Abstract
Aims/hypothesis
The aim of this study was to perform a detailed analysis of cytokine toxicity in the new human EndoC-βH1 beta cell line.
Methods
The expression profile of the antioxidative enzymes in the new human EndoC-βH1 beta cells was characterised and compared with that of primary beta cells in the human pancreas. The effects of proinflammatory cytokines on reactive oxygen species formation, insulin secretory responsiveness and apoptosis of EndoC-βH1 beta cells were determined.
Results
EndoC-βH1 beta cells were sensitive to the toxic action of proinflammatory cytokines. Glucose-dependent stimulation of insulin secretion and an increase in the ATP/ADP ratio was abolished by proinflammatory cytokines without induction of IL-1β expression. Cytokine-mediated caspase-3 activation was accompanied by reactive oxygen species formation and developed more slowly than in rodent beta cells. Cytokines transiently increased the expression of unfolded protein response genes, without inducing endoplasmic reticulum stress-marker genes. Cytokine-mediated NFκB activation was too weak to induce inducible nitric oxide synthase expression. The resultant lack of nitric oxide generation in EndoC-βH1 cells, in contrast to rodent beta cells, makes these cells dependent on exogenously generated nitric oxide, which is released from infiltrating immune cells in human type 1 diabetes, for full expression of proinflammatory cytokine toxicity.
Conclusions/interpretation
EndoC-βH1 beta cells are characterised by an imbalance between H2O2-generating and -inactivating enzymes, and react to cytokine exposure in a similar manner to primary human beta cells. They are a suitable beta cell surrogate for cytokine-toxicity studies.
Similar content being viewed by others
Introduction
The generation of the new permanent human EndoC-βH1 beta cell line by Ravassard et al and Scharfmann et al [1, 2] has opened up new perspectives for diabetes research. This new human beta cell line has been shown to express all target structures crucial for physiological beta cell function and insulin secretion, and is characterised by excellent responsiveness to glucose and other secretagogues [1–3], but not to pyruvate and lactate [3]. Although this cell line has been used in a few studies exploring cytokine toxicity [4–6], the mechanisms of cytokine toxicity to human beta cells as they pertain to type 1 diabetes are not yet fully understood. Although the mechanisms of beta cell death in rat and mouse models of type 1 diabetes mellitus have been revealed in the last decades [7–15], our knowledge of in vitro cytokine action in human beta cells is limited. In the present study, we aimed to provide a detailed analysis of the mechanisms underlying cytokine action and toxicity in the human EndoC-βH1 beta cell line.
Methods
Maintenance and treatment of the human EndoC-βH1 beta cell line and EndoC-βH1 pseudoislets
EndoC-βH1 cells (Endocells, Paris, France) were cultured as previously described (see electronic supplementary material [ESM] Methods for details) [1]. Pseudoislets were generated and cultured as described in ESM Methods. The cell lines used were routinely checked for mycoplasma and were free from mycoplasma contamination. For cytokine toxicity analysis, cells and pseudoislets were treated with proinflammatory cytokines (see ESM Methods for details). 3-Morpholinosydnonimine (SIN-1) (50 μmol/l) or diethylenetriamine (DETA)-nitric oxide (NO) (100 μmol/l) were applied in the absence or presence of cytokines for 7 days or 24 h, respectively.
RNA isolation, cDNA preparation, RT-PCR, western blotting and immunofluorescence
Total RNA was isolated using the RNeasy Mini Kit (Qiagen, Hilden, Germany). After quality control, 1 μg of RNA was reverse transcribed using random hexamer primers. QuantiTect SYBR Green (Qiagen) was employed, as described in detail in the ESM Methods. Antibodies against copper-zinc superoxide dismutase (CuZnSOD) (1:3000), manganese superoxide dismutase (MnSOD) (1:3000), glutathione peroxidase (GPx)1 (1:7500), catalase (CAT) (1:5000), IL-1β (1:100), nuclear factor erythroid-2 related factor 2 (NRF2) (1:1000) and β-actin (1:250) (as the loading control) were used to analyse protein expression by western blotting, as described in detail in the ESM Methods. For immunofluorescence, human EndoC-βH1 cells were stained with specific antibodies for CuZnSOD, MnSOD, GPx, CAT and insulin (for details, see ESM Methods).
Human pancreases and in situ PCR analysis
Human pancreases from non-diabetic donors were obtained by organ resection during surgical intervention or from organ donors (ESM Table 1). Tissue was handled and processed as approved by the Hannover Medical School Ethics Committee. The in situ PCR analysis was performed and quantified as previously described (for details, see ESM Table 2) [16]. The primer sequences used are listed in ESM Table 3.
