Abstract
Purpose
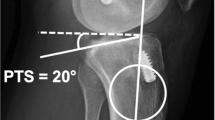
The posterior tibial slope (PTS) is considered a risk factor for anterior cruciate ligament (ACL) injury. However, the influence of PTS on graft failure following ACL reconstruction remains relatively unknown. Therefore, this systematic review was conducted to investigate whether PTS could be a potential risk factor for graft failure after ACL reconstruction.
Methods
PubMed, EMBASE, Cochrane Library, Web of Science, China National Knowledge Infrastructure Database, and Wanfang Database were comprehensively searched from inception to March 31, 2021. Observational studies reporting the associations of medial tibial plateau slope (MTPS) or lateral tibial plateau slope (LTPS) with graft failure after ACL reconstruction were evaluated.
Results
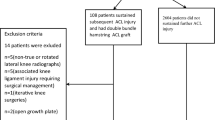
Twenty studies involving 12 case–control studies, 4 retrospective studies and 4 cross-sectional studies including 5326 patients met the final inclusion criteria. The high heterogeneity and the characteristics of nonrandomized controlled trials limited data synthesis. Fifteen of the 20 included studies detected a significant association between increased PTS and ACL graft failure, while 5 studies concluded that increased PTS was not associated with ACL graft failure. Ten studies suggested that MTPS is associated with ACL graft failure, and six studies suggested that LTPS is associated with ACL graft failure. The mean MTPS values for nonfailure group ranged from 3.5° ± 2.5° to 14.4° ± 2.8°. For the graft failure group, MTPS ranged from 4.71° ± 2.41° to 17.2° ± 2.2°. The mean LTPS values for nonfailure group ranged from 2.9° ± 2.1° to 11.9° ± 3.0°. For the graft failure group, LTPS ranged from 5.5° ± 3.0° to 13.3° ± 3.0°. The reported PTS values that caused ACL graft failure was greater than 7.4° to 17°.
Conclusion
Based on the current clinical evidence, increased PTS is associated with a higher risk of ACL graft failure after ACL reconstruction. Despite various methods of measuring PTS have high reliability, there is still vast disagreement in the actual value of PTS.
Level of evidence
IV.




Similar content being viewed by others
References
Bayer S, Meredith SJ, Wilson KW, de Sa D, Pauyo T, Byrne K et al (2020) Knee morphological risk factors for anterior cruciate ligament injury: a systematic review. J Bone Jt Surg Am 102:703–718
Bernhardson AS, Aman ZS, Dornan GJ, Kemler BR, Storaci HW, Brady AW et al (2019) Tibial slope and its effect on force in anterior cruciate ligament grafts: anterior cruciate ligament force increases linearly as posterior tibial slope increases. Am J Sports Med 47:296–302
Bowman EN, Limpisvasti O, Cole BJ, ElAttrache NS (2021) Anterior cruciate ligament reconstruction graft preference most dependent on patient age: a survey of United States surgeons. Arthroscopy 37:1559–1566
Christensen JJ, Krych AJ, Engasser WM, Vanhees MK, Collins MS, Dahm DL (2015) Lateral tibial posterior slope is increased in patients with early graft failure after anterior cruciate ligament reconstruction. Am J Sports Med 43:2510–2514
Chung SC, Chan WL, Wong SH (2011) Lower limb alignment in anterior cruciate ligament-deficient versus -intact knees. J Orthop Surg (Hong Kong) 19:303–308
Cooper JD, Wang W, Prentice HA, Funahashi TT, Maletis GB (2019) The association between tibial slope and revision anterior cruciate ligament reconstruction in patients ≤21 years old: a matched case-control study including 317 revisions. Am J Sports Med 47:3330–3338
Cusumano A, Capitani P, Messina C, de Girolamo L, Viganò M, Ravasio G et al (2021) Different timing in allograft and autograft maturation after primary anterior cruciate ligament reconstruction does not influence the clinical outcome at mid-long-term follow-up. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06785-41-10
