Abstract
Purpose
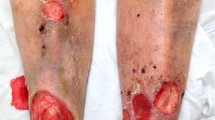
Localized cooling is widely used in treating soft tissue injuries by modulating swelling, pain, and inflammation. One of the primary outcomes of localized cooling is vasoconstriction within the underlying skin. It is thought that in some instances, cryotherapy may be causative of tissue necrosis and neuropathy via cold-induced ischaemia leading to nonfreezing cold injury (NFCI). The purpose of this study is to quantify the magnitude and persistence of vasoconstriction associated with cryotherapy.
Methods
Data are presented from testing with four different FDA approved cryotherapy devices. Blood perfusion and skin temperature were measured at multiple anatomical sites during baseline, active cooling, and passive rewarming periods.
Results
Local cutaneous blood perfusion was depressed in response to cooling the skin surface with all devices, including the DonJoy (DJO, p = 2.6 × 10−8), Polar Care 300 (PC300, p = 1.1 × 10−3), Polar Care 500 Lite (PC500L, p = 0.010), and DeRoyal T505 (DR505, p = 0.016). During the rewarming period, parasitic heat gain from the underlying tissues and the environment resulted in increased temperatures of the skin and pad for all devices, but blood perfusion did not change significantly, DJO (n.s.), PC300 (n.s.), PC500L (n.s.), and DR505 (n.s.).
Conclusions
The results demonstrate that cryotherapy can create a deep state of vasoconstriction in the local area of treatment. In the absence of independent stimulation, the condition of reduced blood flow persists long after cooling is stopped and local temperatures have rewarmed towards the normal range, indicating that the maintenance of vasoconstriction is not directly dependent on the continuing existence of a cold state. The depressed blood flow may dispose tissue to NFCI.



Similar content being viewed by others
References
Adie S, Naylor JM, Harris IA (2010) Cryotherapy after total knee arthroplasty: a systematic review and meta-analysis of randomized controlled trials. J Arthroplast 25:709–715
Airaksinen OV, Kyrklund N, Latvala K, Kouri JP, Grönblad M, Kolari P (2003) Efficacy of cold gel for soft tissue injuries a prospective randomized double-blinded trial. Am J Sports Med 31:680–684
Barber FA (2000) A comparison of crushed ice and continuous flow cold therapy. Am J Knee Surg 13:97
Barber FA, McGuire DA, Click S (1998) Continuous-flow cold therapy for outpatient anterior cruciate ligament reconstruction. Arthroscopy 14:130–135
Bassett FH III, Kirkpatrick JS, Engelhardt DL, Malone TR (1992) Cryotherapy-induced nerve injury. Am J Sports Med 20:516–518
Bleakley C (2004) The use of ice in the treatment of acute soft-tissue injury: a systematic review of randomized controlled trials. Am J Sports Med 32:251–261
Bleakley CM (2006) Cryotherapy for acute ankle sprains: a randomised controlled study of two different icing protocols. Br J Sports Med 40:700–705
Brown WC, Hahn DB (2009) Frostbite of the feet after cryotherapy: a report of two cases. J Foot Ankle Surg 48:577–580
Clough G, Chipperfield A, Byrne C, de Mul F, Gush R (2009) Evaluation of a new high power, wide separation laser Doppler probe: potential measurement of deeper tissue blood flow. Microvasc Res 78:155–161
Cohn B, Draeger R, Jackson D (1989) The effects of cold therapy in the postoperative management of pain in patients undergoing anterior cruciate ligament reconstruction. Am J Sports Med 17:344–349
Curl WW, Smith BP, Marr A, Rosencrance E, Holden M, Smith TL (1997) The effect of contusion and cryotherapy on skeletal muscle microcirculation. J Sports Med Phys Fit 37:279
Faul F, Erdfelder E, Buchner A, Lang A-G (2009) Statistical power analyses using G* Power 3.1: tests for correlation and regression analyses. Behav Res Methods 41:1149–1160
Faul F, Erdfelder E, Lang A-G, Buchner A (2007) G* Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods 39:175–191
Flack VF, Afifi AA, Lachenbruch PA, Schouten HJA (1988) Sample size determinations for the two rater kappa statistic. Psychometrika 53:321–325
Fleiss JL (1986) Design and analysis of clinical experiments. Wiley, New York, pp 1–31
Francis TJ (1984) Non freezing cold injury: a historical review. J R Nav Med Serv 70:134–139
Francis TJ, Golden FS (1985) Non-freezing cold injury: the pathogenesis. J R Nav Med Serv 71:3–8
Hamlet MP (2001) Nonfreezing cold injury. Wilderness Med Mosby, St. Louis, pp 129–134
Hodges GJ, Zhao K, Kosiba WA, Johnson JM (2006) The involvement of nitric oxide in the cutaneous vasoconstrictor response to local cooling in humans. J Physiol 574:849–857
Irwin MS (1996) Nature and mechanism of peripheral nerve damage in an experimental model of non-freezing cold injury. Ann R Coll Surg Engl 78:372–379
Jia J, Pollock M (1999) Cold nerve injury is enhanced by intermittent cooling. Muscle Nerve 22:1644–1652
Johnson JM, Kellogg DL (2010) Local thermal control of the human cutaneous circulation. J Appl Physiol 109:1229–1238
Knight KL (1995) Cryotherapy in sport injury management. Human Kinetics, Champaign, pp 1–20
