Abstract
Aims/hypothesis
We investigated whether heterogeneous nuclear ribonucleoproteins F and K (hnRNP F, hnRNP K) mediate insulin inhibition of renal Agt expression and prevention of hypertension and kidney injury in an Akita mouse model of type 1 diabetes.
Methods
Adult male Akita mice (12 weeks old) were treated with insulin implants and killed at week 16. Untreated non-Akita littermates served as controls. The effects of insulin on blood glucose, systolic BP (SBP), renal proximal tubular cell (RPTC) gene expression and interstitial fibrosis were studied. We also examined immortalised rat RPTCs stably transfected with control plasmid or with plasmid containing rat Agt promoter in vitro.
Results
Insulin treatment normalised blood glucose levels and SBP, inhibited renal AGT expression but enhanced hnRNP F, hnRNP K and angiotensin-converting enzyme-2 expression, attenuated renal hypertrophy and glomerular hyperfiltration and decreased urinary albumin/creatinine ratio, as well as AGT and angiotensin II levels, in Akita mice. In vitro, insulin inhibited Agt but stimulated Hnrnpf and Hnrnpk expression in high-glucose media via p44/42 mitogen-activated protein kinase signalling in RPTCs. Transfection with Hnrnpf or Hnrnpk small interfering RNAs prevented insulin inhibition of Agt expression in RPTCs.
Conclusions/interpretation
These data indicate that insulin prevents hypertension and attenuates kidney injury, at least in part, through suppressing renal Agt transcription via upregulation of hnRNP F and hnRNP K expression in diabetic Akita mice. HnRNP F and hnRNP K may be potential targets in the treatment of hypertension and kidney injury in diabetes.
Similar content being viewed by others
Introduction
Intensive insulin therapy is the most effective treatment for preventing the progression of nephropathy in type 1 diabetes, although the underlying mechanisms remain incompletely understood [1–3]. The existence of a local renin–angiotensin system (RAS) within the kidney is well established [4]. Renal proximal tubular cells (RPTCs) express all components of the RAS [5–7]. Intrarenal RAS gene expression and urinary angiotensinogen (AGT, the sole precursor of angiotensins) levels are elevated in animal models of diabetes and hypertension and in humans with hypertension and/or diabetes [8–12]. Transgenic (Tg) mice specifically overexpressing Agt in their RPTCs develop hypertension, albuminuria, and tubular apoptosis [13–15]. Moreover, renal Agt overexpression and hyperglycaemia act in concert to enhance hypertension and kidney injury in diabetic mice [16, 17], indicating important roles for intrarenal RAS activation and hyperglycaemia in the development of hypertension and kidney injury in diabetes.
We previously reported that insulin inhibits high-glucose stimulation of rat renal Agt expression and RPTC hypertrophy via a putative insulin-responsive element in the Agt promoter [18–20] that interacts with two nuclear proteins, heterogeneous nuclear ribonucleoproteins F and K (hnRNP F, hnRNP K) in vitro [21, 22]. Recently, we observed that hnRNP F overexpression inhibited renal Agt expression and attenuated hypertension and kidney hypertrophy in Akita (mouse model of type 1 diabetes) Tg mice specifically overexpressing hnRNP F in their RPTCs [23]. These findings suggest that hnRNP F either acts alone or interacts with hnRNP K or other transcriptional factors to inhibit renal Agt transcription in diabetes.
The aim of the present study was to investigate the contribution of hnRNP F and hnRNP K to insulin inhibition of renal Agt expression and prevention of hypertension and kidney injury in Akita mice.
