Abstract
Purpose
Orthopedic literature remains divided on the utility of biologic augmentation to optimize outcomes after isolated meniscal repair. The aim of this systematic review is to analyze the clinical outcomes and re-operation rates of biologically augmented meniscal repairs.
Methods
PubMed, CINAHL, Cochrane, and EMBASE databases were queried in October 2020 for published literature on isolated meniscal repair with biological augmentation. Studies were assessed for quality and risk of bias by two appraisal tools. Patient demographics, meniscal tear characteristics, surgical procedure, augmentation type, post-operative rehabilitation, patient reported outcome measures, and length of follow-up were recorded, reviewed, and analyzed by two independent reviewers.
Results
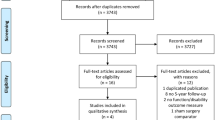
Of 3794 articles, 18 met inclusion criteria and yielded 537 patients who underwent biologic augmentation of meniscal repair. The biologically augmented repair rates were 5.8–27.0% with PRP augmentation, 0.0–28.5% with fibrin clot augmentation, 0.0–12.9% with marrow stimulation, and 0.0% with stem cell augmentation. One of seven studies showed lower revision rates with augmented meniscal repair compared to standard repair techniques, whereas five of seven found no benefit. Three of ten studies found significant functional improvement of biologically augmented repair versus standard repair techniques and six of ten studies found no difference. There was significant heterogeneity in methods for biologic preparation, delivery, and post-operative rehabilitation protocols.
Conclusion
Patients reported significant improvements in functional outcomes scores after repair with biological augmentation, though the benefit over standard repair controls is questionable. Revision rates after biologically augmented meniscal repair also appear similar to standard repair techniques. Clinicians should bear this in mind when considering biologic augmentation in the setting of meniscal repair.
Level of evidence
IV.



Similar content being viewed by others
Abbreviations
- PRP:
-
Platelet-rich plasma
- MSC:
-
Mesenchymal stem cells
- BMP:
-
Bone morphogenic protein
- PRISMA:
-
Preferred Reporting Items for Systematic Review and Meta Analysis
- MCMS:
-
Modified Coleman Methodology Score
- JBI:
-
Joanna Briggs Institute
- VAS:
-
Visual Analog Scale
- IKDC:
-
International Knee Documentation Committee
- TAS:
-
Tegner Activity Score
- DVT:
-
Deep vein thrombosis
- CRP:
-
C-reactive protein
- LOE:
-
Level of evidence
- Mos:
-
Months
- MS:
-
Marrow stimulation
- SC:
-
Stem cells
- Wk/wks:
-
Week/weeks
- NWB:
-
Non-weight-bearing
- WBAT:
-
Weight-bearing as tolerated
- PWB:
-
Partial weight-bearing
References
Ahn J-H, Kwon O-J, Nam T-S (2015) Arthroscopic repair of horizontal meniscal cleavage tears with marrow-stimulating technique. Arthroscopy 31(1):92–98
Arnoczky SP, Warren RF (1982) Microvasculature of the human meniscus. Am J Sports Med 10(2):90–95
Arnoczky SP, Warren RF, Spivak JM (1988) Meniscal repair using an exogenous fibrin clot. An experimental study in dogs. J Bone Jt Surg 70(8):1209–1217
Bernard CD, Kennedy NI, Tagliero AJ, Camp CL, Saris DBF, Levy BA, Stuart MJ, Krych AJ (2020) Medial meniscus posterior root tear treatment: a matched cohort comparison of nonoperative management, partial meniscectomy, and repair. Am J Sports Med 48(1):128–132
Biedert RM (2000) Treatment of intrasubstance meniscal lesions: a randomized prospective study of four different methods. Knee Surg Sport Traumatol Arthrosc 8(2):104–108
Ciemniewska-Gorzela K, Bąkowski P, Naczk J, Jakob R, Piontek T (2020) Complex meniscus tears treated with collagen matrix wrapping and bone marrow blood injection: clinical effectiveness and survivorship after a minimum of 5 years’ follow-up. Cartilage 1(1):1–11
Clayton RAE, Court-Brown CM (2008) The epidemiology of musculoskeletal tendinous and ligamentous injuries. Injury 39(12):1338–1344
