Abstract
Purpose
To compare muscle strength, muscle endurance, and postural stability in both the affected and unaffected ankles between patients with chronic ankle instability (CAI) who underwent conservative treatment and those who underwent the modified Broström procedure (MBP).
Methods
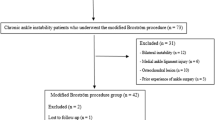
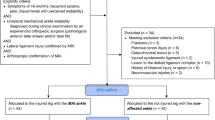
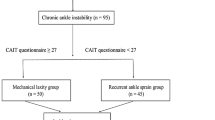
A total of 67 patients (37, conservative treatment; 30, MBP) participated. Muscle strength and muscle endurance were measured using an isokinetic device, and postural stability was tested using a postural stabilometry system. We used the independent t test for continuous variables with a normal distribution and Fisher’s exact test for categorical variables.
Results
There was no difference in the muscle strengths of the affected and unaffected ankles between the groups. The muscle endurance of plantarflexion and inversion muscles was significantly lower in the affected ankles of the conservative treatment group than in those of the MBP group (plantarflexion: 209 ± 103.1 vs. 318 ± 162.2, p = 0.001; inversion: 93 ± 58.7 vs. 154 ± 65.9, p < 0.001). Static postural stability testing showed no significant differences between the affected and unaffected ankles of the two groups. In the dynamic postural stability test, the overall, anterior–posterior, and medial–lateral stability indices were all significantly higher in the affected ankles of the conservative treatment group than in those of the MBP group (p < 0.001, p = 0.004, p = 0.004, respectively), with no differences observed in the unaffected ankles.
Conclusion
The MBP may significantly improve muscle endurance and dynamic postural stability in CAI patients in whom conservative treatment has failed. Therefore, clinicians should consider using MBP instead of conservative treatment when patients show severe muscle weakness or dynamic postural instability.
Level of evidence
Case–control study, Level III.

Similar content being viewed by others
References
Abdel-Aziem AA, Draz AH (2014) Chronic ankle instability alters eccentric eversion/inversion and dorsiflexion/plantarflexion ratio. J Back Musculoskelet Rehabil 27(1):47–53
Barber-Westin SD, Noyes FR (2011) Factors used to determine return to unrestricted sports activities after anterior cruciate ligament reconstruction. Arthroscopy 27(12):1697–1705
Beckman SM, Buchanan TS (1995) Ankle inversion injury and hypermobility: effect on hip and ankle muscle electromyography onset latency. Arch Phys Med Rehabil 76(12):1138–1143
Cao Y, Hong Y, Xu Y, Zhu Y, Xu X (2018) Surgical management of chronic lateral ankle instability: a meta-analysis. J Orthop Surg Res 13(1):159
Chew CP, Koo KOT, Lie DTT (2018) Periosteal flap augmentation of the modified Broström gould procedure for chronic lateral ankle instability. J Orthop Surg Hong Kong 26(1):2309499018757530
Guillo S, Bauer T, Lee JW, Takao M, Kong SW, Stone JW, Mangone PG, Molloy A, Perera A, Pearce CJ, Michels F, Tourne Y, Ghorbani A, Calder J (2013) Consensus in chronic ankle instability: aetiology, assessment, surgical indications and place for arthroscopy. Orthop Traumatol Surg Res 99(8 Suppl):S411–S419
Hertel J (2002) Functional anatomy, pathomechanics, and pathophysiology of lateral ankle instability. J Athl Train 37(4):364–375
Hiller CE, Nightingale EJ, Lin CW, Coughlan GF, Caulfield B, Delahunt E (2011) Characteristics of people with recurrent ankle sprains: a systematic review with meta-analysis. Br J Sports Med 45(8):660–672
Hubbard TJ, Hicks-Little CA (2008) Ankle ligament healing after an acute ankle sprain: an evidence-based approach. J Athl Train 43(5):523–552
Kaminski TW, Hartsell HD (2002) Factors contributing to chronic ankle instability: a strength perspective. J Athl Train 37(4):394–405
Kerkhoffs GM, Handoll HH, de Bie R, Rowe BH, Struijs PA (2007) Surgical versus conservative treatment for acute injuries of the lateral ligament complex of the ankle in adults. Cochrane Database Sys Rev 18(2):CD000380
Lee JH, Heo JW, Lee DH (2018) Comparative postural stability in patients with lateral meniscus versus medial meniscus tears. Knee 25(2):256–261
