Abstract
Purpose
To compare graft dimensions, functional outcomes, and failure rates following anterior cruciate ligament reconstruction (ACLR) with either five-strand or four-strand hamstring autograft options.
Methods
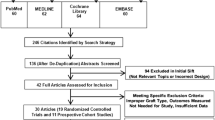
Three databases (MEDLINE, PubMed, and EMBASE) were searched from inception to 22 April 2023 for level I and II studies comparing five- and four-strand hamstring autografts in ACLR. The authors adhered to the PRISMA and R-AMSTAR guidelines as well as the Cochrane Handbook for Systematic Reviews of Interventions. Data on demographics, surgical details and rehabilitation, graft diameter, patient-reported outcome measures (PROMs), and rates of positive Lachman test, positive pivot shift test, and graft rupture were extracted. PROMs included Knee Osteoarthritis and Outcome Score (KOOS) subscales, Lysholm, and International Knee Documentation Committee (IKDC).
Results
One randomized controlled trial (RCT) and four prospective cohort studies with 572 patients were included. Graft diameters were larger in the five-strand group with a mean difference of 0.93 mm (95% CI 0.61 to 1.25, p < 0.001, I2 = 66%). The five-strand group reported statistically higher KOOS ADL subscale and Lysholm scores with a mean difference of 4.85 (95% CI 0.14 to 9.56, p = 0.04, I2 = 19%) and 3.01 (95% CI 0.48 to 5.53, p = 0.02, I2 = 0%), respectively. There were no differences in KOOS symptoms, pain, quality of life, or sports subscales, or IKDC scores. There were no differences in rates of positive Lachman test, positive pivot shift test, or graft rupture with pooled odds ratios of 0.62 (95% CI 0.13 to 2.91, n.s., I2 = 80%), 0.94 (95% CI 0.51 to 1.75, n.s., I2 = 31%), and 2.13 (95% CI 0.38 to 12.06, n.s., I2 = 0%), respectively.
Conclusions
Although five-stranded hamstring autografts had significantly larger graft diameters compared to four-stranded grafts with a mean difference of 0.93 mm, similar graft rupture rates and clinical laxity assessments were identified following ACLR. While some PROMs were statistically superior in the five-stranded hamstring groups, the threshold for the minimal clinical important difference was not reached indicating similar clinical outcomes overall.
Level of Evidence
Level II.







Similar content being viewed by others
Data availability
Data can be made available upon reasonable request at prushoth.vivekanantha@medportal.ca.
Abbreviations
- ACL:
-
Anterior cruciate ligament
- ACLR:
-
Reconstruction
- PRISMA:
-
Preferred reporting items for systematic reviews and meta-analyses
- R-AMSTAR:
-
Revised assessment of multiple systematic reviews
- MINORS:
-
Methodological index for non-randomized studies
- KOOS:
-
Knee osteoarthritis and outcome score
- QoL:
-
Quality of life
- ADL:
-
Activities of daily living
- IKDC:
-
International knee documentation committee
References
Adams BG, Nowak MJ, Egan AC, Donohue MA, Galvin JW, Arrington ED (2023) Autograft-only and allograft-augmented hamstring autograft have similar failure rates after anterior cruciate ligament reconstruction. Arthrosc Sports Med Rehabil 5(3):e725–e730
Attia AK, Nasef H, ElSweify KH, Adam MA, AbuShaaban F, Arun K (2020) Failure rates of 5-strand and 6-strand vs quadrupled hamstring autograft ACL reconstruction: a comparative study of 413 patients with a minimum 2-year follow-up. Orthop J Sports Med 8(8):2325967120946326
Bengtsson J, Möllborg J, Werner S (1996) A study for testing the sensitivity and reliability of the Lysholm knee scoring scale. Knee Surg Sports Traumatol Arthrosc 4(1):27–31
