Abstract
Purpose
The purpose of this systematic review was to determine the return to sport rates following surgical management of ostechondritis dissecans of the elbow.
Methods
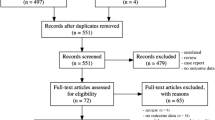
The databases EMBASE, PubMed, and MEDLINE were searched for relevant literature from database inception until August 2020 and studies were screened by two reviewers independently and in duplicate for studies reporting rates of return to sport following surgical management of posterior shoulder instability. A meta-analysis of proportions was used to combine the rates of return to sport using a random effects model. A risk of bias assessment was performed for all included studies using the MINORS score.
Results
Overall, 31 studies met inclusion criteria and comprised of 548 patients (553 elbows) with a median age of 14 (range 10–18.5) and a median follow-up of 39 months (range 5–156). Of the 31 studies included, 14 studies (267 patients) had patients who underwent open stabilization, 11 studies (152 patients) had patients who underwent arthroscopic stabilization, and 6 studies (129 patients) had patients who underwent arthroscopic–assisted stabilization. The pooled rate of return to any level of sport was 97.6% (95% CI 94.8–99.5%, I2 = 32%). In addition, the pooled rate of return to the preinjury level was 79.1% (95% CI 70–87.1%, I2 = 78%). Moreover, the pooled rate of return to sport rate at the competitive level was 86.9% (95% CI 77.3–94.5%, I2 = 64.3%), and the return to sport for overhead athletes was 89.4% (95% CI 82.5–95.1%, I2 = 59%). The overall return to sport after an arthroscopic procedure was 96.4% (95% CI 91.3–99.6%, I2 = 1%) and for an open procedure was 97.8% (95% CI 93.7–99.9%, I2 = 46%). All functional outcome scores showed improvement postoperatively and the most common complication was revision surgery for loose body removal (19 patients).
Conclusion
Surgical management of osteochondritis dissecans of the elbow resulted in a high rate of return to sport, including in competitive and overhead athletes. Similar rates of return to sport were noted across both open and arthroscopic procedures.
Level of evidence
Level IV.





Similar content being viewed by others
Abbreviations
- OCD:
-
Osteochondritis dissecans
- PRISMA:
-
Preferred reporting items for systematic reviews and meta-analyses
- OATS:
-
Osteochondral autograft transplantation
- MEPS:
-
Mayo elbow performance score
- DASH:
-
Disabilities of the arm, shoulder and hand
References
Arai Y, Hara K, Inoue H, Minami G, Kida Y, Fujiwara H, Kubo T (2019) Early Clinical results of arthroscopically assisted drilling via the radius in a distal-to-proximal direction for osteochondritis dissecans of the elbow. Orthop J Sports Med. https://doi.org/10.1177/2325967119868937
Bae DS, Ingall EM, Miller PE, Eisenberg K (2020) Early results of single-plug autologous osteochondral grafting for osteochondritis dissecans of the capitellum in adolescents. J Pediatr Orthop 40:78–85
Baumgarten TE, Andrews JR, Satterwhite YE (1998) The arthroscopic classification and treatment of osteochondritis dissecans of the capitellum. Am J Sports Med 26:520–523
van Bergen CJ, van den Ende KI, Ten Brinke B, Eygendaal D (2016) Osteochondritis dissecans of the capitellum in adolescents. World J Orthop 7:102–108
Bojanić I, Smoljanović T, Dokuzović S (2012) Osteochondritis dissecans of the elbow: excellent mid-term follow-up results in teenage athletes treated by arthroscopic debridement and microfracture. Croat Med J 53:40–47
Bradley JP, Petrie RS (2001) Osteochondritis dissecans of the humeral capitellum. Diagnosis and treatment. Clin Sports Med 20:565–590
Byrd JWT, Jones KS (2002) Arthroscopic surgery for isolated capitellar osteochondritis dissecans in adolescent baseball players: minimum three-year follow-up. Am J Sports Med 30:474–482
