Abstract
Purpose
National monitoring of variation in the quality of infection control in paediatric intensive care units (PICUs) requires comparisons of risk-adjusted rates. To inform the development of a national monitoring system, we evaluated the effects of risk-adjustment and outcome definition on comparisons of blood-stream infection (BSI) rates in PICU, using linkage of risk-factor data captured by national audit (PICANet) with laboratory records of BSI.
Methods
Admission data for two children’s hospitals 2003–2010 were extracted from PICANet and linked using multiple identifiers with laboratory BSI records. We calculated trends of PICU-acquired BSI, defined as BSI occurring between at least 2 days after admission until up to 2 days following discharge. In one PICU, we compared rates of all PICU-acquired BSI with clinically significant PICU-acquired BSI submitted to the national surveillance system.
Results
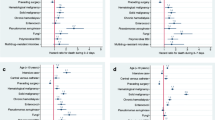
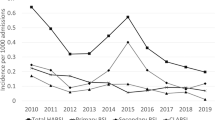
Of 20,924 admissions, 1,428 (6.8 %) were linked to 1,761 PICU-acquired BSI episodes. The crude incidence rate-ratio for PICU-acquired BSI between PICUs was 1.15 [95 % confidence interval (CI) 1.05–1.26] but increased to 1.26 (1.14–1.39) after risk-adjustment. Rates of PICU-acquired BSI were 13.44 (95 % CI 12.60–14.28) per 1,000 bed-days at PICU 1 and 18.05 (95 % CI 16.80–19.32) at PICU 2. Of PICU-acquired BSI at PICU 2, 41 % was classified as clinically significant. Rates of PICU-acquired BSI decreased by 10 % per year between 2003 and 2010 for skin organisms and 8 % for non-skin organisms.
Conclusions
Risk-adjustment and standardisation of outcome measures are essential for fair comparisons of BSI rates between PICUs. Linkage of risk-factor data and BSI surveillance is feasible and could allow national risk-adjusted monitoring.



Similar content being viewed by others
Notes
Full model: log(infections) = β1 × quarter-year of admission + β2 × PICU + β3 × admission type + β4 × diagnosis group + β5 × renal support + β6 × sex + β7 × age + β8 × PIM2 + β9 × admission source + β10 × mechanical ventilation + β11 × quarter of year + log(length of stay).
References
Lakshmi KS, Jayashree M, Singhi S, Ray P (2007) Study of nosocomial primary bloodstream infections in a pediatric intensive care unit. J Trop Pediatr 53(2):87–92. doi:10.1093/tropej/fml073
Abou Elella R, Najm H, Balkhy H, Bullard L, Kabbani M (2010) Impact of bloodstream infection on the outcome of children undergoing cardiac surgery. Pediatr Cardiol 31(4):483–489. doi:10.1007/s00246-009-9624-x
Elward A, Hollenbeak C, Warren D, Fraser V (2005) Attributable cost of nosocomial primary bloodstream infection in pediatric intensive care unit patients. Pediatrics 115(4):868
Yogaraj J, Elward A, Fraser V (2002) Rate, risk factors, and outcomes of nosocomial primary bloodstream infection in pediatric intensive care unit patients. Pediatrics 110(3):481
Pronovost P, Goeschel C, Colantuoni E, Watson S, Lubomski L, Berenholtz S, Thompson D, Sinopoli D, Cosgrove S, Sexton J (2010) Sustaining reductions in catheter related bloodstream infections in Michigan intensive care units: observational study. BMJ 340:c309
Bhutta A, Gilliam C, Honeycutt M, Schexnayder S, Green J, Moss M, Anand K (2007) Reduction of bloodstream infections associated with catheters in paediatric intensive care unit: stepwise approach. BMJ 334(7589):362–365
Miller MR, Griswold M, Harris JM II, Yenokyan G, Huskins WC, Moss M, Rice TB, Ridling D, Campbell D, Margolis P, Muething S, Brilli RJ (2010) Decreasing PICU catheter-associated bloodstream infections: nACHRI’s quality transformation efforts. Pediatrics 125(2):206–213. doi:10.1542/peds.2009-1382
Department of Health (2005) Saving Lives: a delivery programme to reduce healthcare associated infections including MRSA. Department of Health, London
Pronovost PJ, Berenholtz SM, Needham DM (2008) Translating evidence into practice: a model for large scale knowledge translation. BMJ 337:a1714. doi:10.1136/bmj.a1714
Lilford R, Mohammed MA, Spiegelhalter D, Thomson R (2004) Use and misuse of process and outcome data in managing performance of acute medical care: avoiding institutional stigma. Lancet 363(9415):1147–1154
Davenport RJ, Dennis MS, Warlow CP (1996) Effect of correcting outcome data for case mix: an example from stroke medicine. BMJ 312(7045):1503–1505
García Álvarez L, Aylin P, Tian J, King C, Catchpole M, Hassall S, Whittaker-Axon K, Holmes A (2011) Data linkage between existing healthcare databases to support hospital epidemiology. J Hosp Infect 79(3):231–235
Lamagni T, Potz N, Powell D, Pebody R, Wilson J, Duckworth G (2011) Mortality in patients with meticillin-resistant Staphylococcus aureus bacteraemia, England 2004–2005. J Hosp Infect 77(1):16–20
Universities of Leeds and Leicester (2012) Paediatric Intensive Care Audit Network National Report 2009–2011. ISBN 9780853163121 Available:http://wwwpicanetorguk/Documents/General/Annual_Report_2012/Ninth_PICANet_Annual_Report_2009_2011_Summary_Reportpdf Accessed 19 September 2012
