Abstract
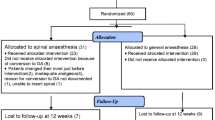
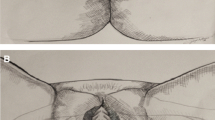
In this study of the surgical repair of pelvic organ prolapse (POP), the vaginal pelvic floor repair with mesh (PFR-Mesh) procedure was used. The procedure is originally named TVM. All 55 patients in the series were operated upon under sedation and local anaesthesia as pain relief. The objectives were twofold. Firstly, the objective was to evaluate peri-operative and immediate post-operative complications. Secondly, the objective was to evaluate the feasibility of performing these relatively complex procedures under sedation and local anaesthesia. The visual analogue scale (VAS) was used to record pain during and after the operations. At a follow-up visit 8–12 weeks post-operatively, a self-instructed questionnaire evaluating subjective opinions of the operation itself and the post-operative period was handed in. Of the 55 patients, anterior, posterior and total PFR-Mesh procedures were performed in 39 (71%), 12 (22%) and 4 (7%) patients, respectively. Mean age was 68 years (52–93). All patients could be operated as scheduled under sedation and local anaesthesia. Mean operative time was 38 min (26–70). Peri-operative complications consisted of two cases of bladder perforation with the superior needle in an anterior repair and vaginal perforation with the inferior needle also in an anterior repair. At the conclusion of the operation VAS was recorded to be 0–3 in 65% of the patients. There were no immediate post-operative complications. Out of 55 patients, 35 (64%) left the ward on the day of operation whilst the remaining 20 (36%) patients stayed for only one night. The safety of the PFR-Mesh procedure and the feasibility of performing these procedures under sedation and local anaesthesia were demonstrated. However, expertise in vaginal surgery is required.

Similar content being viewed by others
References
Brubaker L (2005) Controversies and uncertainties: abdominal versus vaginal surgery for pelvic organ prolapse. Am J Obstet Gynecol 192:690–693
Benson JT, Lucente V, McClellan E (1996) Vaginal versus abdominal reconstructive surgery for the treatment of pelvic support defects: a prospective randomized study with long-term outcome evaluation. Am J Obstet Gynecol 175:1418–1422
Maher CF, Qatawneh AM, Dwyer PL, Carey MP, Cornish A, Schluter PJ (2004) Abdominal sacral colpopexy or vaginal sacrospinous colpopexy for vaginal vault prolapse: a prospective randomized trial. Am J Obstet Gynecol 190:20–26
Mølsted-Pedersen L, Rudnicki M, Lose G (2006) Transvaginal repair of enterocele and vaginal vault prolapse using autologous fascia lata graft. Acta Obstet Gynecol Scand 85:874–878
Milani R, Salvatore S, Soligo M, Pifarotti P, Meschia M, Cortese M (2004) Functional and anatomic outcome of anterior and posterior vaginal prolapse repair with prolene mesh. Br J Obstet Gynaecol 111:1–5
Miklos JR, Sze EH, Karram MM (1995) Vaginal correction of pelvic organ relaxation using local anesthesia. Obstet Gynecol 86:922–924
Jomaa M (2001) Combined tension-free vaginal tape and prolapse repair under local anesthesia in patients with symptoms of both urinary incontinence and prolapse. Gynecol Obstet Invest 51:184–186
Moore RD, Miklos JR (2003) Colpocleisis and tension-free vaginal tape sling for severe uterine and vaginal prolapse and stress urinary incontinence under local anesthesia. J Am Assoc Gynecol Laparosc 11:276–280
Axelson SM, Bek KM (2004) Anterior vaginal wall repair using local anesthesia. Eur J Obstet Gynecol 112:214–216
Buchsbaum GM, Duecy EE (2005) Local anesthesia with sedation for transvaginal correction of advanced genital prolapse. Am J Obstet Gynecol 193:2173–2176
Berrocal J, Clavé H, Cosson M, Debodinance PH, Garbin O, Jacquetin B, Rosenthal C, Salet-Lizée D, Villet R (2004) Conceptual advances in the surgical management of genital prolapse. J Gynecol Obstet Biol Reprod 33:577–587
Shull BL, Bachofen C, Coates KW, Kuehl TJ (2000) A transvaginal approach to repair of apical and other associated sites of pelvic organ prolapse using uterosacral ligaments. Am J Obstet Gynecol 183:1365–1374
LaSala AC, Schimpf OM (2007) Occurrence of postoperative hematomas after prolapse repair using a mesh augmentation system. Obstet Gynecol 109:569–572
Acknowledgement
Fifty percent of the cost of the PFR-Mesh system was financed by Johnson & Johnson Medical.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Flam, F. Sedation and local anaesthesia for vaginal pelvic floor repair of genital prolapse using mesh. Int Urogynecol J 18, 1471–1475 (2007). https://doi.org/10.1007/s00192-007-0350-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-007-0350-8