Dean RS, Larson CM, Waterman BR (2021) Posterior tibial slope: understand bony morphology to protect knee cruciate ligament grafts. Arthroscopy 37:2029–2030
Dejour D, Pungitore M, Valluy J, Nover L, Saffarini M, Demey G (2019) Tibial slope and medial meniscectomy significantly influence short-term knee laxity following ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 27:3481–3489
Dejour H, Bonnin M (1994) Tibial translation after anterior cruciate ligament rupture. Two radiological tests compared. J Bone Jt Surg Br 76:745–749
Dekker TJ, Godin JA, Dale KM, Garrett WE, Taylor DC, Riboh JC (2017) Return to sport after pediatric anterior cruciate ligament reconstruction and its effect on subsequent anterior cruciate ligament injury. J Bone Jt Surg Am 99:897–904
Di Benedetto P, Buttironi MM, Mancuso F, Beltrame A, Gisonni R, Causero A (2020) Anterior cruciate ligament reconstruction: the role of lateral posterior tibial slope as a potential risk factor for failure. Acta Biomed 91:e2020024–e2020024
Digiacomo JE, Palmieri-Smith RM, Redman JA III, Lepley LK (2018) Examination of knee morphology after secondary ipsilateral ACL injury compared with those that have not been reinjured: a preliminary study. J Sport Rehabil 27:73–82
Everhart JS, Jones MH, Yalcin S, Reinke EK, Huston LJ, Andrish JT et al (2021) The clinical radiographic incidence of posttraumatic osteoarthritis 10 years after anterior cruciate ligament reconstruction: data from the MOON Nested Cohort. Am J Sports Med 49:1251–1261
Funchal LFZ, Astur DC, Ortiz R, Cohen M (2019) The presence of the arthroscopic “floating meniscus” sign as an indicator for surgical intervention in patients with combined anterior cruciate ligament and Grade II medial collateral ligament injury. Arthroscopy 35:930–937
Gaj E, Monaco E, De Carli A, Wolf MR, Massafra C, Redler A et al (2020) Measurement technique for posterior tibial slope on radiographs can affect its relationship to the risk of anterior cruciate ligament rupture. Int Orthop 45:1469–1475
Grassi A, Macchiarola L, Urrizola Barrientos F, Zicaro JP, Costa Paz M, Adravanti P et al (2019) Steep posterior tibial slope, anterior tibial subluxation, deep posterior lateral femoral condyle, and meniscal deficiency are common findings in multiple anterior cruciate ligament failures: an MRI case-control study. Am J Sports Med 47:285–295
Grassi A, Signorelli C, Urrizola F, Macchiarola L, Raggi F, Mosca M et al (2019) Patients with failed anterior cruciate ligament reconstruction have an increased posterior lateral tibial plateau slope: a case-controlled study. Arthroscopy 35:1172–1182
Grassi A, Signorelli C, Urrizola F, Raggi F, Macchiarola L, Bonanzinga T et al (2018) Anatomical features of tibia and femur: Influence on laxity in the anterior cruciate ligament deficient knee. Knee 25:577–587
Gupta R, Singhal A, Malhotra A, Soni A, Masih GD, Raghav M (2020) Predictors for anterior cruciate ligament (ACL) re-injury after successful primary ACL reconstruction (ACLR). Malays Orthop J 14:50–56
Hashemi J, Chandrashekar N, Gill B, Beynnon BD, Slauterbeck JR, Schutt RC Jr et al (2008) The geometry of the tibial plateau and its influence on the biomechanics of the tibiofemoral joint. J Bone Jt Surg Am 90:2724–2734
Hohmann E, Bryant A, Reaburn P, Tetsworth K (2010) Does posterior tibial slope influence knee functionality in the anterior cruciate ligament-deficient and anterior cruciate ligament-reconstructed knee? Arthroscopy 26:1496–1502
Hosseinzadeh S, Kiapour AM (2020) Sex differences in anatomic features linked to anterior cruciate ligament injuries during skeletal growth and maturation. Am J Sports Med 48:2205–2212
Hudek R, Schmutz S, Regenfelder F, Fuchs B, Koch PP (2009) Novel measurement technique of the tibial slope on conventional MRI. Clin Orthop Relat Res 467:2066–2072
Imhoff FB, Mehl J, Comer BJ, Obopilwe E, Cote MP, Feucht MJ et al (2019) Slope-reducing tibial osteotomy decreases ACL-graft forces and anterior tibial translation under axial load. Knee Surg Sports Traumatol Arthrosc 27:3381–3389
