Abstract
Background
Degenerative lumbar spondylolisthesis (DSPL), as opposed to other degenerative spinal conditions, is disregarded in the assessment of hip stability after total hip arthroplasty (THA). This study aimed to determine whether patients with DSPL have different acetabular anteversion compared to patients with normal spine before and following THA.
Methods
Preoperative and postoperative 6‑month lateral pelvic radiographs in standing and sitting positions from 91 patients who underwent primary THA were retrospectively compared for spinopelvic parameters between patients with DSPL (n = 31) and with normal spine (n = 34).
Results
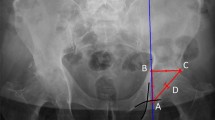
Compared to control patients in the standing position, patients with DSPL had significantly increased preoperative pelvic tilt (24° in DSPL vs. 8° in controls; p < 0.01), pelvic–femoral angle (194° in DSPL vs. 174° in controls; p < 0.05), decreased lumbar lordosis (35° in DSPL vs. 43° in controls; p < 0.05), increased postoperative pelvic tilt (22° in DSPL vs. 7° in controls; p < 0.01), pelvic–femoral angle (187° in DSPL vs. 179° in controls; p < 0.05), and acetabular anteversion (31° in DSPL vs. 23° in controls; p < 0.05). Preoperative (p = 0.181) and postoperative (p = 0.201) sitting pelvic tilt did not differ. There were positive correlations between preoperative standing pelvic tilt and postoperative standing acetabular anteversion, pelvic–femoral angle, and combined sagittal index (CSI) in DSPL (R2 = 0.8416; R2 = 0.9180; R2 = 0.9459, respectively, p < 0.01) and in controls (R2 = 0.6872; R2 = 0.6176; R2 = 0.7129, respectively, p < 0.01).
Conclusion
While the imbalance of seated sagittal plane is usually insignificant and compensable, the mechanism by which DSPL patients achieve a standing posture is different from control patients, with more hip extension and posterior tilt of the pelvis. Special attention should be paid to the risk of impingement caused by the increase of acetabular anteversion in the postoperative standing position.
Zusammenfassung
Hintergrund
Die degenerative lumbale Spondylolisthesis (DSPL) wird im Gegensatz zu anderen degenerativen Wirbelsäulenerkrankungen bei der Beurteilung der Hüftstabilität nach Hüfttotalendoprothese (HTEP) vernachlässigt. Ziel dieser Studie war es, festzustellen, ob Patienten mit DSPL im Vergleich zu Patienten mit normaler Wirbelsäule vor und nach der HTEP eine andere azetabuläre Anteversion aufweisen.
Methoden
Präoperative und postoperative 6‑Monats-Röntgenaufnahmen des lateralen Beckens in stehender und sitzender Position von 91 Patienten, die sich einer primären HTEP unterzogen, wurden retrospektiv hinsichtlich spinopelviner Parameter zwischen Patienten mit DSPL (n = 31) und normaler Wirbelsäule (n = 34) verglichen.
Ergebnisse
Im Vergleich zu den Kontrollpatienten in stehender Position wiesen Patienten mit DSPL eine signifikant erhöhte präoperative Beckenkippung (24° bei DSPL vs. 8° bei der Kontrollgruppe; p < 0,01), einen Becken-Oberschenkel-Winkel (194° bei DSPL vs. 174° bei der Kontrollgruppe; p < 0,05), eine verringerte Lendenlordose (35° bei DSPL vs. 43° bei der Kontrollgruppe; p < 0,05) sowie eine erhöhte postoperative Beckenkippung (22° bei DSPL vs. 7° bei der Kontrollgruppe; p < 0,01), Becken-Oberschenkel-Winkel (187° bei DSPL vs. 179° bei der Kontrollgruppe; p < 0,05) und Azetabulum-Anteversion (31° bei DSPL vs. 23° bei der Kontrollgruppe; p < 0,05). Die präoperative (p = 0,181) und postoperative (p = 0,201) Beckenkippung im Sitzen unterschied sich nicht. Es gab positive Korrelationen zwischen der präoperativen Beckenkippung im Stehen und der postoperativen Azetabulum-Anteversion im Stehen, dem Becken-Oberschenkel-Winkel und dem kombinierten Sagittal-Index (CSI) bei DSPL (R2 = 0,8416; R2 = 0,9180; R2 = 0,9459; jeweils p < 0,01) und bei der Kontrollgruppe (R2 = 0,6872; R2 = 0,6176; R2 = 0,7129; jeweils p < 0,01).
Schlussfolgerung
Während die Dysbalance der Sagittalebene im Sitzen in der Regel unbedeutend und kompensierbar ist, unterscheidet sich der Mechanismus, durch den DSPL-Patienten eine stehende Haltung erreichen, von Kontrollpatienten, durch mehr Hüftextension und eine posteriorere Kippung des Beckens. Besonderes Augenmerk sollte auf das Impingement-Risiko gelegt werden, das durch die Zunahme der azetabulären Anteversion in der postoperativen Stehposition entsteht.









