Abstract
Purpose
To compare the outcome, recovery and surgical findings after shoulder arthroscopy of clinically defined traumatic and non-traumatic rotator cuff pathology in middle-aged patients.
Methods
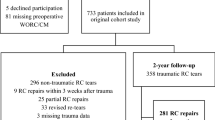
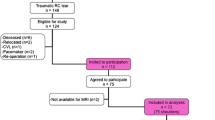
Of the patients who underwent rotator cuff surgery, 37 patients who reported a preceding shoulder injury related to their shoulder symptoms (traumatic group) were compared to a control group of 58 patients without a preceding injury (non-traumatic group), matched by age, body mass index and comorbidities. Data included demographic details, patient history, surgical findings, the Oxford Shoulder Score questionnaires and overall satisfaction from surgery.
Results
The mean follow-up time was 33.2 ± 14.4 months. More concomitant pathologies were found in the study group. The proportion of large and massive supraspinatus tears was double in the study group (43%) compared to the control group (22%). The Oxford Shoulder Score (OSS) improved significantly after surgery in both groups (p < 0.001) with no differences between groups in OSS and overall satisfaction from surgery. Patients in the study group felt recovered at an average time of 6.1 ± 4.6 months from surgery, while patients in the control group felt recovered at 4.2 ± 2.6 months (p = 0.02). Patients who were operated at the first 6 months after the injury had better improvement in OSS than patients who were operated later.
Conclusion
Surgical arthroscopy for rotator pathology of the shoulder in middle-aged patients improved pain and function regardless of a traumatic onset; however, earlier repair after trauma resulted in better outcome scores. Larger full-thickness tears and concomitant pathologies were more common after injury.
Study design
Level III.

Similar content being viewed by others
References
Bassett RW, Cofield RH (1983) Acute tears of the rotator cuff: the timing of surgical repair. Clin Orthop Relat Res 175:18–24
Bjornsson HC, Norlin R, Johansson K, Adolfsson LE (2011) The influence of age, delay of repair, and tendon involvement in acute rotator cuff tears: structural and clinical outcomes after repair of 42 shoulders. Acta Orthop 82:187–192
Braune C, von Eisenhart-Rothe R, Welsch F, Teufel M, Jaeger A (2003) Midterm results and quantitative comparison of postoperative shoulder function in traumatic and non-traumatic rotator cuff tears. Arch Orthop Trauma Surg 123:419–424
Butler BR, Byrne AN, Higgins LD, Shah A, Fowler RL (2013) Results of the repair of acute rotator cuff tears is not influenced by tear retraction. Int J Shoulder Surg 7:91–109
Colvin AC, Egorova N, Harrison AK, Moskowitz A, Flatow EL (2012) National trends in rotator cuff repair. J Bone Jt Surg Am 94:227–233
Dawson J, Harris KK, Doll H, Fitzpatrick R, Carr A (2016) A comparison of the Oxford shoulder score and shoulder pain and disability index: factor structure in the context of a large randomized controlled trial. Patient Relat Outcome Meas 7:195–203
Duncan NS, Booker SJ, Gooding BW, Geoghegan J, Wallace WA, Manning PA (2015) Surgery within 6 months of an acute rotator cuff tear significantly improves outcome. J Shoulder Elbow Surg 24:1876–1880
Gerber C, Hersche O, Farron A (1996) Isolated rupture of the subscapularis tendon. J Bone Jt Surg Am 78:1015–1023
Gerber C, Meyer DC, Schneeberger AG, Hoppeler H, von Rechenberg B (2004) Effect of tendon release and delayed repair on the structure of the muscles of the rotator cuff: an experimental study in sheep. J Bone Jt Surg Am 86:1973–1982
Hantes ME, Karidakis GK, Vlychou M, Varitimidis S, Dailiana Z, Malizos KN (2011) A comparison of early versus delayed repair of traumatic rotator cuff tears. Knee Surg Sports Traumatol Arthrosc 19:1766–1770
Ide J, Tokiyoshi A, Hirose J, Mizuta H (2007) Arthroscopic repair of traumatic combined rotator cuff tears involving the subscapularis tendon. J Bone Jt Surg Am 89:2378–2388
Jeong JY, Song SY, Yoo JC, Park KM, Lee SM (2017) Comparison of outcomes with arthroscopic repair of acute-on-chronic within 6 months and chronic rotator cuff tears. J Shoulder Elbow Surg 26:648–655
Lahteenmaki HE, Virolainen P, Hiltunen A, Heikkila J, Nelimarkka OI (2006) Results of early operative treatment of rotator cuff tears with acute symptoms. J Shoulder Elbow Surg 15:148–153
Mall NA, Lee AS, Chahal J, Sherman SL, Romeo AA, Verma NN, Cole BJ (2013) An evidenced-based examination of the epidemiology and outcomes of traumatic rotator cuff tears. Arthroscopy 29(2):366–376
Mukovozov I, Byun S, Farrokhyar F, Wong I (2013) Time to surgery in acute rotator cuff tear: a systematic review. Bone Jt Res 2:122–128
Namdari S, Henn RF III, Green A (2008) Traumatic anterosuperior rotator cuff tears: the outcome of open surgical repair. J Bone Jt Surg Am 90:1906–1913
Petersen SA, Murphy TP (2011) The timing of rotator cuff repair for the restoration of function. J Shoulder Elbow Surg 20:62–68
Post M, Silver R, Singh M (1983) Rotator cuff tear. Diagnosis and treatment. Clin Orthop Relat Res 173:78–91
Tan M, Lam PH, Le BT, Murrell GA (2016) Trauma versus no trauma: an analysis of the effect of tear mechanism on tendon healing in 1300 consecutive patients after arthroscopic rotator cuff repair. J Shoulder Elbow Surg 25(1):12–21
Yamaguchi K, Ditsios K, Middleton WD, Hildebolt CF, Galatz LM, Teefey SA (2006) The demographic and morphological features of rotator cuff disease: a comparison of asymptomatic and symptomatic shoulders. J Bone Jt Surg Am 88:1699–1704
Yamamoto A, Takagishi K, Osawa T et al (2010) Prevalence and risk factors of a rotator cuff tear in the general population. J Shoulder Elbow Surg 19:116–120
Funding
No external source of funding was used.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was done in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments.
Rights and permissions
About this article
Cite this article
Haviv, B., Rutenberg, T.F., Bronak, S. et al. Arthroscopic rotator cuff surgery following shoulder trauma improves outcome despite additional pathologies and slow recovery. Knee Surg Sports Traumatol Arthrosc 26, 3804–3809 (2018). https://doi.org/10.1007/s00167-018-4969-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-4969-4