Abstract
Purpose
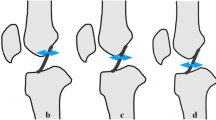
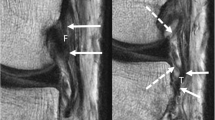
To assess the reliability and predictive value of quantifying anterior cruciate ligament (ACL) tear location on magnetic resonance imaging (MRI) and assess the predictive value of tear location on the eligibility for arthroscopic primary repair of proximal ACL tears.
Methods
In this case–control study, all adult patients undergoing acute ACL surgery between 2008 and 2020 were retrospectively reviewed. All patients were treated with the treatment algorithm of undergoing primary repair when proximal tears with sufficient tissue quality were present intraoperatively, and otherwise underwent single-bundle ACL reconstruction. Sagittal MRI images were reviewed to measure proximal and distal remnant lengths along the anterior aspect of the torn ligament, and tear location was calculated as distal remnant divided by total remnant length. Interobserver and intraobserver reliability for remnant measurements were calculated. Then, receiver operating curve analysis (ROC) was performed to calculate the optimal cut-off for the possibility of primary repair with the different measurements.
Results
Two hundred and forty-eight patients were included, of which 151 underwent repair (61%). Inter- and intraobserver reliability ranged between 0.92 and 0.96 [95% confidence interval (CI) 0.55–0.98] and 0.91–0.97 (95% CI 0.78–0.98, respectively). All patients with a tear location of ≥ 80% on MRI could undergo repair, whereas all patients with tear location of < 60% required reconstruction. The positive predictive value of a proximal quarter tear (≥ 75%) on primary repair was 94%. Older age was correlated with more proximal tear location (p < 0.001), but there was no correlation between tear location and gender, BMI, or timing of surgery (all n.s).
Conclusion
This study showed that tear location could reliably be quantified on MRI by assessing distal and proximal remnant lengths. Tear location in the proximal quarter of the ACL was found to have a positive predictive value for repairability of 94%. These findings may assist orthopaedic surgeons in evaluating which patients are eligible for primary ACL repair preoperatively.
Level of evidence
III.




Similar content being viewed by others
References
Collins JE, Katz JN, Donnell-Fink LA et al (2013) Cumulative incidence of ACL reconstruction after ACL injury in adults: role of age, sex, and race. Am J Sports Med 41:544–549
Weaver J, Derkash R, Freeman J et al (1985) Primary knee ligament repair-revisited. ClinOrthopRelat Res 199:185–191
Feagin JACW Jr (1976) Isolated tear of the anterior cruciate ligament: 5-year follow-up study. Am J Sports Med 4:95–100
Chambat P, Guier C, Sonnery-Cottet B et al (2013) The evolution of ACL reconstruction over the last fifty years. Int Orthop 37:181–186
Kamath GV, Murphy T, Creighton RA et al (2014) Anterior cruciate ligament injury, return to play, and reinjury in the elite collegiate athlete. Am J Sports Med 42:1638–1643
Sanders TL, Kremers HM, Bryan AJ et al (2016) Is anterior cruciate ligament reconstruction effective in preventing secondary meniscal tears and osteoarthritis? Am J Sports Med 44:1699–1707. https://doi.org/10.1177/0363546516634325
Hoogeslag RAG, Brouwer RW, Boer BC et al (2019) Acute anterior cruciate ligament rupture: repair or reconstruction? Two-year results of a randomized controlled clinical trial. Am J Sport Med 47:567–577
Jonkergouw A, van der List JP, DiFelice GS (2019) Arthroscopic primary repair of proximal anterior cruciate ligament tears: outcomes of the first 56 consecutive patients and the role of additional internal bracing. Knee Surg Sport TraumatolArthrosc 27:21–28
Kösters C, Glasbrenner J, Spickermann L et al (2020) Repair with dynamic intraligamentary stabilization versus primary reconstruction of acute anterior cruciate ligament tears: 2-year results from a prospective randomized study. Am J Sports Med 48:1108–1116
Murray MM, Kalish LA, Fleming BC et al (2019) Bridge-enhanced anterior cruciate ligament repair: two-year results of a first-in-human study. Orthop J Sport Med 7:232596711882435