Methods
Reagents
d-glucose, d-mannitol, human insulin, PD98059 (an inhibitor of p44/42 mitogen-activated protein kinase [p44/42 MAPK]), wortmannin and Ly 294,002 (specific inhibitors of phosphatidylinositol 3-kinase) and anti-β-actin monoclonal antibody were purchased from Sigma-Aldrich Canada (Oakville, ON, Canada). U0126 (an inhibitor of p44/42 MAPK) was from Cell Signaling Technology (New England Biolabs, Whitby, ON, Canada). Normal glucose (5 mmol/l d-glucose) DMEM (catalogue no. 12320), penicillin/streptomycin and FBS were procured from Invitrogen (Burlington, ON, Canada). Insulin implants (Linβit), containing insulin of bovine, porcine or human origin (note: species of origin is not specified by the manufacturer), with a release rate of approximately 0.1 U (implant)−1 day−1 for >30 days), were bought from Linshin (Scarborough, ON, Canada). The pGL4 [Luc/Puro] vector containing the luciferase reporter was obtained from Promega (Sunnyvale, CA, USA). Rat Agt promoter (N-1495 to N+18) [24] was cloned from rat genomic DNA by conventional polymerase chain reaction with specific primers (NCBI reference sequence NW_003812957.1; sense primer: AAA GGT ACC AGT CTC TCT GGT CAC TAC CCA T and anti-sense primer: AAA AAG CTT GCC CAG ACA AGC ACA GCT AT) and inserted into pGL4.20 vector via Kpn I and Hind III restriction sites. Rat cAMP-responsive element binding protein (CREB) cDNA was cloned in our laboratory (J. S. D. Chan) and inserted into pRSV vector [25]. Rabbit polyclonal antibodies specific to hnRNP F (CTARRYIGIVKQAGLER, corresponding to amino acids 215 to 230 of mouse and human hnRNP F) [21] and polyclonal antibodies against rat AGT were generated in our laboratory (J. S. D. Chan) [26]. The following antibodies were used: rabbit polyclonal anti-hnRNP K, anti-transforming growth factor-beta 1 (TGF-β1), anti-ACE antibody (Santa Cruz Biotechnology, Santa Cruz, CA, USA), anti-ACE-2 antibody (R&D Systems, Minneapolis, MN, USA) and monoclonal anti-collagen type IV antibody (Chemicon International, Temecula, CA, USA). Scrambled Silencer Negative Control No. 1 siRNA and Hnrnpf and Hnrnpk small interfering RNAs (siRNAs) were obtained from Ambion (Austin, TX, USA) [22]. Oligonucleotides were synthesised by Invitrogen. Restriction and modifying enzymes were obtained from Invitrogen and Roche Biochemicals (Laval, QC, Canada).
Physiological studies
Adult male heterozygous Akita mice with a mutated Ins2 gene (C57BL6-Ins2 Akita/J) were purchased from Jackson Laboratories (Bar Harbor, ME, USA). Akita mice (10 weeks old) were divided into two groups, one with and one without insulin implants, at week 12 (eight mice per group), as described previously [16]. Briefly, diabetic mice received a subcutaneous insulin implant (two Linβit implants per 20 g body weight (BW) and one Linβit implant for each additional 5 g BW). Blood glucose levels were determined with small drops (about 2–3 μl/drop) of blood collected from the tail vein, following 4–5 h fasting, with an Accu-Chek Performa System (Roche Diagnostics, Laval, QC, Canada). Unless otherwise noted, data were collected from male Akita mice aged 10–16 weeks. Non-Akita littermates of the same age and sex served as wild type (WT) controls. All mice were allowed free access to standard mouse chow and water. Animal care and procedures were approved by the CRCHUM Animal Care Committee and followed the Principles of Laboratory Animal Care (NIH publication no. 85-23, revised 1985: http://grants1.nih.gov/grants/olaw/references/phspol.htm, accessed 20 November 2012).
Systolic BP (SBP) was measured with a BP-2000 tail-cuff pressure monitor (Visitech Systems, Apex, NC, USA) [13, 14, 16, 17, 23] in the morning, at least two or three times a week, for 5 weeks. The mice were accustomed to the procedure for at least 15–20 min per day for 5 days before the first SBP measurement. SBP values represent the mean ± SEM of two or three determinations per week per mouse per group. Twenty-four hours before the mice were killed, the BW was recorded and the mice were housed individually in metabolic cages. Blood from each individual mouse was collected (∼500–1,000 μl) by intracardiac exsanguination before its death and then centrifuged to obtain serum. Urine (∼100–400 μl/mouse) was collected and assayed by ELISA for albumin (Albuwell; Exocell, Philadelphia, PA, USA) and creatinine (Creatinine Companion; Exocell) [13, 14, 16, 17, 23].
