Abstract
Purpose
The treatment approach for a patient with knee joint focal cartilage lesion is a difficult decision. To date, there has been no randomized clinical trial involving Hydrogel (Cartiva™). This study evaluated and compared the results of a hydrogel implant (Cartiva™) with autologous osteochondral transplantation (AOT) for treating knee joint focal cartilage lesions.
Methods
Thirty-eight symptomatic patients, with a focal cartilage lesion of Outerbridge grades III or IV, were randomized into one of two groups according to the inclusion and exclusion criteria. Group I underwent AOT, and Group II was treated with a Hydrogel implant. Patients were evaluated preoperatively and again postoperatively at 6, 12, and 24 months using the subjective International Knee Documentation Committee (IKDC) scores, Visual Analog Scale for Pain (VAS Pain), Activities of Daily Living Scale (ADLS) and Lysholm score.
Results
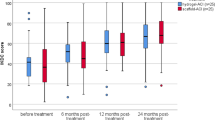
Both groups showed significant improvements from baseline (pre-surgery) to post-surgery (6, 12, and 24 months; p < 0.05), but there was no difference between the groups. Regarding complications, prolonged pain was observed in four patients (10.5%), two from each group, with a regression of symptoms within 1 year.
Conclusion
The Hydrogel implant showed similar efficiency as the autologous osteochondral graft for treating knee joint focal cartilage lesions. Both techniques showed satisfactory results compared to preoperative status. The Hydrogel implant was safe and effective, and it provided good stability and joint function at 2-year follow-up.
Level of evidence
I.



Similar content being viewed by others
Abbreviations
- IKDC:
-
International Knee Documentation Committee
- VAS Pain:
-
Visual Analog Scale for Pain
- ADLS:
-
Activities of Daily Living Scale
- AOT:
-
Autologous osteochondral transplantation
- MRI:
-
Magnetic resonance imaging
References
Andrew SL, Meier SW (2004) Osteochondral autograft replacement. In: Articular lesions: a practical guide toward assessment and treatment, vol 8. Springer, New York, pp 73–81
Beyerlein J, Imhoff AB (2003) Salucartilage a new synthetic replacement for the arthroscopic treatment of focal osteonecrosis. Arthroscopy 16:34–39
Brittberg M, Winalski CS (2003) Evaluation of cartilage injuries and repair. J Bone Jt Surg Am 85A(suppl 2):58–69
Bosch U, Meller R, Tröger JH, Zeichen J (2003) Cartiva-a synthetic cartilage replacement for the minimally invasive treatment of osteochondral defects. Arthroscopy 16:40–43
Cole BJ, Pascual-Garrido C, Grumet RC (2010) Surgical management of articular cartilage defects in the knee. Instr Course Lect 59:181–204
Cohen M, Amaro JT, Fernandes RSC, Arliani GG, Astur DC, Kaleka CC, Cohen C, Skaf A (2012) Transplante osteocondral autólogo no tratamento de lesões condrais na patela. Rev Bras Ortop 47(3):348–353
Curl WW, Krome J, Gordon ES, Rushing J, Smith BP, Poehling GG (1997) Cartilage injuries: a review of 31,516 knee arthroscopies. Arthroscopy 13(4):456–460
Falez F, Sciarretta FV (2005) Treatment of osteochondral symptomatic defects of the knee with SaluCartilage. J Bone Jt Surg Br 87-B(Suppl II):202
Farr J II, Gomoll A (2012) Articular Cartilage repair with bioscaffolds. In: Scott WN (ed) Insall & Scott surgery of the knee, chap 26, 5th edn. Churchill Livingstone, Elsevier, pp 214–220.e2
Gomoll AH, Madry H, Knutsen G, van Dijk N, Seil R, Brittberg M, Kon E (2010) The subchondral bone in articular cartilage repair: current problems in the surgical management. Knee Surg Sports Traumatol Arthrosc 18(4):434–447
Gomoll AH, Minas T (2011) Chapter 5-debridement, microfracture, and osteochondral autograft transfer for treatment of cartilage defects. In: Minas T et al A primer in cartilage repair and joint preservation of the knee, (part 2): cartilage repair surgical techniques. Saunders Elsevier, Philadelphia, pp 48–53
Gudas R, Gudaite A, Mickevicius T, Masiulis N, Simonailyté R, Cekanausaskas E, Skurvydas A (2013) Comparison of osteochondral autologous transplantation, microfracture, or debridement techniques in articular cartilage lesions associated with anterior cruciate ligament injury: a prospective study a 3-year follow-up. Arthroscopy 29(1):89–97
