Abstract
Purpose
To examine whether increased lateral femoral condyle ratio (LFCR) correlates with increased risk of Anterior cruciate ligament (ACL) injury (1) and to evaluate the relationship between the LFCR and anterolateral complex (ALC) injury in non-contact ACL torn knees (2).
Methods
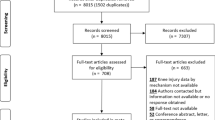
Six hundred and seventy-two patients who underwent ACL reconstruction surgery between 2013 and 2019 were retrospectively reviewed, and 120 patients were finally included in the study. Forty patients (ACL + ALC injury) were included in the study group, while forty patients with isolated ACL injury (isolated ACL injury group) and 40 patients who suffered from meniscal tear without ACL or ALC injury were matched in a 1:1 fashion by age, sex, and BMI to the study group (ACL + ALC injury). The LFCR was measured on standard lateral radiographs in a blinded fashion. The differences between the three groups were analyzed by ANOVA. A ROC (Receiver Operating Characteristic) curve was produced to determine risk of ACL injury and risk of concomitant ALC injury in non-contact ACL injury.
Results
The mean LFCR was 71.9% ± 3.1% in the ACL + ALC injury group, 68.4% ± 3.2% in the isolated ACL injury group, and 66.8% ± 2.6% in the control group (patients who suffered from meniscal tear without ACL or ALC injury). Significantly greater LFCR was found in the ACL + ALC injury group than that in the isolated ACL injury group (p < 0.017). Greater LFCR was additionally confirmed in the ACL injury group as compared to the control group (p < 0.05). ROC curve analysis demonstrated that LFCR > 68.3% was predictive for an increased risk of ACL injury in the entire cohort. LFCR > 69.4% was predictive for an increased risk of ALC injury in non-contact ACL ruptured patients.
Conclusion
Increased LFCR was found to be associated with greater risk of ALC injury in non-contact ACL ruptured patients. Additionally, increased LFCR was further confirmed to be correlated with increased risk of ACL injury in an Asian population. The data from this study may help recognize patients undergoing ACL reconstruction that could benefit from additional extra-articular tenodesis.
Level of evidence
III.






Similar content being viewed by others
References
Boden BP, Dean GS, Feagin JA Jr, Garrett WE Jr (2000) Mechanisms of anterior cruciate ligament injury. Orthopedics 23(6):573–578
Hewett TE, Myer GD, Ford KR, Heidt RS Jr, Colosimo AJ, McLean SG, van den Bogert AJ, Paterno MV, Succop P (2005) Biomechanical measures of neuromuscular control and valgus loading of the knee predict anterior cruciate ligament injury risk in female athletes: a prospective study. Am J Sports Med 33(4):492–501
Hofbauer M, Thorhauer ED, Abebe E, Bey M, Tashman S (2014) Altered tibiofemoral kinematics in the affected knee and compensatory changes in the contralateral knee after anterior cruciate ligament reconstruction. Am J Sports Med 42(11):2715–2721
Quatman CE, Hewett TE (2009) The anterior cruciate ligament injury controversy: is “valgus collapse” a sex-specific mechanism? Br J Sports Med 43(5):328–335
Salmon L, Russell V, Musgrove T, Pinczewski L, Refshauge K (2005) Incidence and risk factors for graft rupture and contralateral rupture after anterior cruciate ligament reconstruction. Arthroscopy 21(8):948–957
Solomonow M, Baratta R, Zhou BH, Shoji H, Bose W, Beck C, D’Ambrosia R (1987) The synergistic action of the anterior cruciate ligament and thigh muscles in maintaining joint stability. Am J Sports Med 15(3):207–213