The GFR was estimated according to the protocol described by Qi et al [27], as recommended by the Animal Models of Diabetic Complications (www.diacomp.org/, accessed 20 November 2012) with slight modifications [28]. Briefly, each mouse received a single intravenous bolus of 5% FITC–inulin and blood samples (each ∼20 μl) were collected from the saphenous vein at 3, 7, 10, 15, 35, 55 and 75 min post-FITC–inulin injection. Plasma fluorescence concentration was measured by Synergy 2 fluorometer (BioTek Instruments, Winooski, VT, USA) with 485 nm excitation wavelength and read at 538 nm emission wavelength. GFR was calculated according to the following equation: GFR = I/(A/α + B/β), where I is the amount of FITC–inulin bolus delivered, A and α are the y intercept and decay constant of the rapid (initial) decay phase, respectively, and B and β are the y intercept and decay constant of the slow decay phase, respectively [27].
The kidneys were removed immediately after GFR measurements, decapsulated and weighed before Percoll gradient isolation of renal proximal tubules (RPTs) [13, 14, 16, 17, 23]. Portions of freshly isolated RPTs from individual mice were immediately processed for total RNA or protein isolation. The remaining RPTs were then pooled, suspended in normal-glucose (5 mmol/l d-glucose plus 20 mmol/l d-mannitol) or high-glucose (25 mmol/l d-glucose) DMEM containing 1% depleted FBS with or without insulin (100 μmol/l) [18–22], and incubated ex vivo at 37°C for 16 h. At the end of the incubation period, RPTs were harvested and assayed for Agt, Hnrnpf, Hnrnpk and Ace2 mRNA expression.
Serum and urinary AGT and angiotensin II measurement
AGT in the serum and urine was quantified by ELISA (Immuno-Biological Laboratories, Minneapolis, MN, USA) [23]. To measure angiotensin II (ANG II) levels, serum and urine samples were extracted using a kit and were assayed by specific ELISA for ANG II (Bachem Americas, Torrance, CA, USA) [14, 17, 23].
Morphological studies
Kidneys were collected in Tissue-Tek cassettes (VWR Canlab, Montreal, QC, Canada), dipped immediately in ice-cold 4% paraformaldehyde, fixed for 24 h at 4°C and then processed by the CHUM Pathology Department. Tissue sections (3–4 μm thick, four or five sections per organ) were counterstained with periodic acid Schiff (PAS) or Masson’s trichrome [14, 16, 17, 23] and analysed under light microscopy by two independent investigators blinded to the treatments. The tubular luminal area and mean glomerular and RPTC volumes were assessed as described previously [14, 16, 17, 23].
Immunohistochemical staining of AGT, hnRNP F, hnRNP K, angiotensin-converting enzyme-2 (ACE-2), ACE, TGF-β1 and collagen IV was performed using a standard avidin–biotin–peroxidase complex method on four or five sections per kidney and three mouse kidneys per group (ABC Staining; Santa Cruz Biotechnology) [13, 14, 16, 17, 23]. Staining was analysed under light microscopy by two independent investigators blinded to treatment groups. TGF-β1- and collagen IV-immunostained images were quantified with National Institutes of Health ImageJ software (version 1.44p; http://imagej.nih.gov/ij) [13, 14, 16, 17, 23]. Immunostaining with non-immune normal rabbit serum in non-Akita mouse kidneys served as controls, and showed no staining (images not shown).
Effect of insulin on Agt, Hnrnpf and Hnrnpk expression in rat RPTCs
Immortalised rat RPTCs from passages 12–18 [6] that express the mRNA and protein of RAS components mimicking RPTCs in vivo were used. The plasmids pGL4-Agt N-1495/+18 were transfected into rat RPTCs, and stable transformants were selected in the presence of 0.6 mg/l of puromycin (Sigma-Aldrich Canada) according to the limiting dilution method [29].
