Abstract
Purpose
The aims of this study were to determine the prevalence of metal hypersensitivity, and identify pre-operative factors which could predict susceptibility to hypersensitivity reactions among patients scheduled for primary total knee arthroplasty (TKA). The present study used a testing method consistent with the recognised biological response to metals.
Methods
A prospective cross-sectional analysis of 220 patients was conducted. All patients received a testing protocol using lymphocyte transformation test to evaluate reactivity to possible contents of orthopaedic implants. Test response is interpreted as stimulation index (SI) values. A comprehensive questionnaire was used to evaluate prior exposure. Patients were categorised according to SI values and the odds ratios (OR) were calculated as comparative effect measure for each predetermined prior exposure factor.
Results
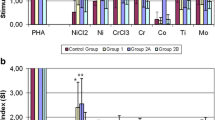
The prevalence of metal sensitivity response was 28% (n = 61) among patients with susceptibility to at least one agent (SI = 2 to 4.9), and 3.2% (n = 7) among patients with true hypersensitivity (SI ≥ 5). The population-weighted prevalence, adjusted for sampling weights of symptomatic knee osteoarthritis, was SI ≥ 5 = 4.7% (95% CI 0.4–11.8%) and SI ≥ 2 = 35.2% (95% CI 24.8–48.6%). Stimulation index levels of response to materials were markedly varied with the highest being aluminium. Female sex, smoking history, cutaneous reaction to jewellery, occupational exposure, and dental procedures were among factors shown to increase the odds of having higher reactivity response to tested metals. Nevertheless, patients with well-functioning prior contralateral TKA did not appear at greater risk of having either sensitivity or susceptibility with odds ratio (OR) = 0.2 (95% CI 0.01–3.2), p: NS and OR = 0.6 (95% CI 0.3–1.2), p: NS, respectively. Prior positive patch test was neither predictor of susceptibility to hypersensitivity OR = 1.2 (95% CI 0.6–2.6) p: NS nor predictor of true hypersensitivity OR = 0.7 (95% CI 0.08–6.1), p: NS.
Conclusion
Among patients scheduled for primary TKA with no prior clinical features of metal allergy the prevalence of true hypersensitivity to at least one metal is just over 3%. Patients are likely to encounter a material to which they have pre-existing susceptibility to hypersensitivity. With certain prior exposure factors, there was increased susceptibility to metal hypersensitivity reaction evoking an acquired condition.
Level of evidence: Level II, prospective cross-sectional study.




Similar content being viewed by others
References
Kurtz S, Ong K, Lau E, Mowat F, Halpern M (2007) Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 89:780–785
Kurtz SM, Ong KL, Lau E, Bozic KJ (2014) Impact of the economic downturn on total joint replacement demand in the United States: updated projections to 2021. J Bone Joint Surg Am 96:624–630
Patel A, Pavlou G, Mujica-Mota RE, Toms AD (2015) The epidemiology of revision total knee and hip arthroplasty in England and Wales: a comparative analysis with projections for the United States. A study using the National Joint Registry dataset. Bone Joint J 97-b:1076–1081
Middleton S, Toms A (2016) Allergy in total knee arthroplasty: a review of the facts. Bone Joint J 98-b:437–441
Gustafson K, Jakobsen SS, Lorenzen ND, Thyssen JP, Johansen JD, Bonefeld CM et al (2014) Metal release and metal allergy after total hip replacement with resurfacing versus conventional hybrid prosthesis. Acta Orthop 85:348–354
Thomsen M, Rozak M, Thomas P (2011) Pain in a chromium-allergic patient with total knee arthroplasty: disappearance of symptoms after revision with a special surface-coated TKA–a case report. Acta Orthop 82:386–388
McLawhorn AS, Bjerke-Kroll BT, Blevins JL, Sculco PK, Lee YY, Jerabek SA (2015) Patient-reported allergies are associated with poorer patient satisfaction and outcomes after lower extremity arthroplasty: a retrospective cohort study. J Arthroplasty 30:1132–1136
