Abstract
Purpose
To describe the trends in the prevalence and incidence of children with psychiatric disorders, the types of medication prescribed, and the type of physician providing the prescriptions.
Method
This retrospective study linked six population-based administrative databases (2008–2015) in Alberta, Canada.
Results
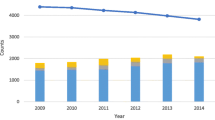
The prevalence of paediatric psychiatric disorders increased from 12.6 per 100 population in 2008 to 15.0 per 100 population in 2015, while the incidence rate increased from 2.0 per 100 population to 2.2 per 100 population in the same period. The proportion of patients dispensed any psychiatric medication increased from 21.4% in 2008 to 28.2% in 2015. Over the same period, dispensations for antidepressants increased from 7.0% to 11.2% and stimulants to treat ADHD, from 11.9% to 15.9%. For antidepressants, general practitioners (GPs) wrote the highest proportion of prescriptions (44.3% in 2011–48.1% in 2015), while paediatricians wrote the lowest proportion (8.7% in 2011–11.0% in 2015) and the proportion by psychiatrists decreased from 33.4% in 2011 to 27.2% in 2015. For stimulants to treat ADHD, paediatricians were the most frequent prescribers (36.9% in 2011–39.3% in 2015) followed by GPs as the second most frequent (33.1% in 2011–33.5% in 2015), while psychiatrists were the least likely to prescribe stimulants for ADHD.
Conclusion
The increasing trend of psychiatric diagnoses and medication prescriptions in the paediatric population is evident using population-based administrative databases. The lack of safety and adverse consequences of medication use in this cohort warrants additional monitoring data.



Similar content being viewed by others
References
Chafe R, Audas R (2014) The unseen high-cost users: children and youth with mental illness. HealthcarePapers 14(2):52–56
Merikangas KR, Nakamura EF, Kessler RC (2009) Epidemiology of mental disorders in children and adolescents. Dial Clin Neurosci 11(1):7–20
Polanczyk GV, Salum GA, Sugaya LS, Caye A, Rohde LA (2015) Annual research review: a meta-analysis of the worldwide prevalence of mental disorders in children and adolescents. J Child Psychol Psychiatry 56(3):345–365. https://doi.org/10.1111/jcpp.12381
Waddell C, Shepherd C, Schwartz C, Barican J (2014) Child and youth mental disorders: prevalence and evidence-based interventions: a research report for the British Columbia ministry of children and family development. Simon Fraser University, Children’s Health Policy Centre
Patten SB, Waheed W, Bresee L (2012) A review of pharmacoepidemiologic studies of antipsychotic use in children and adolescents. Can J Psychiatry 57(12):717–721. https://doi.org/10.1177/070674371205701202
Alessi-Severini S, Biscontri RG, Collins DM, Sareen J, Enns MW (2012) Ten years of antipsychotic prescribing to children: a Canadian population-based study. Can J Psychiatry 57(1):52–58. https://doi.org/10.1177/070674371205700109
Ronsley R, Scott D, Warburton WP, Hamdi RD, Louie DC, Davidson J, Panagiotopoulos C (2013) A population-based study of antipsychotic prescription trends in children and adolescents in British Columbia, from 1996 to 2011. Can J Psychiatry 58(6):361–369. https://doi.org/10.1177/070674371305800608
Hauck TS, Lau C, Wing LLF, Kurdyak P, Tu K (2017) ADHD treatment in primary care: demographic factors, medication trends, and treatment predictors. Can J Psychiatry 62(6):393–402. https://doi.org/10.1177/0706743716689055
Brault MC, Lacourse E (2012) Prevalence of prescribed attention-deficit hyperactivity disorder medications and diagnosis among Canadian preschoolers and school-age children: 1994-2007. Can J Psychiatry 57(2):93–101
Doey T, Handelman K, Seabrook JA, Steele M (2007) Survey of atypical antipsychotic prescribing by Canadian child psychiatrists and developmental pediatricians for patients aged under 18 years. Can J Psychiatry 52(6):363–368. https://doi.org/10.1177/070674370705200605
Government of Canada Canada’s health care system. https://www.canada.ca/en/health-canada/services/canada-health-care-system.html
Meng X, D’Arcy C, Tempier R (2014) Long-term trend in pediatric antidepressant use, 1983–2007: a population-based study. Can J Psychiatry 59(2):89–97. https://doi.org/10.1177/070674371405900204
