Abstract
Purpose
Anterior cruciate ligament (ACL) tears have a major impact on the individual and society. Long term effects may be mediated by injuries that occur concurrently to the ACL tear. The purpose of this study was to describe in a nationwide cohort the traumatic meniscal injuries and bone marrow lesions concomitant to ACL tears, their age and sex distribution and the rate any association with ACL reconstruction.
Methods
All ACL tears in Iceland from 2006 to 2011 and their concomitant bone marrow lesions and meniscal injuries were identified from MRI reports. These injuries were further classified by location, sex and age. The cohort was divided into under 17, 17–29, 30–49 and above 50 to reflect likely differences in the mechanisms of injury and risk factors that may vary with age. Data from the Icelandic Social Insurance Administration were used identify all those who were operated. Descriptive analysis was performed to show the proportion of ACL injured knees sustaining concomitant injuries and how these injuries varied with age, sex, and subsequent treatment
Results
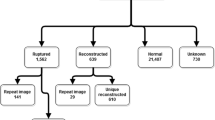
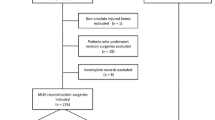
1365 knees with ACL ruptures were included. Only 13% of knees had no concomitant injury identified. Overall, 57% of knees had a bone marrow lesion in at least one location and 70% of knees had at least one traumatic meniscal injury. A greater number of combined lateral tibial and femoral bone marrow lesion was seen in younger age groups (χ2 (3) = 113.32, p < 0.0001). Bruises in the medial compartment were the least common concomitant injuries. More injuries were related to higher chances of ACL reconstruction (OR 1.6, 95% CI 1.4–1.7). Age was associated with risk of all injury types and locations with older age generally being associated with fewer injuries.
Conclusion
In an ACL ruptured cohort, the overall incidence of BMLs may be lower and meniscus injuries higher than previously reported. However, these injuries are more prevalent in the younger cohort potentially resulting in a poorer long-term prognosis. Knowledge of the association between age and concomitant injuries will help guide rehabilitation.
Level of evidence
II.



Similar content being viewed by others
References
Ageberg E, Forssblad M, Herbertsson P, Roos EM (2010) Sex differences in patient-reported outcomes after anterior cruciate ligament reconstruction: data from the Swedish knee ligament register. Am J Sports Med 38:1334–1342
Ajuied A, Wong F, Smith C, Norris M, Earnshaw P, Back D, Davies A (2014) Anterior cruciate ligament injury and radiologic progression of knee osteoarthritis: a systematic review and meta-analysis. Am J Sports Med 42:2242–2252
Amin S, Guermazi A, LaValley MP, Niu J, Clancy M, Hunter DJ, Grigoryan M, Felson DT (2008) Complete anterior cruciate ligament tear and the risk for cartilage loss and progression of symptoms in men and women with knee osteoarthritis. Osteoarthr Cartil 16:897–902
Aravindh P, Wu T, Chan CX, Wong KL, Krishna L (2018) Association of compartmental bone bruise distribution with concomitant intra-articular and extra-articular injuries in acute anterior cruciate ligament tears after noncontact sports trauma. Orthop J Sports Med. https://doi.org/10.1177/2325967118767625
Balasingam S, Sernert N, Magnusson H, Kartus J (2018) Patients with concomitant intra-articular lesions at index surgery deteriorate in their knee injury and osteoarthritis outcome score in the long term more than patients with isolated anterior cruciate ligament rupture: a study from the swedish national anterior cruciate ligament register. Arthroscopy 34:1520–1529