Dai W-L, Zhang H, Lin Z-M, Shi Z-J (2019) Wang J Efficacy of platelet-rich plasma in arthroscopic repair for discoid lateral meniscus tears. BMC Musculoskeletal Disord 20(1):113
Dean CS, Chahla J, Matheny LM, Mitchell JJ, LaPrade RF (2017) Outcomes after biologically augmented isolated meniscal repair with marrow venting are comparable with those after meniscal repair with concomitant anterior cruciate ligament reconstruction. Am J Sports Med 45(6):1341–1348
Englund M, Guermazi A, Gale D, Hunter DJ, Aliabadi P, Clancy M, Felson DT (2008) Incidental meniscal findings on knee MRI in middle-aged and elderly persons. N Engl J Med 359(11):1108–1115
Everhart JS, Cavendish PA, Eikenberry A, Magnussen RA, Kaeding CC, Flanigan DC (2019) Platelet-rich plasma reduces failure risk for isolated meniscal repairs but provides no benefit for meniscal repairs with anterior cruciate ligament reconstruction. Am J Sports Med 47(8):1789–1796
Freedman KB, Nho SJ, Cole BJ (2003) Marrow stimulating technique to augment meniscus repair. Arthroscopy 19(7):794–798
Griffin JW, Hadeed MM, Werner BC, Diduch DR, Carson EW, Miller MD (2015) Platelet-rich plasma in meniscal repair: does augmentation improve surgical outcomes? Clin Orthop Relat Res 473(5):1665–1672
Haunschild ED, Huddleston HP, Chahla J, Gilat R, Cole BJ, Yanke AB (2020) Platelet-rich plasma augmentation in meniscal repair surgery: a systematic review of comparative studies. Arthroscopy 36(6):1765–1774
Henning CE, Lynch MA, Yearout KM, Vequist SW, Stallbaumer RJ, Decker KA (1990) Arthroscopic meniscal repair using an exogenous fibrin clot. Clin Orthop Relat Res 252:64–72
Horie MD, Driscoll MD, Sampson HW, Sekiya I, Caroom CT, Prockop DJ, Thomas DB (2012) Implantation of allogenic synovial stem cells. J Bone Jt Surg 94(8):701–712
Horie M, Sekiya I, Muneta T, Ichinose S, Matsumoto K, Saito H, Murakami T, Kobayashi E (2009) Intra-articular injected synovial stem cells differentiate into meniscal cells directly and promote meniscal regeneration without mobilization to distant organs in rat massive meniscal defect. Stem Cells 27(4):878–887
Howarth WR, Brochard K, Campbell SE, Grogan BF (2016) Effect of microfracture on meniscal tear healing in a goat (capra hircus) model. Orthopedics 39(2):105–110
Ishida K, Kuroda R, Miwa M, Tabata Y, Hokugo A, Kawamoto T, Sasaki K, Doita M, Kurosaka M (2007) The regenerative effects of platelet-rich plasma on meniscal cells in vitro and its in vivo application with biodegradable gelatin hydrogel. Tissue Eng 13(5):1103–1112
Ishimura M, Tamai S, Fujisawa Y (1991) Arthroscopic meniscal repair with fibrin glue. Arthroscopy 7(2):177–181
Jakobsen RB, Engebretsen L, Slauterbeck JR (2005) An analysis of the quality of cartilage repair studies. J Bone Jt Surg 87(10):2232–2239
James EW, LaPrade CM, Feagin JA, LaPrade RF (2015) Repair of a complete radial tear in the midbody of the medial meniscus using a novel crisscross suture transtibial tunnel surgical technique: a case report. Knee Surg Sport Traumatol Arthrosc 23(9):2750–2755
Jong RH, Ha JK, Jang SH, Lee DW, Kim JG (2013) Arthroscopic inside-out repair of complete radial tears of the meniscus with a fibrin clot. Knee Surg Sport Traumatol Arthrosc 21(9):2126–2130
Kamimura T, Kimura M (2014) Meniscal repair of degenerative horizontal cleavage tears using fibrin clots clinical and arthroscopic outcomes in 10 cases. Orthop J Sports Med 2(11):1–7
Kaminski R, Kulinski K, Kozar-Kaminska K, Wasko MK, Langner M, Pomianowski S (2019) Repair Augmentation of unstable, complete vertical meniscal tears with bone marrow venting procedure: a prospective, randomized, double-blind, parallel-group, placebo-controlled study. Arthroscopy 35(5):1500–1508
Kaminski R, Kulinski K, Kozar-Kaminska K, Wielgus M, Langner M, Wasko MK, Kowalczewski J, Pomianowski S (2018) A prospective, randomized, double-blind, parallel-group, placebo-controlled study evaluating meniscal healing, clinical outcomes, and safety in patients undergoing meniscal repair of unstable, complete vertical meniscal tears (bucket handle) augmented with platelet-rich plasma. Biomed Res Int 2018:9315815