Lee JH, Lee SH, Choi GW, Jung HW, Jang WY (2018) Individuals with recurrent ankle sprain demonstrate postural instability and neuromuscular control deficits in unaffected side. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-018-5190-1
Lephart SM, Kocher MS, Fu FH, Borsa PA, Harner CD (1992) Proprioception following anterior cruciate ligament reconstruction. J Sport Rehabil 1(3):188–196
Li HY, Zheng JJ, Zhang J, Cai YH, Hua YH, Chen SY (2016) The improvement of postural control in patients with mechanical ankle instability after lateral ankle ligaments reconstruction. Knee Surg Sports Traumatol Arthrosc 24(4):1081–1085
Li X, Killie H, Guerrero P, Busconi BD (2009) Anatomical reconstruction for chronic lateral ankle instability in the high-demand athlete: functional outcomes after the modified Broström repair using suture anchors. Am J Sports Med 37(3):488–494
Matsui K, Takao M, Miyamoto W, Matsushita T (2016) Early recovery after arthroscopic repair compared to open repair of the anterior talofibular ligament for lateral instability of the ankle. Arch Orthop Trauma Surg 136(1):93–100
McKeon PO, Hertel J (2008) Systematic review of postural control and lateral ankle instability, part I: can deficits be detected with instrumented testing. J Athl Train 43(3):293–304
Michels F, Pereira H, Calder J, Matricali G, Glazebrook M, Guillo S, Karlsson J, Acevedo J, Batista J, Bauer T, Calder J, Carreira D, Choi W, Corte-Real N, Glazebrook M, Ghorbani A, Giza E, Guillo S, Hunt K, Karlsson J, Kong SW, Lee JW, Michels F, Molloy A, Mangone P, Matsui K, Nery C, Ozeki S, Pearce C, Pereira H, Perera A, Pijnenburg B, Raduan F, Stone J, Takao M, Tourne Y, Vega J (2018) Searching for consensus in the approach to patients with chronic lateral ankle instability: ask the expert. Knee Surg Sports Traumatol Arthrosc 26(7):2095–2102
Michelson JD, Hutchins C (1995) Mechanoreceptors in human ankle ligaments. J Bone Joint Surg Br 77(2):219–224
Mitchell A, Dyson R, Hale T, Abraham C (2008) Biomechanics of ankle instability. Part 1: reaction time to simulated ankle sprain. Med Sci Sports Exerc 40(8):1515–1521
Myers JB, Riemann BL, Hwang JH, Fu FH, Lephart SM (2003) Effect of peripheral afferent alteration of the lateral ankle ligaments on dynamic stability. Am J Sports Med 31(4):498–506
Vitale TD, Fallat LM (1988) Lateral ankle sprains: evaluation and treatment. J Foot Surg 27(3):248–258
Webster KA, Gribble PA (2010) Functional rehabilitation interventions for chronic ankle instability: a systematic review. J Sport Rehabil 19(1):98–114
Wilkerson GB, Nitz AJ (1994) Dynamic ankle stability: mechanical and neuromuscular interrelationships. J Sport Rehabil 3(1):43–57
Willems TM, Witvrouw E, Delbaere K, Mahieu N, De Bourdeaudhuij I, De Clercq D (2005) Intrinsic risk factors for inversion ankle sprains in male subjects: a prospective study. Am J Sports Med 33(3):415–423
Witchalls J, Blanch P, Waddington G, Adams R (2012) Intrinsic functional deficits associated with increased risk of ankle injuries: a systematic review with meta-analysis. Br J Sports Med 46(7):515–523
Wu X, Song W, Zheng C, Zhou S, Bai S (2015) Morphological study of mechanoreceptors in collateral ligaments of the ankle joint. J Orthop Surg Res 10:92
Yoo JS, Yang EA (2016) Clinical results of an arthroscopic modified Broström operation with and without an internal brace. J Orthop Traumatol 17(4):353–360
Funding
This research was supported by the NRF Grant funded by the Korea government (NRF-2018R1C1B6005202).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No financial biases exist for any author.
Ethical approval
The institutional review board of the Korea University Anam Hospital approved this study (No: ED17143).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lee, J.H., Lee, S.H., Jung, H.W. et al. Modified Broström procedure in patients with chronic ankle instability is superior to conservative treatment in terms of muscle endurance and postural stability. Knee Surg Sports Traumatol Arthrosc 28, 93–99 (2020). https://doi.org/10.1007/s00167-019-05582-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-019-05582-4