Abstract
Purpose
Ulinastatin, a serine protease inhibitor, inhibits several pro-inflammatory proteases and decreases inflammatory cytokine levels and mortality in experimental sepsis. We studied the effect of ulinastatin on 28-day all-cause mortality in a double-blind trial in patients with severe sepsis in seven Indian hospitals.
Methods
Patients with sepsis were randomized within 48 h of onset of one or more organ failures to receive intravenous administration of ulinastatin (200,000 IU) or placebo 12 hourly for 5 days.
Results
Of 122 randomized subjects, 114 completed the study (55 receiving ulinastatin, 59 receiving placebo). At baseline, the mean APACHE II score was 13.4 (SD = 4.4), 48 (42 %) patients were receiving mechanical ventilation, 58 (51 %) were on vasopressors, and 35 % had multiple organ failure. In the modified intention-to-treat analysis (patients receiving six or more doses of study drugs), 28-day all-cause mortality was 7.3 % with ulinastatin (4 deaths) versus 20.3 % (12 deaths) with placebo (p = 0.045). On multivariate analysis too, treatment with ulinastatin (odds ratio 0.26, 95 % CI 0.07–0.95; p = 0.042) independently decreased 28-day all-cause mortality. However, the mortality difference did not reach statistical significance in the intention-to-treat analysis [10.2 % (6/59 deaths) with ulinastatin versus 20.6 % (13/63 deaths) in the placebo group; p = 0.11]. The ulinastatin group had lower incidence of new-onset organ failure (10 vs. 26 patients, p = 0.003), more ventilator-free days (mean ± SD 19.4 ± 10.6 days vs. 10.2 ± 12.5 days, p = 0.019), and shorter hospital stay (11.8 ± 7.1 days vs. 24.2 ± 7.2 days, p < 0.001).
Conclusions
In this pilot study, intravenous administration of ulinastatin reduced mortality in patients with severe sepsis in the modified intention-to-treat analysis, but not in the intention-to-treat analysis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sepsis is a common cause of morbidity and mortality in critically ill patients, and its incidence is increasing worldwide annually [1, 2]. The pathogenesis of sepsis is complex and is believed to be initiated by the interaction between pathogen-associated molecular patterns and pattern recognition receptors on host immune cells [3, 4]. This sets off a series of pro-inflammatory mechanisms including synthesis and release of cytokines and complement, chemotaxis and activation of neutrophils, and initiation of coagulation [3–5]. These, in turn, have widespread effects on other cells including inflammatory cells, immune response, endocrine and autonomic nervous systems, and vascular endothelium, mainly aimed at limiting spread or eliminating the infecting pathogen [3–6]. Current opinion suggests that the systemic inflammatory response syndrome (SIRS) that characterizes severe sepsis results from an excessive activation of pro-inflammatory mediators, which have pleiotropic effects that overwhelm the body’s anti-inflammatory mechanisms, leading to widespread vascular, endothelial, and organ dysfunction that is often fatal [3–6].
Many of the intermediaries in the systemic inflammatory processes are serine proteases. These include trypsin, thrombin, chymotrypsin, kallikrein, plasmin, neutrophil elastase, cathepsin, neutrophil protease-3, and coagulation factors IXa, Xa, XIa, and XlIa [7, 8]. It is now being recognized that besides their proteolytic activity, these proteases have an important role in regulation of inflammation through inter- and intracellular signaling pathways [8, 9]. To counter-regulate the effect of these proteases, several protease inhibitors are produced by the liver in the presence of inflammation; these include acute phase reactants such as α1-antitrypsin and proteins of the inter-α-inhibitor family [9]. Urinary trypsin inhibitor is one such important protease inhibitor found in human blood and urine; it has been also referred to in the literature as ulinastatin or bikunin [10, 11]. It is an acidic glycoprotein (molecular weight 30 kDa) and Kunitz-type serine protease inhibitor composed of 143 amino acid residues and includes two Kunitz-type domains [7, 10]. It is cleaved from the larger inter-α-trypsin inhibitor molecule by neutrophil elastase in the presence of inflammation, and is believed to play an important anti-inflammatory role [8–12].
