Abstract
Purpose
This systematic review aimed to investigate the therapeutic relationship (TR) between mental health professionals (MHPs) and their patients in community mental health services (CMHS).
Methods
PubMed (Medline), PsycINFO, CINAHL, CENTRAL, and Web of Science were searched for studies that assessed TR in CMHS using quantitative measures developed specifically for this setting (i.e., Helping Alliance Scale [HAS] and the Scale to Assess the Therapeutic Relationship [STAR]). Studies were included if they considered adult patients with a psychiatric disorder and/or any MHP working in CMHS. Meta-analysis and narrative synthesis assessed the association between patients’ and MHPs’ ratings and identified predictors of TR.
Results
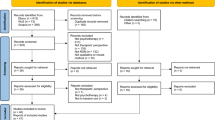
Of 1934 studies, 15 were included in the review, including 3004 patients. A total of 1127 patients and 963 MHPs were considered in the meta-analysis. The heterogeneity of the studies was high, and there was no significant difference between the patients’ and MHPs’ TR ratings in the random-effects model (standardized mean difference [SMD]: − 0.39 [95% CI: − 1.03; 0.24]). In the multivariable meta-regression, only duration of illness was significantly associated with TR ratings (unstandardized regression coefficient [B]: 0.388 [95% CI: 0.217; 0.558]). A recovery-oriented service, shared decision-making, and the recognition of patient needs contributed to more positive TR ratings.
Conclusion
Patients and MHPs converged in their TR ratings, although patients gave lower ratings. Routine assessment of TR in CMHS can inform reflective practice and service development, as TR can be assessed easily and early in the treatment process. Future research should focus on developing and testing interventions to improve TR in CMHS.


Similar content being viewed by others
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
References
Catty J (2004) “The vehicle of success”: theoretical and empirical perspectives on the therapeutic alliance in psychotherapy and psychiatry. Psychol Psychother 77:255–272. https://doi.org/10.1348/147608304323112528
Johansson H, Eklund M (2003) Patients’ opinion on what constitutes good psychiatric care. Scand J Caring Sci 17:339–346. https://doi.org/10.1046/j.0283-9318.2003.00233.x
Priebe S, Mccabe R (2008) Therapeutic relationships in psychiatry: the basis of therapy or therapy in itself? Int Rev Psychiatry 20:521–526. https://doi.org/10.1080/09540260802565257
Catty J, Winfield H, Clement S (2007) The therapeutic relationship in secondary mental health care: a conceptual review of measures. Acta Psychiatr Scand 116:238–252. https://doi.org/10.1111/j.1600-0447.2007.01070.x
Horvath AO, Symonds BD (1991) Relation between working alliance and outcome in psychotherapy: a meta-analysis. J Couns Psychol 38:139–149. https://doi.org/10.1037/0022-0167.38.2.139
Wampold BE (2015) How important are the common factors in psychotherapy? An update. World Psychiatry 14:270–277. https://doi.org/10.1002/wps.20238
McGuire-Snieckus R, McCabe R, Catty J et al (2007) A new scale to assess the therapeutic relationship in community mental health care: STAR. Psychol Med 37:85–95. https://doi.org/10.1017/S0033291706009299
McCabe R, Priebe S (2004) The therapeutic relationship in the treatment of severe mental illness: a review of methods and findings. Int J Soc Psychiatry 50:115–128. https://doi.org/10.1177/0020764004040959
Priebe S, McCabe R (2006) The therapeutic relationship in psychiatric settings. Acta Psychiatr Scand 113:69–72. https://doi.org/10.1111/j.1600-0447.2005.00721.x
Priebe S, Watts J, Chase M, Matanov A (2005) Processes of disengagement and engagement in assertive outreach patients: qualitative study. Br J Psychiatry 187:438–443. https://doi.org/10.1192/bjp.187.5.438
Priebe S, Gruyters T (1993) The role of the helping alliance in psychiatric community care: a prospective study. J Nerv Ment Dis 181:552
Weiss M, Gaston L, Propst A, Zicherman V (1997) The role of the alliance in the pharmacologic treatment of depression. J Clin Psychiatry 58:18656
Luborsky L, McLellan AT, Woody GE et al (1985) Therapist success and its determinants. Arch Gen Psychiatry 42:602–611. https://doi.org/10.1001/archpsyc.1985.01790290084010
Tattan T, Tarrier N (2000) The expressed emotion of case managers of the seriously mentally ill: the influence of expressed emotion on clinical outcomes. Psychol Med 30:195–204. https://doi.org/10.1017/S0033291799001579