Bisson LJ, Kluczynski MA, Hagstrom LS, Marzo JM (2013) A prospective study of the association between bone contusion and intra-articular injuries associated with acute anterior cruciate ligament tear. Am J Sports Med 41:1801–1807
Boden BP, Dean GS, Feagin JA, Garrett WE (2000) Mechanisms of anterior cruciate ligament injury. Orthopedics 23:573–578
Bordoni V, di Laura FG, Previtali D, Tamborini S, Candrian C, Cristallo Lacalamita M, Del Grande F, Filardo G (2019) Bone bruise and anterior cruciate ligament tears: presence, distribution pattern, and associated lesions in the pediatric population. Am J Sports Med 47:3181–3186
Conway JR, Lex A, Gehlenborg N (2017) UpSetR: an R package for the visualization of intersecting sets and their properties. Bioinform Oxf Engl 33:2938–2940
Culvenor AG, Collins NJ, Guermazi A, Cook JL, Vicenzino B, Khan KM, Beck N, van Leeuwen J, Crossley KM (2015) Early knee osteoarthritis is evident one year following anterior cruciate ligament reconstruction: a magnetic resonance imaging evaluation. Arthritis Rheumatol 67:946–955
Driban JB, Lohmander S, Frobell RB (2017) Posttraumatic bone marrow lesion volume and knee pain within 4 weeks after anterior cruciate ligament injury. J Athl Train 52:575–580
Dufka FL, Lansdown DA, Zhang AL, Allen CR, Ma CB, Feeley BT (2016) Accuracy of MRI evaluation of meniscus tears in the setting of ACL injuries. Knee 23:460–464
Englund M, Guermazi A, Gale D, Hunter DJ, Aliabadi P, Clancy M, Felson DT (2008) Incidental meniscal findings on knee MRI in middle-aged and elderly persons. N Engl J Med 359:1108–1115
Filardo G, Kon E, Tentoni F, Andriolo L, Di Martino A, Busacca M, Di Matteo B, Marcacci M (2016) Anterior cruciate ligament injury: post-traumatic bone marrow oedema correlates with long-term prognosis. Int Orthop 40:183–190
Frobell RB (2011) Change in cartilage thickness, posttraumatic bone marrow lesions, and joint fluid volumes after acute ACL disruption: a two-year prospective mri study of sixty-one subjects. J Bone Jt Surg Am 93:1096–1103
Frobell RB, Le Graverand M-P, Buck R, Roos EM, Roos HP, Tamez-Pena J, Totterman S, Lohmander LS (2009) The acutely ACL injured knee assessed by MRI: changes in joint fluid, bone marrow lesions, and cartilage during the first year. Osteoarthr Cartil 17:161–167
Frobell RB, Roos EM, Roos HP, Ranstam J, Lohmander LS (2010) A randomized trial of treatment for acute anterior cruciate ligament tears. N Engl J Med 363:331
Graf BK, Cook DA, De Smet AA, Keene JS (1993) “Bone bruises” on magnetic resonance imaging evaluation of anterior cruciate ligament injuries. Am J Sports Med 21:220–223
Granan L-P, Bahr R, Steindal K, Furnes O, Engebretsen L (2008) Development of a national cruciate ligament surgery registry: the Norwegian National Knee Ligament Registry. Am J Sports Med 36:308–315
Harris KP, Driban JB, Sitler MR, Cattano NM, Balasubramanian E (2017) Tibiofemoral osteoarthritis after surgical or nonsurgical treatment of anterior cruciate ligament rupture: a systematic review. J Athl Train 52:507–517
Herzog MM, Marshall SW, Lund JL, Pate V, Mack CD, Spang JT (2018) Trends in incidence of ACL reconstruction and concomitant procedures among commercially insured individuals in the United States, 2002–2014. Sports Health 10:523–531
Kim SY, Spritzer CE, Utturkar GM, Toth AP, Garrett WE, DeFrate LE (2015) Knee Kinematics during noncontact anterior cruciate ligament injury as determined from bone bruise location. Am J Sports Med 43:2515–2521
Kluczynski MA, Kang JV, Marzo JM, Bisson LJ (2016) Magnetic resonance imaging and intra-articular findings after anterior cruciate ligament injuries in ice hockey versus other sports. Orthop J Sports Med. https://doi.org/10.1177/2325967116646534
