Abstract
Background
Spinal pain and major depression are prevalent conditions in adult populations and are particularly impactful in the military. However, the temporal relationship between these two conditions remains poorly understood.
Methods
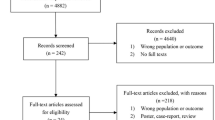
Using data extracted from electronic medical records, we assessed the association between incident diagnoses of spinal pain and major depression in a cohort of 48,007 Canadian Armed Forces personnel followed from January 2017 to August 2018. We used multivariate Poisson regression to measure the association between the period prevalence of these two conditions. We used probabilistic bias modelling to correct our estimates for misclassification of spinal pain and major depression.
Results
After correcting for misclassification with probabilistic bias modelling, subjects newly diagnosed with spinal pain during the study period were 1.41 times (95% interval 1.25, 1.59) more likely also to be diagnosed with incident major depression, and personnel newly diagnosed with major depression were 1.28 times (95% interval 1.17, 1.39) more likely also to be diagnosed with spinal pain, compared to undiagnosed counterparts of the same age and sex. Without bias corrections, we would have overestimated the magnitude of the association between major depression and spinal pain by a factor of approximately 2.0.
Conclusion
Our results highlight a moderate and bi-directional association between two of the most prevalent disorders in military populations. Our results also highlight the importance of correcting for misclassification in electronic medical record data research.

Similar content being viewed by others
References
Vos T, Abajobir AA, Abate KH et al (2017) Global, regional, and national incidence, prevalence, and years lived with disability for 328 diseases and injuries for 195 countries, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet 390:1211–1259. https://doi.org/10.1016/S0140-6736(17)32154-2
Gadermann AM, Engel CC, Naifeh JA et al (2012) Prevalence of DSM-IV major depression among U.S. military personnel: meta-analysis and simulation. Mil Med 177:47–59
Goodwin L, Wessely S, Hotopf M et al (2015) Are common mental disorders more prevalent in the U.K. serving military compared to the general working population? Psychol Med 45:1881–1891. https://doi.org/10.1017/S0033291714002980
Rusu C, Zamorski MA, Boulos D, Garber BG (2016) Prevalence comparison of past-year mental disorders and suicidal behaviours in the Canadian Armed Forces and the Canadian General Population. Can J Psychiatry 61:46S-55S. https://doi.org/10.1177/0706743716628856
Mcfarlane A, Sriapada R, Ganoczy D, et al (2011) Mental health in the Australian Defence Force 2010 ADF mental health and wellbeing study: Full report. Canberra. Accessed 6 Aug 2021
Ursano RJ, Kessler RC, Stein MB et al (2016) Risk factors, methods, and timing of suicide attempts among U.S. Army Soldiers JAMA Psychiatr 73:741–749. https://doi.org/10.1001/jamapsychiatry.2016.0600
Pflanz SE, Ogle AD (2006) Job stress, depression, work performance, and perceptions of supervisors in military personnel. Mil Med 171:861–865. https://doi.org/10.7205/MILMED.171.9.861
Littman AJ, Jacobson IG, Boyko EJ et al (2013) Weight change following U.S. military service. Int J Obes 37:244–253. https://doi.org/10.1038/ijo.2012.46
Clark LL, Hu Z (2015) Diagnoses of low back pain, active component, U.S. Armed Forces, 2010–2014. MSMR 22:8–11
Armed Forces Health Surveillance Center (AFHSC) (2012) Medical evacuations from operation iraqi freedom/operation new dawn, active and reserve components, U.S. Armed Forces, 2003–2011. MSMR 19:18–21
Vun E, Turner S, Sareen J et al (2018) Prevalence of comorbid chronic pain and mental health conditions in Canadian Armed Forces active personnel: analysis of a cross-sectional survey. C open 6:E528–E536. https://doi.org/10.9778/cmajo.20180093
