Abstract
Purpose
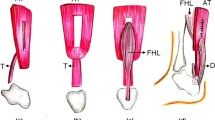
Achilles tendon ruptures (ATR) result in loss of strength and function of the gastrosoleus—Achilles tendon complex, probably because of gradual tendon elongation and calf muscle atrophy, even after surgical repair. Flexor hallucis longus (FHL) augmentation not only reinforces the repair and provides new blood supply to the tendon, but also protects the repair, internally splinting the repaired Achilles tendon, maintaining optimal tension. We prospectively compared the clinical outcomes of patients with acute ATR, managed with either percutaneous repair only or percutaneous repair and FHL augmentation.
Methods
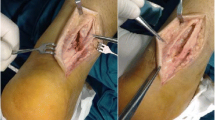
Patients with acute ATR undergoing operative management were divided into two groups. Thirty patients underwent percutaneous repair under local anesthesia, and 32 patients underwent percutaneous repair augmented by FHL tendon, harvested through a 3 cm longitudinal posteromedial incision, and transferred to the calcaneus, under epidural anesthesia. All patients were treated by a single surgeon between 2015 and 2019 and were followed prospectively for 24 months.
Results
The percutaneous only group was younger than the augmented one (35.4 ± 8.0 vs 40.4 ± 6.6 years, p = 0.01). In the augmented group, 25 patients stayed overnight and only 5 were day cases, whereas in the percutaneous only group 4 patients stayed overnight and 28 of them were day cases (p < 0.001). The duration of the procedure was significantly longer in the augmented group (38.9 ± 5.2 vs 13.2 ± 2.2 min, p < 0.001). At 24 months after repair, the Achilles tendon resting angle (ATRA) was better in the augmented group (−0.5 ± 1.7 vs −4.0 ± 2.7, p < 0.001), as was Achilles tendon rupture score (ATRS) (91.7 ± 2.2 vs 89.9 ± 2.4, p = 0.004). Calf circumference of the injured and the non-injured leg did not differ between the groups, as did the time interval to single toe raise and the time interval to walking in tiptoes. Although plantarflexion strength of the operated leg was significantly weaker than the non-operated leg in both groups, the difference in isometric strength of the operated leg between the groups was not significant at 24 months (435 ± 37.9 vs 436 ± 39.7 N, n.s.).
Conclusion
Percutaneous repair and FHL tendon augmentation may have a place in the management of acute Achilles tendon ruptures, reducing tendon elongation and improving functional outcome.
Level of evidence
Level II.


Similar content being viewed by others
References
Abdelatif NMN, Batista JP (2021) Endoscopic flexor hallucis longus transfer for the management of acute Achilles tendon ruptures in professional soccer players. Foot Ankle Int 43(2):164–175
Arshad Z, Lau EJS, Leow SH, Bhatia M (2021) Management of chronic Achilles ruptures: a scoping review. Int Orthop 45(10):2543–2559
Attia AK, Khamis KM, Dhooghe P, Bariteau JT, Labib SA, Myerson MS (2022) Outcomes and complications of open vs minimally invasive surgical repair of acute Achilles tendon rupture: a systematic review and meta-analysis of randomized controlled trials. Foot Ankle Orthop. https://doi.org/10.1177/03635465211053619
Batista JP, Abdelatif NMN, Del Vecchio JJ, Diniz P, Pereira H (2020) Endoscopic flexor hallucis longus transfer for the management of acute Achilles tendon ruptures: a prospective case series report with a minimum of 18 months’ follow-up. J Foot Ankle Surg 59(5):927–937
Batista JP, Del Vecchio JJ, Van Dijk N, Pereira H (2020) Endoscopic FHL transfer to augment Achilles disorders. J ISAKOS 5(2):109–114
Carmont MR, Grävare Silbernagel K, Brorsson A, Olsson N, Maffulli N, Karlsson J (2015) The Achilles tendon resting angle as an indirect measure of Achilles tendon length following rupture, repair, and rehabilitation. Asia-Pacific J Sport Med Arthrosc Rehabil Technol 2(2):49–55
Carmont MR, Maffulli N (2008) Modified percutaneous repair of ruptured Achilles tendon. Knee Surg Sports Traumatol Arthrosc 16(2):199–203
Carmont MR, Silbernagel KG, Edge A, Mei-Dan O, Karlsson J, Maffulli N (2013) Functional outcome of percutaneous Achilles repair: improvements in Achilles tendon total rupture score during the first year. Orthop J Sport Med. https://doi.org/10.1177/2325967113494584
Diniz P, Ferreira AS, Figueiredo L, Batista JP, Abdelatif N, Pereira H, Kerkhoffs GMMJ, Finkelstein SN, Ferreira FC (2022) Early analysis shows that endoscopic flexor hallucis longus transfer has a promising cost-effectiveness profile in the treatment of acute Achilles tendon ruptures. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-022-07146-5
Eliasson P, Agergaard AS, Couppé C, Svensson R, Hoeffner R, Warming S et al (2018) The ruptured Achilles tendon elongates for 6 months after surgical repair regardless of early or late weightbearing in combination with ankle mobilization: a randomized clinical trial. Am J Sports Med 46(10):2492–2502
Grassi A, Amendola A, Samuelsson K, Svantesson E, Romagnoli M, Bondi A et al (2018) Minimally invasive versus open repair for acute Achilles tendon rupture meta-analysis showing reduced complications, with similar outcomes, after minimally invasive surgery. J Bone Joint Surg 100-A(22):1969–1981
