Abstract
Purpose
There is widespread recognition of the importance and complexity of measuring neighborhood contexts within research on child psychopathology. In this study, we assessed the cross-sectional associations between two measures of neighborhood quality and internalizing and externalizing behaviors in preadolescence.
Methods
Drawing on baseline data from the Adolescent Brain Cognitive Development Study (n = 10,577 preadolescents), we examined two multi-component assessments of neighborhood quality in relation to children’s internalizing and externalizing symptoms: the Area Deprivation Index (ADI), which measures socioeconomic adversity, and the Child Opportunity Index 2.0 (COI), which measures economic, educational, and environmental opportunity. Both measures were categorized into quintiles. We then used mixed-effects linear regression models to examine bivariate and adjusted associations.
Results
The bivariate associations displayed strong inverse associations between the COI and ADI and externalizing symptoms, with a graded pattern of fewer externalizing behaviors with increasing neighborhood quality. Only the ADI was associated with externalizing behaviors in models adjusted for child and family characteristics. We did not observe a clear association between either measure of neighborhood quality and internalizing behaviors in bivariate or adjusted models.
Conclusions
Neighborhood quality, as measured by the COI and ADI, was associated with externalizing behaviors in preadolescent children. The association using the ADI persisted after adjustment for family-level characteristics, including financial strain. Our results indicate that different assessments of neighborhood quality display distinct associations with preadolescent behavioral health. Future research is needed to assess the association between neighborhood quality and behavior trajectories and to identify place-based intervention strategies.


Similar content being viewed by others
Data availability
The Adolescent Brain Cognitive Development (ABCD) Study is an open-access database and can be accessed at https://abcdstudy.org, held in the NIMH Data Archive. Data can be accessed following a data request to the NIH data access committee (https://nda.nih.gov/), which should include information on the planned topic of study. The following data sets were generated under NIMH Data Archive: Comparing two measures of neighborhood quality and internalizing and externalizing behaviors in the Adolescent Brain Cognitive Development Study #2214 (https1015154/xd5b-7z89).
References
Dunn EC, Masyn KE, Yudron M, Jones SM, Subramanian SV (2014) Translating multilevel theory into multilevel research: challenges and opportunities for understanding the social determinants of psychiatric disorders. Soc Psychiatry Psychiatr Epidemiol 49(6):859–872. https://doi.org/10.1007/s00127-013-0809-5
Nicotera N (2007) Measuring Neighborhood: A Conundrum for Human Services Researchers and Practitioners. Am J Community Psychol 40(1):26–51. https://doi.org/10.1007/s10464-007-9124-1
Duncan DT, Kawachi I (2018) Neighborhoods and Health. Oxford University Press
Rajaratnam JK, Burke JG, O’Campo P (2006) Maternal and child health and neighborhood context: The selection and construction of area-level variables. Health Place 12(4):547–556. https://doi.org/10.1016/j.healthplace.2005.08.008
Maxwell MY, Taylor RL, Barch DM (2022) Relationship Between Neighborhood Poverty and Externalizing Symptoms in Children: Mediation and Moderation by Environmental Factors and Brain Structure. Child Psychiatry Hum Dev. https://doi.org/10.1007/s10578-022-01369-w
Ip KI, Sisk LM, Horien C, Conley MI, Rapuano KM, Rosenberg MD, Gee DG (2022) Associations among Household and Neighborhood Socioeconomic Disadvantages, Resting-state Frontoamygdala Connectivity, and Internalizing Symptoms in Youth. J Cogn Neurosci 34(10):1810–1841. https://doi.org/10.1162/jocn_a_01826
Alavi N, Roberts N, DeGrace E (2017) Comparison of parental socio-demographic factors in children and adolescents presenting with internalizing and externalizing disorders. Int J Adolesc Med Health. https://doi.org/10.1515/ijamh-2015-0049