Studies in patients have shown that there is a decrease in serum levels of ulinastatin in sepsis, with the lowest levels being found in patients with severe sepsis and septic shock [12]. As compared to wild-type mice, mortality due to experimental sepsis is higher in genetically modified knockout mice that lack the genes for synthesis of urinary trypsin inhibitor [11, 13]. Several preclinical studies have shown a reduction in the systemic inflammatory response and organ dysfunction due to sepsis in animals treated with ulinastatin [13–17]. On the basis of a few small clinical studies that have shown a trend towards reduced mortality and duration of hospitalization with ulinastatin in severe sepsis [18, 19], some authors have suggested that ulinastatin may have a role as a novel therapy in severe sepsis [20, 21]. We therefore conducted this pilot study to evaluate the efficacy of ulinastatin in Indian patients with severe sepsis.
Methods
This randomized, double-blind, placebo-controlled trial was conducted in the intensive care units (ICUs) of seven tertiary care hospitals in India; the study protocol was approved by the institutional review boards at each center. The study protocol is available from the Indian clinical trials registry at http://www.ctri.nic.in (clinical trial number CTRI/2009/091/000650).
Adults, aged 18–60 years (both inclusive), with severe sepsis, admitted to the ICU between September 2009 and June 2010 were eligible for enrollment into the study. Sepsis was defined as evidence of infection (defined as presence of white blood cells in a normally sterile body fluid, perforated abdominal viscus, evidence of pneumonia, or presence of a condition associated with a high risk of bacterial infection, e.g., ascending cholangitis), and the presence of at least three of the four SIRS criteria [22]. Severe sepsis was defined as the presence of sepsis as defined above, along with dysfunction of at least one organ or system. Cardiovascular system failure was defined as systolic blood pressure ≤90 mmHg or mean arterial pressure ≤70 mmHg for at least 1 h despite adequate fluid resuscitation, or the use of vasopressors to maintain arterial pressure above these levels or unexplained metabolic acidosis (pH ≤ 7.30 or base deficit ≥5.0 mmol/L) with plasma lactate greater than 1.5 times the upper limit of normal. Renal failure was defined as urine output <0.5 mL/kg/h for 1 h, or serum creatinine levels greater than 2.5 times the upper limit; respiratory failure as PaO2/FiO2 ≤250 in the presence of other dysfunctional organs or ≤200 if only lung; hematologic dysfunction by platelet count <80,000/mm3 or 50 % drop in preceding 3 days [22]. Only patients with organ dysfunction of ≤48 h duration were eligible for inclusion.
Pregnant or breastfeeding women, patients with platelet count <30,000/mm3, history of organ transplantation, poorly controlled neoplasm, end-stage chronic kidney or liver disease, and patients weighing >135 kg were excluded. Patients in whom limitation of care was planned or who were expected to die within the next 24 h were also excluded.
Block randomization (block size of 4) using a computer-generated sequence was used to ensure balance between treatments; blinding of the sequence was maintained in sealed, opaque envelopes. Blinding of treatment allocation in participating centers was done using serially numbered packages of the study medication; package numbered 1 was to be used for the first patient, and so on. After obtaining written informed consent, patients were randomized in a 1:1 ratio to receive ulinastatin or placebo in addition to standard care. Randomized patients received an intravenous infusion of either 200,000 IU ulinastatin (U-tryp, Bharat Serum and Vaccines Ltd, India) or identical placebo dissolved in 250 mL of 0.9 % saline given intravenously over 1 h every 12 h for 5 days in a double-blind evaluation. For patients with fluid restriction, 100 mL of 0.9 % saline could be used. Infusion could be interrupted for 1 day, if there was greater than three times increase in liver enzymes over baseline levels.