Kemmochi M, Sasaki S, Takahashi M, Nishimura T, Aizawa C, Kikuchi J (2018) The use of platelet-rich fibrin with platelet-rich plasma support meniscal repair surgery. J Orthopaed 15(2):711–720
Lyman S, Hidaka C, Valdez AS, Hetsroni I, Pan TJ, Do H, Dunn WR, Marx RG (2013) Risk factors for meniscectomy after meniscal repair. Am J Sports Med 41(12):2772–2778
Majewski M, Susanne H, Klaus S (2006) Epidemiology of athletic knee injuries: a 10-year study. Knee 13(3):184–188
Moola S, Munn Z, Tufanaru C, Aromataris E, Sears K, Sfetcu R, Currie M, Qureshi R, Mattis P, Lisy K, Mu P-F (2020) Chapter 7: systematic reviews of etiology and risk. JBI Man Evid Synth. https://doi.org/10.46658/JBIMES-20-08
Nakayama H, Kanto R, Kambara S, Iseki T, Onishi S, Yoshiya S (2019) Successful treatment of degenerative medial meniscal tears in well-alignedss knees with fibrin clot implantation. Knee Surg Sport Traumatol Arthrosc 28(11):3466–3473
Pujol N, Salle De Chou E, Boisrenoult P, Beaufils P (2014) Platelet-rich plasma for open meniscal repair in young patients: any benefit? Knee Surg Sport Traumatol Arthrosc 23(1):51–58
Pujol N, Tardy N, Boisrenoult P, Beaufils P (2015) Long-term outcomes of all-inside meniscal repair. Knee Surg Sport Traumatol Arthrosc 23(1):219–224
Sekiya I, Koga H, Otabe K, Nakagawa Y, Katano H, Ozeki N, Mizuno M, Horie M, Kohno Y, Katagiri K, Watanabe N, Muneta T (2019) Additional use of synovial mesenchymal stem cell transplantation following surgical repair of a complex degenerative tear of the medial meniscus of the knee: a case report. Cell Transplant 28(11):1445–1454
Sochacki KR, Varshneya K, Calcei JG, Safran MR, Abrams GD, Donahue J, Sherman SL (2020) Comparing meniscectomy and meniscal repair: a matched cohort analysis utilizing a national insurance database. Am J Sports Med 48(10):2353–2359
Stein T, Mehling AP, Welsch F, Von Eisenhart-Rothe R, Jäger A (2010) Long-term outcome after arthroscopic meniscal repair versus arthroscopic partial meniscectomy for traumatic meniscal tears. Am J Sports Med 38(8):1542–1548
Tallon C, Coleman BD, Khan KM, Maffulli N (2001) Outcome of surgery for chronic achilles tendinopathy a critical review. Am J Sports Med 29(3):315–320
Taylor SA, Rodeo SA (2013) Augmentation techniques for isolated meniscal tears. Curr Rev Musculoskelet Med 6(2):95–101
Trams E, Kulinski K, Kozar-Kaminska K, Pomianowski S, Kaminski R (2020) The clinical use of platelet-rich plasma in knee disorders and surgery—a systematic review and meta-analysis. Life 10(6):94
Tudor F, McDermott ID, Myers P (2014) Meniscal repair: a review of current practice. Orthop Traum 28:88–96
Van Trommel MF, Simonian PT, Potter HG, Wickiewicz TL (1998) Arthroscopic meniscal repair with fibrin clot of complete radial tears of the lateral meniscus in the avascular zone. Arthroscopy 14(4):360–365
Wells ME, Scanaliato JP, Dunn JC, Garcia ESJ (2021) Meniscal Injuries: mechanism and classification. Sports Med Arthrosc 29(3):154–157
Author information
Authors and Affiliations
Contributions
RK was the primary author of the manuscript and primary reviewer. EAO developed the concept and search strategy and assisted in manuscript drafting and review, as well as served as the discordant reviewer. GM was the secondary literature reviewer. TC and OS aided in manuscript preparation and editing. SL performed statistical analysis and table design. LSO oversaw and provided senior support as well as editing of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The author declares that they have no conflict of interest.
Funding
None.
Ethical approval
This manuscript was exempt from IRB review.
Informed consent
N/A.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Keller, R.E., O’Donnell, E.A., Medina, G.I.S. et al. Biological augmentation of meniscal repair: a systematic review. Knee Surg Sports Traumatol Arthrosc 30, 1915–1926 (2022). https://doi.org/10.1007/s00167-021-06849-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06849-5