Bronfenbrenner U (1992) Ecological systems theory. Six theories of child development: Revised formulations and current issues. Jessica Kingsley Publishers, London, England, pp 187–249
Davison KK, Birch LL (2001) Childhood overweight: a contextual model and recommendations for future research. Obes Rev 2(3):159–171. https://doi.org/10.1046/j.1467-789x.2001.00036.x
Krieger N (2021) Ecosocial Theory, Embodied Truths, and the People’s Health. Oxford University Press
Krieger N (2011) Epidemiology and the People’s Health: Theory and Context. Oxford University Press
Krieger N, Alegría M, Almeida-Filho N, da Silva JB, Barreto ML, Beckfield J, Walters KL (2010) Who, and what, causes health inequities? Reflections on emerging debates from an exploratory Latin American/North American workshop. J Epidemiol Commun Health 64(9):747–749
Delany-Brumsey A, Mays VM, Cochran SD (2014) Does Neighborhood Social Capital Buffer the Effects of Maternal Depression on Adolescent Behavior Problems? Am J Community Psychol 53(3):275–285. https://doi.org/10.1007/s10464-014-9640-8
Lenzi M, Vieno A, Perkins DD, Pastore M, Santinello M, Mazzardis S (2012) Perceived Neighborhood Social Resources as Determinants of Prosocial Behavior in Early Adolescence. Am J Community Psychol 50(1):37–49. https://doi.org/10.1007/s10464-011-9470-x
McBride Murry V, Berkel C, Gaylord-Harden NK, Copeland-Linder N, Nation M (2011) Neighborhood Poverty and Adolescent Development. J Res Adolesc 21(1):114–128. https://doi.org/10.1111/j.1532-7795.2010.00718.x
Bishop AS, Walker SC, Herting JR, Hill KG (2020) Neighborhoods and health during the transition to adulthood: A scoping review. Health Place 63:102336. https://doi.org/10.1016/j.healthplace.2020.102336
Leventhal T, Dupéré V (2019) Neighborhood Effects on Children’s Development in Experimental and Nonexperimental Research. Annual Review of Developmental Psychology 1(1):149–176. https://doi.org/10.1146/annurev-devpsych-121318-085221
White RMB, Witherspoon DP, Wei W, Zhao C, Pasco MC, Maereg TM (2021) Adolescent Development in Context: A Decade Review of Neighborhood and Activity Space Research. J Res Adolesc 31(4):944–965. https://doi.org/10.1111/jora.12623
Plybon LE, Kliewer W (2001) Neighborhood Types and Externalizing Behavior in Urban School-Age Children: Tests of Direct, Mediated, and Moderated Effects. J Child Fam Stud 10(4):419–437. https://doi.org/10.1023/A:1016781611114
Lynch M (2003) Consequences of Children’s Exposure to Community Violence. Clin Child Fam Psychol Rev 6(4):265–274. https://doi.org/10.1023/B:CCFP.0000006293.77143.e1
Chang L-Y, Wang M-Y, Tsai P-S (2016) Neighborhood disadvantage and physical aggression in children and adolescents: A systematic review and meta-analysis of multilevel studies. Aggressive Behav 42(5):441–454. https://doi.org/10.1002/ab.21641
Iruka IU, Gardner-Neblett N, Telfer NA, Ibekwe-Okafor N, Curenton SM, Sims J, Neblett EW (2022) Effects of Racism on Child Development: Advancing Antiracist Developmental Science. Ann Rev Developmen Psychol 4(1):109–132. https://doi.org/10.1146/annurev-devpsych-121020-031339
Slopen N, Heard-Garris N (2022) Structural Racism and Pediatric Health—A Call for Research to Confront the Origins of Racial Disparities in Health. JAMA Pediatr 176(1):13–15. https://doi.org/10.1001/jamapediatrics.2021.3594
Arcaya MC, Tucker-Seeley RD, Kim R, Schnake-Mahl A, So M, Subramanian SV (2016) Research on neighborhood effects on health in the United States: A systematic review of study characteristics. Soc Sci Med 168:16–29. https://doi.org/10.1016/j.socscimed.2016.08.047
Minh A, Muhajarine N, Janus M, Brownell M, Guhn M (2017) A review of neighborhood effects and early child development: How, where, and for whom, do neighborhoods matter? Health Place 46:155–174. https://doi.org/10.1016/j.healthplace.2017.04.012
Barch DM, Albaugh MD, Baskin-Sommers A, Bryant BE, Clark DB, Dick AS, Xie L (2021) Demographic and mental health assessments in the adolescent brain and cognitive development study: Updates and age-related trajectories. Developm Cogn Neurosci. https://doi.org/10.1016/j.dcn.2021.101031
Kind AJH, Buckingham WR (2018) Making Neighborhood-Disadvantage Metrics Accessible — The Neighborhood Atlas. N Engl J Med 378(26):2456–2458. https://doi.org/10.1056/NEJMp1802313