In addition to the study medications, patients also received antibiotics, intravenous fluids, enteral or parenteral nutrition, transfusion of blood and blood products, and supportive care for organ dysfunction including mechanical or non-invasive ventilation, vasopressors (noradrenaline, adrenaline, dopamine, or vasopressin), or dialysis as per the standard treatment protocols followed in each ICU. Investigators were encouraged to follow the Surviving Sepsis Campaign guidelines. No concomitant medications were prohibited in the study.
Baseline characteristics including demographics, preexisting conditions, organ dysfunction, infection, and hematologic and other laboratory tests were assessed within the 24 h prior to infusion of the first dose of study medication. Blood samples were also obtained on the day of discharge. Patients were followed up till 28 days after the start of treatment. The primary end-point for this study was 28-day all-cause mortality. Secondary end-points included onset of new organ failure, duration of vasopressor use, ventilator-free days till day 28, and length of hospital stay. New-onset organ failure was defined as occurrence of organ failure after randomization. The definitions used were the same as those used in inclusion criteria; liver dysfunction was defined as serum bilirubin ≥2.0 mg/dL when bilirubin was <2.0 mg/dL at baseline and central nervous system failure was defined as Glasgow coma scale (GCS) ≤10 after randomization in patients who had baseline GCS >10.
Statistical analysis
Data analysis was carried out using the Graph Pad Instat and SPSS version 14 software package. Forward stepwise multiple logistic regression analysis was used for assessment of the primary end-point. Other categorical data were compared between the treatment groups by Pearson’s Chi-squared test or Fisher’s exact test, as appropriate. The unpaired t test was used for continuous variables and the Mann–Whitney test for ordinal data like the APACHE II score.
Sample size calculation was performed assuming a 28-day all-cause mortality of 30 % in the control group and 10 % in the study group. A sample size of 59 completed patients in each group was required to attain a power of 80 % at a significance level of 5 %. The primary efficacy end-point of 28-day all-cause mortality was assessed in the modified intention-to-treat population which was defined a priori. This primary analysis population included all randomized patients who had received at least six doses of the study medication. Safety was assessed in the safety population, defined as all subjects who received even a single dose of the study medication. Mortality difference in the intention-to-treat population that included all randomized subjects was analyzed as a secondary end-point.
Results
During the 10-month study period, 224 patients met the inclusion criteria. Of these, 102 patients were excluded; 99 because of presence of one or more exclusion criteria, or refusal of consent to participate in the study and three patients were not enrolled as they were expected to die within 24 h (Fig. 1). Of the 122 randomized subjects, 114 completed the study (55 subjects in the ulinastatin group and 59 subjects in the control group). Five subjects discontinued from the study (three subjects withdrew consent and two due to protocol violation). Three patients who died within 48 h of enrollment were not included for analysis in the modified intention-to-treat population. Of the 114 patients who completed the study, one patient in the ulinastatin group received six doses and one patient each in the placebo group received six and seven doses; all others received the 10 scheduled doses of study medications.
Baseline characteristics
At baseline, the two treatment groups were similar with respect to demographic characteristics, cause of sepsis, number of organs affected, pattern of organ dysfunction, and need for vasopressors or mechanical ventilation (Table 1). Infection was microbiologically confirmed in 26 patients (23 %). Approximately 35 % of patients had multiple organ failure at baseline, 51 % required vasopressors, and 42 % received mechanical ventilation. For details of organisms causing sepsis and antibiotics used, see Electronic Supplementary Material.
Outcomes
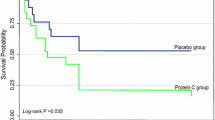
The 28-day mortality, the primary end-point of this study, showed a significant difference (Table 2) in the two treatment groups; there were four deaths (7.3 %) in the ulinastatin group versus 12 deaths (20.3 %) in the placebo group. On stepwise multiple logistic regression, treatment with ulinastatin was found to produce a statistically significant decrease in risk of death (odds ratio 0.26, 95 % confidence limits 0.07–0.95; p = 0.042). Other variables independently associated with mortality were acute renal failure and mechanical ventilation at baseline (Table 3). Of the four deaths in the ulinastatin group one patient each died as a result of ARDS, acute renal failure, refractory shock, and multiple organ failure. Of the 12 deaths in the placebo group five patients died as a result of ARDS, five as a result of refractory shock, and one each as a result of intracranial hemorrhage and multiple organ failure. All deaths were attributed by the investigators to progression of underlying sepsis. The Kaplan–Meier plot for survival in the two groups is shown in Fig. 2.
