Abstract
Purposes
To better assess and reduce suicidal risk in first-episode psychosis (FEP), we aimed to investigate the evolution of suicidal thoughts and behaviors (STBs) and associated factors in FEP.
Method
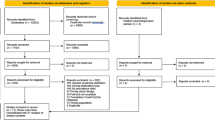
This systematic review (PROSPERO-CRD42020168050) meets PRISMA guidelines. PubMed, Medline, PsycINFO, Embase, EBM Reviews and references lists of relevant articles were searched (February 2020) to identify longitudinal studies, published in English or in French, that assessed the prevalence of STBs at entry to services and over follow-up, and examined factors associated with STBs among all persons with affective and non-affective FEP from a defined catchment area. Screening, data extraction and quality assessment using the adapted Newcastle Ottawa Scale were done independently by two reviewers. Results on prevalence and associated factors are presented by type of STB.
Results
Of 3,177 references, 17 studies of 11 non-overlapping samples (n = 14,907) with varying lengths of follow-up (1–41.7 years) were included. The prevalence of STBs decreased over follow-up. Up to 21.6% made at least one suicide attempt, 27% had suicidal ideation, and 1–4.3% died by suicide during follow-up. Of 53 factors assessed across studies, only male sex, depressive symptoms, and STBs occurring early during follow-up were associated with subsequent STBs. Early intervention for psychosis decreased STBs in the first three years. Other factors were assessed in a single study, yielded conflicting results, or were not associated with STBs.
Conclusions
The high prevalence of STBs following onset of psychosis highlights the need for early detection and intervention and ongoing assessment of suicidal risk throughout follow-up, with attention to identified risk factors. The heterogeneity of the studies precluded a meta-analysis and several factors were each assessed by a single study. Additional well-designed longitudinal studies of STBs and associated factors are warranted.

Similar content being viewed by others
Availability of data and material
All relevant data are within the manuscript and its Supporting Information files.
Code availability
Not applicable.
References
World Health Organization (2019) Suicide. https://www.who.int/news-room/fact-sheets/detail/suicide. 2019, September, 9
Franklin JC, Ribeiro JD, Fox KR, Bentley KH, Kleiman EM, Huang X, Musacchio KM, Jaroszewski AC, Chang BP, Nock MK (2017) Risk factors for suicidal thoughts and behaviors: a meta-analysis of 50 years of research. Psychol Bull 143(2):187–232. https://doi.org/10.1037/bul0000084
Huang X, Fox KR, Ribeiro JD, Franklin JC (2018) Psychosis as a risk factor for suicidal thoughts and behaviors: a meta-analysis of longitudinal studies. Psychol Med 48(5):765–776. https://doi.org/10.1017/S0033291717002136
Nordentoft M, Laursen TM, Agerbo E, Qin P, Hoyer EH, Mortensen PB (2004) Change in suicide rates for patients with schizophrenia in Denmark, 1981–97: nested case-control study. BMJ 329(7460):261. https://doi.org/10.1136/bmj.38133.622488.63
Yuen K, Harrigan SM, Mackinnon AJ, Harris MG, Yuen HP, Henry LP, Jackson HJ, Herrman H, McGorry PD (2014) Long-term follow-up of all-cause and unnatural death in young people with first-episode psychosis. Schizophr Res 159(1):70–75. https://doi.org/10.1016/j.schres.2014.07.042
Simon GE, Stewart C, Yarborough BJ, Lynch F, Coleman KJ, Beck A, Operskalski BH, Penfold RB, Hunkeler EM (2018) Mortality rates after the first diagnosis of psychotic disorder in adolescents and young adults. JAMA Psychiat 75(3):254–260. https://doi.org/10.1001/jamapsychiatry.2017.4437