Brinkman JC, Tummala SV, Hassebrock JD, McQuivey KS, Makovicka JL, Economopoulos KJ (2023) Mid-term outcomes of the all-soft quadriceps tendon autograft are noninferior to hamstring autograft in primary anterior cruciate ligament reconstruction: comparison with minimum 5-year follow-up. Arthroscopy 39(4):1008–1013
Calvo R, Figueroa D, Figueroa F, Vaisman A, Schmidt-Hebbel A, Morales N, Izquierdo G (2017) Five-strand hamstring autograft versus quadruple hamstring autograft with graft diameters 8.0 millimeters or more in anterior cruciate ligament reconstruction: clinical outcomes with a minimum 2-year follow-up. Arthroscopy 33(5):1007–1013
Chang MJ, Choi YS, Shin JH, Yoon TH, Kim TW, Chang CB, Kang S-B (2022) Comparison of failure rates and functional outcomes between hamstring autografts and hybrid grafts in anterior cruciate ligament reconstruction: a systematic review and meta-analysis. Orthop Traumatol Surg Res. https://doi.org/10.1016/j.otsr.2022.103499
Choi N-H, Lee D-M, Victoroff BN (2023) Bone morphological characteristics as risk factors for anterior cruciate ligament injury: comparison between contact and noncontact injury. Orthop J Sports Med 11(6):23259671231179756
Crawford K, Briggs KK, Rodkey WG, Steadman JR (2007) Reliability, validity, and responsiveness of the IKDC score for meniscus injuries of the knee. Arthroscopy 23(8):839–844
Detsky AS, Naylor CD, O’Rourke K, McGeer AJ, L’Abbé KA (1992) Incorporating variations in the quality of individual randomized trials into meta-analysis. J Clin Epidemiol 45(3):255–265
Duerr R, Ormseth B, Adelstein J, Garrone A, DiBartola A, Kaeding C, Flanigan D, Siston R, Magnussen R (2023) Elevated posterior tibial slope is associated with anterior cruciate ligament reconstruction failures: a systematic review and meta-analysis. Arthroscopy. https://doi.org/10.1016/j.arthro.2022.12.034
Foissey C, Thaunat M, Caron E, Haidar I, Vieira TD, Gomes L, Freychet B, Sonnery-Cottet B, Fayard J-M (2022) Combining anterior cruciate ligament reconstruction with lateral extra-articular procedures in skeletally immature patients is safe and associated with a low failure rate. Arthrosc Sports Med Rehabil 4(6):e1941–e1951
Hasoon J, Al-Dadah O (2023) Knee anatomic geometry accurately predicts risk of anterior cruciate ligament rupture. Acta Radiol 64(5):1904–1911
Higgins JPT, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21(11):1539–1558
Hopper GP, Pioger C, Philippe C, El Helou A, Campos JP, Gousopoulos L, Carrozzo A, Vieira TD, Sonnery-Cottet B (2022) Risk factors for anterior cruciate ligament graft failure in professional athletes: an analysis of 342 patients with a mean follow-up of 100 months from the SANTI Study Group. Am J Sports Med 50(12):3218–3227
Horvath A, Meredith SJ, Nishida K, Hoshino Y, Musahl V (2020) Objectifying the Pivot Shift Test. Sports Med Arthrosc Rev 28(2):36–40
Ignozzi AJ, Moran TE, Werner BC (2023) No difference could be detected in clinical outcomes of 5-strand and quadruple hamstring autografts of similar diameter in anterior cruciate ligament reconstruction: a retrospective cohort study. HSS J 19(1):62–68
Itoh M, Itou J, Okazaki K, Iwasaki K (2023) Estimation failure risk by 0.5-mm differences in autologous hamstring graft diameter in anterior cruciate ligament reconstruction: a meta-analysis. Am J Sports Med. https://doi.org/10.1177/03635465221150654