Uhorchak JM, Scoville CR, Williams GN, Arciero RA, St Pierre P, Taylor DC (2003) Risk factors associated with noncontact injury of the anterior cruciate ligament: a prospective four-year evaluation of 859 West Point cadets. Am J Sports Med 31(6):831–842
LaPrade RF, Burnett QM 2nd (1994) Femoral intercondylar notch stenosis and correlation to anterior cruciate ligament injuries. A prospective study. Am J Sports Med 22(2):198–203
Pfeiffer TR, Burnham JM, Hughes JD, Kanakamedala AC, Herbst E, Popchak A, Shafizadeh S, Irrgang JJ, Debski RE, Musahl V (2018) An increased lateral femoral condyle ratio is a risk factor for anterior cruciate ligament injury. J Bone Jt Surg Am 100(10):857–864
Hewett TE, Ford KR, Hoogenboom BJ, Myer GD (2010) Understanding and preventing acl injuries: current biomechanical and epidemiologic considerations—update 2010. N Am J Sports Phys Ther 5(4):234–251
Cavaignac E, Ancelin D, Chiron P, Tricoire JL, Wytrykowski K, Faruch M, Chantalat E (2017a) Historical perspective on the “discovery” of the anterolateral ligament of the knee. Knee Surg Sports Traumatol Arthrosc 25(4):991–996
Claes S, Vereecke E, Maes M, Victor J, Verdonk P, Bellemans J (2013) Anatomy of the anterolateral ligament of the knee. J Anat 223(4):321–328
Geeslin AG, Chahla J, Moatshe G, Muckenhirn KJ, Kruckeberg BM, Brady AW, Coggins A, Dornan GJ, Getgood AM, Godin JA et al (2018) Anterolateral knee extra-articular stabilizers: a robotic sectioning study of the anterolateral ligament and distal iliotibial band kaplan fibers. Am J Sports Med 46(6):1352–1361
Kennedy MI, LaPrade CM, Geeslin AG, LaPrade RF (2018) An overview of clinically relevant biomechanics of the anterolateral structures of the knee. Tech Orthop 33(4):213–218
Rasmussen MT, Nitri M, Williams BT, Moulton SG, Cruz RS, Dornan GJ, Goldsmith MT, LaPrade RF (2016) An in vitro robotic assessment of the anterolateral ligament, part 1: secondary role of the anterolateral ligament in the setting of an anterior cruciate ligament injury. Am J Sports Med 44(3):585–592
Kennedy MI, Claes S, Fuso FA, Williams BT, Goldsmith MT, Turnbull TL, Wijdicks CA, LaPrade RF (2015) The anterolateral ligament: an anatomic, radiographic, and biomechanical. Analysis 43(7):1606–1615
Terry GC, LaPrade RF (1996) The biceps femoris muscle complex at the knee. Its anatomy and injury patterns associated with acute anterolateral-anteromedial rotatory instability. Am J Sports Med 24(1):2–8
Kim SY, Spritzer CE, Utturkar GM, Toth AP, Garrett WE, DeFrate LE (2015) Knee kinematics during noncontact anterior cruciate ligament injury as determined from bone bruise location. Am J Sports Med 43(10):2515–2521
Papalia R, Torre G, Vasta S, Zampogna B, Pedersen DR, Denaro V, Amendola A (2015) Bone bruises in anterior cruciate ligament injured knee and long-term outcomes. A review of the evidence. Open Access J Sports Med 6:37–48
Caterine S, Litchfield R, Johnson M, Chronik B, Getgood A (2015) A cadaveric study of the anterolateral ligament: re-introducing the lateral capsular ligament. Knee Surg Sports Traumatol Arthrosc 23(11):3186–3195
Getgood A, Brown C, Lording T, Amis A, Claes S, Geeslin A, Musahl V (2019) The anterolateral complex of the knee: results from the International ALC Consensus Group Meeting. Knee Surg Sports Traumatol Arthrosc 27(1):166–176
Parsons EM, Gee AO, Spiekerman C, Cavanagh PR (2015) The biomechanical function of the anterolateral ligament of the knee. Am J Sports Med 43(3):669–674
Terry GC, Norwood LA, Hughston JC, Caldwell KM (1993) How iliotibial tract injuries of the knee combine with acute anterior cruciate ligament tears to influence abnormal anterior tibial displacement. Am J Sports Med 21(1):55–60