Acevedo-Garcia D, Noelke C, McArdle N, Sofer N, Hardy EF, Weiner M, Reece J (2020) Racial And Ethnic Inequities In Children’s Neighborhoods: Evidence From The New Child Opportunity Index 20. Health Aff 39(10):1693–1701. https://doi.org/10.1377/hlthaff.2020.00735
Sykes AG (2021) Pediatric Trauma in the California-Mexico Border Region: Injury Disparities by Area Deprivation Index. University of California, San Diego. Retrieved from https://www.proquest.com/openview/787a8d21df4e126bf68e814e84d83dda/1?pq-origsite=gscholar&cbl=18750&diss=y
Oates G, Rutland S, Juarez L, Friedman A, Schechter MS (2021) The association of area deprivation and state child health with respiratory outcomes of pediatric patients with cystic fibrosis in the United States. Pediatr Pulmonol 56(5):883–890. https://doi.org/10.1002/ppul.25192
Schraw JM, Peckham-Gregory EC, Rabin KR, Scheurer ME, Lupo PJ, Oluyomi A (2020) Area deprivation is associated with poorer overall survival in children with acute lymphoblastic leukemia. Pediatr Blood Cancer. https://doi.org/10.1002/pbc.28525
Mullins TS, Campbell EM, Hogeveen J (2020) Neighborhood Deprivation Shapes Motivational-Neurocircuit Recruitment in Children. Psychol Sci 31(7):881–889. https://doi.org/10.1177/0956797620929299
Slopen N, Cosgrove C, Acevedo-Garcia D, Hatzenbuehler ML, Shonkoff JP, Noelke C (2023) Neighborhood Opportunity and Mortality Among Children and Adults in Their Households. Pediatrics. https://doi.org/10.1542/peds.2022-058316
Fritz CQ, Fleegler EW, DeSouza H, Richardson T, Kaiser SV, Sills MR, Goyal M (2022) Child Opportunity Index and Changes in Pediatric Acute Care Utilization in the COVID-19 Pandemic. Pediatrics. https://doi.org/10.1542/peds.2021-053706
Krager MK, Puls HT, Bettenhausen JL, Hall M, Thurm C, Plencner LM, Beck AF (2021) The Child Opportunity Index 20 and Hospitalizations for Ambulatory Care Sensitive Conditions. Pediatrics. https://doi.org/10.1542/peds.2020-032755
Thorpe D, Mirhashem R, Shen J, Roulston C, Fox K, Schleider J (2023) Ecological-Systems Contributors to Internalizing Symptoms in a US Sample of Adolescents During the COVID-19 Pandemic. J Clin Child Adoles Psychol https://doi.org/10.1080/15374416.2023.2246556
Volkow ND, Koob GF, Croyle RT, Bianchi DW, Gordon JA, Koroshetz WJ, Weiss SRB (2018) The conception of the ABCD study: From substance use to a broad NIH collaboration. Developm Cogn Neurosci 32:4–7. https://doi.org/10.1016/j.dcn.2017.10.002
Booth JM, Shaw DS (2020) Relations among Perceptions of Neighborhood Cohesion and Control and Parental Monitoring across Adolescence. J Youth Adolesc 49(1):74–86. https://doi.org/10.1007/s10964-019-01045-8
Garavan H, Bartsch H, Conway K, Decastro A, Goldstein RZ, Heeringa S, Zahs D (2018) Recruiting the ABCD sample: Design considerations and procedures. Developm Cogn Neurosci 32:16–22. https://doi.org/10.1016/j.dcn.2018.04.004
Compton WM, Dowling GJ, Garavan H (2019) Ensuring the Best Use of Data: The Adolescent Brain Cognitive Development Study. JAMA Pediatr 173(9):809–810. https://doi.org/10.1001/jamapediatrics.2019.2081
Fan CC, Marshall A, Smolker H, Gonzalez MR, Tapert SF, Barch DM, Herting MM (2021) Adolescent Brain Cognitive Development (ABCD) study Linked External Data (LED): Protocol and practices for geocoding and assignment of environmental data. Develop Cogn Neurosci. https://doi.org/10.1016/j.dcn.2021.101030
Johnson AE, Zhu J, Garrard W, Thoma FW, Mulukutla S, Kershaw KN, Magnani JW (2021) Area Deprivation Index and Cardiac Readmissions: Evaluating Risk-Prediction in an Electronic Health Record. J Am Heart Assoc. https://doi.org/10.1161/JAHA.120.020466
Fairfield KM, Black AW, Ziller EC, Murray K, Lucas FL, Waterston LB, Han PKJ (2020) Area Deprivation Index and Rurality in Relation to Lung Cancer Prevalence and Mortality in a Rural State. JNCI Cancer Spectrum. https://doi.org/10.1093/jncics/pkaa011
Achenbach TM, Ruffle TM (2000) The Child Behavior Checklist and Related Forms for Assessing Behavioral/Emotional Problems and Competencies. Pediatr Rev 21(8):265–271. https://doi.org/10.1542/pir.21-8-265
Achenbach TM, Rescorla L (2001) Manual for the ASEBA school-age forms & profiles: an integrated system of multi-informant assessment
