Abstract
Purpose
To compare the clinical and radiological outcomes in patients undergoing anterior cruciate ligament reconstruction (ACLR) with, or without, LARS augmentation.
Methods
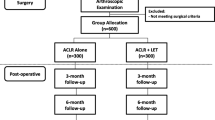
One-hundred and thirty-six patients that underwent double-bundle ACLR with (DB Hams/LARS, n = 67), or without (DB Hams, n = 69), LARS augmentation, were assessed clinically and with Magnetic Resonance Imaging (MRI) at a minimum of 7-years post-surgery. Patients were assessed via patient-reported outcome measures (PROMs), KT-1000 (laxity), isokinetic knee extensor and flexor strength and a 4-hop test battery. Limb symmetry indices (LSIs) were calculated. The Whole-Organ Magnetic Resonance Imaging Score (WORMS) evaluated knee status via MRI. Sport participation, secondary operations, ACL re-tears and contralateral ACL tears were reported.
Results
No differences (n.s.) were observed in demographics, PROMs, KT-1000 scores or strength and hop LSIs. Normal (< 3 mm side-to-side differences) KT-1000 scores were observed in 64 (92.8%) and 59 (88.1%) of DB Hams and DB Hams/LARS patients, respectively. Comparative rates of satisfaction were reported. Knee flexor strength and hop test LSIs were all ˃95% in both groups, which was 94.2% and 96.7% for knee extensor strength in the DB Hams and DB Hams/LARS cohorts, respectively. While 53 (76.8%) and 52 (77.6%) of the DB Hams and DB Hams/LARS patients had returned to pivoting sports, 42 (60.9%) and 41 (61.2%) were participating in pivoting sports at the minimum 7-year review. No difference (n.s.) was observed in the WORMS (12.3 DB Hams, 16.7 DB Hams/LARS). Of the cohort assessed, 8 (11%) DB Hams and 11 (16%) DB Hams/LARS patients had undergone secondary surgery. In addition to one patient in each group that demonstrated ACL rupture on MRI, an additional cohort of patients were excluded from the current analysis due to prior re-tear (DB Hams n = 6, DB Hams/LARS n = 8) or contralateral ACL tear (DB Hams n = 4, DB Hams/LARS n = 4).
Conclusions
Comparable outcomes were observed after double-bundle ACLR using autologous hamstrings with, or without, LARS augmentation. Therefore, while these outcomes do not justify the additional use of synthetic augmentation given the lack of further benefit and additional cost, higher rates of graft failure, synovitis and early osteoarthritic change previously reported were not observed.
Level of Evidence
III.

Similar content being viewed by others
References
Ardern CL, Taylor NF, Feller JA, Webster KE (2014) Fifty-five per cent return to competitive sport following anterior cruciate ligament reconstruction surgery: an updated systematic review and meta-analysis including aspects of physical functioning and contextual factors. Br J Sports Med 48:1543–1552
Aujla RS, Ebert JR, Annear PT (2021) Anterior cruciate ligament reconstruction using autologous hamstrings augmented with the ligament augmentation and reconstruction system versus hamstrings alone: a comparative cohort study. Orthop J Sports Med 9:23259671211046630
Barber-Westin SD, Noyes FR, McCloskey JW (1999) Rigorous statistical reliability, validity, and responsiveness testing of the Cincinnati knee rating system in 350 subjects with uninjured, injured, or anterior cruciate ligament-reconstructed knees. Am J Sports Med 27:402–416
Bodendorfer BM, Michaelson EM, Shu HT, Apseloff NA, Spratt JD, Nolton EC et al (2019) Suture augmented versus standard anterior cruciate ligament reconstruction: a matched comparative analysis. Arthroscopy 35:2114–2122
Culvenor AG, Collins NJ, Guermazi A, Cook JL, Vicenzino B, Khan KM et al (2015) Early knee osteoarthritis is evident one year following anterior cruciate ligament reconstruction: a magnetic resonance imaging evaluation. Arthritis Rheumatol 67:946–955
Culvenor AG, Collins NJ, Guermazi A, Cook JL, Vicenzino B, Whitehead TS et al (2016) Early patellofemoral osteoarthritis features one year after anterior cruciate ligament reconstruction: symptoms and quality of life at three years. Arthritis Care Res (Hoboken) 68:784–792