Similar content being viewed by others
Abbreviations
- AA:
-
Acetabular anteversion
- AI:
-
Ante-inclination
- BMI:
-
Body mass index
- CSI:
-
Combined sagittal index
- DSPL:
-
Degenerative lumbar spondylolisthesis
- ICC:
-
Intraclass correlation coefficient
- IRB:
-
Institutional review board
- LL:
-
Lumbar lordosis
- PFA:
-
Pelvic-femoral angle
- PI:
-
Pelvic incidence
- PT:
-
Pelvic tilt
- SS:
-
Sacral slope
- THA:
-
Total hip arthroplasty
References
Heckmann N, McKnight B, Stefl M, Trasolini NA, Ike H, Dorr LD (2018) Late dislocation following total hip arthroplasty: spinopelvic imbalance as a causative factor. J Bone Joint Surg Am 100(21):1845–1853
Buckland AJ, Ayres EW, Shimmin AJ, Bare JV, McMahon SJ, Vigdorchik JM (2020) Prevalence of sagittal spinal deformity among patients undergoing total hip arthroplasty. J Arthroplasty 35(1):160–165
Ellenrieder M, Bader R, Bergschmidt P, Frohlich S, Mittelmeier W (2015) Coexistent lumbar spine disorders have a crucial impact on the clinical outcome after total hip replacement. J Orthop Sci 20(6):1046–1052
Lewinnek GE, Lewis JL, Tarr R, Compere CL, Zimmerman JR (1978) Dislocations after total hip-replacement arthroplasties. J Bone Joint Surg Am 60(2):217–220
DelSole EM, Vigdorchik JM, Schwarzkopf R, Errico TJ, Buckland AJ (2017) Total hip arthroplasty in the spinal deformity population: does degree of sagittal deformity affect rates of safe zone placement, instability, or revision? J Arthroplasty 32(6):1910–1917
Tezuka T, Heckmann ND, Bodner RJ, Dorr LD (2019) Functional safe zone is superior to the Lewinnek safe zone for total hip arthroplasty: why the Lewinnek safe zone is not always predictive of stability. J Arthroplasty 34(1):3–8
He LC, Wang YX, Gong JS, Griffith JF, Zeng XJ, Kwok AW, Leung JC, Kwok T, Ahuja AT, Leung PC (2014) Prevalence and risk factors of lumbar spondylolisthesis in elderly Chinese men and women. Eur Radiol 24(2):441–448
Warashina H, Kato M, Kitamura S, Kusano T, Hasegawa Y (2019) The progression of osteoarthritis of the hip increases degenerative lumbar spondylolisthesis and causes the change of spinopelvic alignment. J Orthop 16(4):275–279
Sasagawa T, Nakamura T (2016) Associated factors for lumbar degenerative spondylolisthesis in Japanese patients with osteoarthritis of the hip: a radiographic study. Asian Spine J 10(5):935–939
Blizzard DJ, Sheets CZ, Seyler TM, Penrose CT, Klement MR, Gallizzi MA, Brown CR (2017) The impact of lumbar spine disease and deformity on total hip arthroplasty outcomes. Orthopedics 40(3):e520–e525
Malkani AL, Garber AT, Ong KL, Dimar JR, Baykal D, Glassman SD, Cochran AR, Berry DJ (2018) Total hip arthroplasty in patients with previous lumbar fusion surgery: are there more dislocations and revisions? J Arthroplasty 33(4):1189–1193
Buckland AJ, Puvanesarajah V, Vigdorchik J, Schwarzkopf R, Jain A, Klineberg EO, Hart RA, Callaghan JJ, Hassanzadeh H (2017) Dislocation of a primary total hip arthroplasty is more common in patients with a lumbar spinal fusion. Bone Joint J 99-B(5):585–591
Esposito CI, Miller TT, Kim HJ, Barlow BT, Wright TM, Padgett DE, Jerabek SA, Mayman DJ (2016) Does degenerative lumbar spine disease influence femoroacetabular flexion in patients undergoing total hip arthroplasty? Clin Orthop Relat Res 474(8):1788–1797
Berliner JL, Esposito CI, Miller TT, Padgett DE, Mayman DJ, Jerabek SA (2018) What preoperative factors predict postoperative sitting pelvic position one year following total hip arthroplasty? Bone Joint J 100-B(10):1289–1296
Luthringer TA, Vigdorchik JM (2019) A preoperative workup of a “hip-spine” total hip arthroplasty patient: a simplified approach to a complex problem. J Arthroplasty 34(7S):S57–S70
Sultan AA, Khlopas A, Piuzzi NS, Chughtai M, Sodhi N, Mont MA (2018) The impact of Spino-pelvic alignment on total hip arthroplasty outcomes: a critical analysis of current evidence. J Arthroplasty 33(5):1606–1616
Queally JM, Abdulkarim A, Mulhall KJ (2009) Total hip replacement in patients with neurological conditions. J Bone Joint Surg Br 91(10):1267–1273
Wagner ER, Kamath AF, Fruth KM, Harmsen WS, Berry DJ (2016) Effect of body mass index on complications and reoperations after total hip arthroplasty. J Bone Joint Surg Am 98(3):169–179