Jaecker V, Drouven S, Naendrup JH, Kanakamedala AC, Pfeiffer T, Shafizadeh S (2018) Increased medial and lateral tibial posterior slopes are independent risk factors for graft failure following ACL reconstruction. Arch Orthop Trauma Surg 138:1423–1431
Koo TK, Li MY (2016) A Guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med 15:155–163
LaPrade RF, Oro FB, Ziegler CG, Wijdicks CA, Walsh MP (2010) Patellar height and tibial slope after opening-wedge proximal tibial osteotomy: a prospective study. Am J Sports Med 38:160–170
Lee CC, Youm YS, Cho SD, Jung SH, Bae MH, Park SJ et al (2018) Does posterior tibial slope affect graft rupture following anterior cruciate ligament reconstruction? Arthroscopy 34:2152–2155
Li Y, Hong L, Feng H, Wang Q, Zhang H, Song G (2014) Are failures of anterior cruciate ligament reconstruction associated with steep posterior tibial slopes? A case control study. Chin Med J (Engl) 127:2649–2653
McGinn T, Wyer PC, Newman TB, Keitz S, Leipzig R, For GG (2004) Tips for learners of evidence-based medicine: 3. Measures of observer variability (kappa statistic). CMAJ 171:1369–1373
Mitchell BC, Siow MY, Bastrom T, Bomar JD, Pennock AT, Parvaresh K et al (2021) Predictive value of the magnetic resonance imaging-based coronal lateral collateral ligament sign on adolescent anterior cruciate ligament reconstruction graft failure. Am J Sports Med 49:935–940
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:332–336
Mouarbes D, Menetrey J, Marot V, Courtot L, Berard E, Cavaignac E (2019) Anterior cruciate ligament reconstruction: a systematic review and meta-analysis of outcomes for quadriceps tendon autograft versus bone-patellar tendon-bone and hamstring-tendon autografts. Am J Sports Med 47:3531–3540
Napier RJ, Garcia E, Devitt BM, Feller JA, Webster KE (2019) Increased radiographic posterior tibial slope is associated with subsequent injury following revision anterior cruciate ligament reconstruction. Orthop J Sports Med 7:2325967119879373
Nerhus TK, Ekeland A, Solberg G, Sivertsen EA, Madsen JE, Heir S (2017) Radiological outcomes in a randomized trial comparing opening wedge and closing wedge techniques of high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 25:910–917
Ni QK, Song GY, Zhang ZJ, Zheng T, Feng Z, Cao YW et al (2020) Steep posterior tibial slope and excessive anterior tibial translation are predictive risk factors of primary anterior cruciate ligament reconstruction failure: a case-control study with prospectively collected data. Am J Sports Med 48:2954–2961
Ro KH, Kim HJ, Lee DH (2018) The transportal technique shows better clinical results than the transtibial techniques for single-bundle anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 26:2371–2380
Rozinthe A, van Rooij F, Demey G, Saffarini M, Dejour D (2021) Tibial slope correction combined with second revision ACLR grants good clinical outcomes and prevents graft rupture at 7–15-year follow-up. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06750-1
Samuelsen BT, Webster KE, Johnson NR, Hewett TE, Krych AJ (2017) Hamstring autograft versus patellar tendon autograft for ACL reconstruction: is there a difference in graft failure rate? a meta-analysis of 47,613 patients. Clin Orthop Relat Res 475:2459–2468
Sauer S, English R, Clatworthy M (2018) The ratio of tibial slope and meniscal bone angle for the prediction of ACL reconstruction failure risk. Surg J (N Y) 4:e152–e159
Shelbourne KD, Benner RW, Jones JA, Gray T (2021) Posterior tibial slope in patients undergoing anterior cruciate ligament reconstruction with patellar tendon autograft: analysis of subsequent ACL graft tear or contralateral ACL tear. Am J Sports Med 49:620–625
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73:712–716
