Abstract
Introduction and hypothesis
The objective of this paper is to study the reproducibility and anatomical risks of anterior sacrospinous ligament (SSL) fixation associated with paravaginal repair using the Pinnacle™ device (Boston Scientific™).
Methods
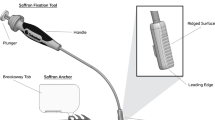
Simplified bilateral anterior SSL fixation associated with paravaginal fixation through the arcus tendineus fascia pelvis (ATFP) was performed on five fresh cadavers using the Pinnacle™ device. Cadaver dissection was then performed by open pelvic surgery.
Results
Eight SSL and ten ATFP were available for analysis. SSL fixations were optimal in four cases, too superficial in three cases, and too high in one case. Mean distance between SSL fixation and ischial spine was 18.6 mm (range 10 to 30 mm). Mean distance between SSL fixation and pudendal nerve was 6.5 mm (range 0 to 15 mm). ATFP fixations were optimal in five cases, good in four cases, and too superficial in one case. In one case (10%), the middle arm of the prosthesis was in contact with the ureter and traction on that arm resulted in ureteral kinking.
Conclusions
Anterior SSL fixation associated with paravaginal repair using the Pinnacle™ device was not reproducible every time in this cadaver study. These results confirm the need for specific training before starting anterior SSL fixations.


Similar content being viewed by others
References
Lousquy R, Costa P, Delmas V, Haab F (2009) Update on the epidemiology of genital prolapse. Prog Urol 19:907–915
Misraï V, Rouprêt M, Seringe E, Vaessen C, Cour F, Haertig A et al (2008) Long-term results of laparoscopic sacral colpopexy for high-grade cystoceles. Prog Urol 18:1068–1074
Richter K (1968) The surgical anatomy of the vaginaefixatio sacrospinalis vaginalis. A contribution to the surgical treatment of vaginal blind pouch prolapse. Geburtshilfe Frauenheilkd 28:321–327
Richardson D, Scotti R, Ostergard D (1989) Surgical management of uterine prolapse in young women. J Reprod Med 34:388–392
Estrade J, Agostini A, Roger V, Dallay D, Blanc B, Cravello L (2005) Posthysterectomy prolapse: results of sacrospinous ligament fixation. J Gynecol Obstet Biol Reprod (Paris) 34:481–487
Beer M, Kuhn A (2005) Surgical techniques for vault prolapse: a review of the literature. Eur J Obstet Gynecol Reprod Biol 119:144–155
Amarenco G, Lanoe Y, Perrigot M, Goudal H (1987) A new canal syndrome: compression of the pudendal nerve in Alcock’s canal or perinal paralysis of cyclists. Presse Med 16:399
Barksdale P, Gasser R, Gauthier C, Elkins T, Wall L (1997) Intraligamentous nerves as a potential source of pain after sacrospinous ligament fixation of the vaginal apex. Int Urogynecol J Pelvic Floor Dysfunct 8:121–125
Winkler H, Tomeszko J, Sand P (2000) Anterior sacrospinous vaginal vault suspension for prolapse. Obstet Gynecol 95:612–615
Goldberg R, Tomezsko J, Winkler H, Koduri S, Culligan P, Sand P (2001) Anterior or posterior sacrospinous vaginal vault suspension: long-term anatomic and functional evaluation. Obstet Gynecol 98:199–204
Ouzaid I, Ben Rhouma S, de Tayrac R, Costa P, Prudhomme M, Delmas V (2010) Mini-invasive posterior sacrospinous ligament fixation using the CAPIO needle driver: an anatomical study. Prog Urol 20:515–519
Meschia M, Bruschi F, Amicarelli F, Pifarotti P, Marchini M, Crosignani P (1999) The sacrospinous vaginal vault suspension: critical analysis of outcomes. Int Urogynecol J Pelvic Floor Dysfunct 10:155–159
Sagsoz N, Ersoy M, Kamaci M, Tekdemir I (2002) Anatomical landmarks regarding sacrospinous colpopexy operations performed for vaginal vault prolapse. Eur J Obstet Gynecol Reprod Biol 101:74–78
Roshanravan S, Wieslander C, Schaffer J, Corton M (2007) Neurovascular anatomy of the sacrospinous ligament region in female cadavers: implications in sacrospinous ligament fixation. Am J Obstet Gynecol 197:660.e1–6
de Tayrac R, Boileau L, Fara J, Monneins F, Raini C, Costa P (2010) Bilateral anterior sacrospinous ligament suspension associated with a paravaginal repair with mesh: short-term clinical results of a pilot study. Int Urogynecol J Pelvic Floor Dysfunct 21:293–298
Bader G (2009) The obturator foramen: the intersection of all the dangers? Gynecol Obstet Fertil 37:687–688
Touboul C, Nizard J, Fauconnier A, Bader G (2008) Major venous hemorrhagic complication during transvaginal cystocele repair using the transobturator approach. Obstet Gynecol 111:492–495
Latthe P, Foon R, Toozs-Hobson P (2007) Transobturator and retropubic tape procedures in stress urinary incontinence: a systematic review and meta-analysis of effectiveness and complications. BJOG 114:522–531
Hazewinkel M, Hinoul P, Roovers J (2009) Persistent groin pain following a trans-obturator sling procedure for stress urinary incontinence: a diagnostic and therapeutic challenge. Int Urogynecol J Pelvic Floor Dysfunct 20:363–365
Conflicts of interest
This study was supported by Boston Scientific, and R. de T., P.C., and V.D. are consultants for Boston Scientific.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cayrac, M., Letouzey, V., Ouzaid, I. et al. Anterior sacrospinous ligament fixation associated with paravaginal repair using the Pinnacle™ device: an anatomical study. Int Urogynecol J 23, 335–340 (2012). https://doi.org/10.1007/s00192-011-1554-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-011-1554-5