Mattila VM, Kyröläinen H, Santtila M, Pihlajamäki H (2017) Low back pain during military service predicts low back pain later in life. PLoS ONE. https://doi.org/10.1371/journal.pone.0173568
Bair MJ, Robinson RL, Katon W, Kroenke K (2003) Depression and pain comorbidity. Arch Intern Med 163:2433. https://doi.org/10.1001/archinte.163.20.2433
Goesling J, Clauw DJ, Hassett AL (2013) Pain and depression: an integrative review of neurobiological and psychological factors. Curr Psychiatr Rep 15:421. https://doi.org/10.1007/s11920-013-0421-0
Terry EL, DelVentura JL, Bartley EJ et al (2013) Emotional modulation of pain and spinal nociception in persons with major depressive disorder (MDD). Pain 154:2759–2768. https://doi.org/10.1016/j.pain.2013.08.009
Fernandez M, Colodro-Conde L, Hartvigsen J et al (2017) Chronic low back pain and the risk of depression or anxiety symptoms: insights from a longitudinal twin study. Spine J 17:905–912. https://doi.org/10.1016/j.spinee.2017.02.009
Pinheiro MB, Ferreira ML, Refshauge K et al (2017) Symptoms of depression and risk of low back pain. Clin J Pain 33:777–785. https://doi.org/10.1097/AJP.0000000000000466
Lépine J-P, Briley M (2004) The epidemiology of pain in depression. Hum Psychopharmacol Clin Exp 19:S3–S7. https://doi.org/10.1002/hup.618
Thériault FL, Hawes RA, Garber BG et al (2019) Incidence of major depression diagnoses in the Canadian Armed Forces: longitudinal analysis of clinical and health administrative data. Soc Psychiatry Psychiatr Epidemiol. https://doi.org/10.1007/s00127-019-01754-2
Thériault FL, Lu D, Hawes RA (2019) Development and validation of a case-finding algorithm for neck and back pain in the Canadian Armed Forces using health administrative data. J Mil Veteran Fam Heal 5:16–26. https://doi.org/10.3138/jmvfh.2018-0039
Manchikanti L, Singh V, Datta S et al (2009) Comprehensive review of epidemiology, scope, and impact of spinal pain. Pain Physician 12:E35-70
Sinnott PL, Siroka AM, Shane AC et al (2012) Identifying neck and back pain in administrative data. Spine. https://doi.org/10.1097/BRS.0b013e3182376508
Deeny SR, Steventon A (2015) Making sense of the shadows: priorities for creating a learning healthcare system based on routinely collected data. BMJ Qual Saf 24:505–515. https://doi.org/10.1136/bmjqs-2015-004278
Thériault FL, Garber BG, Momoli F et al (2019) Mental health service utilization in depressed Canadian Armed Forces personnel. Can J Psychiatry 64:59–67. https://doi.org/10.1177/0706743718787792
Thériault FL, Gabler K, Naicker K (2016) Health and lifestyle information survey of Canadian Armed Forces Personnel 2013/2014 regular forces report. Department of National Defence, Ottawa Canada
Levine DS, Sripada RK, Ganoczy D et al (2016) Poorer physical health is associated with greater mental health service utilization in a sample of depressed U.S. Army National Guard Soldiers Mil Med 181:803–810. https://doi.org/10.7205/MILMED-D-15-00287
Lash TL, Fox MP, Fink AK (2009) Applying quantitative bias analysis to epidemiological data. Springer
Greenland S (1996) Basic methods for sensitivity analysis of biases. Int J Epidemiol 25:1107–1116
StataCorp (2015) Stata Statistical Software: Release 14. Accessed 11 Dec 2020
Schmaling KB, Nounou ZA (2019) Incident chronic spinal pain and depressive disorders: data from the national comorbidity survey. J Pain 20:481–488. https://doi.org/10.1016/j.jpain.2018.11.002
Bondesson E, Larrosa Pardo F, Stigmar K et al (2018) Comorbidity between pain and mental illness—evidence of a bidirectional relationship. Eur J Pain 22:1304–1311. https://doi.org/10.1002/ejp.1218
Chang M-H, Hsu J-W, Huang K-L et al (2015) Bidirectional association between depression and fibromyalgia syndrome: a nationwide longitudinal study. J Pain 16:895–902. https://doi.org/10.1016/j.jpain.2015.06.004