Horvath AO, Bedi RP (2002) The alliance. Psychotherapy relationships that work: therapist contributions and responsiveness to patients. Oxford University Press, New York, pp 37–69
Cummings AL, Hallberg ET, Slemon A, Martin J (1992) Participants’ memories for therapeutic events and ratings of session effectiveness. J Cogn Psychother 6:113–124
Kivlighan DM Jr, Arthur EG (2000) Convergence in client and counselor recall of important session events. J Couns Psychol 47:79–84. https://doi.org/10.1037/0022-0167.47.1.79
Reis BF, Brown LG (1999) Reducing psychotherapy dropouts: maximizing perspective convergence in the psychotherapy dyad. Psychother Theory Res Pract Train 36:123–136. https://doi.org/10.1037/h0087822
Tryon GS, Collins Blackwell S, Felleman Hammel E (2007) A meta-analytic examination of client–therapist perspectives of the working alliance. Psychother Res 17:629–642. https://doi.org/10.1080/10503300701320611
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 29:372,n71. https://doi.org/10.1136/bmj.n71
Catty J, White S, Koletsi M et al (2011) Therapeutic relationships in vocational rehabilitation: predicting good relationships for people with psychosis. Psychiatry Res 187:68–73. https://doi.org/10.1016/j.psychres.2010.10.018
Gaston L, Thompson L, Gallagher D et al (1998) Alliance, technique, and their interactions in predicting outcome of behavioral, cognitive, and brief dynamic therapy. Psychother Res 8:190–209. https://doi.org/10.1093/ptr/8.2.190
Horvath AO (2011) Alliance in common factor land: a view through the research lens. Res Psychother Psychopathol Process Outcome 14:121–135. https://doi.org/10.4081/ripppo.2011.45
Armijo-Olivo S, Stiles CR, Hagen NA et al (2012) Assessment of study quality for systematic reviews: a comparison of the Cochrane Collaboration Risk of Bias Tool and the Effective Public Health Practice Project Quality Assessment Tool: methodological research. J Eval Clin Pract 18:12–18. https://doi.org/10.1111/j.1365-2753.2010.01516.x
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7:177–188. https://doi.org/10.1016/0197-2456(86)90046-2
RStudio Team (2021) RStudio: Integrated Development Environment for R
Balduzzi S, Rücker G, Schwarzer G (2019) How to perform a meta-analysis with R: a practical tutorial. Evid Based Ment Health 22:153–160. https://doi.org/10.1136/ebmental-2019-300117
Schwarzer G (2021) meta: General package for meta-analysis
Ali MK, Hack SM, Brown CH et al (2018) Racial differences in mental health recovery among veterans with serious mental illness. J Racial Ethnic Health Disparities 5:235–242. https://doi.org/10.1007/s40615-017-0363-z
Arvidsson H, Olin E, Strand J, Tidefors I (2014) Effects of the Two-Way Communication Checklist (2-COM): a one-year cluster randomized study in a group of severely mentally ill persons. Int J Soc Psychiatry 60:95–102. https://doi.org/10.1177/0020764012467145
Catty J, White S, Clement S et al (2013) Continuity of care for people with psychotic illness: its relationship to clinical and social functioning. Int J Soc Psychiatry 59:5–17. https://doi.org/10.1177/0020764011421440
Catty J, Cowan N, Poole Z et al (2012) Attachment to the clinical team and its association with therapeutic relationships, social networks, and clinical well-being. Psychol Psychother 85:17–35. https://doi.org/10.1111/j.2044-8341.2010.02011.x
Fornells-Ambrojo M, Pocock P, Mintah R et al (2018) Co-morbid personality disorder in early intervention psychosis clients is associated with greater key worker emotional involvement. Early Interv Psychiatry 12:143–152. https://doi.org/10.1111/eip.12286
Jaeger S, Weißhaupt S, Flammer E, Steinert T (2014) Control beliefs, therapeutic relationship, and adherence in schizophrenia outpatients: a cross-sectional study. Am J Health Behav 38:914–923. https://doi.org/10.5993/AJHB.38.6.13
Junghan UM, Leese M, Priebe S, Slade M (2007) Staff and patient perspectives on unmet need and therapeutic alliance in community mental health services. Br J Psychiatry 191:543–547. https://doi.org/10.1192/bjp.bp.107.037978
Kvrgic S, Cavelti M, Beck E-M et al (2013) Therapeutic alliance in schizophrenia: the role of recovery orientation, self-stigma, and insight. Psychiatry Res 209:15–20. https://doi.org/10.1016/j.psychres.2012.10.009
McCabe R, John P, Dooley J et al (2016) Training to enhance psychiatrist communication with patients with psychosis (TEMPO): cluster randomised controlled trial. Br J Psychiatry 209:517–524. https://doi.org/10.1192/bjp.bp.115.179499