Basketter DA, Briatico-Vangosa G, Kaestner W, Lally C, Bontinck WJ (1993) Nickel, cobalt and chromium in consumer products: a role in allergic contact dermatitis? Contact Dermatitis 28:15–25
Bloemke AD, Clarke HD (2015) Prevalence of self-reported metal allergy in patients undergoing primary total knee arthroplasty. J Knee Surg 28:243–246
Duarte I, Mendonca RF, Korkes KL, Lazzarini R, Hafner MFS (2018) Nickel, chromium and cobalt: the relevant allergens in allergic contact dermatitis. Comparative study between two periods: 1995–2002 and 2003–2015. An Bras Dermatol 93:59–62
Granchi D, Cenni E, Tigani D, Trisolino G, Baldini N, Giunti A (2008) Sensitivity to implant materials in patients with total knee arthroplasties. Biomaterials 29:1494–1500
Lutzner J, Hartmann A, Dinnebier G, Spornraft-Ragaller P, Hamann C, Kirschner S (2013) Metal hypersensitivity and metal ion levels in patients with coated or uncoated total knee arthroplasty: a randomised controlled study. Int Orthop 37:1925–1931
Thyssen JP, Jakobsen SS, Engkilde K, Johansen JD, Soballe K, Menne T (2009) The association between metal allergy, total hip arthroplasty, and revision. Acta Orthop 80:646–652
Hallab NJ, Caicedo M, Finnegan A, Jacobs JJ (2008) Th1 type lymphocyte reactivity to metals in patients with total hip arthroplasty. J Orthop Surg Res 3:6
Hallab NJ, Jacobs JJ (2009) Biologic effects of implant debris. Bull NYU Hosp Jt Dis 67:182–188
Basko-Plluska JL, Thyssen JP, Schalock PC (2011) Cutaneous and systemic hypersensitivity reactions to metallic implants. Dermatitis 22:65–79
Hallab N, Merritt K, Jacobs JJ (2001) Metal sensitivity in patients with orthopaedic implants. J Bone Joint Surg Am 83:428–436
Bach F, Hirschhorn K (1964) lymphocyte interaction: a potential histocompatibility test in vitro. Science 143:813–814
Bain B, Vas MR, Lowenstein L (1964) the development of large immature mononuclear cells in mixed leukocyte cultures. Blood 23:108–116
Everness KM, Gawkrodger DJ, Botham PA, Hunter JA (1990) The discrimination between nickel-sensitive and non-nickel-sensitive subjects by an in vitro lymphocyte transformation test. Br J Dermatol 122:293–298
Marcusson JA (1996) Contact allergies to nickel sulfate, gold sodium thiosulfate and palladium chloride in patients claiming side-effects from dental alloy components. Contact Dermatitis 34:320–323
Räsänen L, Sainio H, Lehto M, Reunala T (1991) Lymphocyte proliferation test as a diagnostic aid in chromium contact sensitivity. Contact Dermatitis 25:25–29
Stejskal VD, Cederbrant K, Lindvall A, Forsbeck M (1994) MELISA-an in vitro tool for the study of metal allergy. Toxicol In Vitro 8:991–1000
Stejskal VD, Danersund A, Lindvall A, Hudecek R, Nordman V, Yaqob A et al (1999) Metal-specific lymphocytes: biomarkers of sensitivity in man. Neuro Endocrinol Lett 20:289–298
Valentine-Thon E, Schiwara HW (2003) Validity of MELISA for metal sensitivity testing. Neuro Endocrinol Lett 24:57–64
Stejskal V, Reynolds T, Bjorklund G (2015) Increased frequency of delayed type hypersensitivity to metals in patients with connective tissue disease. J Trace Elem Med Biol 31:230–236
Paxton EW, Fithian DC, Stone ML, Silva P (2003) The reliability and validity of knee-specific and general health instruments in assessing acute patellar dislocation outcomes. Am J Sports Med 31:487–492
(1995) The World Health Organization Quality of Life assessment (WHOQOL): position paper from the World Health Organization. Soc Sci Med 41:1403–1409
Birtwhistle R, Morkem R, Peat G, Williamson T, Green ME, Khan S et al (2015) Prevalence and management of osteoarthritis in primary care: an epidemiologic cohort study from the Canadian Primary Care Sentinel Surveillance Network. CMAJ Open 3:E270-275
Nussbaum DA, Gailloud P, Murphy K (2004) A review of complications associated with vertebroplasty and kyphoplasty as reported to the Food and Drug Administration medical device related web site. J Vasc Interv Radiol 15:1185–1192