Churchill RW, Munoz J, Ahmad CS (2016) Osteochondritis dissecans of the elbow. Curr Rev Musculoskelet Med 9:232–239
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188
Edmonds EW, Polousky J (2013) A review of knowledge in osteochondritis dissecans: 123 years of minimal evolution from König to the ROCK Study Group. Clin Orthop 471:1118–1126
Freeman M, Tukey J (1950) Transformations related to the angular and the square root. Ann Math Stat 21:607–611
Funakoshi T, Momma D, Matsui Y, Kamishima T, Matsui Y, Kawamura D, Nagano Y, Iwasaki N (2018) Autologous osteochondral mosaicplasty for centrally and laterally located, advanced capitellar osteochondritis dissecans in teenage athletes: clinical outcomes, radiography, and magnetic resonance imaging findings. Am J Sports Med 46:1943–1951
Greiwe RM, Saifi C, Ahmad CS (2010) Pediatric sports elbow injuries. Clin Sports Med 29:677–703
Harada M, Ogino T, Takahara M, Ishigaki D, Kashiwa H, Kanauchi Y (2002) Fragment fixation with a bone graft and dynamic staples for osteochondritis dissecans of the humeral capitellum. J Shoulder Elb Surg 11:368–372
Hennrikus WP, Miller PE, Micheli LJ, Waters PM, Bae DS (2015) Internal fixation of unstable in situ osteochondritis dissecans lesions of the capitellum. J Pediatr Orthop 35:467–473
Higgins JPT, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Stat Med 21:1539–1558
Iwasaki N, Kato H, Ishikawa J, Masuko T, Funakoshi T, Minami A (2009) Autologous osteochondral mosaicplasty for osteochondritis dissecans of the elbow in teenage athletes. J Bone Joint Surg Am 91:2359–2366
Miller JJ (1978) The inverse of the Freeman-Tukey double arcsine transformation. Am Stat 32:138
Jones KJ, Wiesel BB, Sankar WN (2010) Arthroscopic management of osteochondritis dissecans of the capitellum: mid-term results in adolescent athletes. J Pediatr Orthop 30:8–13
Kida Y, Morihara T, Kotoura Y, Hojo T, Tachiiri H, Sukenari T, Iwata Y, Furukawa R, Oda R, Arai Y, Fujiwara H, Kubo T (2014) Prevalence and clinical characteristics of osteochondritis dissecans of the humeral capitellum among adolescent baseball players. Am J Sports Med 42:1963–1971
Kirsch JM, Thomas JR, Khan M, Townsend WA, Lawton JN, Bedi A (2017) Return to play after osteochondral autograft transplantation of the capitellum: a systematic review. Arthroscopy 33:1412–1420
Kiyoshige Y, Takagi M, Yuasa K, Hamasaki M (2000) Closed-wedge osteotomy for osteochondritis dissecans of the capitellum: a 7 to 12year follow-up. Am J Sports Med 28:534–537
Koehler SM, Walsh A, Lovy AJ, Pruzansky JS, Shukla DR, Hausman MR (2015) Outcomes of arthroscopic treatment of osteochondritis dissecans of the capitellum and description of the technique. J Shoulder Elbow Surg 24:1607–1612
Kosaka M, Nakase J, Takahashi R, Toratani T, Ohashi Y, Kitaoka K, Tsuchiya H (2013) Outcomes and Failure Factors in Surgical Treatment for Osteochondritis Dissecans of the Capitellum. J Pediatr Orthop 33:719–724
Kumar V, Bhatnagar N, Lodhi JS (2018) Grade I Osteochondritis Dissecans in a Young Professional Athlete. Indian J Orthop 52:344–352
Kuwahata Y, Inoue G (1998) Osteochondritis dissecans of the elbow managed by Herbert screw fixation. Orthopedics 21:449–451
Landis JR, Koch GG (1977) The Measurement of Observer Agreement for Categorical Data. Biometrics 33:159
Lewine EB, Miller PE, Micheli LJ, Waters PM, Bae DS (2016) Early Results of Drilling and/or Microfracture for Grade IV Osteochondritis Dissecans of the Capitellum. J Pediatr Orthop 36:803–809
Logli AL, Bernard CD, O’Driscoll SW, Sanchez-Sotelo J, Morrey ME, Krych AJ, Camp CL (2019) Osteochondritis dissecans lesions of the capitellum in overhead athletes: a review of current evidence and proposed treatment algorithm. Curr Rev Musculoskelet Med 12:1–12
Lu Y, Li YJ, Guo SY, Zhang HL (2018) Is there any difference between open and arthroscopic treatment for osteochondritis dissecans (OCD) of the humeral capitellum: a systematic review and meta-analysis. Int Orthop 42:601–607