Heikkinen J, Lantto I, Piilonen J, Flinkkilä T, Ohtonen P, Siira P et al (2017) Tendon length, calf muscle atrophy, and strength deficit after acute Achilles tendon rupture: long-term follow-up of patients in a previous study. J Bone Joint Surg 99-A(18):1509–1515
Larsson E, Helander KN, Falkheden Henning L, Heiskanen M, Carmont MR, Grävare Silbernagel K, Brorsson A (2022) Achilles tendon resting angle is able to detect deficits after an Achilles tendon rupture, but it is not a surrogate for direct measurements of tendon elongation, function or symptoms. Knee Surg Sports Traumatol Arthrosc 10:1–8. https://doi.org/10.1007/s00167-022-07142-9
Lever CJ, Bosman HA, Robinson AHN (2018) The functional and dynamometer-tested results of transtendinous flexor hallucis longus transfer for neglected ruptures of the Achilles tendon at six years’ follow-up. Bone Joint J 100B(5):584–589
Lui TH, Chan WC, Maffulli N (2016) Endoscopic flexor hallucis longus tendon transfer for chronic achilles tendon rupture. Sports Med Arthrosc 24(1):38–41
Maffulli N, Del Buono A, Spiezia F, Maffulli GD, Longo UG, Denaro V (2013) Less-invasive semitendinosus tendon graft augmentation for the reconstruction of chronic tears of the Achilles tendon. Am J Sports Med 41(4):865–871
Maffulli N, D’Addona A, Maffulli GD, Gougoulias N, Oliva F (2020) Delayed (14–30 days) percutaneous repair of achilles tendon ruptures offers equally good results as compared with acute repair. Am J Sports Med 48(5):1181–1188
Maffulli N, Gougoulias N, Maffulli GD, Oliva F, Migliorini F (2022) Slowed-down rehabilitation following percutaneous repair of Achilles tendon rupture. Foot Ankle Int 43(2):244–252
Maffulli N, Oliva F, Maffulli GD, Del BA, Gougoulias N (2018) Surgical management of chronic Achilles tendon ruptures using less invasive techniques. Foot Ankle Surg 24(2):164–170
Maffulli N, Peretti GM (2019) Surgery or conservative management for Achilles tendon rupture? BMJ. https://doi.org/10.1136/bmj.k5344
Maffulli N, Peretti GM (2020) Treatment decisions for acute Achilles tendon ruptures. Lancet 395(10222):397–398. https://doi.org/10.1016/S0140-6736(19)33133-2
Meulenkamp B, Woolnough T, Cheng W, Shorr R, Stacey D, Richards M et al (2021) What is the best evidence to guide management of acute Achilles tendon ruptures? A systematic review and network meta-analysis of randomized controlled trials. Clin Orthop Relat Res 479(10):2119–2131
Moher D, Schulz KF, Altman D (2001) The CONSORT statement: revised recommendations for improving the quality of reports of parallel-group randomized trials. J Am Med Assoc 285(15):1987–1991
Ochen Y, Beks RB, Van Heijl M, Hietbrink F, Leenen LPH, Van Der Velde D et al (2019) Operative treatment versus nonoperative treatment of Achilles tendon ruptures: systematic review and meta-analysis. BMJ. https://doi.org/10.1136/bmj.k5120
Oksanen MM, Haapasalo HH, Elo PP, Laine HJ (2014) Hypertrophy of the flexor hallucis longus muscle after tendon transfer in patients with chronic Achilles tendon rupture. Foot Ankle Surg 20(4):253–257
Olsson N, Nilsson-Helander K, Karlsson J, Eriksson BI, Thomée R, Faxén E et al (2011) Major functional deficits persist 2 years after acute Achilles tendon rupture. Knee Surg Sports Traumatol Arthrosc 19(8):1385–1393
Saxena A, Maffulli N, Jin A, Isa E, Arthur WP, Asthana S (2021) Acute Achilles tendon rupture repair in athletically active patients: results on 188 tendons. J Foot Ankle Surg 60(5):935–940. https://doi.org/10.1053/j.jfas.2021.01.009
Sadek AF, Fouly EH, Laklok MA, Amin MF (2015) Functional and MRI follow-up after reconstruction of chronic ruptures of the Achilles tendon Myerson type III using the triple-loop plantaris tendon wrapped with central turndown flap: a case series. J Orthop Surg Res. https://doi.org/10.1186/s13018-015-0256-y
Tallon C, Maffulli N, Ewen SWB (2001) Ruptured Achilles tendons are significantly more degenerated than tendinopathic tendons. Med Sci Sports Exerc 33(12):1983–1990
Tam KF, Lui THMR (2017) Imaging of the Achilles Tendon after surgical repair. Open Orthop J 11(1):697–703
Vega J, Vilá J, Batista J, Malagelada F, Dalmau-Pastor M (2018) Endoscopic flexor hallucis longus transfer for chronic noninsertional Achilles tendon rupture. Foot Ankle Int 39(12):1464–1472
Funding
No funding was received
Author information
Authors and Affiliations
Contributions
All authors contributed to the preparation of the manuscript and approved its content. NM: Performed the surgical procedures, and supervised the patient’s post-operative rehabilitation; FO: Did the follow-up assessment; PC: Analyzed the data; NG and PC: Prepared the initial manuscript; NM and NG: As senior authors, edited the final form of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The present investigation was approved by our local ethics committee.
Informed consent
All patients gave their signed informed consent to participate.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Maffulli, N., Gougoulias, N., Christidis, P. et al. Primary augmentation of percutaneous repair with flexor hallucis longus tendon for Achilles tendon ruptures reduces tendon elongation and may improve functional outcome. Knee Surg Sports Traumatol Arthrosc 31, 94–101 (2023). https://doi.org/10.1007/s00167-022-07183-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-07183-0