Abstract
Purpose
Identifying predictive factors for all-cause reoperation after anterior cruciate ligament reconstruction could inform clinical decision making and improve risk mitigation. The primary purposes of this study are to (1) determine the incidence of all-cause reoperation after anterior cruciate ligament reconstruction, (2) identify predictors of reoperation after anterior cruciate ligament reconstruction using machine learning methodology, and (3) compare the predictive capacity of the machine learning methods to that of traditional logistic regression.
Methods
A longitudinal geographical database was utilized to identify patients with a diagnosis of new anterior cruciate ligament injury. Eight machine learning models were appraised on their ability to predict all-cause reoperation after anterior cruciate ligament reconstruction. Model performance was evaluated via area under the receiver operating characteristics curve. To explore modeling interpretability and radiomic feature influence on the predictions, we utilized a game-theory-based method through SHapley Additive exPlanations.
Results
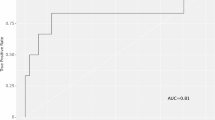
A total of 1400 patients underwent anterior cruciate ligament reconstruction with a mean postoperative follow-up of 9 years. Two-hundred and eighteen (16%) patients experienced a reoperation after anterior cruciate ligament reconstruction, of which 6% of these were revision ACL reconstruction. SHapley Additive exPlanations plots identified the following risk factors as predictive for all-cause reoperation: diagnosis of systemic inflammatory disease, distal tear location, concomitant medial collateral ligament repair, higher visual analog scale pain score prior to surgery, hamstring autograft, tibial fixation via radial expansion device, younger age at initial injury, and concomitant meniscal repair. Pertinent negatives, when compared to previous studies, included sex and timing of surgery. XGBoost was the best-performing model (area under the receiver operating characteristics curve of 0.77) and outperformed logistic regression in this regard.
Conclusions
All-cause reoperation after anterior cruciate ligament reconstruction occurred at a rate of 16%. Machine learning models outperformed traditional statistics and identified diagnosis of systemic inflammatory disease, distal tear location, concomitant medial collateral ligament repair, higher visual analog scale pain score prior to surgery, hamstring autograft, tibial fixation via radial expansion device, younger age at initial injury, and concomitant meniscal repair as predictive risk factors for reoperation. Pertinent negatives, when compared to previous studies, included sex and timing of surgery. These models will allow surgeons to tabulate individualized risk for future reoperation for patients undergoing anterior cruciate ligament reconstruction.
Level of evidence
III.






Similar content being viewed by others
Data availability
The data pertinent to this study is stored on the statistical analysis software, REDcap, and may be made available upon reasonable request.
References
Allahabadi S, Mittal A, Coughlan MJ, Kim AE, Hung NJ, Pandya NK (2022) Outcomes, including graft tears, contralateral anterior cruciate ligament tears, and all-cause ipsilateral knee operations, are similar for adult-type, transphyseal, and partial transphyseal anterior cruciate ligament reconstruction using hamstring autograft in pediatric and adolescent patients. Arthrosc Sports Med Rehabil 4:e1465–e1474
Bayliss L, Jones LD (2019) The role of artificial intelligence and machine learning in predicting orthopaedic outcomes. Bone Joint J 101-b:1476–1478
Bowyer K, Chawla N, Hall L, Kegelmeyer WP (2002) SMOTE: synthetic minority oversampling technique. J Artif Intell Res 16:321–357
Collins GS, Reitsma JB, Altman DG, Moons KG (2015) Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. BMJ 350:g7594
Compagnoni R, Gualtierotti R, Randelli P (2018) Total joint arthroplasty in patients with inflammatory rheumatic diseases. Adv Ther 35:1133–1139
Csintalan RP, Inacio MC, Funahashi TT, Maletis GB (2014) Risk factors of subsequent operations after primary anterior cruciate ligament reconstruction. Am J Sports Med 42:619–625
Gramfort A, Michel V, Pedregosa F, Thirion B, Varoquaux G (2011) Scikit-learn: machine learning in Python. J Mach Learn Res 12:2825–2830
Haeberle HS, Helm JM, Navarro SM, Karnuta JM, Schaffer JL, Callaghan JJ et al (2019) Artificial intelligence and machine learning in lower extremity arthroplasty: a review. J Arthroplasty 34:2201–2203
Herzog MM, Marshall SW, Lund JL, Pate V, Mack CD, Spang JT (2018) Trends in incidence of ACL reconstruction and concomitant procedures among commercially insured individuals in the United States, 2002–2014. Sports Health 10:523–531
Hughes JD, Hughes JL, Bartley JH, Hamilton WP, Brennan KL (2017) Infection rates in arthroscopic versus open rotator cuff repair. Orthop J Sports Med 5:2325967117715416