Lyons ML, Werner BC, Gluck JS, Freilich AM, Dacus AR, Diduch DR, Chhabra AB (2015) Osteochondral autograft plug transfer for treatment of osteochondritis dissecans of the capitellum in adolescent athletes. J Shoulder Elbow Surg 24:1098–1105
Maruyama M, Harada M, Satake H, Uno T, Takagi M, Takahara M (2016) Bone-peg grafting for osteochondritis dissecans of the humeral capitellum. J Orthop Surg 24:51–56
Maruyama M, Takahara M, Harada M, Satake H, Takagi M (2014) Outcomes of an open autologous osteochondral plug graft for capitellar osteochondritis dissecans: time to return to sports. Am J Sports Med 42:2122–2127
Matsuura T, Iwame T, Iwase J, Sairyo K (2020) Osteochondritis dissecans of the capitellum: review of the literature. J Med Investig 67:217–221
Matsuura T, Iwame T, Suzue N, Kashiwaguchi S, Iwase T, Hamada D, Sairyo K (2020) Long-term outcomes of arthroscopic debridement with or without drilling for osteochondritis dissecans of the capitellum in adolescent baseball players: a ≥10-year follow-up study. Arthroscopy 36:1273–1280
Matsuura T, Suzue N, Iwame T, Nishio S, Sairyo K (2014) Prevalence of osteochondritis dissecans of the capitellum in young baseball players: results based on ultrasonographic findings. Orthop J Sports Med. https://doi.org/10.1177/2325967114545298
Mihara K, Tsutsui H, Nishinaka N, Yamaguchi K (2009) Nonoperative treatment for osteochondritis dissecans of the capitellum. Am J Sports Med 37:298–304
Mihata T, Quigley R, Robicheaux G, McGarry MH, Neo M, Lee TQ (2013) Biomechanical characteristics of osteochondral defects of the humeral capitellum. Am J Sports Med 41:1909–1914
Mirzayan R, Lim MJ (2016) Fresh osteochondral allograft transplantation for osteochondritis dissecans of the capitellum in baseball players. J Shoulder Elbow Surg 25:1839–1847
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA (2015) Preferred Reporting Items for Systematic Review and Meta-Analysis Protocols (PRISMA-P) 2015 statement. Syst Rev 4:1
Nishinaka N, Tsutsui H, Yamaguchi K, Uehara T, Nagai S, Atsumi T (2014) Costal osteochondral autograft for reconstruction of advanced-stage osteochondritis dissecans of the capitellum. J Shoulder Elbow Surg 23:1888–1897
Nissen CW (2014) Osteochondritis dissecans of the elbow. Clin Sports Med 33:251–265
Nobuta S, Ogawa K, Sato K, Nakagawa T, Hatori M, Itoi E (2008) Clinical outcome of fragment fixation for osteochondritis dissecans of the elbow. Ups J Med Sci 113:201–208
Oshiba H, Itsubo T, Ikegami S, Nakamura K, Uchiyama S, Kato H (2016) Results of bone peg grafting for capitellar osteochondritis dissecans in adolescent baseball players. Am J Sports Med 44:3171–3178
Otoshi K, Kikuchi S, Kato K, Sato R, Igari T, Kaga T, Konno S (2017) Age-specific prevalence and clinical characteristics of humeral medial epicondyle apophysitis and osteochondritis dissecans: ultrasonographic assessment of 4249 players. Orthop J Sports Med. https://doi.org/10.1177/2325967117707703
Sato K, Iwamoto T, Matsumura N, Suzuki T, Nishiwaki Y, Oka Y, Nakamura T (2018) Costal osteochondral autograft for advanced osteochondritis dissecans of the humeral capitellum in adolescent and young adult athletes: clinical outcomes with a mean follow-up of 4.8 years. J Bone Joint Surg Am 100:903–913
Shah A, Kay J, Memon M, Coughlin RP, Simunovic N, Nho SJ, Ayeni OR (2019) What makes suture anchor use safe in hip arthroscopy? A systematic review of techniques and safety profile. Arthroscopy 35:1280–1293
Shimada K, Temporin K, Oura K, Tanaka H, Noguchi R (2017) Anconeus muscle-pedicle bone graft with periosteal coverage for osteochondritis dissecans of the humeral capitellum. Orthop J Sports Med. https://doi.org/10.1177/2325967117727531s
Shimada K, Yoshida T, Nakata K, Hamada M, Akita S (2005) Reconstruction with an osteochondral autograft for advanced osteochondritis dissecans of the elbow. Clin Orthop Relat Res 435:140–147