Caspase-3 assay, flow cytometric quantification of total cell death and reactive oxygen species measurement
Cells were seeded at a density of 7000 cells/well onto 96-well coated plates 5 days before the addition of test compounds. A total of 50 pseudoislets of comparable size were handpicked, followed by treatment with the indicated cytokines. Activation of caspase-3 was quantified using the Caspase-Glo-3/7 kit (Promega, Mannheim, Germany) according to the manufacturer’s instructions. Samples were measured on the GloMax-Multi Detection System (Promega) and data were imported into Instinct software version 3.1.2 (Promega) prior to data analysis. Data are expressed as percentages of cells without exposure to test compounds. Total cell death was quantified using flow cytometry (CyFlow ML, Partec, Münster, Germany), as described in the ESM Methods. Overall oxidative and nitrosative stress by DCF fluorescence and hydroxyl radical production by 3′-(p-hydroxyphenyl) fluorescein were assessed as previously described (see ESM Methods for details) [10].
Insulin secretion, ATP content and NFкB reporter gene assay
The assessment of insulin secretion and ATP content, and the quantification of NFкB activity, was performed using established methods [3]. Details are provided in the ESM Methods.
Data analysis
All data are expressed as means ± SEM. Unless otherwise stated statistical analyses were performed by one-way ANOVA followed by the Bonferroni test using the Prism analysis program (GraphPad, San Diego, CA, USA). Only p values of <0.05 were considered significant.
Results
Antioxidative enzyme expression in human EndoC-βH1 beta cells
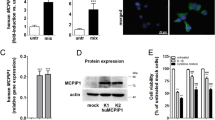
EndoC-βH1 beta cells exhibited high expression of the superoxide dismutase isoenzymes (mitochondrial MnSOD [also known as SOD2] and cytoplasmic CuZnSOD [also known as SOD1]) by both RT-PCR at the gene level as well as by western blotting at the protein level (Table 1, Fig. 1a). In contrast, gene and protein expression of the H2O2-inactivating enzymes CAT and GPx (GPX1) was much lower (p < 0.01) (Table 1, Fig. 1a). This observation was verified by specific immunofluorescent staining for the aforementioned antioxidative enzymes. As shown in Fig. 1b, EndoC-βH1 beta cells revealed strong immunostaining for CuZnSOD and MnSOD, and markedly weaker immunostaining for GPx1, followed by CAT.
Antioxidative enzyme protein expression in EndoC-βH1 beta cells. (a) The western blots shown are representative of four to eight independent experiments. Positive controls (PCs) for antibodies were performed in RINm5F-CuZnSOD cells, RINm5F-MnSOD cells, RINm5F-CAT cells and RINm5F-GPx. (b) For immunofluorescence analyses, EndoC-βH1 cells were seeded onto coated chamber slides and fixed and immunostained after 3 days. Green, protein of interest; red, insulin; blue (DAPI), nuclei. Images were captured and analysed with an IX81 fluorescence microscope (Olympus, Hamburg, Germany) using a × 60 oil objective; scale bar, 1 μm
Antioxidative enzyme expression in primary beta cells of human pancreases
To determine the gene expression profile of these antioxidative enzymes in the different cell types of human pancreatic islets, we performed in situ PCR analyses in human pancreatic sections. The expression of genes encoding superoxide inactivating enzymes (CuZnSOD and MnSOD) and H2O2-inactivating enzymes (GPX1 and CAT) was detected in both non-beta cells and beta cells (Fig. 2a). The superoxide dismutases showed the highest expression levels of all the investigated antioxidative enzymes, and the level was around 1.4-fold higher in non-beta cells than in beta cells (Fig. 2b, ESM Table 2). However, the expression levels of the H2O2-inactivating enzymes GPX1 and CAT were markedly lower in beta cells than in non-beta cells. CAT revealed the lowest expression (15-fold lower), followed by GPX1 (threefold lower) in beta cells, when compared with the respective expression levels in non-beta cells (Fig. 2b, ESM Table 2).
Gene expression of different antioxidative enzymes in human pancreatic islets by in situ PCR. (a) Gene expression of CuZnSOD, MnSOD, CAT and GPX1 in non-beta cells and beta cells, as visualised by a green fluorescence staining (Cy2) followed by immunostaining for insulin (Cy3, red) to identify beta cells and nuclear counterstaining with DAPI (blue); Scale bar, 10 μm (arrow denotes an erythrocyte). Orange colour indicates an overlay of green enzyme gene and red insulin staining. (b) Densitometric quantification was performed, as described in the legend to ESM Table 2. Sections were analysed with an Olympus BX61 microscope (Olympus, Hamburg, Germany) using a × 40 objective. Pictures are representative of 20 islets analysed in each of four human pancreases
Cytokine toxicity in human EndoC-βH1 beta cells
Proinflammatory cytokines induced time-dependent activation of the effector caspase-3, with a significant effect after 3 days and the strongest effect after 7 days of incubation with cytokines (Fig. 3a). IL-1β (60 U/ml) and TNF-α (185 U/ml) mildly induced caspase-3 activation, whereas IFN-γ (14 U/ml) alone had no effect (Fig. 3b). The IL-1β-induced caspase-3 activation was slightly potentiated by TNF-α or IFN-γ (Fig. 3b). A combination of TNF-α and IFN-γ also caused a slight potentiation (Fig. 3b). The effect of IL-1β was concentration-dependent, as shown by the greater caspase-3 activation in the presence of the 10× IL-1β (600 U/ml) concentration (Fig. 3b). The most prominent effect was observed with a mixture of the three cytokines (IL-1β, TNF-α and IFN-γ) (Fig. 3b). This observation is in accordance with total cell death rates, as assessed by counterstaining with propidium iodide and Hoechst dye upon treatment with cytokines (ESM Fig. 1).
