Abstract
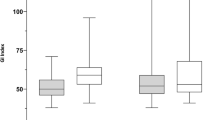
Objectives: To investigate the relationship between the attenuation of impedance cardiac output (ICco) measurements and lung fluid content in critically ill patients.¶Design: Observational study.¶Setting: Intensive Care Unit of a major teaching hospital in Hong Kong.¶Patients: Twenty-four critically ill patients who required a pulmonary artery catheter.¶Measurements and main results: Triplicate thermodilution cardiac output (TDco) and BoMed NCCOM3 (ICco) measurements were made simultaneously on a single occasion in each patient. Lung fluid accumulation was assessed by: (a) thoracic impedance (Zo), (b) radiological assessment of chest X-rays using an alveolar consolidation score (0–4) and (c) scoring the degree of hypoxia and use of positive end-expiratory pressure (PEEP). Offsets (TDco–ICco)/TDco, expressed as percentage, were compared with these indices of excess lung fluid. Patients were divided into those with sepsis (n = 13), fluid balance problems (n = 5) and cardiothoracic problems (n = 6). Mean cardiac output values were: 6.7 l/min TDco (range 3.6–12.9) and 5.2 l/min ICco (range 2.7–9.0). Overall the TDco and ICco values showed great variance, with a bias and limits of agreement of 1.49 ± 4.16 l/min, or ± 69 %. In septic patients, increasing offset was correlated with decreases in Zo (r = 0.73, P = 0.005) and increases in alveolar consolidation score (r = 0.72, P = 0.005).¶Conclusions: The BoMed under-estimates cardiac output in critically ill patients. In septic patients the degree of attenuation of ICco can be related to the extent of lung injury and fluid accumulation within the thorax.
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Received: 14 September 1999/Final revision received: 2 February 2000/Accepted: 9 March 2000
Rights and permissions
About this article
Cite this article
Critchley, L., Calcroft, R., Tan, P. et al. The effect of lung injury and excessive lung fluid, on impedance cardiac output measurements, in the critically ill. Intensive Care Med 26, 679–685 (2000). https://doi.org/10.1007/s001340051232
Issue Date:
DOI: https://doi.org/10.1007/s001340051232