Huque MH, Carlin JB, Simpson JA, Lee KJ (2018) A comparison of multiple imputation methods for missing data in longitudinal studies. BMC Med Res Methodol 18:168
Janssen RPA, van Melick N, van Mourik JBA, Reijman M, van Rhijn LW (2018) ACL reconstruction with hamstring tendon autograft and accelerated brace-free rehabilitation: a systematic review of clinical outcomes. BMJ Open Sport Exerc Med 4:e000301
Jordan MI, Mitchell TM (2015) Machine learning: trends, perspectives, and prospects. Science 349:255–260
Kaeding CC, Pedroza AD, Reinke EK, Huston LJ, Moon Consortium, Spindler KP (2015) Risk factors and predictors of subsequent ACL injury in either knee after ACL reconstruction: prospective analysis of 2488 primary ACL reconstructions from the MOON cohort. Am J Sports Med 43:1583–1590
Ko S, Pareek A, Ro D, Lu Y, Camp C, Martin RK et al (2022) Artificial intelligence in orthopedics: three strategies for deep learning with orthopedic specific imaging. Knee Surg Sports Traumatol Arthrosc 30:758–761
Kunze KN, Polce EM, Clapp I, Nwachukwu BU, Chahla J, Nho SJ (2021) Machine learning algorithms predict functional improvement after hip arthroscopy for femoroacetabular impingement syndrome in athletes. J Bone Joint Surg Am 103:1055–1062
Kunze KN, Polce EM, Ranawat AS, Randsborg P-H, Williams RJ, Allen AA et al (2021) Application of machine learning algorithms to predict clinically meaningful improvement after arthroscopic anterior cruciate ligament reconstruction. Orthop J Sports Med 9:23259671211046576
Lemme NJ, Yang DS, Barrow B, O’Donnell R, Daniels AH, Cruz AI (2021) Risk factors for failure after anterior cruciate ligament reconstruction in a pediatric population: a prediction algorithm. Orthop J Sports Med 9:2325967121991165
Lian Q, Lian Y, Li K, Yang Q, Li K, Zheng Y et al (2022) Complications of primary total hip arthroplasty among patients with rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis, and primary osteoarthritis. BMC Musculoskelet 23:924
Lord L, Cristiani R, Edman G, Forssblad M, Stålman A (2020) One sixth of primary anterior cruciate ligament reconstructions may undergo reoperation due to complications or new injuries within 2 years. Knee Surg Sports Traumatol Arthrosc 28:2478–2485
Lu Y, Forlenza E, Wilbur R, Lavoie-Gagne O, Fu M, Yanke A et al (2021) Machine-learning model successfully predicts patients at risk for prolonged postoperative opioid use following elective knee arthroscopy. Knee Surg Sports Traumatol Arthrosc 30:762–772
Lu Y, Pareek A, Wilbur RR, Leland DP, Krych AJ, Camp CL (2021) understanding anterior shoulder instability through machine learning: new models that predict recurrence, progression to surgery, and development of arthritis. Orthop J Sports Med 9:23259671211053330
Lundberg SM, Nair B, Vavilala MS, Horibe M, Eisses MJ, Adams T et al (2018) Explainable machine-learning predictions for the prevention of hypoxaemia during surgery. Nat Biomed Eng 2:749–760
Luo W, Phung D, Tran T, Gupta S, Rana S, Karmakar C et al (2016) Guidelines for developing and reporting machine learning predictive models in biomedical research: a multidisciplinary view. J Med Internet Res 18:e323
Lyman S, Koulouvaris P, Sherman S, Do H, Mandl LA, Marx RG (2009) Epidemiology of anterior cruciate ligament reconstruction: trends, readmissions, and subsequent knee surgery. J Bone Joint Surg Am 91:2321–2328
Ma L, Fan S (2017) CURE-SMOTE algorithm and hybrid algorithm for feature selection and parameter optimization based on random forests. BMC Bioinform 18:169
Magnussen RA, Meschbach NT, Kaeding CC, Wright RW, Spindler KP (2015) ACL graft and contralateral ACL tear risk within ten years following reconstruction: a systematic review. J Bone Joint Surg Am 3:e3
Martin RK, Wastvedt S, Pareek A, Persson A, Visnes H, Fenstad AM et al (2022) Predicting anterior cruciate ligament reconstruction revision: a machine learning analysis utilizing the Norwegian knee ligament register. J Bone Joint Surg Am 104:145–153
Martin RK, Wastvedt S, Pareek A, Persson A, Visnes H, Fenstad AM et al (2022) Predicting subjective failure of ACL reconstruction: a machine learning analysis of the Norwegian Knee Ligament Register and patient reported outcomes. J ISAKOS. https://doi.org/10.1016/j.jisako.2021.12.005
Martin RK, Wastvedt S, Pareek A, Persson A, Visnes H, Fenstad AM et al (2022) Machine learning algorithm to predict anterior cruciate ligament revision demonstrates external validity. Knee Surg Sports Traumatol Arthrosc 30:368–375
Martini ML, Neifert SN, Gal JS, Oermann EK, Gilligan JT, Caridi JM (2021) Drivers of prolonged hospitalization following spine surgery: a game-theory-based approach to explaining machine learning models. J Bone Joint Surg Am 103:64–73
Moons KG, Donders RA, Stijnen T, Harrell FE Jr (2006) Using the outcome for imputation of missing predictor values was preferred. J Clin Epidemiol 59:1092–1101