Cytokine-mediated toxicity to EndoC-βH1 beta cells. Cells were incubated with IL-1β (60 or 600 U/ml [×10]), TNF-α (185 U/ml), IFN-γ (14 U/ml), IL-1β (60 U/ml) + TNF-α (185 U/ml), IL-1β (60 U/ml) + IFN-γ (14 U/ml) or TNF-α (185 U/ml) + IFN-γ (14 U/ml), or with a cytokine mixture (IL-1β [60 U/ml] + TNF-α [185 U/ml] + IFN-γ [14 U/ml]). (a) Time-dependent caspase-3 activation (white circles, untreated cells; black squares, cells treated with IL-1β × 10; black circles, cells treated with cytokine mixture). (b) Caspase-3 activation by various cytokines after 7 days. (c) NFκB activation after 24 h. (d) Overall oxidative stress after 7 days. (e) Hydroxyl radical generation after 7 days. (f) Caspase-3 activation by DETA-NO (100 μmol/l) after 24 h and (g) by SIN-1 (50 μmol/l) after 7 days in the absence or presence of cytokine mixture. (h) Overall oxidative and nitrosative stress by DETA-NO after 24 h or (i) by SIN-1 after 7 days of cytokine mixture exposure. Data are means ± SEM of four to eight independent experiments. *p < 0.05, **p < 0.01, ***p < 0.001 vs untreated; † p < 0.05 and ‡ p < 0.01 vs treated with the same cytokine (ANOVA followed by Bonferroni)
Next, we studied whether the formation of EndoC-βH1 islet-like structures (pseudoislets) rendered EndoC-βH1 beta cells more sensitive to proinflammatory cytokines. As shown in ESM Fig. 2a, 24 h exposure of pseudoislets to IL-1β alone and/or the cytokine mixture resulted in significant caspase-3 activation, suggesting that pseudoislets exhibit an earlier and greater sensitivity towards cytokine toxicity than equivalent EndoC-βH1 monolayers. These results were confirmed by counterstaining with propidium iodide and Hoechst dye (ESM Fig. 2b).
Insights into the mechanisms underlying cytokine-mediated toxicity in human EndoC-βH1 beta cells
Incubation of EndoC-βH1 cells for 24 h with IL-1β alone (60 U/ml) or with IL-1β in combination with TNF-α or with IFN-γ resulted in activation of the transcription factor NFκB (Fig. 3c). A comparable level of activation was also seen at the 10× concentration of IL-1β (600 U/ml) (Fig. 3c). TNF-α or IFN-γ alone or TNF-α and IFN-γ in combination showed no effect (Fig. 3c). The mixture of IL-1β, TNF-α and IFN-γ caused the strongest activation of NFκB (Fig. 3c). In addition, the gene expression of NRF1 and NRF2 (also known as NFE2L1 and NFE2L2) was determined in EndoC-βH1 cells before and after stimulation with beta cell toxic cytokines. As shown in ESM Fig. 3 exposure of EndoC-βH1 cells to IL-1β alone or a cytokine mixture for 1, 3, and 7 days had no effect on de novo synthesis of NRF1 (ESM Fig. 3a) or NRF2 (ESM Fig. 3b). This observation was confirmed by western blotting (ESM Fig. 3c). Thus, NRF2 is unlikely to be involved in regulating the antioxidant response upon cytokine-mediated toxicity in EndoC-βH1 cells.
Cytokines increased DCF fluorescence, a universal indicator of nitro-oxidative stress by reactive species, after 7 days of exposure (Fig. 3d). The most potent stimulation of DCF fluorescence was caused by the mixture of the three cytokines (Fig. 3d). The effects of IL-1β (60 and 600 U/ml) alone and in combination with TNF-α or IFN-γ were also significant, but less pronounced (Fig. 3d). Upon incubation with the cytokine mixture, a pronounced significant induction of hydroxyl radical formation was evident (Fig. 3e).