Among the secondary end-points, there were 6 deaths (10.2 %) in the ulinastatin group (n = 59) in the intention-to-treat population which included all randomized subjects versus 13 deaths (20.6 %) in the control group (n = 63; p = 0.11). New onset of organ dysfunction was seen in 10 subjects in the ulinastatin group and 26 subjects in the placebo group (p = 0.003). Number of ventilator-free days up to day 28 (mean ± SD) was significantly more (19.4 ± 10.6 days) in the ulinastatin group and 10.2 ± 12.5 days in the placebo group (p = 0.019). Mean hospital stay too was less in the ulinastatin group by an average of 12.4 days (p = 0.001).
Complications
Intracranial hemorrhage was the only unexpected serious adverse event in one patient; this patient was from the placebo group. There were no infusion-related adverse events associated with treatment with ulinastatin.
Discussion
This prospective, double-blind, randomized, placebo-controlled trial of ulinastatin in patients with severe sepsis showed that intravenous administration of ulinastatin in a dose of 200,000 units twice daily for 5 days was associated with a reduction in 28-day all-cause mortality (the primary end-point) to 7.3 versus 20.3 % in the placebo control group. A few small studies, published in Chinese-language journals, have shown lower mortality in patients treated with ulinastatin [19, 23, 24]. Small randomized controlled trials have also been conducted by a single group of investigators comparing standard treatment with intravenous administration of ulinastatin in combination with alpha thymosin and found a reduction of mortality in patients with severe sepsis [25–27]. Since these studies have all used a combination of two novel agents, it is unclear whether the survival benefit seen was due to either one of these agents, or the combination. A small Korean study showed that mortality was lower in patients with severe sepsis treated with ulinastatin (18.6 vs. 27 % in the control group) [18]. Our results further corroborate these studies and suggest that treatment with ulinastatin may reduce mortality in severe sepsis in humans.
Highly selective serine protease inhibitors that act on only a few steps in the multipronged inflammatory response involved in the pathogenesis of sepsis like coagulation (tissue factor pathway inhibitor, activated protein C, thrombomodulin, and antithrombin III), complement cascade (C1 inhibitor), or neutrophil elastase (sivelestat) have failed to provide substantial clinical benefit in clinical trials [3–6, 21]. In contrast, ulinastatin inhibits a wide variety of pro-inflammatory serine protease enzymes including trypsin, thrombin, kallikrein, plasmin, cathepsin, neutrophil elastase, neutrophil protease-3, and coagulation factors IXa, Xa, XIa, and XlIa [7–11, 28]. Although the exact mechanism of action of ulinastatin in sepsis is not clear, it is likely that it may attenuate the inflammatory response by acting at multiple sites. In animal models of sepsis, exogenously administered ulinastatin has been shown to reduce levels of TNF-α, IL-1, IL-6, cytokine-induced neutrophil chemoattractant-1 (CINC-1), myeloperoxidase, free oxygen radicals, high mobility group box 1 (HMGB1), interleukin (IL)-6, interleukin-8 (IL-8), malondialdehyde, and soluble intercellular adhesion molecule-1 (sICAM-1) in serum and in organs like lung, kidney, and intestine of rats with lipopolysaccharide-induced SIRS [13–16, 28–34]. Ulinastatin also decreases phosphorylation of p38 mitogen-activated protein kinase (p38-MAPK) which in turn attenuates activation of NF-κB and downregulates expression of the TNF-α gene [33]. Studies in humans too have shown that patients with sepsis treated with intravenous administration of ulinastatin have lower serum levels of pro-inflammatory markers like TNF-α, IL-1β, IL-4, IL-6, and C-reactive protein, while levels of anti-inflammatory cytokine IL-10 was significantly higher [19, 23, 35–37]. It also reduces thrombomodulin levels and decreases endothelial dysfunction [38].