Duchman KR, Lynch TS, Spindler KP (2017) Graft selection in anterior cruciate ligament surgery: who gets what and why? Clin Sports Med 36:25–33
Ebert JR, Annear PT (2019) ACL Reconstruction using autologous hamstrings augmented with the ligament augmentation and reconstruction system provides good clinical scores, high levels of satisfaction and return to sport, and a low retear rate at 2 years. Orthop J Sports Med 7:2325967119879079
Ebert JR, Edwards P, Yi L, Joss B, Ackland T, Carey-Smith R et al (2018) Strength and functional symmetry is associated with post-operative rehabilitation in patients following anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 26:2353–2361
Falconer TM, Tusak L, Breidahl WH, Annear PT (2015) The LARS augmented 4-tunnel hamstring “hybrid” ACLR graft construction allows accelerated rehabilitation without knee laxity - case series of 111 patients after 2 years. J Musc Res. https://doi.org/10.1142/S0218957715500207
Falconiero RP, DiStefano VJ, Cook TM (1998) Revascularization and ligamentization of autogenous anterior cruciate ligament grafts in humans. Arthroscopy 14:197–205
Haberfield MJ, Patterson BE, Crossley KM, Bruder AM, Guermazi A, Whitehead TS et al (2021) Should return to pivoting sport be avoided for the secondary prevention of osteoarthritis after anterior cruciate ligament reconstruction? A prospective cohort study with MRI, radiographic and symptomatic outcomes. Osteoarthritis Cartilage. https://doi.org/10.1016/j.joca.2021.04.003
Hamido F, Al Harran H, Al Misfer AR, El Khadrawe T, Morsy MG, Talaat A et al (2015) Augmented short undersized hamstring tendon graft with LARS(R) artificial ligament versus four-strand hamstring tendon in anterior cruciate ligament reconstruction: preliminary results. Orthop Traumatol Surg Res 101:535–538
Hunter DJ, Guermazi A, Lo GH, Grainger AJ, Conaghan PG, Boudreau RM et al (2011) Evolution of semi-quantitative whole joint assessment of knee OA: MOAKS (MRI Osteoarthritis Knee Score). Osteoarthritis Cartilage 19:990–1002
Irrgang JJ, Anderson AF, Boland AL, Harner CD, Kurosaka M, Neyret P et al (2001) Development and validation of the international knee documentation committee subjective knee form. Am J Sports Med 29:600–613
Jenkins DH (1978) The repair of cruciate ligaments with flexible carbon fibre. A longer term study of the induction of new ligaments and of the fate of the implanted carbon. J Bone Joint Surg Br 60B:520–522
Jungmann PM, Baum T, Nevitt MC, Nardo L, Gersing AS, Lane NE et al (2016) Degeneration in ACL injured knees with and without reconstruction in relation to muscle size and fat content-data from the osteoarthritis initiative. PLoS One 11:e0166865
Kdolsky RK, Gibbons DF, Kwasny O, Schabus R, Plenk H Jr (1997) Braided polypropylene augmentation device in reconstructive surgery of the anterior cruciate ligament: long-term clinical performance of 594 patients and short-term arthroscopic results, failure analysis by scanning electron microscopy, and synovial histomorphology. J Orthop Res 15:1–10
Klein W, Jensen KU (1992) Synovitis and artificial ligaments. Arthroscopy 8:116–124
Lord L, Cristiani R, Edman G, Forssblad M, Stalman A (2020) One sixth of primary anterior cruciate ligament reconstructions may undergo reoperation due to complications or new injuries within 2 years. Knee Surg Sports Traumatol Arthrosc 28:2478–2485
Makisalo SE, Visuri T, Viljanen A, Jokio P (1996) Reconstruction of the anterior cruciate ligament with carbon fibres: unsatisfactory results after 8 years. Knee Surg Sports Traumatol Arthrosc 4:132–136
Maletius W, Gillquist J (1997) Long-term results of anterior cruciate ligament reconstruction with a Dacron prosthesis. The frequency of osteoarthritis after seven to eleven years. Am J Sports Med 25:288–293