Gudas R, Gudaite A, Pocius A, Gudiene A, Cekanauskas E, Monastyreckiene E, Basevicius A (2012) Ten-year follow-up of a prospective, randomized clinical study of mosaic osteochondral autologous transplantation versus microfracture for the treatment of osteochondral defects in the knee joint of athletes. Am J Sports Med 40(11):2499–2508
Hangody L, Füles P (2003) Autologous osteochondral mosaicplasty for the treatment of full-thickness defects of weight-bearing joints: ten years of experimental and clinical experience. J Bone Jt Surg Am 85-A(Suppl 2):25–32
Hangody L, Ráthonyi GK, Duska Z, Vásárhelyi G, Füles P, Módis L (2004) Autologous Osteochondral Mosaicplasty. Surgical Technique. J Bone Jt Surg Am 86-A(Suppl 1):65–72
Henry SE, Deasy BM, Chu CR (2012) Articular cartilage: biology, biomechanics, and healing response. In: Scott WN (ed) Insall & scott surgery of the knee, 5th edn. Elsevier, Philadelphia, pp 146–154
Horas U, Pelinkovic D, Herr G, Aigner T, Schnettler R (2003) Autologous chondrocyte implantation and osteochondral cylinder transplantation in cartilage repair of the knee joint. A prospective, comparative trial. J Bone Jt Surg Am 85-A(2):185–192
Intzoglou KS, Mastrokalos DS, Korres DS, Papaparaskeva K, Koulalis D, Babis GC (2014) Donor’s site evaluation after restoration with autografts or synthetic plugs in rabbits. World J Orthop 5(4):550–556
Lahav A, Burks RT, Greis PE, Chapman AW, Ford GM, Fink BP (2006) Clinical outcomes following osteochondral autologous transplantation (OATS). J Knee Surg 1 19(3):169–173
Laprell H, Petersen W (2001) Autologous osteochondral transplantation using the diamond bone-cutting system (DBCS): 6–12 years’ follow-up of 35 patients with osteochondral defects at the knee joint. Arch Orthop Trauma Surg 121(5):248–253
Lange J, Follak N, Nowotny T, Merk H (2006) Results of SaluCartilage implantation for stage IV chondral defects in the knee joint area. Unfallchirurg 109(3):193–199
Lira-Neto OA, Franciozi CES, Granata Junior GSM, Queiroz AAB, Carneiro Filho M, Navarro RD (2010) Tratamento cirúrgico das lesões osteocondrais do joelho com mosaicoplastia. Rev Bras Ortop 45(2):166–173
Ma HL, Hung SC, Wang ST, Chang MC, Chen TH (2004) Osteochondral autografts transfer for post-traumatic osteochondral defect of the knee—2 to 5 years follow-up. Injury 35:1286–1292
Maiotti M, Massoni C, Allegra F (2005) The use of poli-hydrogel cylindrical implants to treat deep chondral defects of the knee. Arthroscopy Association of North America, Vancouver, B.C
Mundi R, Bedi A, Chow L, Crouch S, Simunovic N, Sibilisky Enselman E, Ayeni OR (2015) Cartilage restoration of the knee: a systematic review and meta-analysis of level 1 studies. Am J Sports Med 43(8):124–132
Ollat D, Lebel B, Thaunat M, Jones D, Mainard L, Dubrana F, Versier G (2011) Mosaic osteochondral transplantations in the knee joint, midterm results of the SFA multicenter study. Orthop Traumatol Surg Res 97(8)[Suppl]):S160–S166
Sciarretta FV (2013) 5 to 8 years follow-up of knee chondral defects treated by PVA-H hydrogel implants. Eur Rev Med Pharmacol Sci 17(22):3031–3038
Spiller KL, Mahner SA, Lownan AM (2011) Hydrogels for the repair of articular cartilage defects. Tissue Eng Part B Rev 17(4):281–299
Solheim E, Hegna J, Oyen J, Harlem T, Strand T (2013) Results at 10–14 years after osteochondral autografting (mosaicplasty) in articular cartilage defects in the knee. Knee 20(4):287–290
Funding
No funding resources.
Author information
Authors and Affiliations
Contributions
AABQ, PD, JA, MF and MC: conception and design, acquisition of data, statistical analysis and interpretation of data, drafting the manuscript, critical revision for important intellectual content, and final approval of the manuscript to be published and are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work were appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
There are no conflicts of interest involved.
Ethical approval
The study was approved by the research ethics committee of the Federal University of Sao Paulo (under the number: 05874612 00000 5505).
Informed consent
All patients underwent the free and informed consent term.
Rights and permissions
About this article
Cite this article
de Queiroz, A.A.B., Debieux, P., Amaro, J. et al. Hydrogel implant is as effective as osteochondral autologous transplantation for treating focal cartilage knee injury in 24 months. Knee Surg Sports Traumatol Arthrosc 26, 2934–2941 (2018). https://doi.org/10.1007/s00167-018-4834-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-4834-5