Besides reduction in 28-day all-cause mortality, ulinastatin also showed beneficial effects on some secondary end-points in the present study like new-onset organ dysfunction. Although the duration of vasopressor use was similar in the two groups, ventilator-free days were significantly higher in the ulinastatin group (19.4 vs. 10.2 days), suggesting faster recovery from severe sepsis. This also translated into a shorter mean hospital stay in the ulinastatin group.
No infusion-related adverse effects were seen in the present study. Adverse effects with ulinastatin are rare and were reported in 0.84 % of patients in a Japanese study [39]. These included increased transaminases (0.36 %), eosinophilia or leucopenia (0.16 %), rash (0.13 %), gastrointestinal symptoms (0.08 %), fever (0.02 %), and local irritation at the injection site (0.02 %). These were reported in less ill patients with pancreatitis or when the drug was used prophylactically in patients undergoing endoscopic retrograde pancreatography, for which the drug is licensed in Japan. None of these effects were seen in the present study, probably because patients were too sick to complain of these symptoms.
Our study has some limitations. Firstly, although larger than previous randomized controlled studies with ulinastatin, the number of patients is relatively small, thereby limiting the power of this study. However, power of a study is more relevant for interpreting results of clinical trials that show no difference between the two treatment arms. Secondly, patients aged >60 years were excluded. This is because unlike in western countries, the number of elderly patients seeking care in Indian ICUs is comparatively small, and limitation of care is often opted for by the family in such cases after a few days of ICU stay owing to socio-economic and cultural reasons [40, 41]. Thirdly, the baseline APACHE II scores were low although patients had significant organ dysfunction, as has also been reported in previous studies from India [42, 43]. This is because the APACHE II score allocates more points to old age than for maximum possible physiological derangement (5 points for age 65–74 years and 6 for age >75 years) [44]. Moreover, septic encephalopathy is also more common in the elderly [45], and the highest possible points for any single physiological variable in the APACHE II system are assigned to the level of consciousness (APACHE II points = 15 minus Glasgow coma score) [44]. These two factors alone could add up to 18 points per patient (6 for age and 12 for coma), accounting for high APACHE II scores in studies from western countries. These differences may limit the generalizability of our results to some extent. However, our study had some strengths too. Whereas all previous studies with ulinastatin in sepsis have been single-center studies, this was a multicenter study. Use of a double-blind design was another strength.
In conclusion, this prospective, multicenter, randomized, double-blind, placebo-controlled pilot study in patients with severe sepsis investigated a novel therapy directed against the systemic inflammatory response. We found that 5-day treatment with intravenous administration of ulinastatin in patients with severe sepsis, when started within 48 h of organ dysfunction, resulted in a reduction in 28-day all-cause mortality to 7.3 % from 20.3 % observed in the placebo group. The reduction in mortality to 10.2 % from 20.6 % in the intention-to-treat population, however, was short of statistical significance (p = 0.11). We also found a reduction in new onset of organ dysfunction, days of mechanical ventilation, and hospital stay. A larger randomized controlled study with ulinastatin is needed to further confirm the survival benefit seen in this pilot study and also to investigate its mechanism of action in humans.