Dutta R, Murray RM, Hotopf M, Allardyce J, Jones PB, Boydell J (2010) Reassessing the long term risk of suicide after a first episode of psychosis (FEP). Early Interv Psychiatry 4:22. https://doi.org/10.1111/j.1751-7893.2010.00215.x
Nordentoft M, Jeppesen P, Abel M, Kassow P, Petersen L, Thorup A, Krarup G, Hemmingsen R, Jorgensen P (2002) OPUS study: suicidal behaviour, suicidal ideation and hopelessness among patients with first-episode psychosis. One-year follow-up of a randomised controlled trial. Br J Psychiatry Suppl 43:s98-106. https://doi.org/10.1192/bjp.181.43.s98
Hjorthøj C, Stürup AE, McGrath JJ, Nordentoft M (2017) Years of potential life lost and life expectancy in schizophrenia: a systematic review and meta-analysis. The Lancet Psychiatry 4(4):295–301. https://doi.org/10.1016/S2215-0366(17)30078-0
World Health Organization (2014) Preventing suicide: a global imperative. Luxembourg
Chanut F, Brabant M (2016) Troubles liés à l’alcool. In: Lalonde P, Pinard P (eds) Psychiatrie clinique: approche bio-psycho-sociale, 4th edn. Chenelière éditeur, Montréal
Madsen T, Karstoft KI, Secher RG, Austin SF, Nordentoft M (2016) Trajectories of suicidal ideation in patients with first-episode psychosis: secondary analysis of data from the OPUS trial. Lancet Psychiatry 3(5):443–450. https://doi.org/10.1016/s2215-0366(15)00518-0
Nock MK, Millner AJ, Joiner TE, Gutierrez PM, Han G, Hwang I, King A, Naifeh JA, Sampson NA, Zaslavsky AM, Stein MB, Ursano RJ, Kessler RC (2018) Risk factors for the transition from suicide ideation to suicide attempt: results from the army study to assess risk and resilience in servicemembers (Army STARRS). J Abnorm Psychol 127(2):139–149. https://doi.org/10.1037/abn0000317
Nock MK, Green JG, Hwang I, McLaughlin KA, Sampson NA, Zaslavsky AM, Kessler RC (2013) Prevalence, correlates, and treatment of lifetime suicidal behavior among adolescents: results from the national comorbidity survey replication adolescent supplement. JAMA Psychiat 70(3):300–310
Klonsky ED, Saffer BY, Bryan CJ (2018) Ideation-to-action theories of suicide: a conceptual and empirical update. Curr Opin Psychol 22:38–43. https://doi.org/10.1016/j.copsyc.2017.07.020
Pompili M, Serafini G, Innamorati M, Lester D, Shrivastava A, Girardi P, Nordentoft M (2011) Suicide risk in first episode psychosis: a selective review of the current literature. Schizophr Res 129(1):1–11. https://doi.org/10.1016/j.schres.2011.03.008
Ventriglio A, Gentile A, Bonfitto I, Stella E, Mari M, Steardo L, Bellomo A (2016) Suicide in the early stage of schizophrenia. Front Psychiatry 7:116. https://doi.org/10.3389/fpsyt.2016.00116
Coentre R, Talina MC, Gois C, Figueira ML (2017) Depressive symptoms and suicidal behavior after first-episode psychosis: a comprehensive systematic review. Psychiatry Res 253:240–248. https://doi.org/10.1016/j.psychres.2017.04.010
Challis S, Nielssen O, Harris A, Large M (2013) Systematic meta-analysis of the risk factors for deliberate self-harm before and after treatment for first-episode psychosis. Acta Psychiatr Scand 127(6):442–454. https://doi.org/10.1111/acps.12074
McGinty J, Sayeed Haque M, Upthegrove R (2018) Depression during first episode psychosis and subsequent suicide risk: a systematic review and meta-analysis of longitudinal studies. Schizophr Res 195:58–66. https://doi.org/10.1016/j.schres.2017.09.040
Menezes NM, Milovan E (2000) First-episode psychosis: a comparative review of diagnostic evolution and predictive variables in adolescents versus adults. The Can J Psychiatry/La Revue Canad Psychiatrie 45(8):710–716