Clark DA, Hicks BM, Angstadt M, Rutherford S, Taxali A, Hyde L, Sripada C (2021) The General Factor of Psychopathology in the Adolescent Brain Cognitive Development (ABCD) Study: A Comparison of Alternative Modeling Approaches. Clin Psychol Sci J Assoc Psychol Sci 9(2):169–182. https://doi.org/10.1177/2167702620959317
Hendrickson, N. K., & McCrimmon, A. W. (2019). Test Review: Behavior Rating Inventory of Executive Function®, Second Edition (BRIEF®2) by Gioia, G. A., Isquith, P. K., Guy, S. C., & Kenworthy, L. Canadian Journal of School Psychology, 34(1), 73–78. https://doi.org/10.1177/0829573518797762
Assari S (2020) Neighborhood Poverty and Amygdala Response to Negative Face. J Econ Pub Finan 6(4):67–85
Gonzalez MR, Palmer CE, Uban KA, Jernigan TL, Thompson WK, Sowell ER (2020) Positive Economic, Psychosocial, and Physiological Ecologies Predict Brain Structure and Cognitive Performance in 9–10-Year-Old Children. Front Hum Neurosci. https://doi.org/10.3389/fnhum.2020.578822
Berg-Nielsen TS, Solheim E, Belsky J, Wichstrom L (2012) Preschoolers’ Psychosocial Problems: In the Eyes of the Beholder? Adding Teacher Characteristics as Determinants of Discrepant Parent-Teacher Reports. Child Psychiatry Hum Dev 43(3):393–413. https://doi.org/10.1007/s10578-011-0271-0
Stevens GWJM, Pels T, Bengi-Arslan L, Verhulst FC, Vollebergh WAM, Crijnen AAM (2003) Parent, teacher and self-reportedproblem behavior in The Netherlands. Soc Psychiatry Psychiatr Epidemiol 38(10):576–585. https://doi.org/10.1007/s00127-003-0677-5
Najman JM, Williams GM, Nikles J, Spence S, Bor W, O’Callaghan M, Shuttlewood GJ (2001) Bias influencing maternal reports of child behaviour and emotional state. Soc Psych Psychiat Epidemiol 36(4):186–194. https://doi.org/10.1007/s001270170062
Vable AM, Diehl SF, Glymour MM (2021) Code Review as a Simple Trick to Enhance Reproducibility, Accelerate Learning, and Improve the Quality of Your Team’s Research. Am J Epidemiol 190(10):2172–2177. https://doi.org/10.1093/aje/kwab092
Schober P, Boer C, Schwarte LA (2018) Correlation Coefficients: Appropriate Use and Interpretation. Anesth Analg 126(5):1763–1768. https://doi.org/10.1213/ANE.0000000000002864
Diler RS, Birmaher B, Axelson D, Goldstein B, Gill M, Strober M, Keller MB (2009) The Child Behavior Checklist (CBCL) and the CBCL-Bipolar Phenotype Are Not Useful in Diagnosing Pediatric Bipolar Disorder. J Child Adolesc Psychopharmacol 19(1):23–30. https://doi.org/10.1089/cap.2008.067
Aris IM, Perng W, Dabelea D, Padula AM, Alshawabkeh A, Vélez-Vega CM, Program Collaborators for Environmental Influences on Child Health Outcomes (2022) Associations of Neighborhood Opportunity and Social Vulnerability With Trajectories of Childhood Body Mass Index and Obesity Among US Children. JAMA Netw Open. https://doi.org/10.1001/jamanetworkopen.2022.47957
Lou S, Giorgi S, Liu T, Eichstaedt JC, Curtis B (2023) Measuring disadvantage: A systematic comparison of United States small-area disadvantage indices. Health Place 80:102997. https://doi.org/10.1016/j.healthplace.2023.102997
US Census Bureau. (2022). Census Bureau Releases New Educational Attainment Data. Census.gov. Retrieved September 12, 2023, from https://www.census.gov/newsroom/press-releases/2022/educational-attainment.html
Clapp JM, Wang Y (2006) Defining neighborhood boundaries: Are census tracts obsolete? J Urban Econ 59(2):259–284. https://doi.org/10.1016/j.jue.2005.10.003
Diez Roux A-V (2007) Neighborhoods and health: where are we and were do we go from here? Rev d’Épidémiol San Publ 55(1):13–21. https://doi.org/10.1016/j.respe.2006.12.003
Roy AL, McCoy DC, Raver CC (2014) Instability versus quality: Residential mobility, neighborhood poverty, and children’s self-regulation. Dev Psychol 50(7):1891–1896. https://doi.org/10.1037/a0036984
Chen MA, LeRoy AS, Majd M, Chen JY, Brown RL, Christian LM, Fagundes CP (2021) Immune and Epigenetic Pathways Linking Childhood Adversity and Health Across the Lifespan. Front Psychol. https://doi.org/10.3389/fpsyg.2021.788351
Kepper M, Sothern M, Zabaleta J, Ravussin E, Velasco-Gonzalez C, Leonardi C, Scribner R (2016) Prepubertal children exposed to concentrated disadvantage: An exploratory analysis of inflammation and metabolic dysfunction. Obesity 24(5):1148–1153. https://doi.org/10.1002/oby.21462