Chaw SH, Chow KY (2015) The allergic patient. In: Chan YK, Kwee Peng NG, Si Mui Sim D (eds) Pharmacological Basis of Acute Care, Springer, Switzerland, pp 213–218
Vasconcelos C, Gailloud P, Martin JB, Murphy KJ (2001) Transient arterial hypotension induced by polymethylmethacrylate injection during percutaneous vertebroplasty. J Vasc Interv Radiol 12:1001–1002
Valentine-Thon E, Müller K, Guzzi G, Kreisel S, Ohnsorge P, Sandkamp M (2006) LTT-MELISA is clinically relevant for detecting and monitoring metal sensitivity. Neuro Endocrinol Lett 27(Suppl 1):17–24
Granchi D, Cenni E, Giunti A, Baldini N (2012) Metal hypersensitivity testing in patients undergoing joint replacement: a systematic review. J Bone Joint Surg Br 94:1126–1134
De Smet KA, Van Der Straeten C, Van Orsouw M, Doubi R, Backers K, Grammatopoulos G (2011) Revisions of metal-on-metal hip resurfacing: lessons learned and improved outcome. Orthop Clin North Am 42:259–269
Graves SE, Rothwell A, Tucker K, Jacobs JJ, Sedrakyan A (2011) A multinational assessment of metal-on-metal bearings in hip replacement. J Bone Joint Surg Am 93(Suppl 3):43–47
Merritt K, Rodrigo JJ (1996) Immune response to synthetic materials. Sensitization of patients receiving orthopaedic implants. Clin Orthop Relat Res 326:71–79
Pinson ML, Coop CA, Webb CN (2014) Metal hypersensitivity in total joint arthroplasty. Ann Allergy Asthma Immunol 113:131–136
Razak A, Ebinesan AD, Charalambous CP (2013) Metal allergy screening prior to joint arthroplasty and its influence on implant choice: a delphi consensus study amongst orthopaedic arthroplasty surgeons. Knee Surg Relat Res 25:186–193
Thomsen M, Rozak M, Thomas P (2013) Use of allergy implants in Germany: results of a survey. Orthopade 42:597–601
Atanaskova Mesinkovska N, Tellez A, Molina L, Honari G, Sood A, Barsoum W et al (2012) The effect of patch testing on surgical practices and outcomes in orthopedic patients with metal implants. Arch Dermatol 148:687–693
Rooker GD, Wilkinson JD (1980) Metal sensitivity in patients undergoing hip replacement. A prospective study. J Bone Joint Surg Br 62-b:502–505
Waterman AH, Schrik JJ (1985) Allergy in hip arthroplasty. Contact Dermatitis 13:294–301
Niki Y, Matsumoto H, Otani T, Yatabe T, Kondo M, Yoshimine F et al (2005) Screening for symptomatic metal sensitivity: a prospective study of 92 patients undergoing total knee arthroplasty. Biomaterials 26:1019–1026
Acknowledgements
None.
Funding
The study was funded through a research grant awarded by Smith & Nephew, Inc. 150 Minuteman Road Andover, Massachusetts 01810 USA.
Author information
Authors and Affiliations
Contributions
TB: data analysis and interpretation, and manuscript writing. FV: data acquisition, interpretation of data, and manuscript writing. JD: design, data acquisition, and analysis and interpretation of data. MB: design, data acquisition, and critical revision of manuscript. JF: design, data acquisition, and critical revision of manuscript. All the authors have been actively involved in the writing and revision of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has received or will receive benefits for personal or professional use from a commercial party related directly or indirectly to the subject of this article.
Ethical approval
Institutional review ethics body approval. Reference Number: 2014–1101. Comité d'éthique de la recherche du CIUSSS du Nord-de-l’Île-de-Montréal (CÉR) Montreal, Canada.
Informed consent
All participants signed a study participation consent form as per study protocol and ethical board approval process.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Boutefnouchet, T., Vallières, F., Delisle, J. et al. Lymphocyte transformation test reveals low prevalence of true metal hypersensitivity among pre-operative total knee arthroplasty patients. Knee Surg Sports Traumatol Arthrosc 30, 4123–4133 (2022). https://doi.org/10.1007/s00167-022-06951-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-06951-2