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (Minors): development and validation of a new instrument. ANZ J Surg 73:712–716
Takahara M, Mura N, Sasaki J, Harada M, Ogino T (2007) Classification, treatment, and outcome of osteochondritis dissecans of the humeral capitellum. J Bone Joint Surg Am 89:1205–1214
Takeba J (2015) Short-term clinical results of arthroscopic osteochondral fixation for elbow osteochondritis dissecans in teenaged baseball players. J Shoulder Elbow Surg 24:1749–1756
Takeda H, Watarai K, Matsushita T (2002) A surgical treatment for unstable osteochondritis dissecans lesions of the humeral capitellum in adolescent baseball players. Am J Sports Med 30:713–717
Tivnon MC, Anzel SH, Waugh TR (1976) Surgical management of osteochondritis dissecans of the capitellum. Am J Sports Med 4:121–128
Uchida S, Utsunomiya H, Taketa T, Sakoda S, Hatakeyama A, Nakamura T, Sakai A (2015) Arthroscopic fragment fixation using hydroxyapatite/poly-L-lactate acid thread pins for treating elbow osteochondritis dissecans. Am J Sports Med 43:1057–1065
Westermann RW, Hancock KJ, Buckwalter JA, Kopp B, Glass N, Wolf BR (2016) Return to sport after operative management of osteochondritis dissecans of the capitellum: a systematic review and meta-analysis. Orthop J Sports Med. https://doi.org/10.1177/2325967116654651
Wulf CA, Stone RM, Giveans MR, Lervick GN (2012) Magnetic resonance imaging after arthroscopic microfracture of capitellar osteochondritis dissecans. Am J Sports Med 40:2549–2556
Yamamoto Y, Ishibashi Y, Tsuda E, Sato H, Toh S (2006) Osteochondral autograft transplantation for osteochondritis dissecans of the elbow in juvenile baseball players: minimum 2-year follow-up. Am J Sports Med 34:714–720
Funding
No funding was provided for this study.
Author information
Authors and Affiliations
Contributions
DC participated in the design of the study, carried out the systematic review, extracted data, provided illustrations, and drafted the manuscript. JK carried out the systematic review, extracted data, completed the statistical analysis and revised the manuscript. Authors MM and DSE participated in the study design and participated in drafting and revising the manuscript. OA conceived of the study and participated in the revision of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
This study does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix Table 1: Search strategy
Appendix Table 1: Search strategy
Medline: 1548 Studies | Embase: 2725 Studies | PubMed: 2031 Studies | |||
|---|---|---|---|---|---|
Strategy | Studies | Strategy | Studies | Strategy | Studies |
1. Osteochondritis Dissecans.mp. or Osteochondritis Dissecans/ | 2394 | 1. Osteochondritis Dissecans.mp. or Osteochondritis Dissecans/ | 3083 | 1. Osteochondritis Dissecans | 2,509 |
2. Ocd.mp. | 9747 | 2. Ocd.mp. | 14,311 | 2. OCD | 9,880 |
3. Sport.mp. or Sports/ | 56,145 | 3. Sport.mp. or Sports/ | 101,408 | 3. Sport | 336,590 |
4. Return to sport/ or return.mp. | 110,778 | 4. Return to Sport/ or return.mp. | 154,089 | 4. Return | 243,648 |
5. Play.mp. | 684,089 | 5. Play.mp. | 857,945 | 5. Play | 687,583 |
6. Activit*.mp. | 3,274,092 | 6. Activit*.mp. | 4,510,279 | 6. Activit* | 3,197,198 |
7. 1 or 2 | 11,588 | 7. 1 or 2 | 16,721 | 7. 1 or 2 | 11,833 |
8. 3 or 4 or 5 or 6 | 3,938,868 | 8. 3 or 4 or 5 or 6 | 5,347,517 | 8. 3 or 4 or 5 or 6 | 4,172,423 |
9. 7 and 8 | 1548 | 9. 7 and 8 | 2725 | 9. 7 and 8 | 2,031 |
Rights and permissions
About this article
Cite this article
Cohen, D., Kay, J., Memon, M. et al. A high rate of children and adolescents return to sport after surgical treatment of osteochondritis dissecans of the elbow: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc 29, 4041–4066 (2021). https://doi.org/10.1007/s00167-021-06489-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06489-9