Kluczynski MA, Marzo JM, Rauh MA, Bernas GA, Bisson LJ (2016) A case-control study comparing bone bruising and intra-articular injuries in patients undergoing anterior cruciate ligament reconstruction with and without medial collateral ligament tears. Orthop J Sports Med. https://doi.org/10.1177/2325967116660053
Kobayashi H, Kanamura T, Koshida S, Miyashita K, Okado T, Shimizu T, Yokoe K (2010) Mechanisms of the anterior cruciate ligament injury in sports activities: a twenty-year clinical research of 1,700 athletes. J Sports Sci Med 9:669–675
Koga H, Nakamae A, Shima Y, Iwasa J, Myklebust G, Engebretsen L, Bahr R, Krosshaug T (2010) Mechanisms for noncontact anterior cruciate ligament injuries: knee joint kinematics in 10 injury situations from female team handball and basketball. Am J Sports Med 38:2218–2225
Krassowski M (2020) krassowski/complex-upset. Zenodo. https://doi.org/10.5281/zenodo.3700590
Krosshaug T, Slauterbeck JR, Engebretsen L, Bahr R (2007) Biomechanical analysis of anterior cruciate ligament injury mechanisms: three-dimensional motion reconstruction from video sequences. Scand J Med Sci Sports 17:508–519
Lattermann C, Jacobs CA, Reinke EK, Scaramuzza EA, Huston LJ, Dunn WR, Spindler KP (2017) Are bone bruise characteristics and articular cartilage pathology associated with inferior outcomes 2 and 6 years after anterior cruciate ligament reconstruction? Cartilage 8:139–145
Lex A, Gehlenborg N, Strobelt H, Vuillemot R, Pfister H (2014) UpSet: visualization of intersecting sets. IEEE Trans Vis Comput Graph 20:1983–1992
Lohmander LS, Englund PM, Dahl LL, Roos EM (2007) The long-term consequence of anterior cruciate ligament and meniscus injuries: osteoarthritis. Am J Sports Med 35:1756–1769
Magosch A, Mouton C, Nührenbörger C, Seil R (2020) Medial meniscus ramp and lateral meniscus posterior root lesions are present in more than a third of primary and revision ACL reconstructions. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06352-3
van Meer BL, Meuffels DE, van Eijsden WA, Verhaar JAN, Bierma-Zeinstra SMA, Reijman M (2015) Which determinants predict tibiofemoral and patellofemoral osteoarthritis after anterior cruciate ligament injury? A systematic review. Br J Sports Med 49:975–983
Murrell GA, Maddali S, Horovitz L, Oakley SP, Warren RF (2001) The effects of time course after anterior cruciate ligament injury in correlation with meniscal and cartilage loss. Am J Sports Med 29:9–14
Nicholls M, Aspelund T, Ingvarsson T, Briem K (2018) Nationwide study highlights a second peak in ACL tears for women in their early forties. Knee Surg Sports Traumatol Arthrosc 26:648–654
Øiestad BE, Engebretsen L, Storheim K, Risberg MA (2009) Knee osteoarthritis after anterior cruciate ligament injury: a systematic review. Am J Sports Med 37:1434–1443
Oiestad BE, Holm I, Aune AK, Gunderson R, Myklebust G, Engebretsen L, Fosdahl MA, Risberg MA (2010) Knee function and prevalence of knee osteoarthritis after anterior cruciate ligament reconstruction: a prospective study with 10 to 15 years of follow-up. Am J Sports Med 38:2201–2210
Patel SA, Hageman J, Quatman CE, Wordeman SC, Hewett TE (2014) Prevalence and location of bone bruises associated with anterior cruciate ligament injury and implications for mechanism of injury: a systematic review. Sports Med 44:281–293
Phelan N, Rowland P, Galvin R, O’Byrne JM (2016) A systematic review and meta-analysis of the diagnostic accuracy of MRI for suspected ACL and meniscal tears of the knee. Knee Surg Sports Traumatol Arthrosc 24:1525–1539
Roemer FW, Frobell R, Hunter DJ, Crema MD, Fischer W, Bohndorf K, Guermazi A (2009) MRI-detected subchondral bone marrow signal alterations of the knee joint: terminology, imaging appearance, relevance and radiological differential diagnosis. Osteoarthr Cartil 17:1115–1131