Expression of inducible (i) NO synthase (NOS) was undetectable in EndoC-βH1 beta cells. Cytokines failed to induce iNOS expression at either the gene or protein level at any analysed time point between 1 and 7 days of incubation (data not shown). Endothelial NOS and neuronal NOS were also not detected (data not shown). Incubation with an iNOS blocker, l-nitroarginine, reduced neither cytokine-mediated toxicity nor DCF oxidation (data not shown). Nevertheless, EndoC-βH1 cells were sensitive to NO toxicity, as documented by both caspase-3 activation and induction of DCF oxidation after exposure to the NO donors SIN-1 and DETA-NO (Fig. 3f–i). SIN-1 and DETA-NO had an additive effect on cytokine-mixture-mediated caspase-3 activation (Fig. 3f,g) and potentiated cytokine-mediated oxidative stress, as measured by DCF (Fig. 3h,i). We used these two NO donors because they differ in their actions and time lines. DETA-NO is known to be a pure NO donor and acts more quickly than SIN-1. SIN-1 is an NO donor that also releases a certain number of superoxide radicals as a by-product. It acts more slowly than other NO donors and therefore allows long-term co-incubations with cytokines (7 days) in studies with EndoC-βH1 cells.
Next, the expression of unfolded protein response (UPR) genes encoding endoplasmic reticulum (ER) adaptive functions and of ER stress markers was analysed after 1, 3 and 7 days of cytokine exposure by real-time RT-PCR (Fig. 4, ESM Fig. 4a–c). The gene expression of GRP94 (also known as HSP90B1) and BIP (also known as HSPA5), which enhance the ER folding capacity, was significantly increased upon exposure to proinflammatory cytokines for 1 day when compared with control cells (Fig. 4a,b). After 3 and 7 days of treatment with IL-1β alone or the cytokine mixture, the induced expression of UPR-encoding genes returned to control levels (Fig. 4a,b). In contrast, the expression of the ER stress genes CHOP (also known as DDIT3) (Fig. 4c), XBP1spliced, ATF6 and ATF4 (ESM Fig. 4a–c) was not affected by IL-1β alone or the cytokine mixture at any analysed time point, strongly indicating that none of the ER stress pathways was activated under these experimental conditions. Interestingly, however, in the presence of the NO donor DETA-NO, beta cell toxic cytokines caused a significant induction of the ER stress markers CHOP (Fig. 4d), XBP1spliced and ATF4, but not of ATF6 (ESM Fig. 4d–f). Thus, the presence of intracellular NO might be required to induce cytokine-mediated ER stress.
Expression of UPR-encoding genes and of the ER stress marker CHOP in response to cytokines in EndoC-βH1 beta cells. Cells were incubated with either IL-1β (600 U/ml) or with a cytokine mixture (IL-1β [60 U/ml], TNF-α [185 U/ml] and IFN-γ [14 U/ml]) for 1, 3 or 7 days, and the following genes were then measured using quantitative real-time PCR: (a) GRP94, (b) BIP, (c) CHOP and (d) CHOP in the presence of 100 μmol/l DETA-NO. Data are means ± SEM of four or five independent experiments. *p < 0.05, **p < 0.01, ***p < 0.001 vs untreated (ANOVA followed by Bonferroni). AU, arbitrary units
Insulin secretory responsiveness of EndoC-βH1 beta cells to stimulation by glucose in the absence or presence of proinflammatory cytokines
Glucose induced a significant concentration-dependent stimulation of insulin secretion from EndoC-βH1 beta cells in the concentration range 5.5–30 mmol/l (Fig. 5a). Exposure of EndoC-βH1 cells to IL-1β (600 U/ml) or to the cytokine mixture (IL-1β, TNF-α and IFN-γ) for 1 h augmented glucose-stimulated insulin secretion (GSIS) (ESM Fig. 5a). This stimulatory effect was abolished after 24 h incubation with cytokines (ESM Fig. 5b), while a prolonged 7-day exposure to cytokines resulted in a virtually complete loss of GSIS (Fig. 5a). Interestingly, even a 7-day exposure to 30 mmol/l glucose failed to induce the expression of IL-1β in human EndoC-βH1 beta cells (Fig. 5d).
Effects of cytokines on insulin secretion and ATP content in EndoC-βH1 beta cells. EndoC-βH1 beta cells were left untreated (white bars), treated with IL-1β (600 U/ml; grey bars) or treated with a cytokine mixture composed of IL-1β (60 U/ml), TNF-α (185 U/ml) and IFN-γ (14 U/ml) (black bars) for 7 days. After overnight starvation and subsequent incubation with glucose (Glc; 3, 5.5, 10 or 30 mmol/l) for 1 h, insulin secretion and ATP content were analysed. Data are means ± SEM of four to eight independent experiments. (a) Insulin secretion, (b) ATP content and (c) ATP/ADP ratio. Data are means ± SEM of four to six independent experiments. *p < 0.05, **p < 0.01 vs 3 mmol/l Glc; † p < 0.05, ‡ p < 0.005 vs the same Glc concentration in untreated cells (ANOVA followed by Bonferroni). (d) IL-1β western blot after 7 days of exposure to 5.5 or 30 mmol/l Glc; the positive control (PC) was a cell extract of human-293 cells transfected with human IL-1β. EndoC-βH1 cell extracts from two independent experiments (Exp.) are shown
ATP content of EndoC-βH1 beta cells in the absence or presence of proinflammatory cytokines
ATP content was not glucose-dependent (Fig. 5b). Exposure to a high concentration of IL-1β (600 U/ml) and to the cytokine mixture for 7 days led to a significant reduction of ATP content at 30 mmol/l glucose (Fig. 5b). The ATP/ADP ratio in human EndoC-βH1 beta cells increased along with increasing glucose concentrations (10 and 30 mmol/l) in the culture medium (Fig. 5c). This increase in the ATP/ADP ratio was blunted by IL-1β (600 U/ml) and the cytokine mixture (Fig. 5c).