Kremen TJ, Arnold MT, Trivellas M, Shi BY, Jones KJ, Garcia-Mansilla I (2022) Combined assessments of patellar tendon and hamstring tendon parameters on preoperative magnetic resonance imaging can improve predictability of hamstring tendon autograft diameter in the setting of anterior cruciate ligament reconstruction. Arthrosc Sports Med Rehabil 4(6):e1913–e1921
Krishna L, Chan CX, Lokaiah L, Chinnasamy D, Goyal S, Wang M, Singh A (2021) Five-strand versus four-strand hamstring autografts in anterior cruciate ligament reconstruction—a prospective randomized controlled study. Arthroscopy 37(2):579–585
Krishna L, Tan XY, Wong FKL, Toh SJ (2018) A 5-strand hamstring autograft achieves outcomes comparable to those of a 4-strand hamstring autograft with a graft diameter of 8 mm or more in anterior cruciate ligament reconstruction. Orthop J Sports Med 6(3):2325967118760815
Kung J, Chiappelli F, Cajulis OO, Avezova R, Kossan G, Chew L, Maida CA (2010) From systematic reviews to clinical recommendations for evidence-based health care: validation of revised assessment of multiple systematic reviews (R-AMSTAR) for grading of clinical relevance. Open Dent J 4:84–91
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700
Lodhia P, Nazari G, Bryant D, Getgood A, McCormack R, STABILITY Group, Getgood AMJ, Bryant DM, Litchfield R, Willits K, Birmingham T, Hewison C, Firth AD, Wanlin S, Pinto R, Martindale A, O’Neill L, Jennings M, Daniluk M, McCormack RG, Boyer D, Zomar M, Moon K, Moon R, Fan B, Mohan B, Payne K, Heard M, Buchko GM, Hiemstra LA, Kerslake S, Tynedal J, MacDonald PB, Stranges G, Mcrae S, Gullett L, Brown H, Legary A, Longo A, Christian M, Ferguson C, Rezansoff A, Mohtadi N, Barber R, Chan D, Campbell C, Garven A, Pulsifer K, Mayer M, Peterson D, Simunovic N, Duong A, Robinson D, Levy D, Skelly M, Shanmugaraj A, Bardana D, Howells F, Tough M, Spalding T, Thompson P, Metcalfe A, Asplin L, Dube A, Clarkson L, Brown J, Bolsover A, Bradshaw C, Belgrove L, Milan F, Turner S, Verdugo S, Lowe J, Dunne D, McGowan K, Suddens C-M, Verdonk PCM, Declerq G, Vuylsteke K, Van Haver M (2022) Performance of 5-strand hamstring autograft anterior cruciate ligament reconstruction in the STABILITY study: a subgroup analysis. Am J Sports Med 50(13):3502–3509
Mariscalco MW, Flanigan DC, Mitchell J, Pedroza AD, Jones MH, Andrish JT, Parker RD, Kaeding CC, Magnussen RA (2013) The influence of hamstring autograft size on patient-reported outcomes and risk of revision after anterior cruciate ligament reconstruction: a Multicenter Orthopaedic Outcomes Network (MOON) Cohort Study. Arthroscopy 29(12):1948–1953
McHugh ML (2012) Interrater reliability: the kappa statistic. Biochem Medica 22(3):276–282
Nagda SH, Altobelli GG, Bowdry KA, Brewster CE, Lombardo SJ (2010) Cost analysis of outpatient anterior cruciate ligament reconstruction: autograft versus allograft. Clin Orthop Relat Res 468(5):1418–1422
Parkinson B, Robb C, Thomas M, Thompson P, Spalding T (2017) Factors that predict failure in anatomic single-bundle anterior cruciate ligament reconstruction. Am J Sports Med 45(7):1529–1536
Paudel YR, Sommerfeldt M, Voaklander D (2023) Incidence and risk factors for revision and contralateral anterior cruciate ligament reconstruction: a population-based retrospective cohort study. Medicine (Baltimore) 102(20):e33669
Perkins CA, Busch MT, Christino MA, Willimon SC (2021) Saucerization and repair of discoid lateral menisci with peripheral rim instability: intermediate-term outcomes in children and adolescents. J Pediatr Orthop 41(1):23–27