Knobloch K, Grasemann R, Spies M, Vogt PM (2008) Midportion achilles tendon microcirculation after intermittent combined cryotherapy and compression compared with cryotherapy alone: a randomized trial. Am J Sports Med 36:2128–2138
Knobloch K, Kraemer R, Lichtenberg A, Jagodzinski M, Gosling T, Richter M, Krettek C (2006) Microcirculation of the ankle after cryo/cuff application in healthy volunteers. Int J Sports Med 27:250–255
Konrath GA, Lock T, Goitz HT, Scheidler J (1996) The use of cold therapy after anterior cruciate ligament reconstruction a prospective, randomized study and literature review. Am J Sports Med 24:629–633
Lee CK, Pardun J, Buntic R, Kiehn M, Brooks D, Buncke HJ (2007) Severe frostbite of the knees after cryotherapy. Orthopedics 30:63–64
MacAuley D (2001) Do textbooks agree on their advice on ice? Clin J Sport Med 11:67–72
McGuire DA, Hendricks SD (2006) Incidences of frostbite in arthroscopic knee surgery postoperative cryotherapy rehabilitation. J Arthrosc Relat Surg 22:1141.e1–e6
Meeusen R, Lievens P (1986) The use of cryotherapy in sports injuries. Sports Med 3:398–414
Minson CT (2010) Thermal provocation to evaluate microvascular reactivity in human skin. J Appl Physiol 109:1239–1246
Moor Instruments. Tissue blood flow and temperature monitoring with moorVMS-LDF. Moor Instruments
Music M, Finderle Z, Cankar K (2011) Cold perception and cutaneous microvascular response to local cooling at different cooling temperatures. Microvasc Res 81:319–324
Razali NM, Wah YB (2011) Power comparisons of Shapiro–Wilk, Kolmogorov–Smirnov, Lilliefors and Anderson–Darling tests. J Stat Model Anal 2:21–33
Rheinecker S (1998) Using ice therapy to alleviate pain and edema. J Am Acad Physician Assist 11:73–81
Royston P (1995) A remark on algorithm AS 181: the W-test for normality. J R Stat Soc 44:547–551
Schaser K-D, Disch AC, Stover JF, Lauffer A, Bail HJ, Mittlmeier T (2006) Prolonged superficial local cryotherapy attenuates microcirculatory impairment, regional inflammation, and muscle necrosis after closed soft tissue injury in rats. Am J Sports Med 35:93–102
Schröder D, Pässler HH (1994) Combination of cold and compression after knee surgery. Knee Surg Sports Traumatol Arthrosc 2:158–165
Singh H, Osbahr DC, Holovacs TF, Cawley PW, Speer KP (2001) The efficacy of continuous cryotherapy on the postoperative shoulder: a prospective, randomized investigation. J Should Elb Surg 10:522–525
Thomas JR, Oakley EHN (2002) Nonfreezing cold injury. In: Pandoff KD, Burr RE (eds) Textbooks of military medicine: medical aspects of harsh environments. Office of the Surgeon General, U. S. Army, Falls Church, VA, pp 467–490
Van Ness PH, Towle VR, Juthani-Mehta M (2008) Testing measurement reliability in older populations: methods for informed discrimination in instrument selection and application. J Aging Health 20:183–197
Walter SD, Eliasziw M, Donner A (1998) Sample size and optimal designs for reliability studies. Stat Med 17:101–110
Warren TA (2004) Intra-articular knee temperature changes: ice versus cryotherapy device. Am J Sports Med 32:441–445
Woolf SK, Barfield WR, Merrill KD, McBryde AMJ (2008) Comparison of a continuous temperature-controlled cryotherapy device to a simple icing regimen following outpatient knee arthroscopy. J Knee Surg 21:15–19
(2014) MoorVMS-LDF Specifications. Moor Instruments. http://gb.moor.co.uk/product/moorvms-ldf-laser-doppler-monitor-ldf/1/o/14/specifications
Acknowledgments
This research was sponsored by National Science Foundation Grants CBET 0828131, CBET 096998, and CBET 1250659, National Institutes of Health Grant R01 EB015522, and the Robert and Prudie Leibrock Professorship in Engineering at the University of Texas at Austin. We would also like to thank Ms. Natalia Mejia for investing long hours of careful and conscientious work in her critical role in extracting data for this publication, and Dr. Michael Mahometa of the Division of Statistics and Scientific Computation, College of Natural Sciences at the University of Texas at Austin for his help and guidance in statistical analysis of data. Comments by the reviewers have been very helpful.
Conflict of interest
A patent application has been submitted by Dr. Khoshnevis and Dr. Diller to the United States Patent and Trademark Office under the title Improved Cryotherapy Devices and Methods to Limit Ischaemic Injury Side Effects. Ownership rights to this patent reside with The University of Texas System. Dr. Diller has served as an expert witness for both plaintiff and defendant counsel since 2000 in numerous legal cases regarding the safety and design of existing cryotherapy devices.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Khoshnevis, S., Craik, N.K. & Diller, K.R. Cold-induced vasoconstriction may persist long after cooling ends: an evaluation of multiple cryotherapy units. Knee Surg Sports Traumatol Arthrosc 23, 2475–2483 (2015). https://doi.org/10.1007/s00167-014-2911-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-014-2911-y