Discussion
Type 1 diabetes is an autoimmune disease characterised by a loss of pancreatic beta cells caused by proinflammatory cytokine-mediated toxicity [13, 17–19]. In the current study, maximal toxicity was observed with a mixture of three cytokines, IL-1β, TNF-α and IFN-γ, which has been shown to simulate the proinflammatory cytokine pattern in the infiltrating immune cells in the islets of Langerhans in patients with type 1 diabetes [13, 16, 20, 21]. Combinations of two of the cytokines (in particular with IL-1β) were less toxic, confirming an earlier observation [5]. However, the cytokine response was more sluggish in EndoC-βH1 beta cells than has been reported in other cell types, at around three times slower than in rodent beta cells [5, 10, 11]. The vulnerability of EndoC-βH1 beta cells towards proinflammatory cytokines could be significantly enhanced by a three-dimensional configuration of EndoC-βH1 beta cells as pseudoislets, which can be attributed to improved cell–cell contact. Our results in EndoC-βH1 beta cells are in line with previous observations in human islets [20, 22–24].
EndoC-βH1 beta cells are well equipped with all components of the cellular machinery for glucose responsiveness, as we have recently shown [3]. In the current study, insulin secretion from EndoC-βH1 beta cells responded to glucose stimulation, confirming earlier observations [1, 3]. Exposure to cytokines abolished GSIS, along with loss of a glucose-induced increase of the ATP/ADP ratio, consistent with previous observations in human islets [25–27]. The observed reduction in GSIS was not accompanied by a parallel induction of IL-1β expression in the EndoC-βH1 beta cells, as previously reported for human beta cells [28].
EndoC-βH1 beta cells show a profile of antioxidative enzyme equipment comparable with that of human and rat beta cells [23, 29]. In particular, they express the superoxide dismutase isoenzymes at a high level and show a very low expression of the H2O2- inactivating enzymes GPx and CAT. The expression of GPx was somewhat higher than that of peroxisomally expressed CAT. This imbalance of superoxide radical-dismutating and H2O2-detoxifying enzymes was also verified in beta cells of islets residing in the human pancreas parenchyma, using a special quantitative in situ PCR technique [16]. This method permits analysis of the gene expression level in each individual cell of the islet [16], thereby bypassing the problems with isolating single cells from isolated human islets [30]. These analyses also revealed that non-beta cells in human islets, in contrast to beta cells, express the H2O2-detoxifying enzymes at the same high level as the superoxide radical-dismutating enzymes. Thus, a comparison between expression levels in the EndoC-βH1 cell line and isolated whole islets is likely to overestimate the expression levels in the latter due to the non-beta cell component in primary human islets. It is therefore not surprising that somewhat higher expression levels of H2O2-inactivating enzymes have been found in isolated human islets [23, 31]. These results provide further support for the fact that beta cells in human pancreatic islets are more susceptible to proinflammatory cytokine toxicity than other islet cell types, further strengthening the concept of a particular vulnerability of beta cells [12]. Thus, the well-known imbalance between the generation and inactivation of H2O2 in pancreatic beta cells, in particular in mitochondria, which comprise the primary intracellular sites of reactive oxygen species (ROS)-mediated cytokine toxicity [9, 10, 12, 14, 29, 32], is also likely to play a crucial role in cytokine toxicity in this new human beta cell line.
Activation of the transcription factor NFκB is a key element in cytokine-mediated beta cell death in rodent insulin-secreting cells [7]. We observed a rather mild activation of this transcription factor in EndoC-βH1 beta cells, much weaker than in rodent insulin-producing cells [11]. This NFκB activation was primarily dependent on IL-1β, which is in line with a corresponding observation in human islets [24]. The weak cytokine-mediated activation of NFκB in EndoC-βH1 beta cells, as in human islets, failed to induce the iNOS pathway [22, 24, 33], which is at variance to rodent beta cells [7, 13, 19, 21, 34–39]. Our results confirm recent studies in EndoC-βH1 beta cells that reported virtually no expression of iNOS [4, 40]. In addition, we documented a lack of expression of other NOS isoforms: endothelial NOS and neuronal NOS. Thus, similar to human islets [24, 41], EndoC-βH1 beta cells are apparently not capable of producing NO.