Heslin M, Lomas B, Lappin JM, Donoghue K, Reininghaus U, Onyejiaka A, Croudace T, Jones PB, Murray RM, Fearon P, Dazzan P, Morgan C, Doody GA (2015) Diagnostic change 10 years after a first episode of psychosis. Psychol Med 45(13):2757–2769. https://doi.org/10.1017/S0033291715000720
Correll CU, Galling B, Pawar A, Krivko A, Bonetto C, Ruggeri M, Craig TJ, Nordentoft M, Srihari VH, Guloksuz S, Hui CLM, Chen EYH, Valencia M, Juarez F, Robinson DG, Schooler NR, Brunette MF, Mueser KT, Rosenheck RA, Marcy P, Addington J, Estroff SE, Robinson J, Penn D, Severe JB, Kane JM (2018) Comparison of early intervention services vs treatment as usual for early-phase psychosis: a systematic review, meta-analysis, and meta-regression. JAMA Psychiat 75(6):555–565. https://doi.org/10.1001/jamapsychiatry.2018.0623
National Institute for Mental Health in England (NIMHE) (2008) Early intervention (EI) acceptance criteria guidance. NIMHE National Early Intervention Programme, England
Early Psychosis Guidelines Writing Group and EPPIC National Support Program (2016) Australian clinical guidelines for early psychosis, 2nd edn. Orygen, The National Centre of Excellence in Youth Mental Health, Melbourne
Ehmann T, Hanson L, Yager J, Dalzell K, Gilbert M (2010) Standards and guidelines for early psychosis intervention (EPI) programs. British Columbia Ministry of Health Services, British Columbia
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097–e1000097. https://doi.org/10.1371/journal.pmed.1000097
Beary M, Hodgson R, Wildgust HJ (2012) A critical review of major mortality risk factors for all-cause mortality in first-episode schizophrenia: clinical and research implications. J Psychopharmacol 26(5 Suppl):52–61. https://doi.org/10.1177/0269881112440512
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P (2013) The Newcastle–Ottawa Scale (NOS) for assessing the quality of nonrandomized studies in meta-analyses. The Ottawa Hospital Research Institute. Accessed January 31, 2020
MacDonald K, Fainman-Adelman N, Anderson KK, Iyer SN (2018) Pathways to mental health services for young people: a systematic review. Soc Psychiatry Psychiatr Epidemiol 53(10):1005–1038. https://doi.org/10.1007/s00127-018-1578-y
Anderson KK, Flora N, Archie S, Morgan C, McKenzie K (2014) A meta-analysis of ethnic differences in pathways to care at the first episode of psychosis. Acta Psychiatr Scand 130(4):257–268. https://doi.org/10.1111/acps.12254
Malla AM, Norman RM (2001) Treating psychosis: is there more to early intervention than intervening early? Can J Psychiatry 46(7):645–648. https://doi.org/10.1177/070674370104600710
Chang WC, Chen ES, Hui CL, Chan SK, Lee EH, Chen EY (2015) Prevalence and risk factors for suicidal behavior in young people presenting with first-episode psychosis in Hong Kong: a 3 year follow-up study. Soc Psychiatry Psychiatr Epidemiol 50(2):219–226. https://doi.org/10.1007/s00127-014-0946-5
Sanchez-Gistau V, Baeza I, Arango C, Gonzalez-Pinto A, de la Serna E, Parellada M, Graell M, Paya B, Llorente C, Castro-Fornieles J (2013) Predictors of suicide attempt in early-onset, first-episode psychoses: a longitudinal 24 month follow-up study. J Clin Psychiatry 74(1):59–66. https://doi.org/10.4088/JCP.12m07632
Melle I, Johannessen JO, Friis S, Haahr U, Joa I, Larsen TK, Opjordsmoen S, Rund BR, Simonsen E, Vaglum P, McGlashan T (2010) Course and predictors of suicidality over the first two years of treatment in first-episode schizophrenia spectrum psychosis. Arch Suicide Res 14(2):158–170. https://doi.org/10.1080/13811111003704787
