Abstract
Objective
Although bolus thermodilution technique for cardiac output (CO) measurement has widespread acceptance, new systems are currently available. We evaluated a continuous CO system (TruCCOMS, Aortech International Inc.) that operates on the thermal conservation principle and we compared it with the reference standard transit time flow measurement (TTFM).
Materials and methods
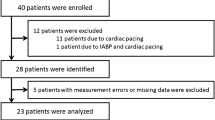
Nine consecutive cardiac surgery patients were evaluated. After general anesthesia and intubation, a TruCCOMS catheter was percutaneously placed in the pulmonary artery (PA). After median sternotomy and pericardiotomy, a TTFM probe was placed around the main PA. Right ventricular (RV) CO measurements were recorded with both TruCCOMS and TTFM at different times: before cardiopulmonary bypass (CPB) (T0), during weaning from CPB (T1), and prior to sternal closure (T2). Data analysis included paired student t test, Pearson correlation test, and Bland–Altman plotting.
Results
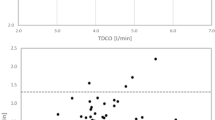
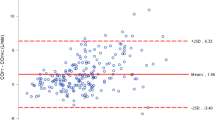
TruCCOMS CO values were significantly lower at T0 (TruCCOMS 4.0 ± 1.0 vs. TTFM 4.5 ± 1.0 L/min; P < 0.0001) and T1 (TruCCOMS 3.6 ± 0.5 vs. TTFM 4.2 ± 0.7 L/min; P < 0.0001), and comparable at T2 (TruCCOMS 4.5 ± 0.7 vs. TTFM 4.6 ± 0.8 L/min; P = 0.4). Pearson test showed a significant correlation between TruCCOMS and TTFM CO measurements (RT0 = 0.9, RT1 = 0.8, RT2 = 0.6; P < 0.0001). Bland–Altmann plotting showed a bias of −0.53 ± 0.43 L (−12%) at T0, −0.64 ± 0.43 L (−14.5%) at T1, and −0.1 ± 0.66 L (−0.8%) at T2.
Conclusion
Although TruCCOMS may significantly underestimate CO, measurement trends correlate with TTFM. For this reason, a negative trend in RV output should trigger more specific diagnostic procedures.



Similar content being viewed by others
References
D’Ancona G, Karamanoukian H, Ricci M, Salerno T, Bergsland J (2001) Intraoperative graft patency verification in cardiac and vascular surgery. Futura, New York
Yelderman ML, Ramsay MA, Quinn MD (1992) Continuous thermodilution cardiac output measurement in intensive care unit patients. J Cardiothorac Vasc Anesth 6:270–274
Haller M, Zöllner C, Briegel J, Forst H (1995) Evaluation of a new continuous thermodilution cardiac output monitor in critically ill patients: a prospective criterion standard study. Crit Care Med 23:860–866
Boldt J, Menges T, Wollbrück M (1994) Is continuous cardiac output measurement using thermodilution reliable in the critically ill patient? Crit Care Med 22:1913–1918
Jacquet L, Hanique G, Glorieux D (1996) Analysis of the accuracy of continuous thermodilution cardiac output measurement. Intensive Care Med 22:1125–1129
Leather HA, Vuylsteke A, Bert C, M’Fam W, Segers P, Sergeant P, Vandermeersch E, Wouters PF (2004) Evaluation of a new continuous cardiac output monitor in off-pump coronary artery surgery. Anaesthesia 59:385–389
Padua G, Canestrelli G, Pala G, Sechi D, Spanu MC (2003) Original insight into continuous cardiac output monitoring: “TruCCOMS”. Correlation with other methods. Minerva Anestesiol 69:617–624
Thierry S, Thebert D, Brocas E, Razzaghi F, Van De Louw A, Loisance D, Teboul JL (2003) Evaluation of a new invasive continuous cardiac output monitoring system: the truCCOMS system. Intensive Care Med 29:2096–2099
Critchley LAH, Critchley JAJH (1999) A meta-analysis of studies using bias and precision statistics to compare cardiac output measurement techniques. J Clin Monit Comput 15:85–91
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
D’Ancona, G., Parrinello, M., Santise, G. et al. Intraoperative validation of a new system for invasive continuous cardiac output measurement. Intensive Care Med 35, 943–947 (2009). https://doi.org/10.1007/s00134-009-1422-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-009-1422-7