van der List JP, Vermeijden HD, Sierevelt IN et al (2019) Arthroscopic primary repair of proximal anterior cruciate ligament tears seems safe but higher level of evidence is needed: a systematic review and meta-analysis of recent literature. Knee Surg Sport TraumatolArthrosc 28:1946–1957
Hoogeslag RAG, Brouwer RW, de Vries AJ et al (2020) Efficacy of nonaugmented, static augmented, and dynamic augmented suture repair of the ruptured anterior cruciate ligament: a systematic review of the literature. Am J Sports Med. https://doi.org/10.1177/0363546520904690
Henle P, Bieri KS, Brand M et al (2018) Patient and surgical characteristics that affect revision risk in dynamic intraligamentary stabilization of the anterior cruciate ligament. Knee Surg Sport TraumatolArthrosc 26:1182–1189
van der List JP, Jonkergouw A, van Noort A et al (2019) Identifying candidates for arthroscopic primary repair of the anterior cruciate ligament: a case-control study. Knee 23:619–627
Goiney CC, Porrino J, Twaddle B et al (2016) The value of accurate magnetic resonance characterization of posterior cruciate ligament tears in the setting of multiligament knee injury: imaging features predictive of early repair vs reconstruction. CurrProblDiagnRadiol 45:10–16
van der List JP, Mintz DN, DiFelice GS (2017) The location of anterior cruciate ligament tears: a prevalence study using magnetic resonance imaging. Orthop J Sport Med 5
Nwachukwu BU, Patel BH, Lu Y et al (2019) Anterior cruciate ligament repair outcomes: an updated systematic review of recent literature. Arthroscopy 35:2233–2247
Nguyen DTT, Ramwadhdoebe THH, van der Hart CPP et al (2014) Intrinsic healing response of the human anterior cruciate ligament: an histological study of reattached ACL remnants. J Orthop Res 32:296–301
Toy B, Yeasting RA, Morse DE, McCann P (1995) Arterial supply to the human anterior cruciate ligament. J Athl Train 30:149–152
Achtnich A, Herbst E, Forkel P et al (2016) Acute proximal anterior cruciate ligament tears: outcomes after arthroscopic suture anchor repair versus anatomic single-bundle reconstruction. Arthroscopy 32:2562–2569
Sherman MF, Lieber L, Bonamo JR et al (1991) The long-term followup of primary anterior cruciate ligament repair. Am J Sports Med 19:243–255
van der List JP, Mintz DN, DiFelice GS (2017) The location of anterior cruciate ligament tears: a prevalence study using magnetic resonance imaging. Orthop J Sport Med 5:2325967117709966
Narvekar A, Gajjar S (2004) Mucoid degeneration of the anterior cruciate ligament. Arthroscopy 20:141–146
Magarian EM, Fleming BC, Harrison SL et al (2010) Delay of 2 or 6 weeks adversely affects the functional outcome of augmented primary repair of the porcine anterior cruciate ligament. Am J Sport Med 38:2528–2534
Lo IKY, De Maat GHR, Valk JW, Frank CB (1999) The gross morphology of torn human anterior cruciate ligaments in unstable knees. Arthroscopy 15:301–306
Gagliardi AG, Carry PM, Parikh HB et al (2019) ACL repair with suture ligament augmentation is associated with a high failure rate among adolescent patients. Am J Sports Med 47:560–566
Funding
No funding was received to perform this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
GSD declares he is a paid consultant and receives research grants from Arthrex (Naples, FL, USA). GK declares that the Department of Orthopedic Surgery of the Amsterdam University Medical Centers received an unrestricted research Grant from Arthrex (Naples, FL, USA).
Ethics approval
This study was approved by the Institutional Review Board of Hospital for Special Surgery, New York, NY, USA.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Vermeijden, H.D., Cerniglia, B., Mintz, D.N. et al. Distal remnant length can be measured reliably and predicts primary repair of proximal anterior cruciate ligament tears. Knee Surg Sports Traumatol Arthrosc 29, 2967–2975 (2021). https://doi.org/10.1007/s00167-020-06312-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-06312-x