Koslosky E, Gendelberg D (2020) Classification in Brief: The Meyerding Classification System of Spondylolisthesis. Clin Orthop Relat Res 478(5):1125–1130
Lazennec JY, Brusson A, Rousseau MA (2013) Lumbar-pelvic-femoral balance on sitting and standing lateral radiographs. Orthop Traumatol Surg Res 99(1 Suppl):S87–103
Lee SH, Lim CW, Choi KY, Jo S (2019) Effect of spine-pelvis relationship in total hip arthroplasty. Hip Pelvis 31(1):4–10
Schwab FJ, Blondel B, Bess S, Hostin R, Shaffrey CI, Smith JS, Boachie-Adjei O, Burton DC, Akbarnia BA, Mundis GM, Ames CP, Kebaish K, Hart RA, Farcy JP, Lafage V, International Spine Study G (2013) Radiographical spinopelvic parameters and disability in the setting of adult spinal deformity: a prospective multicenter analysis. Spine 38(13):E803–E812
Stefl M, Lundergan W, Heckmann N, McKnight B, Ike H, Murgai R, Dorr LD (2017) Spinopelvic mobility and acetabular component position for total hip arthroplasty. Bone Joint J 99-B(1 Supple A):37–45
Phan D, Bederman SS, Schwarzkopf R (2015) The influence of sagittal spinal deformity on anteversion of the acetabular component in total hip arthroplasty. Bone Joint J 97-B(8):1017–1023
Kanawade V, Dorr LD, Wan Z (2014) Predictability of acetabular component angular change with postural shift from standing to sitting position. J Bone Joint Surg Am 96(12):978–986
Koo TK, Li MY (2016) A guideline of selecting and reporting Intraclass correlation coefficients for reliability research. J Chiropr Med 15(2):155–163
Barrey C, Jund J, Noseda O, Roussouly P (2007) Sagittal balance of the pelvis-spine complex and lumbar degenerative diseases. A comparative study about 85 cases. Eur Spine J 16(9):1459–1467
Kobayashi H, Endo K, Sawaji Y, Matsuoka Y, Nishimura H, Murata K, Takamatsu T, Suzuki H, Aihara T, Yamamoto K (2019) Global sagittal spinal alignment in patients with degenerative low-grade lumbar spondylolisthesis. J Orthop Surg 27(3):2309499019885190
Esposito CI, Carroll KM, Sculco PK, Padgett DE, Jerabek SA, Mayman DJ (2018) Total hip arthroplasty patients with fixed Spinopelvic alignment are at higher risk of hip dislocation. J Arthroplasty 33(5):1449–1454
Lazennec JY, Brusson A, Folinais D, Zhang A, Pour AE, Rousseau MA (2015) Measuring extension of the lumbar-pelvic-femoral complex with the EOS(R) system. Eur J Orthop Surg Traumatol 25(6):1061–1068
Eddine TA, Migaud H, Chantelot C, Cotten A, Fontaine C, Duquennoy A (2001) Variations of pelvic anteversion in the lying and standing positions: analysis of 24 control subjects and implications for CT measurement of position of a prosthetic cup. Surg Radiol Anat 23(2):105–110
Sierra RJ, Raposo JM, Trousdale RT, Cabanela ME (2005) Dislocation of primary THA done through a posterolateral approach in the elderly. Clin Orthop Relat Res 441:262–267
Author information
Authors and Affiliations
Contributions
All co-authors actively participated in this study and have read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
K. Shen, L. Lin, E. Feng, Y. Zhang, L. Xiao, F. Lin and Z. Li declare that they have no competing interests.
Ethical standards
All procedures performed in studies involving human participants or on human tissue were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards. This study was approved by the Ethics Committee of Fuzhou Second Hospital affiliated to Xiamen University. Written informed consent was obtained from all patients enrolled in the investigation.
Additional information
Kaiwei Shen and Liqiong Lin are first co-authors, they contributed equally to the work.
Study design
Retrospective comparative case series (nonrandomized clinical study design).
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request; please contact the corresponding author Dr. Feng. Administrative permission was received from Fuzhou Second Hospital affiliated to Xiamen University (No. 47, Shangteng Road, Cangshan District, Fuzhou, China) to access the medical records.
Rights and permissions
About this article
Cite this article
Shen, K., Lin, L., Feng, E. et al. Influence of sagittal degenerative spondylolisthesis on anteversion of the acetabular component in total hip arthroplasty. Orthopäde 50, 664–673 (2021). https://doi.org/10.1007/s00132-021-04069-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00132-021-04069-w