To study the effect of insulin, 75–85% confluent stable transformants were synchronised overnight in serum-free 5 mmol/l d-glucose DMEM, then incubated in normal-glucose (5 mmol/l d-glucose plus 20 mmol/l d-mannitol) or high-glucose (25 mmol/l d-glucose) DMEM containing 1% depleted FBS and various concentrations of insulin (10−13 to 10−5 mol/l or 0.1 pmol/l to 10 μmol/l) for 24 h with or without PD 98059 (1 × 10−5 mol/l) or Ly 294,002 ((1 × 10−6 mol/l) or wortmannin (1 × 10−6 mol/l) or U0126 (1 × 10−6 mol/l) as described previously [18–20]. Promoter activity was measured by the luciferase activity assay [28]. RPTCs stably transfected with the plasmid pGL4 served as controls.
In additional studies, stable transformants (RPTCs) were transfected with scrambled siRNA or Hnrnpf siRNA or Hnrnpk siRNA [22], or with pRSV (empty vector), pRSV-Creb, pRSV-Hnrnpf and/or pRSV-Hnrnpk and the effects of insulin on Agt promoter activity and Agt mRNA expression were analysed after 24 h of incubation.
Real time-quantitative PCR (RT-qPCR) assays and western blotting
The expression of Agt, Hnrnpf, Hnrnpk, Ace, Ace2 and β-actin mRNA in mouse liver, isolated RPTs and cultured rat RPTCs was quantified by RT-qPCR using forward and reverse primers corresponding to their cDNA sequence as described previously [17, 21–23].
Western blotting was performed as described previously [21–23]. The relative density of AGT, hnRNP F, hnRNP K and β-actin bands was quantified by computerised laser densitometry (ImageQuant software [version 5.1]; Molecular Dynamics, Sunnyvale, CA, USA).
Statistical analysis
Statistical significance between the experimental groups was analysed by one-way ANOVA and subsequent Bonferroni test. Values are expressed as mean ± SEM. p < 0.05 was considered to be statistically significant.
Results
Physiological variables in mice
Blood glucose levels were significantly elevated in Akita mice compared with WT controls (Fig. 1a and Table 1). Insulin treatment decreased, though never completely normalised, blood glucose levels in Akita mice. Average SBP was significantly higher (by 20–25 mmHg) in Akita mice at the age of 11 weeks than in WT mice (p < 0.005) (Fig. 1b and Table 1) and remained higher for the duration of the study. Insulin treatment completely normalised SBP in Akita mice.
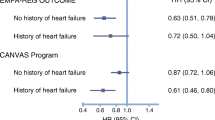
Insulin normalises elevated blood glucose levels, lowers systolic BP and ameliorates kidney injury in male Akita mice. (a) Longitudinal changes in mean blood glucose levels with fasting for 4–5 h in male WT (circles), Akita (triangles) and Akita mice treated with insulin implants (Akita-Ins, squares). (b) Longitudinal changes in mean SBP (measured two or three times per mouse per week in the morning without fasting) in male WT, Akita and Akita-Ins mice. Baseline SBP was measured daily over a 5-day period before initiation of treatment. (c–f) Urinary ACR (c), GFR (d), urinary ANG II (e) and urinary AGT levels (f) at week 16 in WT controls, Akita and Akita-Ins mice. Urinary AGT and ANG II levels were normalised with urinary creatinine levels. Values are means ± SEM, n = 8 per group. *p < 0.05, **p < 0.01 and ***p < 0.001, WT vs Akita. † p < 0.05 and †† p < 0.01, Akita vs Akita-Ins
Kidney size, kidney weight (KW, both kidneys), KW/BW ratio and heart weight (HW)/BW ratio were higher in Akita mice than in WT control mice. Insulin treatment normalised the KW/BW ratio and attenuated the HW/BW ratio in Akita mice (Table 1).
The albumin/creatinine ratio (ACR; Fig. 1c) and GFR (Fig. 1d) were significantly higher at the age of 16 weeks in male Akita mice than in WT mice, and these changes were normalised by insulin treatment.
Urinary levels of ANG II (Fig. 1e) and AGT (Fig. 1f) were significantly higher in Akita mice than in WT mice. Insulin treatment normalised the urinary ANG II levels and partially attenuated urinary AGT levels in Akita mice.
Histological and functional studies
Unlike WT controls, Akita mice developed renal structural damage (Fig. 2a). Histological findings included tubular luminal dilation with an accumulation of cell debris in the tubular lumen. Insulin treatment of Akita mice markedly reversed, though never completely resolved these abnormalities.