Nonetheless, we observed significant ROS production after stimulation with the cytokine mixture, and this production was not reduced by the iNOS blocker l-nitroarginine. This excludes an NO-mediated component in the increased DCF oxidation. The imbalance of the expression of superoxide radical-dismutating and H2O2-detoxifying enzymes in EndoC-βH1 beta cells supports the conclusion that H2O2 generation is responsible for the increased DCF fluorescence. In the case of proinflammatory cytokine toxicity, the mitochondria are the site of H2O2 formation [9], generated through the action of MnSOD upon superoxide radicals originating from the respiratory chain [10]. This increased H2O2 production is ultimately the basis for the generation of the highly toxic hydroxyl radical in the Fenton reaction [10]. Indeed, the results of this study show a significant production of hydroxyl radicals upon exposure to the cytokine mixture. The magnitude of hydroxyl radical production in EndoC-βH1 beta cells is lower than that in rodent cells, where hydroxyl radical formation is fostered through an interaction between H2O2 and NO [10].
ER stress is thought to contribute to the toxic effects of proinflammatory cytokines in rodent beta cells [8]. In the present study, we observed a significant activation of UPR genes fostering cytoprotective ER chaperone protein expression in EndoC-βH1 beta cells after 1 day, which vanished after longer exposure to the cytokine mixture. However, the cytokine mixture did not induce the expression of CHOP, the most important proapoptotic ER stress marker in rodent beta cells [8], or of other ER stress response genes, which is at variance with beta cells of rodent origin [11, 42, 43]. This observation is in contrast to a recent report by Brozzi et al [4]. This difference may be related to the use of 2% FCS in their incubation medium [4]. In our experiments, we followed the original tissue culture protocol devised for this particular cell line by the manufacturer (Endocells). A possible reason for the failure to detect ER stress in response to proinflammatory cytokines might be the lack of iNOS expression and concomitant NO production in EndoC-βH1 beta cells. This theory is supported by the observation that proinflammatory cytokines mildly increased the expression of ER stress markers in the presence of the NO donor DETA-NO. Our results are in agreement with the only partial and weak ER stress marker expression observed in pancreatic beta cells from patients with type 1 diabetes [44]. Thus, beta cells of human origin are apparently capable of better coping with cytokine-mediated stress.
An explanation for the observed discrepancy in cytokine toxicity between beta cells of rodent and human origin could be the lack of endogenous NO production in beta cells of human islets. In the pancreatic islets of type 1 diabetes patients, the membrane-permeable NO originates from the infiltrating immune cells [16]. This NO could, in the presence of a trace metal, promote (in a reaction with H2O2) the formation of the highly toxic hydroxyl radical [10], thereby contributing to beta cell demise. The observation that the NO donors SIN-1 and DETA-NO increased the sensitivity of EndoC-βH1 beta cells to cytokine toxicity provides support for a role of NO in the toxic effect of proinflammatory cytokines in beta cells of human origin. This situation is also known from other autoimmune diseases, where iNOS is induced only in the infiltrating immune cells, and not in the cells of the target organ [45]. This difference between the in vitro and in vivo situation might explain the weaker in vitro toxicity of the cytokines towards the EndoC-βH1 beta cells, as compared with rodent beta cells. The lack of NO production in human beta cells [22, 24] as well as in EndoC-βH1 beta cells thus emphasises the role of the beta cell as an innocent bystander, rather than an active participant, in the process of autoimmune-mediated beta cell destruction in patients with type 1 diabetes mellitus.
Abbreviations
- CAT:
-
Catalase
- CuZnSOD:
-
Copper-zinc superoxide dismutase
- DETA-NO:
-
Diethylenetriamine–nitric oxide
- ER:
-
Endoplasmic reticulum
- GPx:
-
Glutathione peroxidase
- GSIS:
-
Glucose-stimulated insulin secretion
- iNOS:
-
Inducible nitric oxide synthase
- MnSOD:
-
Manganese superoxide dismutase
- NO:
-
Nitric oxide
- ROS:
-
Reactive oxygen species
- SIN-1:
-
3-Morpholinosydnonimine
- UPR:
-
Unfolded protein response
References
Ravassard P, Hazhouz Y, Pechberty S et al (2011) A genetically engineered human pancreatic beta cell line exhibiting glucose-inducible insulin secretion. J Clin Invest 121:3589–3597
Scharfmann R, Pechberty S, Hazhouz Y et al (2014) Development of a conditionally immortalized human pancreatic beta cell line. J Clin Invest 124:2087–2098
