Abstract
Purpose
Although soft tissue balancing is considered important for successful total knee arthroplasty (TKA), it is unclear whether the laxity and balance achieved intraoperatively change postoperatively. A recent study demonstrated anaesthesia significantly influenced knee joint laxity after TKA; however, there has been no comparison of the varus–valgus laxity immediately after TKA and in the postoperative period under the same anesthetic conditions. Therefore, quantitative stress arthrometric studies were conducted under identical conditions to identify changes in coronal ligament laxity after TKA spontaneously.
Methods
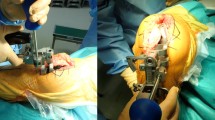
A consecutive series of 28 knees with varus of more than 5° in 28 patients undergoing staged bilateral TKAs was prospectively evaluated. Postoperative varus–valgus laxity was measured immediately after surgery, with the patient still under spinal anaesthesia; and again at the time of the contralateral TKA, again under anaesthesia. The mean time between the first and second operations was 9.7 ± 7.3 months.
Results
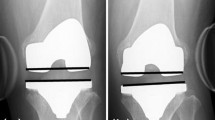
Mean medial laxity significantly changed from 2.4° ± 1.6° just after the first operation under anaesthesia to 3.8° ± 1.4° just after contralateral TKA under anaesthesia (p < 0.001), but no significant change occurred in lateral laxity (5.6° ± 2.4° just after the first operation and 5.7° ± 2.1° after contralateral TKA, n.s.). Significant negative correlations were identified between laxity immediately after surgery and the amount of laxity change on both the medial (R = − 0.63, p < 0.001) and lateral sides (R = − 0.53, p < 0.001).
Conclusion
Spontaneous soft tissue correction occurs after TKA. The findings from this study provides a rationale that it is not necessary for surgeons to perform the medial soft tissue release until the soft tissue tension is equalized on both the medial and lateral sides which has the risk of excessive release leading to instability. In situations where the surgeon is confronted with a knee that becomes too tight or too loose depending on the insert thickness, it is recommended to choose the thicker insert with the understanding that the knee will initially have a slightly tighter medial compartment that will loosen over time. The results of this study provide technical considerations that can help a surgeon achieve adequate postoperative stability.
Level of evidence
IV.






Similar content being viewed by others
References
Bellemans J, D’Hooghe P, Vandenneucker H, Van Damme G, Victor J (2006) Soft tissue balance in total knee arthroplasty: does stress relaxation occur perioperatively? Clin Orthop Relat Res 452:49–52
Bellemans J, Vandenneucker H, Vanlauwe J, Victor (2010) The influence of coronal plane deformity on mediolateral ligament status: an observational study in varus knees. Knee Surg Sports Traumatol Arthrosc 18:152–156
Cho WS, Byun SE, Lee SJ, Yoon J (2015) Laxity after complete release of the medial collateral ligament in primary total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 23(6):1816–1823
Dorr LD, Boiardo RA (1986) Technical considerations in total knee arthroplasty. Clin Orthop Relat Res 205:5–11
Griffin FM. Insall JN. Scuderi GR (2000) Accuracy of soft tissue balancing in total knee arthroplasty. J Arthroplast 15:970–973
Insall JN, Binazzi R, Soudry M, Mestriner LA (1985) Total knee arthroplasty. Clin Orthop Relat Res 192:13–22
Ishii Y, Matsuda Y, Ishii R, Sakata S, Omori G (2003) Coronal laxity in extension in vivo after total knee arthroplasty. J Orthop Sci 8:538–542
Ishii Y, Matsuda Y, Noguchi H, Kiga H (2005) Effect of soft tissue tension on measurements of coronal laxity in mobile-bearing total knee arthroplasty. J Orthop Sci 10:496–500
Krackow KA, Mihalko WM (1999) The effect of medial release on flexion and extension gaps in cadaveric knees: implications for soft-tissue balancing in total knee arthroplasty. Am J Knee Surg 124:222–228
Matsuda S, Ito H.(2015) Ligament balancing in total knee arthroplasty—medial stabilizing technique. Asia Pac J Sports Med Arthrosc Rehabil Technol 2(4):108–113
Matsuda Y, Ishii Y, Noguchi H, Ishii R (2005) Varus–valgus balance and range of movement after total knee arthroplasty. J Bone Jt Surg Br 87:804–808
Nakajima A, Aoki Y, Murakami M, Nakagawa K (2014) Changes in joint gap balances between intra- and postoperation in total knee arthroplasty. Adv Orthop 2014:790806
Sekiya H, Takatoku K, Takada H, Sasanuma H, Sugimoto N (2009) Postoperative lateral ligamentous laxity diminishes with time after TKA in the varus knee. Clin Orthop Relat Res 467:1582–1586
Takeda M, Ishii Y, Noguchi H, Matsuda Y, Sato J (2012) Changes in varus–valgus laxity after total knee arthroplasty over time. Knee Surg Sports Traumatol Arthrosc 20:1988–1993
Tsukeoka T, Tsuneizumi Y (2016) Varus and valgus stress tests after total knee arthroplasty with and without anesthesia. Arch Orthop Trauma Surg 136(3):407–411
Yagishita K, Muneta T, Yamamoto H, Shinomiya K (2001) The relationship between postoperative ligament balance and preoperative varus deformity in total knee arthroplasty. Bull Hosp Jt Dis 60:23–28
Yoshihara Y, Arai Y, Nakagawa S, Inoue H, Ueshima K, Fujiwara H, Oda R, Taniguchi D, Kubo T (2016) Assessing coronal laxity in extension and flexion at a minimum of 10 years after primary total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 24(8):2512–2516
Funding
No funding of whatever form was provided for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Ethical approval
This study was ethically approved by Chiba Rehabilitation Center Institution Review Board (ID number of approval: Iryou22-5)
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Tsukeoka, T., Tsuneizumi, Y. Residual medial tightness in extension is corrected spontaneously after total knee arthroplasty in varus knees. Knee Surg Sports Traumatol Arthrosc 27, 692–697 (2019). https://doi.org/10.1007/s00167-018-4967-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-4967-6