Arora N, Knowles S, Gomes T, Mamdani MM, Juurlink DN, Carlisle C, Tadrous M (2016) Interprovincial variation in antipsychotic and antidepressant prescriptions dispensed in the Canadian pediatric population. Can J Psychiatry 61(12):758–765. https://doi.org/10.1177/0706743716649190
Katz LY, Kozyrskyj AL, Prior HJ, Enns MW, Cox BJ, Sareen J (2008) Effect of regulatory warnings on antidepressant prescription rates, use of health services and outcomes among children, adolescents and young adults. Can Med Assoc J 178(8):1005
Tournier M, Greenfield B, Galbaud du Fort G, Ducruet T, Zito JM, Cloutier A-M, Moride Y (2010) Patterns of antidepressant use in Quebec children and adolescents: trends and predictors. Psychiatry Res 179(1):57–63. https://doi.org/10.1016/j.psychres.2010.06.007
Lam D, Gorman DA, Patten S, Pringsheim T (2013) The pharmacoepidemiology of selective serotonin reuptake inhibitors for children and adolescents in Canada from 2005 to 2009: a database analysis. Pediatric Drugs 15(4):319–327. https://doi.org/10.1007/s40272-013-0014-8
Cipriani A, Zhou X, Del Giovane C, Hetrick SE, Qin B, Whittington C, Coghill D, Zhang Y, Hazell P, Leucht S, Cuijpers P, Pu J, Cohen D, Ravindran AV, Liu Y, Michael KD, Yang L, Liu L, Xie P (2016) Comparative efficacy and tolerability of antidepressants for major depressive disorder in children and adolescents: a network meta-analysis. Lancet (London, England) 388(10047):881–890. https://doi.org/10.1016/S0140-6736(16)30385-3
Currie J, Stabile M, Jones L (2014) Do stimulant medications improve educational and behavioral outcomes for children with ADHD? J Health Econ 37:58–69. https://doi.org/10.1016/j.jhealeco.2014.05.002
Star K, Norén GN, Nordin K, Edwards IR (2011) Suspected adverse drug reactions reported for children worldwide: an exploratory study using VigiBase. Drug Saf 34(5):415–428. https://doi.org/10.2165/11587540-000000000-00000
Correll CU, Carlson HE (2006) Endocrine and metabolic adverse effects of psychotropic medications in children and adolescents. J Am Acad Child Adolesc Psychiatry 45(7):771–791. https://doi.org/10.1097/01.chi.0000220851.94392.30
Correll CU, Carlson HE (2006) Endocrine and Metabolic Adverse Effects of Psychotropic Medications in Children and Adolescents. J Am Acad Child Adolesc Psychiatry 45(7):771–791. https://doi.org/10.1097/01.chi.0000220851.94392.30
Davidson S (2011) Davidson where we are and where we need to be the state of child and youth mental health in Canada: past problems and future fantasies. Healthcare Q 14(2):8–13. https://doi.org/10.12927/hcq.2011.22358
Floersch J (2004) The subjective experience of youth psychotropic treatment. Soc Work Mental Health 1(4):51–69. https://doi.org/10.1300/J200v01n04_04
Cohen D, McCubbin M, Collin J, Pérodeau G (2001) Medications as social phenomena. Health 5(4):441–469. https://doi.org/10.1177/136345930100500403
Lakhan SE, Hagger-Johnson GE (2007) The impact of prescribed psychotropics on youth. Clin Pract Epidemiol Mental Health 3:21. https://doi.org/10.1186/1745-0179-3-21
Kisely S, Lin E, Lesage A, Gilbert C, Smith M, Campbell LA, Vasiliadis H-M (2009) Use of administrative data for the surveillance of mental disorders in 5 provinces. Can J Psychiatry 54(8):571–575. https://doi.org/10.1177/070674370905400810
Acknowledgements
We want to thank Jeff Bakal, Lead of Health Research Methods and Analytics Alberta Health Services/University of Alberta, and SPOR Data Platform for his input into developing this paper.
Funding
None declared.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors are unaware of any real or perceived conflicts of interest.
Data access
Data for this manuscript came from multiple administrative databases accessed through the Health Research Methods and Analytics unit, Alberta Health Services.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Leung, B.M.Y., Kellett, P., Youngson, E. et al. Trends in psychiatric disorders prevalence and prescription patterns of children in Alberta, Canada. Soc Psychiatry Psychiatr Epidemiol 54, 1565–1574 (2019). https://doi.org/10.1007/s00127-019-01714-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-019-01714-w