Sonnery-Cottet B, Mogos S, Thaunat M, Archbold P, Fayard JM, Freychet B et al (2014) Proximal tibial anterior closing wedge osteotomy in repeat revision of anterior cruciate ligament reconstruction. Am J Sports Med 42:1873–1880
Southam BR, Colosimo AJ, Grawe B (2018) Underappreciated factors to consider in revision anterior cruciate ligament reconstruction: a current concepts review. Orthop J Sports Med 6:2325967117751689
Wang YL, Yang T, Zeng C, Wei J, Xie DX, Yang YH et al (2017) Association between tibial plateau slopes and anterior cruciate ligament injury: a meta-analysis. Arthroscopy 33:1248–1259
Webb JM, Salmon LJ, Leclerc E, Pinczewski LA, Roe JP (2013) Posterior tibial slope and further anterior cruciate ligament injuries in the anterior cruciate ligament-reconstructed patient. Am J Sports Med 41:2800–2804
Winkler PW, Wagala NN, Hughes JD, Lesniak BP, Musahl V (2021) A high tibial slope, allograft use, and poor patient-reported outcome scores are associated with multiple ACL graft failures. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06460-8
Won HH, Chang CB, Je MS, Chang MJ, Kim TK (2013) Coronal limb alignment and indications for high tibial osteotomy in patients undergoing revision ACL reconstruction. Clin Orthop Relat Res 471:3504–3511
Wright RW, Haas AK, Huston LJ (2013) Radiographic findings in revision anterior cruciate ligament reconstructions from the Mars cohort. J Knee Surg 26:239–247
Ziegler CG, DePhillipo NN, Kennedy MI, Dekker TJ, Dornan GJ, LaPrade RF (2021) Beighton Score, tibial slope, tibial subluxation, quadriceps circumference difference, and family history are risk factors for anterior cruciate ligament graft failure: a retrospective comparison of primary and revision anterior cruciate ligament reconstructions. Arthroscopy 37:195–205
Acknowledgements
The National Natural Science Foundation of China (81874017, 81960403, 82060405, 82060413, and 82160422); Natrual Science Foundation of Gansu Province of China (20JR5RA320, and 21JR7RA393); Cuiying Scientific and Technological Innovation Program of Lanzhou University Second Hospital (CY2017-ZD02, CY2017-QN11, CY2020-BJ03, and CY2021-MS-B02); Fundamental Research Funds for the Central Universities (lzujbky-2021-kb30).
Funding
Funding was provided by The National Natural Science Foundation of China (81874017, 81960403, 82060405, 82060413, and 82160422), Natrual Science Foundation of Gansu Province of China (20JR5RA320), Cuiying Scientific and Technological Innovation Program of Lanzhou University Second Hospital (CY2017-ZD02, CY2017-QN11, and CY2020-BJ03) and Fundamental Research Funds for the Central Universities (lzujbky-2021-kb30).
Author information
Authors and Affiliations
Contributions
We declare that each author (ZL, JJ, QY, YT, XL, JH, KZ, LW, FT, BG, YX, MW) has participated in the following work for this manuscript. Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work; drafting the work or revising it critically for important intellectual content; final approval of the version to be published; agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding authors
Ethics declarations
Conflict of interest
All authors declared that there is no conflict of interest.
Ethical approval
This systematic review did not used any human data that belonged to our patients. All of the data was extracted from the previous studies that have been published previously. The registered number of systematic review has been added to the Methods section, which was erased due to the request for reviewing. And the abbreviations of previously erased names have been released in the Methods section.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, Z., Jiang, J., Yi, Q. et al. An increased posterior tibial slope is associated with a higher risk of graft failure following ACL reconstruction: a systematic review. Knee Surg Sports Traumatol Arthrosc 30, 2377–2387 (2022). https://doi.org/10.1007/s00167-022-06888-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-06888-6