gynecol Obstet 282:33–41
Digesu GA, Khuller V, Cardozo L, Salvatore S (2003) Overactive bladder symptoms: do we need urodynamics? Neurourol Urodyn 22:105–108
de Boer TA, Salvatore S, Cardozo L et al (2010) Pelvic organ prolapse and overactive bladder. Neurourol Urodyn 29(1):30–39
Johnston SL, Farrell SA, Bouchard C et al (2004) The detection and management of vaginal atrophy. J Obstet Gynaecol Can 26(5):503–508
Hextall A, Cardozo L (2001) The role of estrogen supplementation in lower urinary tract dysfunction. Int Urogynecol J Pelvic Floor Dysfunct 12:258–261
Calleja-Agius J, Brincat MP (2009) Urogenital atrophy. Climacteric 12:279–285
Cody JD, Richardson K, Moehrer B, Hextall A, Glazener CMA. (2009) Oestrogen therapy for urinary incontinence in post-menopausal women. Cochrane Database Syst Rev 4:CD001405. doi:10.1002/14651858.CD001405.pub2
Kupelian V, Rosen RC, Link CL et al (2009) Association of urological symptoms and chronic illness in men and women: contributions of symptom severity and duration–results from the BACH Survey. J Urol 181:694–700
Acknowledgments
The Department of Obstetrics and Gynecology, Mount Sinai Hospital and University Health Network, Toronto provided funding.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Diamond, P., Hassonah, S., Alarab, M. et al. The prevalence of detrusor overactivity amongst patients with symptoms of overactive bladder: a retrospective cohort study. Int Urogynecol J 23, 1577–1580 (2012). https://doi.org/10.1007/s00192-012-1781-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-012-1781-4