Gurgul-Convey E, Kaminski MT, Lenzen S (2015) Physiological characterization of the human EndoC-βH1 β-cell line. Biochem Biophys Res Commun 464:13–19
Brozzi F, Nardelli TR, Lopes M et al (2015) Cytokines induce endoplasmic reticulum stress in human, rat and mouse beta cells via different mechanisms. Diabetologia 58:2307–2316
Grieco FA, Moore F, Vigneron F et al (2014) IL-17A increases the expression of proinflammatory chemokines in human pancreatic islets. Diabetologia 57:502–511
Fred RG, Kappe C, Ameur A et al (2015) Role of the AMP kinase in cytokine-induced human EndoC-βH1 cell death. Mol Cell Endocrinol 414:53–63
Eizirik DL, Mandrup-Poulsen T (2001) A choice of death-the signal-transduction of immune-mediated beta cell apoptosis. Diabetologia 44:2115–2133
Eizirik DL, Miani M, Cardozo AK (2013) Signalling danger: endoplasmic reticulum stress and the unfolded protein response in pancreatic islet inflammation. Diabetologia 56:234–241
Gurgul E, Lortz S, Tiedge M, Jörns A, Lenzen S (2004) Mitochondrial catalase overexpression protects insulin-producing cells against toxicity of reactive oxygen species and proinflammatory cytokines. Diabetes 53:2271–2280
Gurgul-Convey E, Mehmeti I, Lortz S, Lenzen S (2011) Cytokine toxicity in insulin-producing cells is mediated by nitro-oxidative stress-induced hydroxyl radical formation in mitochondria. J Mol Med 89:785–798
Kacheva S, Lenzen S, Gurgul-Convey E (2011) Differential effects of proinflammatory cytokines on cell death and ER stress in insulin-secreting INS1E cells and the involvement of nitric oxide. Cytokine 55:195–201
Lenzen S (2008) Oxidative stress: the vulnerable β-cell. Biochem Soc Trans 36:343–347
Mandrup-Poulsen T (2003) Beta cell death and protection. Ann N Y Acad Sci 1005:32–42
Mehmeti I, Gurgul-Convey E, Lenzen S, Lortz S (2011) Induction of the intrinsic apoptosis pathway in insulin-secreting cells is dependent on oxidative damage of mitochondria but independent of caspase-12 activation. Biochim Biophys Acta 1813:1827–1835
Melloul D (2008) Role of NF-kB in β-cell death. Biochem Soc Trans 36:334–339
Jörns A, Arndt T, Meyer zu Vilsendorfet al A (2014) Islet infiltration, cytokine expression and beta cell death in the NOD mouse, BB rat, Komeda rat, LEW.1AR1-iddm rat and humans with type 1 diabetes. Diabetologia 57:512–521
Atkinson MA, Maclaren NK (1994) The pathogenesis of insulin-dependent diabetes mellitus. N Engl J Med 331:1428–1436
Mandrup-Poulsen T (2003) Apoptotic signal transduction pathways in diabetes. Biochem Pharmacol 66:1433–1440
Hansen JB, Moen IW, Mandrup-Poulsen T (2014) Iron: the hard player in diabetes pathophysiology. Acta Physiol (Oxf) 210:717–732
Eizirik DL, Sandler S, Welsh N et al (1994) Cytokines suppress human islet function irrespective of their effects on nitric oxide generation. J Clin Invest 93:1968–1974
Nerup J, Mandrup-Poulsen T, Helqvist S et al (1994) On the pathogenesis of IDDM. Diabetologia 37(Suppl 2):S82–S89
Welsh N, Eizirik DL, Sandler S (1994) Nitric oxide and pancreatic beta cell destruction in insulin dependent diabetes mellitus: don’t take NO for an answer. Autoimmunity 18:285–290
Welsh N, Margulis B, Borg LA et al (1995) Differences in the expression of heat-shock proteins and antioxidant enzymes between human and rodent pancreatic islets: implications for the pathogenesis of insulin-dependent diabetes mellitus. Mol Med 1:806–820
Hindlycke H, Lu T, Welsh N (2012) Cytokine-induced human islet cell death in vitro correlates with a persistently high phosphorylation of STAT-1, but not with NF-kB activation. Biochem Biophys Res Commun 418:845–850
Kawahara DJ, Kenney JS (1991) Species differences in human and rat islet sensitivity to human cytokines. Monoclonal anti-interleukin-1 (IL-1) influences on direct and indirect IL-1-mediated islet effects. Cytokine 3:117–124
Soldevila G, Buscema M, Doshi M, James RF, Bottazzo GF, Pujol-Borrell R (1991) Cytotoxic effect of IFN-γ plus TNF-α on human islet cells. J Autoimmun 4:291–306
Padgett LE, Broniowska KA, Hansen PA, Corbett JA, Tse HM (2013) The role of reactive oxygen species and proinflammatory cytokines in type 1 diabetes pathogenesis. Ann N Y Acad Sci 1281:16–35
Maedler K, Sergeev P, Ris F et al (2002) Glucose-induced β cell production of IL-1β contributes to glucotoxicity in human pancreatic islets. J Clin Invest 110:851–860
Tiedge M, Lortz S, Drinkgern J, Lenzen S (1997) Relation between antioxidant enzyme gene expression and antioxidative defense status of insulin-producing cells. Diabetes 46:1733–1742
Banerjee M, Otonkoski T (2009) A simple two-step protocol for the purification of human pancreatic beta cells. Diabetologia 52:621–625
Eizirik DL, Sammeth M, Bouckenooghe T et al (2012) The human pancreatic islet transcriptome: expression of candidate genes for type 1 diabetes and the impact of pro-inflammatory cytokines. PLoS Genet 8:e1002552
