Abstract
Purpose
Local infiltration analgesia (LIA) has attracted growing interest in recent years. To prolong the positive effects of LIA, a continuous intraarticular perfusion has been introduced in total knee arthroplasty with good clinical results. The purpose of the present study was to evaluate if similar results can be obtained with the use of a continuous periarticular perfusion in unicondylar knee arthroplasty (UKA).
Methods
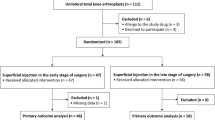
50 consecutively selected patients undergoing UKA received either a single-shot LIA (control group; n = 25) or single-shot LIA combined with a continuous postoperative periarticular perfusion for 2 postoperative days (intervention group, n = 25). VAS (visual analogue scale) for pain, pain medication consumption and range of flexion were recorded postoperatively for 6 days. The catheter was removed after 2 days.
Results
Only minor advantages of using a continuous periarticular catheter could be shown. Patients in the intervention group showed significant lower VAS scores on day 1 and required significant less pain medication on day 6. Further, there was a significant difference in the range of flexion on day 3, on which patients of the intervention group were able to bend the knee joint on average by 12° more than patients of the control group. On the other days, any significant differences between the two groups were not observed.
Conclusion
In summary, the present study could not identify any superiority of a periarticular catheter over single-shot LIA in UKA. Because of additional costs and the potential risk of infection, the conclusion of this study is to not recommend adding a periarticular catheter to the single-shot LIA in UKA.
Level of evidence
II



Similar content being viewed by others
Abbreviations
- UKA:
-
Unicondylar knee arthroplasty
- LIA:
-
Local infiltration analgesia
- VAS:
-
Visual analogue scale
- ROM:
-
Range of motion
- LMWHs:
-
Low-molecular-weight heparins
References
Ali A, Sundberg M, Hansson U, Malmvik J, Flivik G (2015) Doubtful effect of continuous intraarticular analgesia after total knee arthroplasty: a randomized double-blind study of 200 patients. Acta Orthop 86:373–377
Bakker SMK, Fenten MGE, Touw DJ, van den Bemt BJF, Heesterbeek PJC, Scheffer G-J, Stienstra R (2018) Pharmacokinetics of 400 mg locally infiltrated ropivacaine after total knee arthroplasty without perioperative tourniquet use. Reg Anesth Pain Med 43:699–704
Blendon RJ, Benson JM (2018) The public and the opioid-abuse epidemic. N Engl J Med 378:407–411
Busch CA, Shore BJ, Bhandari R, Ganapathy S, MacDonald SJ, Bourne RB, Rorabeck CH, McCalden RW (2006) Efficacy of periarticular multimodal drug injection in total knee arthroplasty. A randomized trial. J Bone Jt Surg Am 88:959–963
Dillon JP, Brennan L, Mitchell D (2012) Local infiltration analgesia in hip and knee arthroplasty: an emerging technique. Acta Orthop Belg 78:158–163
Essving P, Axelsson K, Åberg E, Spännar H, Gupta A, Lundin A (2011) Local infiltration analgesia versus intrathecal morphine for postoperative pain management after total knee arthroplasty: a randomized controlled trial. Anesth Analg 113:926–933
Fenten MGE, Bakker SMK, Touw DJ, van den Bemt BJF, Scheffer GJ, Heesterbeek PJC, Stienstra R (2017) Pharmacokinetics of 400 mg ropivacaine after periarticular local infiltration analgesia for total knee arthroplasty. Acta Anaesthesiol Scand 61:338–345
Gómez-Cardero P, Rodríguez-Merchán EC (2010) Postoperative analgesia in TKA: ropivacaine continuous intraarticular infusion. Clin Orthop 468:1242–1247
Horlocker TT (2010) Pain management in total joint arthroplasty: a historical review. Orthopedics 33:14–19
Kerr DR, Kohan L (2008) Local infiltration analgesia: a technique for the control of acute postoperative pain following knee and hip surgery: a case study of 325 patients. Acta Orthop 79:174–183
Knudsen K, Beckman Suurküla M, Blomberg S, Sjövall J, Edvardsson N (1997) Central nervous and cardiovascular effects of i.v. infusions of ropivacaine, bupivacaine and placebo in volunteers. Br J Anaesth 78:507–514
Manchikanti L, Helm S, Fellows B, Janata JW, Pampati V, Grider JS, Boswell MV (2012) Opioid epidemic in the United States. Pain Phys 15:ES9–38
Puolakka PAE, Rorarius MGF, Roviola M, Puolakka TJS, Nordhausen K, Lindgren L (2010) Persistent pain following knee arthroplasty. Eur J Anaesthesiol 27:455–460
Schwab P-E, Yombi J, Lavand’homme P, Thienpont E, (2019) Comparison of local infiltration analgesia with single injection femoral nerve block in total knee arthroplasty. Acta Orthop Belg 85:122–129
Toftdahl K, Nikolajsen L, Haraldsted V, Madsen F, Tønnesen EK, Søballe K (2007) Comparison of peri- and intraarticular analgesia with femoral nerve block after total knee arthroplasty: a randomized clinical trial. Acta Orthop 78:172–179
Funding
No funding was received for the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors MM, PB, JH, RB declare that they have no conflict of interest. The author ET declares that he is providing consultancies for Convatec, KCI, LIMA, Medacta and Zimmer Biomet. He also declares that he receives royalties from LIMA, Medacta and Zimmer Biomet. He further declares that he is part of the European knee society board. The author JB declares that he has no conflict of interest, receives honoraria from DePuy, Conformis, Pajunk and Smith & Nephew.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the ethic committee of the local state medical council (Approv. No. F-2017-025).
Informed consent
Informed consent was obtained from all individual participants included in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Meier, M., Burkhardt, P., Huth, J. et al. Additional periarticular catheter shows no superiority over single-shot local infiltration analgesia alone in unicondylar knee replacement. Knee Surg Sports Traumatol Arthrosc 29, 627–632 (2021). https://doi.org/10.1007/s00167-020-05981-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-05981-y