Abstract
Purpose
To compare the occurrence of short-term postoperative complications between inpatient and outpatient anterior cruciate ligament reconstruction.
Methods
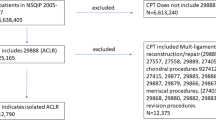
The ACS National Surgical Quality Improvement Program (NSQIP) database was utilized to identify patients undergoing arthroscopic anterior cruciate ligament reconstruction (ACLR) from 2007 to 2017. A total of 18,052 patients were available for analysis following application of exclusion criteria. Patients were categorized based on location of surgery. Inpatients and outpatient ACLR groups were matched by demographics and preoperative laboratory values and differences in 30-day complication rates following surgery were assessed. Significance was set with alpha < 0.05.
Results
From 2007 to 2017, there was an increasing frequency for outpatient ACLR (p < 0.001), while the incidence of inpatient ACLR remained largely constant (n.s). Groups were matched to include 1818 patients in each cohort. Within the first 30 days of surgery, patients in the inpatient ACLR group experienced significantly greater rates of superficial incisional SSI (0.6% vs 0.1%, p = 0.026) and composite surgical complications (0.6% vs 0.2%, p = 0.019), as well as a greater rate of reoperation (0.7% vs 0.2%, p = 0.029). Inpatient procedures also demonstrated a greater rate of deep surgical incisional SSI (0.2% vs 0.0%, n.s) and readmission to hospital (0.8% vs 0.7%, n.s).Outpatient ACLR procedures were also associated with a significantly greater relative value unit (RVU)/h compared with inpatient ACLRs (0.17 vs 0.14, p < 0.001).
Conclusions
Inpatient ACLR may have an increased risk of postoperative complications compared to outpatient ACLR during the short-term postoperative period. Although some patients may require admission post-operatively for medical and/or pain management, doing so is not necessarily without a degree of risk.
Level of evidence
III.


Similar content being viewed by others
References
Abeles A, Kwasnicki RM, Pettengell C, Murphy J, Darzi A (2017) The relationship between physical activity and post-operative length of hospital stay: a systematic review. Int J Surg 44:295–302
Andres F (1989) Contributions by Brown-Sequard on spinal cord trauma and pathology. Brain Res Bull 22:3–5
Basques BA, Erickson BJ, Leroux T, Griffin JW, Frank RM, Verma NN et al (2017) Comparative outcomes of outpatient and inpatient total shoulder arthroplasty: an analysis of the Medicare dataset. Bone Jt J 99:934–938
Cattanach N, Sheedy R, Gill S, Hughes A (2014) Physical activity levels and patients' expectations of physical activity during acute general medical admission. Intern Med J 44:501–504
Crawford DC, Li CS, Sprague S, Bhandari M (2015) Clinical and cost implications of inpatient versus outpatient orthopedic surgeries: a systematic review of the published literature. Orthop Rev (Pavia) 7:6177–6177
Davenport SJ, Arnold M, Hua C, Schenck A, Batten S, Taylor NF (2015) Physical activity levels during acute inpatient admission after hip fracture are very low. Physiother Res Int 20:174–181
De Klein K, Valkenet K, Veenhof C (2019) Perspectives of patients and health-care professionals on physical activity of hospitalized patients. Physiother Theory Pract. https://doi.org/10.1080/09593985.2019.16265171-8
Dobing S, Frolova N, McAlister F, Ringrose J (2016) Sleep quality and factors influencing self-reported sleep duration and quality in the general internal medicine inpatient population. PLoS ONE 11:e0156735
Ferrari D, Lopes TJ, Franca PF, Azevedo FM, Pappas E (2017) Outpatient versus inpatient anterior cruciate ligament reconstruction: a systematic review with meta-analysis. Knee 24:197–206
Goh J, Ladiges WC (2014) Exercise enhances wound healing and prevents cancer progression during aging by targeting macrophage polarity. Mech Ageing Dev 139:41–48
Grant MC, Yang D, Wu CL, Makary MA, Wick EC (2017) Impact of enhanced recovery after surgery and fast track surgery pathways on healthcare-associated infections: results from a systematic review and meta-analysis. Ann Surg 265:68–79
Hsiao WC, Braun P, Dunn DL, Becker ER, Yntema D, Verrilli DK et al (1992) An overview of the development and refinement of the Resource-Based Relative Value Scale. The foundation for reform of U.S. physician payment. Med Care 30:Ns1–12
Huisman TH (1987) High-performance liquid chromatography as a method to identify haemoglobin abnormalities. Acta Haematol 78:123–126
Huntley SR, McGee AS, Johnson JL, Debell HA, McKissack HM, McGwin G et al (2019) Outcomes of inpatient versus outpatient elective foot and ankle surgery. Cureus 11:e4058
Kadhim M, Gans I, Baldwin K, Flynn J, Ganley T (2016) Do surgical times and efficiency differ between inpatient and ambulatory surgery centers that are both hospital owned? J Pediatr Orthop 36:423–428
Kakupa DK, Muenze PK, Byl B, Wilmet MD (2016) Study of the prevalence of nosocomial infections and associated factors in the two university hospitals of Lubumbashi, Democratic Republic of Congo. Pan Afr Med J 24:275