Nicholas SJ, D’Amato MJ, Mullaney MJ, Tyler TF, Kolstad K, McHugh MP (2004) A prospectively randomized double-blind study on the effect of initial graft tension on knee stability after anterior cruciate ligament reconstruction. Am J Sports Med 32:1881–1886
Noyes FR, Barber SD, Mooar LA (1989) A rationale for assessing sports activity levels and limitations in knee disorders. Clin Orthop Relat Res 246:238–249
Patterson BE, Culvenor AG, Barton CJ, Guermazi A, Stefanik JJ, Morris HG et al (2018) Worsening knee osteoarthritis features on magnetic resonance imaging 1 to 5 years after anterior cruciate ligament reconstruction. Am J Sports Med 46:2873–2883
Peterfy CG, Guermazi A, Zaim S, Tirman PF, Miaux Y, White D et al (2004) Whole-organ magnetic resonance imaging score (WORMS) of the knee in osteoarthritis. Osteoarthritis Cartilage 12:177–190
Pinczewski LA, Lyman J, Salmon LJ, Russell VJ, Roe J, Linklater J (2007) A 10-year comparison of anterior cruciate ligament reconstructions with hamstring tendon and patellar tendon autograft: a controlled, prospective trial. Am J Sports Med 35:564–574
Pugh L, Mascarenhas R, Arneja S, Chin PY, Leith JM (2009) Current concepts in instrumented knee-laxity testing. Am J Sports Med 37:199–210
Rading J, Peterson L (1995) Clinical experience with the Leeds-Keio artificial ligament in anterior cruciate ligament reconstruction. A prospective two-year follow-up study. Am J Sports Med 23:316–319
Richmond JC, Manseau CJ, Patz R, McConville O (1992) Anterior cruciate reconstruction using a Dacron ligament prosthesis. A long-term study. Am J Sports Med 20:24–28
Roemer FW, Frobell R, Lohmander LS, Niu J, Guermazi A (2014) Anterior cruciate ligament osteoarthritis score (ACLOAS): Longitudinal MRI-based whole joint assessment of anterior cruciate ligament injury. Osteoarthritis Cartilage 22:668–682
Saper MG (2018) Quadriceps tendon autograft anterior cruciate ligament reconstruction with independent suture tape reinforcement. Arthrosc Tech 7:e1221–e1229
Shea KG, Carey JL, Richmond J, Sandmeier R, Pitts RT, Polousky JD et al (2015) The American academy of orthopaedic surgeons evidence-based guideline on management of anterior cruciate ligament injuries. J Bone Joint Surg Am 97:672–674
Tegner Y, Lysholm J (1985) Rating systems in the evaluation of knee ligament injuries. Clin Orthop Relat Res 198:43–49
Vaquette C, Viateau V, Guerard S, Anagnostou F, Manassero M, Castner DG et al (2013) The effect of polystyrene sodium sulfonate grafting on polyethylene terephthalate artificial ligaments on in vitro mineralisation and in vivo bone tissue integration. Biomaterials 34:7048–7063
Viateau V, Manassero M, Anagnostou F, Guerard S, Mitton D, Migonney V (2013) Biological and biomechanical evaluation of the ligament advanced reinforcement system (LARS AC) in a sheep model of anterior cruciate ligament replacement: a 3-month and 12-month study. Arthroscopy 29:1079–1088
Webster KE, Hewett TE (2021) Anterior cruciate ligament injury and knee osteoarthritis: an umbrella systematic review and meta-analysis. Clin J Sport Med. https://doi.org/10.1097/JSM.0000000000000894
Wiggins AJ, Grandhi RK, Schneider DK, Stanfield D, Webster KE, Myer GD (2016) Risk of secondary injury in younger athletes after anterior cruciate ligament reconstruction: a systematic review and meta-analysis. Am J Sports Med 44:1861–1876
Funding
Independent funding in the form of a research grant was provided by Corin to assist this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Ethics approval was obtained by the Hollywood Private Hospital (HPH382).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ebert, J.R., Nairn, R., Breidahl, W. et al. Double-bundle anterior cruciate ligament reconstruction using autologous hamstrings with LARS augmentation demonstrates comparable outcomes to hamstrings alone, without evidence of synovitis or early osteoarthritis. Knee Surg Sports Traumatol Arthrosc 30, 2320–2328 (2022). https://doi.org/10.1007/s00167-021-06801-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06801-7