References
Angus DC, Linde-Zwirble WT, Lidicker J, Clermont G, Carcillo J, Pinsky MR (2001) Epidemiology of severe sepsis in the United States: analysis of incidence, outcome, and associated costs of care. Crit Care Med 29:1303–1310
Vincent JL, Rello J, Marshall J, Silva E, Anzueto A, Martin CD, Moreno R, Lipman J, Gomersall C, Sakr Y, Reinhart K (2009) International study of the prevalence of infection and outcomes of infections in intensive care units. JAMA 302:2323–2329
Rittirsch D, Flierl MA, Ward PA (2008) Harmful molecular mechanisms in sepsis. Nat Rev Immunol 8:776–787
Van der Poll T, Opal SM (2008) Host-pathogen interaction in sepsis. Lancet Infect Dis 8:32–43
Levi M, van der Poll T (2013) Endothelial injury in sepsis. Intensive Care Med 39:1839–1842
Angus D, van der Poll T (2013) Severe sepsis and septic shock. N Engl J Med 369:840–851
Inoue K, Takano H (2011) Urinary trypsin inhibitor, an alternative therapeutic option for inflammatory disorders. In: Nagal A (ed) Inflammatory diseases—a modern perspective. InTech, Croatia. ISBN: 978-953-307-444-3. http://www.intechopen.com/books/inflammatory-diseases-a-modernperspective/urinary-trypsin-inhibitor-an-alternative-therapeutic-option-for-inflammatory-disorders. Accessed 1 June 2013
Sharony R, Yu PJ, Park J, Galloway AC, Mignatti P, Pintucci G (2010) Protein targets of inflammatory serine proteases and cardiovascular disease. J Inflamm (Lond) 7:45
Kessenbrock K, Dau T, Jenne DE (2011) Tailor-made inflammation: how neutrophil serine proteases modulate the inflammatory response. J Mol Med 89:23–28
Pugia MJ, Lott JA (2005) Pathophysiology and diagnostic value of urinary trypsin inhibitors. Clin Chem Lab Med 43:1–16
Shigetomi H, Onogi A, Kajiwara H, Yoshida S, Furukawa N, Haruta S, Tanase Y, Kanayama S, Noguchi T, Yamada Y, Oi H, Kobayashi H (2010) Anti-inflammatory actions of serine protease inhibitors containing the Kunitz domain. Inflamm Res 59:679–687
Lim YP, Bendelja K, Opal SM, Siryaporn E, Hixson DC, Palardy JE (2003) Correlation between mortality and the levels of inter-alpha inhibitors in the plasma of patients with severe sepsis. J Infect Dis 188:919–926
Wakahara K, Kobayashi H, Yagyu T, Matsuzaki H, Kondo T, Kurita N et al (2005) Bikunin suppresses lipopolysaccharide-induced lethality through down-regulation of tumor necrosis factor-α and interleukin-1β in macrophages. J Infect Dis 191:930–938
Ueki M, Taie S, Chujo K, Asaga T, Iwanaga Y, Ono J, Maekawa N (2007) Urinary trypsin inhibitor reduces inflammatory response in kidney induced by lipopolysaccharide. J Biosci Bioeng 104:315–320
Tanaka R, Fujita M, Tsuruta R, Fujimoto K, Aki HS, Kumagai K et al (2010) Urinary trypsin inhibitor suppresses excessive generation of superoxide anion radical, systemic inflammation, oxidative stress, and endothelial injury in endotoxemic rats. Inflamm Res 59:597–606
Huang N, Wang F, Wang Y, Hou J, Li J, Deng X (2013) Ulinastatin improves survival of septic mice by suppressing inflammatory response and lymphocyte apoptosis. J Surg Res 182:296–302
Cao YZ, Tu YY, Chen X, Wang BL, Zhong YX, Liu MH (2012) Protective effect of ulinastatin against murine models of sepsis: inhibition of TNF-α and IL-6 and augmentation of IL-10 and IL-13. Exp Toxicol Pathol 64:543–547
Moon SW, Lee SW, Hong YS, Park DW, Jang IJ, Yoon YH, Lim SI (2009) The effects of urinary trypsin inhibitor on the outcomes of severe sepsis and septic shock patients. J Korean Soc Emerg Med 20:80–85
Shao Y, Zhang L, Deng L, Yao H (2005) Clinical study on effects of ulinastatin on patients with systemic inflammatory response syndrome. Zhongguo Wei Zhong Bing Ji Jiu Yi Xue 17:228–230