Insulin ameliorates glomerulotubular fibrosis and suppresses pro-fibrotic gene expression in Akita mice. (a) PAS staining in kidneys of WT control, Akita and Akita mice treated with insulin implant (Akita-Ins). Magnification ×100 and ×600. (b) Masson’s trichrome staining of collagenous components in kidneys of WT, Akita and Akita-Ins mice. Magnification ×600. (c) Semi-quantitative analysis of Masson’s trichrome staining in glomerulotubular areas of kidney sections from WT, Akita and Akita-Ins mice at the age of 16 weeks. (d) Immunohistochemical staining for TGF-β1 and (e) RT-qPCR of Tgfb1 mRNA expression in RPTs of WT, Akita and Akita-Ins mice. Magnification ×600. (f) Immunostaining for collagen type IV α1 and (g) RT-qPCR of Col4a1 in RPTs of WT, Akita and Akita-Ins mice. Magnification ×600. Values are means ± SEM, n = 8. ***p < 0.001
Renal tubular luminal area, glomerular tuft volume and RPTC volume were significantly increased in Akita mice compared with WT mice (Table 1). Insulin treatment normalised the tubular luminal area and glomerular tuft volume but did not completely reverse the increase in RPTC volume in Akita mice.
Masson’s trichrome staining, TGF-β1 and collagen type IV immunostaining revealed increased levels of collagenous components (Fig. 2b), TGF-β1 (Fig. 2d) and collagen type IV (Fig. 2f) in kidneys of Akita mice compared with WT controls. Once again, insulin treatment normalised these changes. Quantitative analysis of Masson trichrome-stained areas (Fig. 2c) and RT-qPCR for Tgfb1 and Col4a1 mRNA expression (Fig. 2e, g) confirmed these findings. These data indicate that insulin treatment effectively prevented tubulointerstitial fibrosis in Akita mice.
AGT, hnRNP F, hnRNP K, ACE and ACE2 levels in mouse kidneys
We detected increased AGT immunostaining in the RPTCs of Akita mice when compared with those of WT controls, and this was normalised by insulin treatment (Fig. 3a). In contrast, the RPTCs of Akita mice exhibited decreased immunostaining for both hnRNP F (Fig. 3b) and hnRNP K (Fig. 3c) compared with WT controls. Insulin treatment led to higher than normal expression of hnRNP F and hnRNP K. Western blotting for AGT, hnRNP F and hnRNP K (Fig. 3d, e, f) and RT-qPCR for Agt, Hnrnpf and Hnrnpk mRNA expression (Fig. 3g, h, i) from isolated RPTs confirmed these findings.
AGT, hnRNP F and hnRNP K expression in mouse kidneys at the age of 16 weeks. (a–c) Immunohistochemical staining for AGT (a), hnRNP F (b) and hnRNP K (c) in kidneys of WT control mouse, Akita mouse and Akita mouse treated with insulin implant (Akita-Ins), employing respective rabbit anti-AGT, anti-hnRNP F and anti-hnRNP K polyclonal antibodies. Magnification ×200. (d–f) Western blotting analysis of AGT (d), hnRNP F (e) and hnRNP K (f) levels in RPTs from kidneys of WT, Akita and Akita-Ins mice. (g–i) RT-qPCR of Agt (g), Hnrnpf (h) and Hnrnpk (i) mRNA expression in RPTs of WT, Akita and Akita-Ins mice. Values are means ± SEM, n = 8 per group. **p < 0.01 and ***p < 0.001
Interestingly, liver Agt mRNA and protein levels and serum AGT and ANG II levels did not differ significantly between the three groups of mice studied (see electronic supplementary material [ESM] Fig. 1).
Immunostaining for ACE-2 was decreased in RPTCs of Akita mice, compared with WT controls, and insulin treatment normalised this decrease (Fig. 4a). In contrast, the RPTCs of Akita mice exhibited increased immunostaining for ACE compared with WT controls (Fig. 4b). Insulin treatment, however, had no apparent effect on ACE levels in RPTCs of Akita mice (Fig. 4b). RT-qPCR for Ace2 and ACE mRNA expression (Fig. 4c, d) in isolated RPTs confirmed these findings.