Kao JT, Giangarra CE, Singer G, Martin S (1995) A comparison of outpatient and inpatient anterior cruciate ligament reconstruction surgery. Arthroscopy 11:151–156
Keylock T, Meserve L, Wolfe A (2018) Low-intensity exercise accelerates wound healing in diabetic mice. Wounds 30:68–71
Khanna R, Kim RB, Lam SK, Cybulski GR, Smith ZA, Dahdaleh NS (2018) Comparing short-term complications of inpatient versus outpatient single-level anterior cervical discectomy and fusion: an analysis of 6940 patients using the ACS-NSQIP database. Clin Spine Surg 31:43–47
Ko CY, Hall BL, Hart AJ, Cohen ME, Hoyt DB (2015) The American College of Surgeons National Surgical Quality Improvement Program: achieving better and safer surgery. Jt Comm J Qual Patient Saf 41:199–204
Krywulak SA, Mohtadi NG, Russell ML, Sasyniuk TM (2005) Patient satisfaction with inpatient versus outpatient reconstruction of the anterior cruciate ligament: a randomized clinical trial. Can J Surg 48:201–206
Lefevre N, Klouche S, Doumbouya N, Chambaz M, Devaux C, Thomas R et al (2014) Hospitalisation en court séjour pour reconstruction du ligament croisé antérieur : étude prospective comparative. J Traumatol Sport 31:71–75
Li G, Weng J, Xu C, Wang D, Xiong A, Zeng H (2019) Factors associated with the length of stay in total knee arthroplasty patients with the enhanced recovery after surgery model. J Orthop Surg Res 14:343
Lunebourg A, Ollivier M, Delahaye D, Argenson JA, Parratte S (2016) Better satisfaction of patients operated on anterior cruciate ligament reconstruction in outpatient setting. A prospective comparative monocentric study of 60 cases. Arch Orthop Trauma Surg 136:1709–1715
Marshall L, Born J (2002) Brain–immune interactions in sleep. Int Rev Neurobiol 52:93–131
McClelland S 3rd, Passias PG, Errico TJ, Bess RS, Protopsaltis TS (2017) Inpatient versus outpatient anterior cervical discectomy and fusion: a perioperative complication analysis of 259,414 patients from the healthcare cost and utilization project databases. Int J Spine Surg 11:11
Mostaghimi L, Obermeyer WH, Ballamudi B, Martinez-Gonzalez D, Benca RM (2005) Effects of sleep deprivation on wound healing. J Sleep Res 14:213–219
Mulligan RP, Parekh SG (2017) Safety of outpatient total ankle arthroplasty vs traditional inpatient admission or overnight observation. Foot Ankle Int 38:825–831
Novak PJ, Bach BR Jr, Bush-Joseph CA, Badrinath S (1996) Cost containment: a charge comparison of anterior cruciate ligament reconstruction. Arthroscopy 12:160–164
Patrick NC, Kowalski CA, Hennrikus WL (2017) Surgical efficiency of anterior cruciate ligament reconstruction in outpatient surgical center versus hospital operating room. Orthopedics 40:297–302
Qin C, Dekker RG, Blough JT, Kadakia AR (2016) Safety and outcomes of inpatient compared with outpatient surgical procedures for ankle fractures. J Bone Jt Surg Am 98:1699–1705
Raval MV, Sakran JV, Medbery RL, Angelos P, Hall BL (2014) Distinguishing QI projects from human subjects research: ethical and practical considerations. Bull Am Coll Surg 99:21–27
Saltzman BM, Cvetanovich GL, Nwachukwu BU, Mall NA, Bush-Joseph CA, Bach BR Jr (2016) Economic analyses in anterior cruciate ligament reconstruction: a qualitative and systematic review. Am J Sports Med 44:1329–1335
Scillia AJ, Issa K, Boylan MR, McDermott JD, McInerney VK, Patel DV et al (2016) Inpatient cruciate ligament reconstruction in the United States: a nationwide database study from 1998 to 2010. Orthopedics 39:e196–202
Tedder C, DeBell H, Dix D, Smith WR, McGwin G Jr, Shah A et al (2019) Comparative analysis of short-term postoperative complications in outpatient versus inpatient total ankle arthroplasty: a database study. J Foot Ankle Surg 58:23–26
Valkering KP, van Bergen CJ, Buijze GA, Nagel PH, Tuinebreijer WE, Breederveld RS (2015) Pain experience and functional outcome of inpatient versus outpatient anterior cruciate ligament reconstruction, an equivalence randomized controlled trial with 12 months follow-up. Knee 22:111–116
Weiser MC, Kim KY, Anoushiravani AA, Iorio R, Davidovitch RI (2018) Outpatient total hip arthroplasty has minimal short-term complications with the use of institutional protocols. J Arthroplasty 33:3502–3507
Whiting PS, Rice CD, Avilucea FR, Bulka CM, Shen MS, Obremskey WT et al (2017) Patients at increased risk of major adverse events following operative treatment of distal radius fractures: inpatient versus outpatient. J Wrist Surg 6:220–226
Funding
There was no outside source of funding utilized for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest statement.
Ethical approval
This was an IRB exempt study due to the use of deidentified data from a national outcomes database.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lu, Y., Lavoie-Gagne, O., Khazi, Z. et al. Inpatient admission following anterior cruciate ligament reconstruction is associated with higher postoperative complications. Knee Surg Sports Traumatol Arthrosc 28, 2486–2493 (2020). https://doi.org/10.1007/s00167-020-06094-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-06094-2