Nester JR, Torino D, Sylvestre D, Young A, Ney SM, Fernandez MM et al (2022) Risk of reoperation after primary anterior cruciate ligament reconstruction in children and adolescents. J Orthop Surg 30:10225536221122340
Pedersen AB, Mikkelsen EM, Cronin-Fenton D, Kristensen NR, Pham TM, Pedersen L et al (2017) Missing data and multiple imputation in clinical epidemiological research. Clin Epidemiol 9:157–166
Ramkumar PN, Karnuta JM, Haeberle HS, Owusu-Akyaw KA, Warner TS, Rodeo SA et al (2021) Association between preoperative mental health and clinically meaningful outcomes after osteochondral allograft for cartilage defects of the knee: a machine learning analysis. Am J Sports Med 49:948–957
Saithna A, Thaunat M, Delaloye JR, Ouanezar H, Fayard JM, Sonnery-Cottet B (2018) Combined ACL and anterolateral ligament reconstruction. JBJS Essent Surg Tech 8:e2
Sanders TL, MaraditKremers H, Bryan AJ, Larson DR, Dahm DL, Levy BA et al (2016) Incidence of anterior cruciate ligament tears and reconstruction: a 21-year population-based study. Am J Sports Med 44:1502–1507
Spragg LM, Prentice HA, Morris A, Funahashi TT, Maletis GB, Csintalan RP (2019) Femoral-tibial fixation affects risk of revision and reoperation after anterior cruciate ligament reconstruction using hamstring autograft. Knee Surg Sports Traumatol Arthrosc 27:3518–3526
Stekhoven DJ, Buhlmann P (2012) MissForest—non-parametric missing value imputation for mixed-type data. Bioinformatics 28:112–118
Sterne JAC, White IR, Carlin JB, Spratt M, Royston P, Kenward MG et al (2009) Multiple imputation for missing data in epidemiological and clinical research: potential and pitfalls. BMJ 338:b2393
Thaunat M, Clowez G, Saithna A, Cavalier M, Choudja E, Vieira TD et al (2017) Reoperation rates after combined anterior cruciate ligament and anterolateral ligament reconstruction: a series of 548 patients from the SANTI study group with a minimum follow-up of 2 years. Am J Sports Med 45:2569–2577
Ushio T, Okazaki K, Mizu-Uchi H, Hamai S, Akasaki Y, Nakashima Y (2017) Anterior cruciate ligament reconstruction in a patient who has received systemic steroids for autoimmune disease. Asia-Pac J Sports Med Arthrosc Rehabil Technol 11:12–14
Van Buuren S (2018) Flexible imputation of missing data. CRC Press, Boca Raton
van Dijck RA, Saris DB, Willems JW, Fievez AW (2008) Additional surgery after anterior cruciate ligament reconstruction: can we improve technical aspects of the initial procedure? Arthroscopy 24:88–95
Weber J, Koch M, Angele P, Zellner J (2018) The role of meniscal repair for prevention of early onset of osteoarthritis. J Exp Orthop 5:10–10
Young EP, Chan PH, Prentice HA, Amar K, Hurvitz AP, Khan NA (2021) Aseptic revision and reoperation risks after meniscectomy at the time of anterior cruciate ligament reconstruction. Am J Sports Med 49:1296–1304
Zhang Z, Ho KM, Hong Y (2019) Machine learning for the prediction of volume responsiveness in patients with oliguric acute kidney injury in critical care. Crit Care 23:112
Acknowledgements
The authors acknowledge that this is novel work being submitted for publication for the first time, the data has not been manipulated/misrepresented, and all authors contributed significantly to the body of work.
Funding
The authors would like to acknowledge the support from the Foderaro-Quattrone Musculoskeletal–Orthopaedic Surgery Research Innovation Fund.
Author information
Authors and Affiliations
Contributions
QJ participated in data collection, analysis, and writing/revision of the manuscript. MJ carried out statistical analysis, machine learning modeling, and writing of the manuscript. AA participated in data collection and revising of the manuscript. YL participated in data collection and revising of the manuscript. KJ participated in data collection and revising of the manuscript. BL contributed to conceptual design of the project and revising of the manuscript. CC contributed to conceptual design, coordination of the study, and revising of the manuscript. AK contributed to conceptual design, coordination of the study, and revising of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors have completed the COI form. All competing interests are listed at the end of the publication.
Ethical approval
The research conducted in this study was compliant with all relevant national regulations.
Informed consent
Informed consent was not required due to the retrospective and chart review nature of the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Johnson, Q.J., Jabal, M.S., Arguello, A.M. et al. Machine learning can accurately predict risk factors for all-cause reoperation after ACLR: creating a clinical tool to improve patient counseling and outcomes. Knee Surg Sports Traumatol Arthrosc 31, 4099–4108 (2023). https://doi.org/10.1007/s00167-023-07497-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-023-07497-7