Opal SM, Lim YP, Cristofaro P, Artenstein AW, Kessimian N, DelSesto D, Parejo N, Palardy JE, Siryaporn E (2011) Inter-alpha inhibitor proteins: a novel therapeutic strategy for experimental anthrax infection. Shock 35:42–44
Antonopoulou A, Giamarellos-Bourboulis EJ (2011) Immunomodulation in sepsis: state of the art and future perspective. Immunotherapy 3:117–128
Bernard GR, Vincent JL, Laterre PF, LaRosa SP, Dhainaut JF, Lopez-Rodriguez A et al (2001) Efficacy and safety of recombinant human activated protein C for severe sepsis. N Engl J Med 344:699–709
Wu TJ, Zhang LN, Kang CC (2013) The effect of ulinastatin on disbalance of inflammation and immune status in patients with severe sepsis. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue 25:219–223
Yang H, Zhen XF, Li HY (2006) Clinical observation of ulinastatin in the treatment of multiorgan dysfunction syndrome. J Guangdong Coll Pharm 6:036
Chen H, He MY, Li YM (2009) Treatment of patients with severe sepsis using ulinastatin and thymosin α1: a prospective, randomized, controlled pilot study. Chin Med J 122:883–888
Li YM, Chen H, Li X, Zhou W, He MY, Chiriva-Internati M, Wachtel MS, Frezza EE (2009) A new immunomodulatory therapy for severe sepsis: ulinastatin plus thymosin alpha 1. J Intensive Care Med 24:47–53
Zhang Y, Chen H, Li YM, Zheng SS, Chen YG, Li LJ, Zhou L, Xie HY, Praseedom RK (2008) Thymosin alpha1- and ulinastatin-based immunomodulatory strategy for sepsis arising from intra-abdominal infection due to carbapenem-resistant bacteria. J Infect Dis 198:723–730
Nakatani K, Takeshita S, Tsujimoto H, Kawamura Y, Sekine I (2001) Inhibitory effect of serine protease inhibitors on neutrophil-mediated endothelial injury. J Leukoc Biol 69:241–247
Inoue K, Takano H, Shimada A, Yanagisawa R, Sakurai M, Yoshino S, Sato H, Yoshikawa T (2005) Urinary trypsin inhibitor protects against systemic inflammation induced by lipopolysaccharide. Mol Pharmacol 67:673–680
Bae HB, Jeong CW, Li M, Kim HS, Kwak SH (2012) Effects of urinary trypsin inhibitor on lipopolysaccharide-induced acute lung injury in rabbits. Inflammation 35:176–182
Tani T, Aoki H, Yoshioka T, Lin KJ, Kodama M (1993) Treatment of septic shock with a protease inhibitor in a canine model: a prospective, randomized, controlled trial. Crit Care Med 21:925–930
Inoue K, Takano H, Yanagisawa R, Yoshikawa T (2008) Protective effects of urinary trypsin inhibitor on systemic inflammatory response induced by lipopolysaccharide. J Clin Biochem Nutr 43:139–142
Zhang X, Liu F, Liu H, Cheng H, Wang W, Wen Q, Wang Y (2011) Urinary trypsin inhibitor attenuates lipopolysaccharide-induced acute lung injury by blocking the activation of p38 mitogen-activated protein kinase. Inflamm Res 60:569–575
Massberg S, Grahl L, von Bruehl ML, Manukyan D, Pfeiler S, Goosmann C, Brinkmann V, Lorenz M, Bidzhekov K, Khandagale AB, Konrad I, Kennerknecht E, Reges K, Holdenrieder S, Braun S, Reinhardt C, Spannagl M, Preissner KT, Engelmann B (2010) Reciprocal coupling of coagulation and innate immunity via neutrophil serine proteases. Nat Med 16:887–896
Endo S, Inada K, Taki K, Hoshi S, Yoshida M (1990) Inhibitory effects of ulinastatin on the production of cytokines: implications for the prevention of septicemic shock. Clin Ther 12:323–326
Kawai S, Sakayori S, Watanabe H, Kobayashi H (1990) Usefulness of a protease inhibitor (urinastatin) in ARDS with infectious diseases. Nihon Kyobu Shikkan Gakkai Zasshi 28:843–851
Aibiki M, Cook JA (1997) Ulinastatin, a human trypsin inhibitor, inhibits endotoxin-induced thromboxane B2 production in human monocytes. Crit Care Med 25:430–434