ACE-2 and ACE expression in mouse kidneys at the age of 16 weeks and the effect of insulin on Agt, Hnrnpf, Hnrnpk and Ace2 mRNA expression in RPTs ex vivo. (a, b) Immunohistochemical staining for ACE-2 (a) and ACE (b) in kidneys of WT control mouse, Akita mouse and Akita mouse treated with insulin implant (Akita-Ins), employing respective rabbit anti-ACE-2 and anti-ACE polyclonal antibodies. Magnification ×600. (c, d) RT-qPCR of Ace2 (c) and Ace (d) mRNA expression in RPTs of WT, Akita and Akita-Ins mice. (e, f) RT-qPCR of Agt, Hnrnpf, Hnrnpk and Ace2 mRNA expression in RPTs isolated from WT (e) and Akita mice (f). Freshly isolated RPTs were incubated in normal-glucose (5 mmol/l d-glucose plus 20 mmol/l d-mannitol) or high-glucose (25 mmol/l d-glucose) medium in the absence or presence of insulin (10−7 mol/l or 100 μmol/l) for 16 h and then harvested for quantification of mRNA expression. The level of mRNA in RPTs incubated in medium containing 5 mmol/l d-glucose plus 20 mmol/l d-mannitol is expressed as percentage of control (100%). Values are means ± SEM, n = 3 per group. *p < 0.05, **p < 0.01 and ***p < 0.001, normal glucose vs control or high glucose vs normal glucose. White bars, normal glucose; light-grey bars, normal glucose + insulin; black bars, high glucose and dark-grey bars, high glucose + insulin
To investigate whether insulin could directly inhibit Agt and enhance Hnrnpf, Hnrnpk and Ace2 expression in RPTs in vivo, we incubated freshly isolated mouse RPTs in the absence or presence of insulin for 16 h ex vivo. Fig. 4e shows high-glucose stimulation of Agt mRNA and inhibition of Hnrnpf, Hnrnpk and Ace2 mRNA expression in RPTs of WT mice. Insulin treatment reversed these changes. Similar trends were also observed for the effect of high glucose and insulin on Agt, Hnrnpf, Hnrnpk and Ace2 mRNA expression in Akita RPTs (Fig. 4f). These findings demonstrate that insulin directly inhibits Agt and stimulates Hnrnpf, Hnrnpk and Ace2 mRNA expression in RPTs cultured ex vivo.
Effect of insulin on Agt, Hnrnpf and Hnrnpk expression in rat RPTCs in vitro
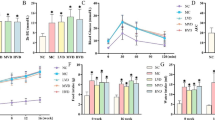
Consistent with our in vivo observations, high glucose (25 mmol/l d-glucose) stimulated Agt promoter activity in RPTCs compared with normal glucose (5 mmol/l d-glucose plus 20 mmol/l d-mannitol), and this change was inhibited by insulin in a dose- and time-dependent manner (Fig. 5a, b, respectively). PD 98059 and U0126, but not wortmannin or Ly 294,002, prevented insulin inhibition of Agt promoter activity (Fig. 5c) and Agt mRNA expression (Fig. 5d) in RPTCs. In contrast, RPTCs cultured in high-glucose medium exhibited decreased Hnrnpf (Fig. 5e) and Hnrnpk (Fig. 5f) mRNA expression as compared with RPTCs cultured in normal-glucose medium. Insulin treatment normalised both Hnrnpf and Hnrnpk expression (Fig. 5e, f). PD 98059 and U0126, but not wortmannin or Ly 294,002, rendered RPTCs insensitive to insulin. Thus, insulin can directly inhibit Agt and enhance Hnrnpf and Hnrnpk expression in RPTCs in high-glucose medium, signalling through the p44/p42 MAPK pathway.