Park SG, Derman M, Dixon LB, et al (2014) Factors associated with shared decision–making preferences among veterans with serious mental illness. PS 65:1409–1413. https://doi.org/10.1176/appi.ps.201400131
Priebe S, Golden E, Kingdon D, et al (2017) Effective patient–clinician interaction to improve treatment outcomes for patients with psychosis: a mixed-methods design
Priebe S, Matanov A, Demi N et al (2012) Community mental health centres initiated by the south-eastern europe stability pact: evaluation in seven countries. Community Ment Health J 48:352–362. https://doi.org/10.1007/s10597-011-9417-6
Reininghaus U, McCabe R, Burns T et al (2011) Measuring patients’ views: a bifactor model of distinct patient-reported outcomes in psychosis. Psychol Med 41:277–289. https://doi.org/10.1017/S0033291710000784
Slade M, Jordan H, Clarke E et al (2014) The development and evaluation of a five-language multi-perspective standardised measure: clinical decision-making involvement and satisfaction (CDIS). BMC Health Serv Res 14:323. https://doi.org/10.1186/1472-6963-14-323
Gunderson J, Najavits L, Leonhard C et al (1997) Ontogeny of the therapeutic alliance in borderline patients. Psychother Res 7:301–309. https://doi.org/10.1080/10503309712331332033
Hersoug AG, Monsen JT, Havik OE, Høglend P (2002) Quality of early working alliance in psychotherapy: diagnoses, relationship and intrapsychic variables as predictors. PPS 71:18–27. https://doi.org/10.1159/000049340
Graves TA, Tabri N, Thompson-Brenner H et al (2017) A meta-analysis of the relation between therapeutic alliance and treatment outcome in eating disorders. Int J Eat Disord 50:323–340. https://doi.org/10.1002/eat.22672
Totura CMW, Fields SA, Karver MS (2018) The role of the therapeutic relationship in psychopharmacological treatment outcomes: a meta-analytic review. PS 69:41–47. https://doi.org/10.1176/appi.ps.201700114
Luborsky L, Crits-Christoph P, Alexander L, et al (1983) Two helping alliance methods for predicting outcomes of psychotherapy: a counting signs: vs.: a global rating method. J Nerv Mental Dis 171:480
Rioli G, Ferrari S, Henderson C et al (2020) Users’ choice and change of allocated primary mental health professional in community-based mental health services: A scoping review. Int J Soc Psychiatry 66:373–381. https://doi.org/10.1177/0020764020910182
Rioli G, Ferrari S, Henderson C, Galeazzi GM (2020) Experiences, opinions and current policies on users’ choice and change of the allocated primary mental health professional: a survey among directors of community mental health centers in the Emilia-Romagna region, Italy. Int J Ment Health Syst 14:41. https://doi.org/10.1186/s13033-020-00373-8
Rioli G, Ferrari S, Vandelli R, et al (2020) The choice and the change of the allocated primary mental health professional in community-based mental health services: a focus-group qualitative study. J Psychopathol. https://doi.org/10.36148/2284-0249-358
Joyce AS, Piper WE (1998) Expectancy, the therapeutic alliance, and treatment outcome in short-term individual psychotherapy. J Psychother Pract Res 7:236–248
Paivio SC (1998) Interpersonal problems, working alliance, and outcome in short-term experiential therapy. Psychother Res 8:392–407. https://doi.org/10.1093/ptr/8.4.392
Sterne JAC, Sutton AJ, Ioannidis JPA et al (2011) Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ 343:d4002. https://doi.org/10.1136/bmj.d4002
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
Conceptualization: Stefan Priebe; literature search: Chiara Visentini, Margherita Pinelli, Giulia Venturi; data analysis: Mattia Marchi; writing—original draft preparation: Mattia Marchi, Giulia Venturi; writing—review and editing: Gian Maria Galeazzi, Stefan Priebe, Mattia Marchi.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical standards
This systematic review is exempt from ethics approval because we are collecting and synthesizing data from previous studies in which ethical approval has already been obtained by the trial investigators at their respective local sites.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Marchi, M., Venturi, G., Visentini, C. et al. The therapeutic relationship in community mental health services: a systematic review of the literature. Soc Psychiatry Psychiatr Epidemiol 59, 731–743 (2024). https://doi.org/10.1007/s00127-023-02581-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-023-02581-2