Pomenta Bastidas MV, Sastre S, Segur Vilalta JM, Rios J, Sabater M, Popescu D (2022) Quadriceps tendon vs hamstring autograft in primary ACL reconstruction—a comparative study with minimum two-year follow-up. Acta Orthop Belg 88(2):347–354
Pradhan P, Kaushal SG, Kocher MS, Kiapour AM (2023) Development of anatomic risk factors for ACL injuries: a comparison between ACL-injured knees and matched controls. Am J Sports Med. https://doi.org/10.1177/03635465231177465
Ro D-H, Lee S, Cho Y, Lee Y-M, Lee M-C, Kim SH (2020) Factors that predicts the size of autologous hamstring tendon graft for double-bundle ACL reconstruction. Indian J Orthop 54(4):444–453
Sadoghi P, Röggla V, Beiglböck H, Schett B, Reschl M, Fischerauer S, Reinbacher P, Widhalm HK (2022) Prediction of individual graft for anterior cruciate ligament reconstruction using anthropometric data. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-022-04682-0
Sanborn RM, Badger GJ, Fleming BC, Kiapour AM, BEAR Trial Team, Fadale PD, Hulstyn MJ, Owens BD, Proffen B, Sant N, Portilla G, Freiberger C, Henderson R, Barnett S, Costa M, Chrostek C, Ecklund K, Micheli LJ, Murray MM, Yen Y-M, Kramer DE (2023) Preoperative risk factors for subsequent ipsilateral ACL revision surgery after an ACL restoration procedure. Am J Sports Med 51(1):49–57
Sideris A, Hamze A, Bertollo N, Broe D, Walsh W (2018) Knee kinematics in anatomic anterior cruciate ligament reconstruction with four- and five-strand hamstring tendon autografts. Orthop Rev 10(3):7738
Singhal D, Kanodia N, Singh R, Singh S, Agrawal S (2021) Predicting quadruple semitendinosus graft size for anterior cruciate ligament reconstruction by patient anthropometric variables: a cohort study of 280 cases. Malays Orthop J 15(3):71–77
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73(9):712–716
Spragg L, Chen J, Mirzayan R, Love R, Maletis G (2016) The effect of autologous hamstring graft diameter on the likelihood for revision of anterior cruciate ligament reconstruction. Am J Sports Med 44(6):1475–1481
Vivekanantha P, Diao D, Cohen D, Murphy B, de Sa D (2023) Strength-based rehabilitation on clinical outcomes in patients post-partial meniscectomy: a systematic review and meta-analysis. Am J Phys Med Rehabil. https://doi.org/10.1097/PHM.0000000000002198
Vivekanantha P, Kahlon H, Cohen D, de Sa D (2022) Isolated medial patellofemoral ligament reconstruction results in similar postoperative outcomes as medial patellofemoral ligament reconstruction and tibial-tubercle osteotomy: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-022-07186-x
Wan KH-M, Lai CY-S, Tang SP-K, Ng EP-L, Moy RL-T, Chan W-L, Lee RH-L, Wong KK-H (2022) The use of five-strand hamstring autograft to increase the graft size in anterior cruciate ligament reconstruction—a prospective cohort study with satisfactory early clinical results. Arthrosc Sports Med Rehabil 4(6):e1923–e1931
Wroble RR, Lindenfeld TN (1988) The stabilized Lachman test. Clin Orthop Relat Res 237:209–212
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There are no relevant conflicts of interest.
Ethical approval
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Vivekanantha, P., Nedaie, S., Grzela, P. et al. Though five-strand hamstring autografts demonstrate greater graft diameter, postoperative outcomes are equivocal to four-strand hamstring autograft preparations: a systematic review and meta-analysis of level I and II studies. Knee Surg Sports Traumatol Arthrosc 31, 4437–4447 (2023). https://doi.org/10.1007/s00167-023-07515-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-023-07515-8