Clarke M, Whitty P, Browne S, Mc Tigue O, Kinsella A, Waddington JL, Larkin C, O’Callaghan E (2006) Suicidality in first episode psychosis. Schizophr Res 86(1–3):221–225. https://doi.org/10.1016/j.schres.2006.05.026
Robinson J, Harris M, Cotton S, Hughes A, Conus P, Lambert M, Schimmelmann BG, McGorry P (2010) Sudden death among young people with first-episode psychosis: an 8–10 year follow-up study. Psychiatry Res 177(3):305–308. https://doi.org/10.1016/j.psychres.2010.03.013
Upthegrove R, Birchwood M, Ross K, Brunett K, McCollum R, Jones L (2010) The evolution of depression and suicidality in first episode psychosis. Acta Psychiatr Scand 122(3):211–218. https://doi.org/10.1111/j.1600-0447.2009.01506.x
Fedyszyn IE, Robinson J, Harris MG, Paxton SJ, Francey S (2012) Predictors of suicide-related behaviors during treatment following a first episode of psychosis: the contribution of baseline, past, and recent factors. Schizophr Res 140(1–3):17–24. https://doi.org/10.1016/j.schres.2012.06.022
Tseliou F, Johnson S, Major B, Rahaman N, Joyce J, Lawrence J, Mann F, Tapfumaneyi A, Chisholm B, Chamberlain-Kent N, Hinton MF, Fisher HL (2017) Gender differences in one-year outcomes of first-presentation psychosis patients in inner-city UK Early Intervention Services. Early Interv Psychiatry 11(3):215–223. https://doi.org/10.1111/eip.12235
Chen EY, Tang JY, Hui CL, Chiu CP, Lam MM, Law CW, Yew CW, Wong GH, Chung DW, Tso S, Chan KP, Yip KC, Hung SF, Honer WG (2011) Three-year outcome of phase-specific early intervention for first-episode psychosis: a cohort study in Hong Kong. Early Interv Psychiatry 5(4):315–323. https://doi.org/10.1111/j.1751-7893.2011.00279.x
Robinson J, Harris M, Harrigan S, Henry L, Farrelly S, Prosser A, Schwartz O, Jackson H, McGorry P (2010) Suicide attempt in first-episode psychosis: a 7.4 year follow-up study. Schizophr Res 116(1):1–8. https://doi.org/10.1016/j.schres.2009.10.009
Harris MG, Burgess PM, Chant DC, Pirkis JE, McGorry PD (2008) Impact of a specialized early psychosis treatment programme on suicide. Retrosp Cohort Study Early Interv Psychiatry 2(1):11–21. https://doi.org/10.1111/j.1751-7893.2007.00050.x
Sonmez N, Rossberg JI, Evensen J, Barder HE, Haahr U, ten Velden HW, Joa I, Johannessen JO, Langeveld H, Larsen TK, Melle I, Opjordsmoen S, Rund BR, Simonsen E, Vaglum P, McGlashan T, Friis S (2016) Depressive symptoms in first-episode psychosis: a 10 year follow-up study. Early Interv Psychiatry 10(3):227–233. https://doi.org/10.1111/eip.12163
Dutta R, Murray RM, Allardyce J, Jones PB, Boydell J (2011) Early risk factors for suicide in an epidemiological first episode psychosis cohort. Schizophr Res 126(1–3):11–19. https://doi.org/10.1016/j.schres.2010.11.021
Sanchez-Gistau V, Baeza I, Arango C, Gonzalez-Pinto A, de la Serna E, Parellada M, Graell M, Paya B, Llorente C, Castro-Fornieles J (2015) The affective dimension of early-onset psychosis and its relationship with suicide. J Child Psychol Psychiatry 56(7):747–755. https://doi.org/10.1111/jcpp.12332
Granello DH (2010) The process of suicide risk assessment: twelve core principles. J Couns Dev 88(3):363–371. https://doi.org/10.1002/j.1556-6678.2010.tb00034.x
Miranda-Mendizabal A, Castellví P, Parés-Badell O, Alayo I, Almenara J, Alonso I, Blasco MJ, Cebrià A, Gabilondo A, Gili M, Lagares C, Piqueras JA, Rodríguez-Jiménez T, Rodríguez-Marín J, Roca M, Soto-Sanz V, Vilagut G, Alonso J (2019) Gender differences in suicidal behavior in adolescents and young adults: systematic review and meta-analysis of longitudinal studies. Int J Public Health 64(2):265–283. https://doi.org/10.1007/s00038-018-1196-1
Zhang J (2014) The gender ratio of Chinese suicide rates: an explanation in Confucianism. Sex Roles: J Res 70(3–4):146–154. https://doi.org/10.1007/s11199-013-0333-9