Siu AL, Bibbins-Domingo K, Grossman DC et al (2016) Screening for depression in adults. JAMA 315:380. https://doi.org/10.1001/jama.2015.18392
Valenstein M, Vijan S, Zeber JE et al (2001) The cost-utility of screening for depression in primary care. Ann Intern Med 134:345. https://doi.org/10.7326/0003-4819-134-5-200103060-00007
Joffres M, Jaramillo A, Dickinson J et al (2013) Recommendations on screening for depression in adults. CMAJ 185:775–782. https://doi.org/10.1503/cmaj.130403
Edmond SN, Heapy AA, Kerns RD (2019) Engaging mental health professionals in addressing pain. JAMA Psychiatr. https://doi.org/10.1001/jamapsychiatry.2019.0254
Parikh SV, Quilty LC, Ravitz P et al (2016) Canadian network for mood and anxiety treatments (CANMAT) 2016 clinical guidelines for the management of adults with major depressive disorder: section 2. Psychol Treat Can J Psychiatr 61:524–539. https://doi.org/10.1177/0706743716659418
Richmond H, Hall AM, Copsey B et al (2015) The effectiveness of cognitive behavioural treatment for non-specific low back pain: a systematic review and meta-analysis. PLoS ONE. https://doi.org/10.1371/journal.pone.0134192
Kroenke K, Wu J, Bair MJ et al (2011) Reciprocal relationship between pain and depression: a 12 month longitudinal analysis in primary care. J Pain 12:964–973. https://doi.org/10.1016/j.jpain.2011.03.003
Kroenke K, Spitzer RL (2002) The PHQ-9: a new depression diagnostic and severity measure. Psychiatr Ann 32:509–515. https://doi.org/10.3928/0048-5713-20020901-06
Schmidt CO, Raspe H, Pfingsten M et al (2007) Back pain in the German adult population. Spine. https://doi.org/10.1097/BRS.0b013e318133fad8
Currie SR, Wang J (2004) Chronic back pain and major depression in the general Canadian population. Pain 107:54–60
Ohayon MM, Schatzberg AF (2010) Chronic pain and major depressive disorder in the general population. J Psychiatr Res 44:454–461. https://doi.org/10.1016/j.jpsychires.2009.10.013
Kendler KS, Gardner CO, Prescott CA (2006) Toward a comprehensive developmental model for major depression in men. Am J Psychiatr 163:115–124. https://doi.org/10.1176/appi.ajp.163.1.115
Crofford LJ (2015) Chronic pain: where the body meets the brain. Trans Am Clin Climatol Assoc 126:167–183
Fikretoglu D, Liu A, Pedlar D, Brunet A (2010) Patterns and predictors of treatment delay for mental disorders in a nationally representative, active Canadian military sample. Med Care 48:10–17. https://doi.org/10.1097/MLR.0b013e3181bd4bf9
van Walraven C (2018) A comparison of methods to correct for misclassification bias from administrative database diagnostic codes. Int J Epidemiol 47:605–616. https://doi.org/10.1093/ije/dyx253
Lash TL, Fox MP, MacLehose RF et al (2014) Good practices for quantitative bias analysis. Int J Epidemiol 43:1969–1985. https://doi.org/10.1093/ije/dyu149
Funding
This work was supported by funding from the Canada Research Chairs program to I.C. and funding from the Surgeon General Health Research Program to FLT. The Research Council of Norway partly supported this work through its Centres of Excellence funding scheme, project number 262700.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. RAH and FLT performed data collection. Data analysis was performed by FLT. The first draft of the manuscript was written by FLT, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
None declared.
Ethical approval
This study was approved by the CAF Deputy Surgeon General and the University of Ottawa Office of Research Ethics and Integrity.
Rights and permissions
About this article
Cite this article
Thériault, F.L., Momoli, F., Hawes, R.A. et al. Spinal pain and major depression in a military cohort: bias analysis of dependent misclassification in electronic medical records. Soc Psychiatry Psychiatr Epidemiol 57, 575–581 (2022). https://doi.org/10.1007/s00127-021-02160-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-021-02160-3