Effect of insulin on Agt promoter activity and on Agt, Hnrnpf and Hnrnpk mRNA expression in rat RPTCs. Cells stably transfected with pGL4 rAgt N-1495/+18 were incubated in normal-glucose (5 mmol/l d-glucose plus 20 mmol/l d-mannitol or high-glucose (25 mmol/l d-glucose) DMEM in the absence or presence of various concentrations of insulin for 24 h (a) or for various time periods (b) with or without PD 98059 (10−5 mol/l), U0126 (10−6 mol/l), wortmannin (10−6 mol/l) or Ly 294,002 (10−6 mol/l) (c). Cells were harvested and assayed for luciferase activity. In (b): black triangles, normal glucose; white squares, normal glucose + insulin (10−7 mol/l or 100 μmol/l); black squares, high glucose; white triangles, high glucose + insulin (10−7 mol/l or 100 mmol/l). (d–f) Effect of insulin on Agt mRNA (d), Hnrnpf mRNA (e) and Hnrnpk mRNA (f) expression in high-glucose medium in the absence or presence of PD 98059, U0126, wortmannin or Ly 294,002. The levels of luciferase activity or mRNA in cells incubated in medium containing 5 mmol/l d-glucose plus 20 mmol/l d-mannitol are expressed as percentage of control (100%). The inhibitory effect of insulin is compared with cells cultured in 25 mmol/l d-glucose only. The results are expressed as means ± SEM, n = 3. **p < 0.01 and ***p < 0.001. Similar results were obtained in two separate experiments
Next, we investigated whether knock-down of hnRNP F or hnRNP K could prevent insulin inhibition of Agt expression at the transcriptional level. Transfection of RPTCs with Hnrnpf siRNA or Hnrnpk siRNA reduced endogenous hnRNP F or hnRNP K protein expression in a concentration-dependent manner in both cases (ESM Fig. 2). Scrambled siRNA had no effect. Transfection with either Hnrnpf siRNA or Hnrnpk siRNA attenuated insulin inhibition of Agt mRNA expression in a concentration-dependent manner (Fig. 6a, b). A combination of siRNAs of both Hnrnpf and Hnrnpk was more effective in attenuating the insulin inhibition of Agt mRNA expression than either of the siRNAs alone (Fig. 6c). Agt promoter activity assays confirmed that Hnrnpf siRNA and Hnrnpk siRNA abolished the inhibitory effect of insulin on Agt promoter activity in RPTCs in high-glucose medium (Fig. 6d, e). Again, a combination of Hnrnpf and Hnrnpk siRNA was more effective than either of the siRNAs alone (Fig. 6f). These findings lend additional support to the notion that insulin inhibition of Agt transcription is mediated, at least in part, via upregulation of both hnRNP F and hnRNP K in RPTCs in vivo.
Effect of Hnrnpf and Hnrnpk siRNAs on insulin inhibition of Agt expression in RPTCs. (a) Effect of Hnrnpf siRNA on Agt mRNA expression in RPTCs incubated in normal- or high-glucose medium with or without insulin quantified by RT-qPCR. (b) Effect of Hnrnpk siRNA on Agt mRNA expression in RPTCs incubated in normal or high glucose medium with or without insulin, quantified by RT-qPCR. (c) Effect of a combination of Hnrfpf and Hnrfpk siRNA on Agt mRNA expression in RPTCs incubated in normal- or high-glucose medium with or without insulin quantified by RT-qPCR. The levels of Agt mRNA in cells incubated in normal-glucose medium are expressed as arbitrary unit 1. The inhibitory effect of insulin was compared with cells cultured in 25 mmol/l d-glucose. (d) Effect of Hnrnpf siRNA or scrambled siRNA (Sc. SiRNA) on Agt promoter activity in RPTCs cultured in normal- or high-glucose medium with or without insulin. (e) Effect of Hnrnpk siRNA or Sc. siRNA on Agt promoter activity in RPTCs cultured in normal- or high-glucose medium with or without insulin. (f) Effect of a combination of Hnrnpf and Hnrnpk siRNAs on Agt promoter activity in RPTCs incubated in normal- or high-glucose medium with or without insulin. Cells were harvested following 24 h of incubation, and Agt promoter activity was assessed by the luciferase activity assay. The results are expressed as percentages of control values (means ± SEM, n = 3). *p < 0.05, **p < 0.01 and ***p < 0.001
Effect of hnRNP F and hnRNP K on CREB-mediated Agt expression in rat RPTCs in vitro
Transfection of rat RPTCs with either pRSV-Hnrnpf or pRSV-Hnrnpk attenuated the stimulatory effect of pRSV-Creb on Agt promoter activity (Fig. 7a), Agt mRNA (Fig. 7b) and AGT protein level (Fig. 7c). A combination of pRSV-Hnrnpf and pRSV-Hnrnpk appeared to be more effective in inhibiting pRSV-Creb-stimulation of Agt gene promoter activity, Agt mRNA expression and AGT protein levels than either pRSV-Hnrnpf or pRSV-Hnrnpk alone.