Lenzen S, Drinkgern J, Tiedge M (1996) Low antioxidant enzyme gene expression in pancreatic islets compared with various other mouse tissues. Free Radic Biol Med 20:463–466
Pavlovic D, Chen MC, Bouwens L, Eizirik DL, Pipeleers D (1999) Contribution of ductal cells to cytokine responses by human pancreatic islets. Diabetes 48:29–33
Welsh N, Eizirik DL, Bendtzen K, Sandler S (1991) Interleukin-1β-induced nitric oxide production in isolated rat pancreatic islets requires gene transcription and may lead to inhibition of the Krebs cycle enzyme aconitase. Endocrinology 129:3167–3173
Cnop M, Welsh N, Jonas JC, Jörns A, Lenzen S, Eizirik DL (2005) Mechanisms of pancreatic β-cell death in type 1 and type 2 diabetes: many differences, few similarities. Diabetes 54(Suppl 2):S97–S107
Eizirik DL, Flodström M, Karlsen AE, Welsh N (1996) The harmony of the spheres: inducible nitric oxide synthase and related genes in pancreatic beta cells. Diabetologia 39:875–890
Eizirik DL, Pavlovic D (1997) Is there a role for nitric oxide in beta-cell dysfunction and damage in IDDM? Diabetes Metab Rev 13:293–307
McDaniel ML, Kwon G, Hill JR, Marshall CA, Corbett JA (1996) Cytokines and nitric oxide in islet inflammation and diabetes. Proc Soc Exp Biol Med 211:24–32
Rabinovitch A (1998) An update on cytokines in the pathogenesis of insulin-dependent diabetes mellitus. Diabetes Metab Rev 14:129–151
Oleson BJ, McGraw JA, Broniowska KA et al (2015) Distinct differences in the responses of the human pancreatic β-cell line EndoC-βH1 and human islets to proinflammatory cytokines. Am J Physiol Regul Integr Comp Physiol 309:R525–R534
Eizirik DL, Welsh N, Hellerstrom C (1993) Predominance of stimulatory effects of interleukin-1 beta on isolated human pancreatic islets. J Clin Endocrinol Metab 76:399–403
Cardozo AK, Ortis F, Storling J et al (2005) Cytokines downregulate the sarcoendoplasmic reticulum pump Ca2+ ATPase 2b and deplete endoplasmic reticulum Ca2+, leading to induction of endoplasmic reticulum stress in pancreatic β-cells. Diabetes 54:452–461
Oyadomari S, Takeda K, Takiguchi M et al (2001) Nitric oxide-induced apoptosis in pancreatic β cells is mediated by the endoplasmic reticulum stress pathway. Proc Natl Acad Sci U S A 98:10845–10850
Marhfour I, Lopez XM, Lefkaditis D et al (2012) Expression of endoplasmic reticulum stress markers in the islets of patients with type 1 diabetes. Diabetologia 55:2417–2420
Lenzen H, Lünnemann M, Bleich A, Manns MP, Seidler U, Jörns A (2012) Downregulation of the NHE3-binding PDZ-adaptor protein PDZK1 expression during cytokine-induced inflammation in interleukin-10-deficient mice. PLoS One 7:e40657
Acknowledgements
The excellent technical assistance of C. Schwab, M. Funck and A. Possler (Hannover Medical School) is gratefully acknowledged. The authors thank R. Scharfmann and P. Ravassard (Institut du cerveau et de la moelle (ICM), Biotechnology & Biotherapy Team, 75013 Paris, France) for advice with the EndoC-βH1 beta cell culture. The authors are very grateful to K. Dobashi (Department of Pediatrics, School of Medicine, University of Occupational and Environmental Health, Kitakyushu, Japan) for the antibodies against CuZnSOD, MnSOD and GPx.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The work leading to this publication has received support from the Innovative Medicines Initiative Joint Undertaking (grant agreement no. 155005, IMIDIA), the resources of which comprise financial contributions from the European Union’s Seventh Framework Programme (FP7/2007-2013) and in-kind contributions from companies in the European Federation of Pharmaceutical Industries and Associations. EG-C was supported by the Menarini Award of the German Diabetes Association and the “Habilitationsförderung für Frauen” of Hannover Medical School.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Contribution statement
EG-C and IM designed and performed experiments, analysed data, and created figures and tables; TP performed experiments with SIN-1; AJ performed in situ PCR experiments; and SL designed experiments, and supervised and coordinated the project. All authors wrote the manuscript and approved the final version of the manuscript. EG-C and IM are the guarantors of this work and take responsibility for the integrity of the data.
Additional information
Ewa Gurgul-Convey and Ilir Mehmeti contributed equally to this study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM
(PDF 871 kb)
Rights and permissions
About this article
Cite this article
Gurgul-Convey, E., Mehmeti, I., Plötz, T. et al. Sensitivity profile of the human EndoC-βH1 beta cell line to proinflammatory cytokines. Diabetologia 59, 2125–2133 (2016). https://doi.org/10.1007/s00125-016-4060-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-016-4060-y