Slater A, Shann F, Pearson G (2003) PIM2: a revised version of the Paediatric Index of Mortality. Intens Care Med 29(2):278–285
Safdar N, Maki D (2004) The pathogenesis of catheter-related bloodstream infection with noncuffed short-term central venous catheters. Intens Care Med 30(1):62–67. doi:10.1007/s00134-003-2045-z
O’Grady N, Alexander M, Dellinger E, Gerberding J, Heard S, Maki D, Masur H, McCormick R, Mermel L, Pearson M (2002) Guidelines for the prevention of intravascular catheter-related infections. Am Acad Pediatr Policy 110(5):e51–e74
Horan TC, Andrus M, Dudeck MA (2008) CDC/NHSN surveillance definition of health care—associated infection and criteria for specific types of infections in the acute care setting. Am J Infect Control 36(5):309–332
StataCorp (2009) Stata statistical software: release 11. StataCorp LP, College Station
Shann F, Pearson G, Slater A, Wilkinson K (1997) Paediatric index of mortality (PIM): a mortality prediction model for children in intensive care. Intens Care Med 23(2):201–207
Harron K, Ramachandra G, Mok Q, Gilbert R (2011) Consistency between guidelines and reported practice for reducing the risk of catheter-related infection in British paediatric intensive care units. Intens Care Med 37(10):1641–1647
Holman CDAJ, Preen DB, Baynham NJ, Finn JC, Semmens JB (2005) A multipurpose comorbidity scoring system performed better than the Charlson index. J Clin Epidemiol 58(10):1006–1014
Armitage J, van der Meulen J (2010) Identifying co-morbidity in surgical patients using administrative data with the Royal College of Surgeons Charlson Score. Brit J Surg 97(5):772–781
Quan H, Sundararajan V, Halfon P, Fong A, Burnand B, Luthi JC, Saunders LD, Beck CA, Feasby TE, Ghali WA (2005) Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Med Care Nov 43(11):1130–1139
Preen DB, Holman CDAJ, Spilsbury K, Semmens JB, Brameld KJ (2006) Length of comorbidity lookback period affected regression model performance of administrative health data. J Clin Epidemiol 59(9):940–946
Centers for Disease Control and Prevention (2012) Central Line-Associated Bloodstream Infection (CLABSI) event: guidelines and procedures for monitoring CLABSI. National Healthcare Safety Network (NHSN) manual Atlanta, GA: NHSN (http://www.cdc.gov/nhsn/PDFs/pscManual/4PSC_CLABScurrent.pdf)
Laupland KB, Gregson DB, Vanderkooi OG, Ross T, Kellner JD (2009) The changing burden of pediatric bloodstream infections in Calgary, Canada, 2000–2006. Pediatr Infect Dis J 28(2):114
Kollef MH, Zilberberg MD, Shorr AF, Vo L, Schein J, Micek ST, Kim M (2011) Epidemiology, microbiology and outcomes of healthcare-associated and community-acquired bacteremia: a multicenter cohort study. J Infection 62(2):130–135
Acknowledgments
The authors would like to thank Tom Fleming (PICANet), Paul Lock and Joanna Bell (Great Ormond Street Hospital), Ollie Bagshaw and Adrian Bigland (Birmingham Children’s Hospital) for helpful advice, contribution of data and facilitation of data retrieval for this paper. We would like to thank all the staff in participating hospitals who have collected data for PICANet. We are grateful to the UK Paediatric Intensive Care Society for continued support and to the members of the PICANet Steering Group and Clinical Advisory Group who are listed on our website http://www.picanet.org.uk/participants.html. This work was supported by funding from the National Institute for Health Research Health Technology Assessment (NIHR HTA) programme (Project number 08/13/47). The views and opinions expressed therein are those of the authors and do not necessarily reflect those of the HTA programme, NIHR, NHS or the Department of Health. The authors state no conflicts of interest. PICANet is funded by the National Clinical Audit and Patient Outcomes Programme via Healthcare Quality Improvement Partnership (HQIP), Health Commission Wales Specialised Services, NHS Lothian/National Service Division NHS Scotland, the Royal Belfast Hospital for Sick Children, Our Lady’s Children’s Hospital, Crumlin, Children’s University Hospital, Temple Street and The Harley Street Clinic, London.
Ethical approval
Collection of personally identifiable data has been approved by the National Information Governance Board (Formerly the Patient Information Advisory Group) http://www.nigb.nhs.uk/s251/registerapp and ethical approval granted by the Trent Medical Research Ethics Committee, ref. 05/MRE04/17. Consent for the use of the data in this study was obtained by the PICANet unit leads.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Harron, K., Wade, A., Muller-Pebody, B. et al. Risk-adjusted monitoring of blood-stream infection in paediatric intensive care: a data linkage study. Intensive Care Med 39, 1080–1087 (2013). https://doi.org/10.1007/s00134-013-2841-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-013-2841-z