Abstract
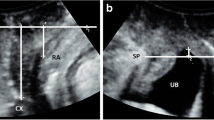
The aim of the present study was to compare clinical and radiological findings when assessing posterior vaginal wall prolapse. Defecography can be used to complement the clinical evaluation in patients with posterior vaginal wall prolapse. Further development of the defecography technique, using contrast medium in the urinary bladder and intraperitoneally, have resulted in cystodefecoperitoneography (CDP). Thirty-eight women underwent clinical examination using the pelvic organ prolapse quantification system (POP-Q) followed by CDP. All patients answered a standardized bowel function questionnaire. Statistical analysis measuring correlation between POP-Q and CDP using Pearson’s correlation coefficient (r) and Spearman’s rank order correlation coefficient (rs) demonstrated a poor to moderate correlation, r=0.49 and rs=0.55. Although there was a strong association between large rectoceles (>3 cm) at CDP and symptoms of rectal emptying difficulties (p<0.001), severity and prevalence of bowel dysfunction showed poor coherence with clinical prolapse staging and findings at radiological imaging. Vaginal topography and POP-Q staging predict neither radiological size nor visceral involvement in posterior vaginal wall prolapse. Radiological evaluation may therefore be a useful complement in selected patients.






Similar content being viewed by others
References
Weber A, Abrams P, Brubaker L et al (2001) The standardization of terminology for researchers in female pelvic floor disorders. Int Urogynecol J 12:178–186
Hall AF, Theofrastous JP, Cundiff GW et al (1996) Interobserver and intraobserver reliability of the proposed International Continence Society, Society of Gynecologic Surgeons, and American Urogynecologic Society pelvic organ prolapse classification system. Am J Obstet Gynecol 175:1467–1470
Bump RC, Mattiasson A, Bo K et al (1996) The standardization of terminology of female pelvic organ prolapse and pelvic floor dysfunction. Am J Obstet Gynecol 175:10–17
Kelvin FM, Hale DS, Maglinte DD, Patten BJ, Benson JT (1999) Female pelvic organ prolapse: diagnostic contribution of dynamic cystoproctography and comparison with physical examination. Am J Roentgenol 173:31–37
Lopéz A, Anzén B, Bremmer S et al (2002) Cystodefecoperitoneography in patients with genital prolapse. Int Urogynecol J 13:22–29
Kelvin FM, Maglinte DD, Hornback JA, Benson JT (1992) Pelvic prolapse: assessment with evacuation proctography (defecography). Radiology 184:547–551
Delemarre JB, Kruyt RH, Doornbos J et al (1994) Anterior rectocele: assessment with radiographic defecography, dynamic magnetic resonance imaging, and physical examination. Dis Colon Rectum 37:249–259
Wiersma TG, Mulder CJ, Reeders JW, Tytgat GN, Van Waes PF (1994) Dynamic rectal examination (defecography). Baillieres Clin Gastroenterol 8:729–741
Maglinte DD, Kelvin FM, Fitzgerald K, Hale DS, Benson JT (1999) Association of compartment defects in pelvic floor dysfunction. Am J Roentgenol 172:439–444
Bremmer S, Ahlback SO, Uden R, Mellgren A (1995) Simultaneous defecography and peritoneography in defecation disorders. Dis Colon Rectum 38:969–973
Kelvin FM, Maglinte DD, Benson JT (1994) Evacuation proctography (defecography): an aid to the investigation of pelvic floor disorders. Obstet Gynecol 83:307–314
Yoshioka K, Matsui Y, Yamada O et al (1991) Physiologic and anatomic assessment of patients with rectocele. Dis Colon Rectum 34:704–708
Bremmer S, Mellgren A, Holmstrom B, Lopez A, Uden R (1997) Peritoneocele: visualization with defecography and peritoneography performed simultaneously. Radiology 202:373–377
Colton T (1974) Statistics in medicine. Little Brown and Company, Boston
Kenton K, Shott S, Brubaker L (1997) Vaginal topography does not correlate well with visceral position in women with pelvic organ prolapse. Int Urogynecol J 8:336–339
Lienemann A, Anthuber C, Baron A, Kohz P, Reiser M (1997) Dynamic MR colpocystorectography assessing pelvic-floor descent. Eur Radiol 7:1309–1317
Lopez A, Anzén B, Bremmer S et al (2001) Durability of success after rectocele repair. Int Urogynecol J 12:97–103
Nichols DH (1991) Surgery for pelvic floor disorders. Surg Clin North Am 71:927–946
Barber MD, Lambers A, Visco AG, Bump RC (2000) Effect of patient position on clinical evaluation of pelvic organ prolapse. Obstet Gynecol 96:18–22
Mellgren A, Johansson C, Dolk A et al (1994) Enterocele demonstrated by defaecography is associated with other pelvic floor disorders. Int J Colorect Dis 9:121–124
Wiersma TG, Mulder CJ, Reeders JW (1997) Dynamic rectal examination: its significant clinical value. Endoscopy 29:462–471
Bremmer S, Mellgren A, Holmstrom B, Uden R (1998) Peritoneocele and enterocele. Formation and transformation during rectal evacuation as studied by means of defaeco-peritoneography. Acta Radiol 39:167–175
Goei R, Baeten C (1990) Rectal intussusception and rectal prolapse: detection and postoperative evaluation with defecography. Radiology 174:124–126
Karlbom U, Nilsson S, Pahlman L, Graf W (1999) Defecographic study of rectal evacuation in constipated patients and control subjects. Radiology 210:103–108
Mellgren A, Bremmer S, Johansson C et al (1994) Defecography. Results of investigations in 2,816 patients. Dis Colon Rectum 37:1133–1141
Mellgren A, Schultz I, Johansson C, Dolk A (1997) Internal rectal intussusception seldom developes into total rectal prolapse. Dis Colon Rectum 40:817–820
Goei R, van Engelshoven J, Schouten H, Baeten C, Stassen C (1989) Anorectal function: defecographic measurement in asymptomatic subjects. Radiology 173:137–141
Yoshioka K, Matsui Y, Yamada O et al (1991) Physiologic and anatomic assessment of patients with rectocele. Dis Colon Rectum 34:704–708
Author information
Authors and Affiliations
Corresponding author
Additional information
Presented in part at the 10th European Symposium on Urogenital Radiology, Uppsala, Sweden, 4–7 September 2003
Editorial Comment: This is an interesting study looking at a new radiographic technique for evaluating pelvic organ support defects. This technique is basically cystodefecography with the addition of an intraperitoneal contrast. The technique itself, while it currently cannot be recommended as standard care, certainly holds interesting possibilities particularly in the detection of complicated enteroceles and high sigmoidoceles. We wish that the authors will continue to look at this technique and determine its eventual role in the evaluation of pelvic organ support defects
Rights and permissions
About this article
Cite this article
Altman, D., López, A., Kierkegaard, J. et al. Assessment of posterior vaginal wall prolapse: comparison of physical findings to cystodefecoperitoneography. Int Urogynecol J 16, 96–103 (2005). https://doi.org/10.1007/s00192-004-1220-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-004-1220-2