Røtterud JH, Ara EA, Forssblad M, Engebretsen L, Arøen A (2013) Effect of meniscal and focal cartilage lesions on patient-reported outcome after anterior cruciate ligament reconstruction: a nationwide cohort study from Norway and Sweden of 8476 patients with 2-year follow-up. Am J Sports Med 41:535–543
Song G, Zhang H, Wang Q, Zhang J, Li Y, Feng H (2016) Bone contusions after acute noncontact anterior cruciate ligament injury are associated with knee joint laxity, concomitant meniscal lesions, and anterolateral ligament abnormality. Arthroscopy 32:2331–2341
Spindler KP, Schils JP, Bergfeld JA, Andrish JT, Weiker GG, Anderson TE, Piraino DW, Richmond BJ, Medendorp SV (1993) Prospective study of osseous, articular, and meniscal lesions in recent anterior cruciate ligament tears by magnetic resonance imaging and arthroscopy. Am J Sports Med 21:551–557
Suter LG, Smith SR, Katz JN, Englund M, Hunter DJ, Frobell R, Losina E (2017) Projecting lifetime risk of symptomatic knee osteoarthritis and total knee replacement in individuals sustaining a complete anterior cruciate ligament tear in early adulthood. Arthritis Care Res 69:201–208
Szkopek K, Warming T, Neergaard K, Jørgensen HL, Christensen HE, Krogsgaard M (2012) Pain and knee function in relation to degree of bone bruise after acute anterior cruciate ligament rupture. Scand J Med Sci Sports 22:635–642
Wittstein J, Vinson E, Garrett W (2014) Comparison between sexes of bone contusions and meniscal tear patterns in noncontact anterior cruciate ligament injuries. Am J Sports Med 42:1401–1407
Wood SN (2011) Fast stable restricted maximum likelihood and marginal likelihood estimation of semiparametric generalized linear models. J R Stat Soc Ser B Stat Methodol 73:3–36
Wood SN (2017) Generalized additive models: an introduction with R. Chapman and Hall/CRC, Boca Raton
Yoon JP, Chang CB, Yoo JH, Kim SJ, Choi JY, Choi J-A, Seong SC, Kim TK (2010) Correlation of magnetic resonance imaging findings with the chronicity of an anterior cruciate ligament tear. J Bone Jt Surg Am 92:353–360
Yoon KH, Yoo JH, Kim K-I (2011) Bone contusion and associated meniscal and medial collateral ligament injury in patients with anterior cruciate ligament rupture. J Bone Jt Surg Am 93:1510–1518
Zhang L, Hacke JD, Garrett WE, Liu H, Yu B (2019) Bone bruises associated with anterior cruciate ligament injury as indicators of injury mechanism: a systematic review. Sports Med 49:453–462
Acknowledgements
The authors would like to thank Thor Aspelund, Brynjólfur Gauti Jónsson, Vébjörn Fivelstad, Sigurjón Björn Grétarsson, Guðni Rafn Harðarson, and Ingvi Karl Jónsson for their help in this project.
Author information
Authors and Affiliations
Contributions
MN, TI and KB conceived and designed the study, MN, TI and KB collected the data and classified the reports. MN analysed the data. MN wrote the initial manuscript. All authors contributed in revising the manuscript and gave their final approval of the submitted version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Funding
University of Iceland research fund.
Ethical approval
National Bioethics Committee of Iceland (Vísindasiðanefnd, VSNb2011100031/03.07).
Informed consent
Not needed for this type of study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nicholls, M., Ingvarsson, T. & Briem, K. Younger age increases the risk of sustaining multiple concomitant injuries with an ACL rupture. Knee Surg Sports Traumatol Arthrosc 29, 2701–2708 (2021). https://doi.org/10.1007/s00167-021-06538-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06538-3