Abe M, Ishikawa M, Soga Y, Suga H, Nakagawa T, Suzuki T (2004) Acute and high dose therapy of urinary trypsin inhibitor could inhibit vascular endothelial cell disorders in critical illness. Crit Care 8(suppl 1):199
Luo PF, Ren Y, Liu Y-L, Xia Z-F (2001) Ulinastatin and thymosin as immune modulators for the treatment of sepsis. Cochrane Database Syst Rev (7):CD009940. doi:10.1002/14651858.CD009940
Kapadia F, Singh M, Divatia J, Vaidyanathan P, Udwadia FE, Raisinghaney SJ, Limaye HS, Karnad DR (2005) End of life limitation and withdrawal of intensive therapy at the end of life: practices in intensive care units in Mumbai, India. Crit Care Med 33:1272–1275
Kulkarni HS, Kulkarni KR, Mallampalli A, Parkar SR, Karnad DR, Guntupalli KK (2011) Comparison of anxiety, depression, and post-traumatic stress symptoms in relatives of ICU patients in an American and an Indian public hospital. Indian J Crit Care Med 15:147–156
Panchabhai TS, Dangayach NS, Krishnan A, Kothari VM, Karnad DR (2009) Oropharyngeal cleansing with 0.2% chlorhexidine for prevention of nosocomial pneumonia in critically ill patients: an open-label randomized trial with 0.01% potassium permanganate as control. Chest 135:1150–1156
Todi S, Chatterjee S, Sahu S, Bhattacharyya M (2010) Epidemiology of severe sepsis in India: an update. Crit Care 14(Suppl 1):382
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: a severity of disease classification system. Crit Care Med 13:818–829
van den Boogaard M, Pickkers P, Slooter AJ, Kuiper MA, Spronk PE, van der Voort PH, van der Hoeven JG, Donders R, van Achterberg T, Schoonhoven L (2012) Development and validation of PRE-DELIRIC (PREdiction of DELIRium in ICu patients) delirium prediction model for intensive care patients: observational multicentre study. Br Med J 344:e420
Conflicts of interest
This study was funded by Bharat Serums and Vaccines Limited, India who provided the study medications, administrative assistance, and study grants to participating centers and funded the statistical analysis by an external statistician.
Dilip R. Karnad was responsible for the study design and helped in the analysis of data and preparing the manuscript. He has received consulting fees from Bharat Serum and Vaccines Limited. He has also received consulting fees from Quintiles Cardiac Safety Services and honoraria for lectures from Abbott Nutrition, India and Bharat Serums and Vaccines Limited. All other authors participated as investigators in the clinical trial and also helped in preparing and reviewing the manuscript; their institutions received grants for this clinical trial. No other conflicts of interest are declared by other authors.
Author information
Authors and Affiliations
Corresponding author
Additional information
Take-home message: Ulinastatin, a protease inhibitor, inhibits several pro-inflammatory proteases and decreases inflammatory cytokine levels and mortality in experimental sepsis. In this pilot study, intravenous administration of ulinastatin (200,000 IU 12 hourly for 5 days) reduced mortality, new onset of organ dysfunction, duration of mechanical ventilation and hospital stay in patients with severe sepsis when started within 48 h of onset of failure of one or more organs.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
About this article
Cite this article
Karnad, D.R., Bhadade, R., Verma, P.K. et al. Intravenous administration of ulinastatin (human urinary trypsin inhibitor) in severe sepsis: a multicenter randomized controlled study. Intensive Care Med 40, 830–838 (2014). https://doi.org/10.1007/s00134-014-3278-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-014-3278-8