Phillips MR, Yang G, Li S, Li Y (2004) Suicide and the unique prevalence pattern of schizophrenia in mainland China:a retrospective observational study. The Lancet 364(9439):1062–1068. https://doi.org/10.1016/S0140-6736(04)17061-X
Borges G, Nock MK, Haro Abad JM, Hwang I, Sampson NA, Alonso J, Andrade LH, Angermeyer MC, Beautrais A, Bromet E, Bruffaerts R, de Girolamo G, Florescu S, Gureje O, Hu C, Karam EG, Kovess-Masfety V, Lee S, Levinson D, Medina-Mora ME, Ormel J, Posada-Villa J, Sagar R, Tomov T, Uda H, Williams DR, Kessler RC (2010) Twelve-month prevalence of and risk factors for suicide attempts in the World Health Organization world mental health surveys. J Clin Psychiatry 71(12):1617–1628. https://doi.org/10.4088/JCP.08m04967blu
Nock MK, Borges G, Bromet EJ, Alonso J, Angermeyer M, Beautrais A, Bruffaerts R, Chiu WT, de Girolamo G, Gluzman S, de Graaf R, Gureje O, Haro JM, Huang Y, Karam E, Kessler RC, Lepine JP, Levinson D, Medina-Mora ME, Ono Y, Posada-Villa J, Williams D (2008) Cross-national prevalence and risk factors for suicidal ideation, plans and attempts. The Br J Psychiatry: J Mental Sci 192(2):98–105. https://doi.org/10.1192/bjp.bp.107.040113
Riecher-Rössler A, Butler S, Kulkarni J (2018) Sex and gender differences in schizophrenic psychoses—a critical review. Arch Womens Ment Health 21(6):627–648. https://doi.org/10.1007/s00737-018-0847-9
Li AWY, Hui CLM, Lee EHM, Chang WC, Chan SKW, Chen EYH (2019) Gender differences in correlates of cognition in first-episode psychosis. Psychiatry Res 271:412–420. https://doi.org/10.1016/j.psychres.2018.12.011
Comacchio C, Lasalvia A, Bonetto C, Cristofalo D, Miglietta E, Petterlini S, De Santi K, Tosato S, Riolo R, Cremonese C, Ceccato E, Zanatta G, Ruggeri M (2020) Gender and 5 years course of psychosis patients: focus on clinical and social variables. Arch Womens Ment Health 23(1):63–70. https://doi.org/10.1007/s00737-019-0945-3
Thorup A, Albert N, Bertelsen M, Petersen L, Jeppesen P, Le Quack P, Krarup G, Jørgensen P, Nordentoft M (2014) Gender differences in first-episode psychosis at 5 year follow-up—two different courses of disease? Results from the OPUS study at 5 year follow-up. Eur Psychiatry 29(1):44–51. https://doi.org/10.1016/j.eurpsy.2012.11.005
Eisenberg ME, Gower AL, McMorris BJ, Rider GN, Shea G, Coleman E (2017) Risk and protective factors in the lives of transgender/gender nonconforming adolescents. J Adolesc Health 61(4):521–526. https://doi.org/10.1016/j.jadohealth.2017.04.014
Chang WC, Chan GH, Jim OT, Lau ES, Hui CL, Chan SK, Lee EH, Chen EY (2015) Optimal duration of an early intervention programme for first-episode psychosis: randomised controlled trial. Br J Psychiatry 206(6):492–500. https://doi.org/10.1192/bjp.bp.114.150144
Albert N, Melau M, Jensen H, Emborg C, Jepsen JR, Fagerlund B, Gluud C, Mors O, Hjorthøj C, Nordentoft M (2017) Five years of specialised early intervention versus two years of specialised early intervention followed by three years of standard treatment for patients with a first episode psychosis: randomised, superiority, parallel group trial in Denmark (OPUS II). BMJ (Clinical research ed.), 356:i6681. https://doi.org/10.1136/bmj.i6681
Iyer SN, Mustafa SS, Moro L, Jarvis GE, Joober R, Abadi S, Casacalenda N, Margolese HC, Abdel-Baki A, Lepage M, Malla A (2020) Suicidality over the first 5 years of psychosis: does extending early intervention have benefits? Can J Psychiatry. https://doi.org/10.1177/0706743720961714