Dodds AL, Halewood C, Gupte CM, Williams A, Amis AA (2014) The anterolateral ligament: anatomy, length changes and association with the Segond fracture. Bone Jt J 96-B(3):325–331
Monaco E, Ferretti A, Labianca L, Maestri B, Speranza A, Kelly MJ, D’Arrigo C (2012) Navigated knee kinematics after cutting of the ACL and its secondary restraint. Knee Surg Sports Traumatol Arthrosc 20(5):870–877
Thein R, Boorman-Padgett J, Stone K, Wickiewicz TL, Imhauser CW, Pearle AD (2016) Biomechanical assessment of the anterolateral ligament of the knee: a secondary restraint in simulated tests of the pivot shift and of anterior stability. J Bone Jt Surg Am 98(11):937–943
Cavaignac E, Li K, Faruch M, Savall F, Chiron P, Huang W, Telmon N (2017b) Three-dimensional geometric morphometric analysis reveals ethnic dimorphism in the shape of the femur. J Exp Orthop 4(1):13
Cavaignac E, Savall F, Faruch M, Reina N, Chiron P, Telmon N (2016) Geometric morphometric analysis reveals sexual dimorphism in the distal femur. Forensic Sci Int 259:246.e241–245
Li K, Cavaignac E, Xu W, Cheng Q, Telmon N, Huang W (2018) Morphometric evaluation of the knee in Chinese population reveals sexual dimorphism and age-related differences. Int Orthop 42(10):2349–2356
Agel J, Arendt EA, Bershadsky B (2005) Anterior cruciate ligament injury in national collegiate athletic association basketball and soccer: a 13-year review. Am J Sports Med 33(4):524–530
Arendt E, Dick R (1995) Knee injury patterns among men and women in collegiate basketball and soccer. NCAA data and review of literature. Am J Sports Med 23(6):694–701
Harmon KG, Ireland ML (2000) Gender differences in noncontact anterior cruciate ligament injuries. Clin Sports Med 19(2):287–302
Claes S, Bartholomeeusen S, Bellemans J (2014) High prevalence of anterolateral ligament abnormalities in magnetic resonance images of anterior cruciate ligament-injured knees. Acta Orthop Belg 80(1):45–49
Helito CP, Demange MK, Helito PV, Costa HP, Bonadio MB, Pecora JR, Rodrigues MB, Camanho GL (2015) Evaluation of the anterolateral ligament of the knee by means of magnetic resonance examination. Rev Bras Ortop 50(2):214–219
Helito CP, Helito PV, Costa HP, Bordalo-Rodrigues M, Pecora JR, Camanho GL, Demange MK (2014) MRI evaluation of the anterolateral ligament of the knee: assessment in routine 1.5-T scans. Skeletal Radiol 43(10):1421–1427
Kosy JD, Mandalia VI, Anaspure R (2015) Characterization of the anatomy of the anterolateral ligament of the knee using magnetic resonance imaging. Skeletal Radiol 44(11):1647–1653
Acknowledgements
The work is supported by grants from the National Natural Science Foundation of China (NO.81902293) (K.L).
Funding
This study was supported by Young Scientists Fund Grand No (81902293).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have declared that no competing interests exist.
Ethical approval
This study was approved by the institutional review board of the First Affiliated Hospital of Chongqing Medical University (IRB approval number: 2016-94).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This work was performed in Department of Orthopaedic Surgery, The First Affiliated Hospital of Chongqing Medical University.
Rights and permissions
About this article
Cite this article
Li, K., Zheng, X., Li, J. et al. Increased lateral femoral condyle ratio is associated with greater risk of ALC injury in non-contact anterior cruciate ligament injury. Knee Surg Sports Traumatol Arthrosc 29, 3077–3084 (2021). https://doi.org/10.1007/s00167-020-06347-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-06347-0