Skinner AT, Bacchini D, Lansford JE, Godwin JW, Sorbring E, Tapanya S, Pastorelli C (2014) Neighborhood Danger, Parental Monitoring, Harsh Parenting, and Child Aggression in Nine Countries. Societies 4(1):45–67. https://doi.org/10.3390/soc4010045
Zuberi A (2016) Neighborhoods and Parenting: Assessing the Influence of Neighborhood Quality on the Parental Monitoring of Youth. Youth & Society 48(5):599–627. https://doi.org/10.1177/0044118X13502365
Acknowledgements
Data used in the preparation of this article were obtained from the ABCD Study (https://abcdstudy.org) held in the NDA. This is a multisite, longitudinal study designed to recruit more than 10,000 children ages 9–10 years and follow them over 10 years into early adulthood. The ABCD study is supported by the National Institutes of Health and additional federal partners under award numbers U01DA041048, U01DA050989, U01DA051016, U01DA041022, U01DA051018, U01DA051037, U01DA050987, U01DA041174, U01DA041106, U01DA041117, U01DA041028, U01DA041134, U01DA050988, U01DA051039, U01DA041156, U01DA041025, U01DA041120, U01DA051038, U01DA041148, U01DA041093, U01DA041089, U24DA041123 and U24DA041147. A full list of supporters is available at https://abcdstudy.org/federal-partners.html. A listing of participating sites and a complete listing of the study investigators can be found at https://abcdstudy.org/consortium_members/. ABCD consortium investigators designed and implemented the study and/or provided data, but did not necessarily participate in the analysis or writing of this report. Most ABCD research sites rely on a central Institutional Review Board (IRB) at the University of California, San Diego, for the ethical review and approval of the research protocol, with a few sites obtaining local IRB approval. The views expressed in this manuscript are those of the authors and do not necessarily reflect the official views of the National Institutes of Health, the Department of Health and Human Services, the US federal government or ABCD consortium investigators. The ABCD data repository grows and changes over time. The ABCD data used in this report came from DOI 1015154/1523041. DOIs can be found at https://nda.nih.gov/abcd/abcd-annual-releases.html. Additional support for this work was made possible from NIEHS R01-ES032295 and R01-ES031074.
Funding
The project described was supported by award numbers T32GM007753 and T32GM144273 from the National Institute of General Medical Sciences, award R01AG066793 from the National Investigation Agency, award R01ES034373 from the National Institute of Environmental Health Sciences, award T32MH017119 from the National Institute of Mental Health, and award P3036220 from the W. K. Kellogg Foundation. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institute of General Medical Sciences, the National Institute of Environmental Health Sciences, the National Institute of Mental Health, the National Institutes of Health, the National Investigation Agency, or the W. K. Kellogg Foundation. Support for this research was also provided by the CZI/Silicon Valley Community Foundation to the Center on the Developing Child at Harvard University.
Author information
Authors and Affiliations
Contributions
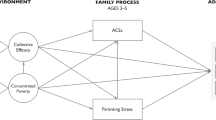
LB and NS conceived and designed the analysis. KAE, KP, SD, RK, and SSO provided feedback on the analysis plan, and both SD and SSO contributed R code to support the analysis. Analyses were conducted by LB and were independently reviewed by RK. LB wrote the paper with significant input from NS. LB created all tables and figures, except Figure 2, which was created by NS. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no relevant financial or non-financial interests to disclose.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Beyer, L., Keen, R., Ertel, K.A. et al. Comparing two measures of neighborhood quality and internalizing and externalizing behaviors in the adolescent brain cognitive development study. Soc Psychiatry Psychiatr Epidemiol (2024). https://doi.org/10.1007/s00127-024-02614-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00127-024-02614-4