Ouellet-Plamondon C, Abdel-Baki A, Salvat É, Potvin S (2017) Specific impact of stimulant, alcohol and cannabis use disorders on first-episode psychosis: 2 year functional and symptomatic outcomes. Psychol Med 47(14):2461–2471. https://doi.org/10.1017/s0033291717000976
Abdel-Baki A, Ouellet-Plamondon C, Salvat É, Grar K, Potvin S (2017) Symptomatic and functional outcomes of substance use disorder persistence 2 years after admission to a first-episode psychosis program. Psychiatry Res 247:113–119. https://doi.org/10.1016/j.psychres.2016.11.007
Klonsky ED, May AM (2015) The three-step theory (3ST): a New theory of suicide rooted in the “Ideation-to-Action” framework. Int J Cogn Ther 8(2):114–129. https://doi.org/10.1521/ijct.2015.8.2.114
Abdel-Baki A, Lalonde P, Gingras N (2016) Schizophrénies. In: Lalonde P, Pinard P (eds) Psychiatrie clinique: approche bio-psycho-sociale, 4th edn. Chenelière éditeur, Montréal
Lappin JM, Heslin M, Jones PB, Doody GA, Reininghaus UA, Demjaha A, Croudace T, Jamieson-Craig T, Donoghue K, Lomas B, Fearon P, Murray RM, Dazzan P, Morgan C (2016) Outcomes following first-episode psychosis—why we should intervene early in all ages, not only in youth. Aust N Z J Psychiatry 50(11):1055–1063. https://doi.org/10.1177/0004867416673454
Dutta R, Murray RM, Allardyce J, Jones PB, Boydell JE (2012) Mortality in first-contact psychosis patients in the U.K.: a cohort study. Psychol Med 42(8):1649–1661. https://doi.org/10.1017/s0033291711002807
Robinson J, Cotton S, Conus P, Schimmelmann BG, McGorry P, Lambert M (2009) Prevalence and predictors of suicide attempt in an incidence cohort of 661 young people with first-episode psychosis. Aust N Z J Psychiatry 43(2):149–157. https://doi.org/10.1080/00048670802607162
O’Carroll PW, Berman AL, Maris RW, Moscicki EK, Tanney BL, Silverman MM (1996) Beyond the tower of babel: a nomenclature for suicidology. Suicide Life-Threat Behav 26(3):237–252. https://doi.org/10.1111/j.1943-278X.1996.tb00609.x
Silverman MM, Berman AL, Sanddal ND, O’Carroll PW, Joiner TE (2007) Rebuilding the tower of Babel: a revised nomenclature for the study of suicide and suicidal behaviors. Part 2: suicide-related ideations, communications, and behaviors. Suicide Life Threat Behav 37(3):264–277. https://doi.org/10.1521/suli.2007.37.3.264
Bornheimer LA, Zhang A, Li J, Hiller M, Tarrier N (2020) Effectiveness of suicide-focused psychosocial interventions in psychosis: a systematic review and meta-Analysis. Psychiatr Serv 71(8):829–838. https://doi.org/10.1176/appi.ps.201900487
Acknowledgements
We thank the three librarians who supported us for this systematic review: Cynthia Gagné and Monique Clar, Université de Montréal, and Caroline Sauvé, Centre hospitalier de l’Université de Montréal.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
RS: Conceptualization, data curation, formal analysis, investigation, methodology, validation, visualization, writing—original draft, writing—review and editing, SNI: Conceptualization, methodology, validation, visualization, writing—review and editing, BK: Data curation, formal analysis, investigation, methodology, AA-B: conceptualization, methodology, validation, visualization, writing—review and editing.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have declared any conflicts of interest.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Sicotte, R., Iyer, S.N., Kiepura, B. et al. A systematic review of longitudinal studies of suicidal thoughts and behaviors in first-episode psychosis: course and associated factors. Soc Psychiatry Psychiatr Epidemiol 56, 2117–2154 (2021). https://doi.org/10.1007/s00127-021-02153-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-021-02153-2