Effect of Hnrnpf, Hnrnpk and Creb on Agt promoter activity, Agt mRNA expression and AGT protein levels in RPTCs. Forty-eight hours after co-transfection of pRSV or pRSV-Creb with or without pRSV-Hnrnpf or pRSV-Hnrnpk into cells stably transfected with pGL4-Agt N-1495/+18 or RPTCs cultured in 5 mmol/l d-glucose medium, the cells were harvested and assayed for luciferase activity (a) or Agt mRNA (b) or AGT protein (c) levels. Relative luciferase activity or Agt mRNA or AGT protein levels in cells transfected with 4.0 μg of pRSV was considered as 100% (control). Each point represents the mean ± SEM (n = 3; assayed in duplicate). *p < 0.05, **p < 0.01 and ***p < 0.001, comparing indicated values
Discussion
This report identifies a novel mechanism underlying insulin inhibition of renal Agt expression and subsequent prevention of hypertension and kidney injury in Akita mice via upregulation of renal expression of hnRNP F and hnRNP K. Our observations suggest that cellular levels of hnRNP F and hnRNP K might play a critical role in regulating Agt expression and RAS activation in vivo.
We reported previously that overexpression of Hnrnpf prevents systemic hypertension and inhibits renal Agt expression and RPTC hypertrophy in diabetic Akita Hnrnpf-Tg mice [23]. However, the molecular regulation of Hnrnpf expression has not been explored. Extending our previous observations, here we provide in vivo and in vitro evidence that insulin stimulates hnRNP F and hnRNP K expression, which is critical for inhibition of renal Agt expression and the antihypertensive and renoprotective actions in Akita mice.
A major limitation of the present study is that our experimental design cannot differentiate between a ‘glucose-lowering effect’ and a ‘direct effect’ of insulin on renal Agt, Hnrnpf and Hnrnpk expression in vivo. Future studies are needed to address this issue.
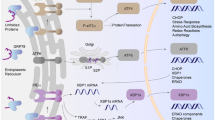
HnRNP F and hnRNP K are members of the pre-mRNA-binding protein family [30] and they regulate gene expression at both the transcriptional and post-transcriptional levels. Indeed, it has been noted that hnRNP F and hnRNP K engage in alternative splicing of various genes [31–34] and associate with TATA-binding protein (TBP), RNA polymerase II (Poly II), nuclear cap-binding protein complex and various transcriptional factors [35–37]. The molecular mechanisms underlying the regulation of gene transcription by hnRNP F and hnRNP K are still incompletely understood.
The Akita mouse is an autosomal dominant model of spontaneous type 1 diabetes in which Ins2 is mutated [38]. Like patients with type 1 diabetes, Akita mice develop hyperglycaemia and systemic hypertension, leading to cardiac hypertrophy and left ventricular diastolic dysfunction, as well as glomerulosclerosis and enhanced oxidative stress in RPTs [17, 23, 39–43].
A novel observation in our study is that, in addition to lowering blood glucose level, insulin treatment also prevents systemic hypertension, attenuates increases in KW/BW and HW/BW ratios and normalises the GFR, ACR, pro-fibrotic gene expression and tubulointerstitial fibrosis in Akita mice. It appears that insulin lowering of SBP is mediated, at least in part, via inhibition of intrarenal Agt expression and RAS activation. This notion is supported by our previous findings that Agt-Tg mice and Akita Agt-Tg mice specifically overexpressing AGT in their RPTCs develop hypertension, renal hypertrophy and tubulointerstitial fibrosis and that RAS blockade reverses these pathologies [13, 17]. These observations imply that intrarenal Agt expression and RAS activation play critical role(s) in the development of hypertension and renal and heart injury.
We did not detect significant differences in liver AGT, serum AGT and serum ANG II levels among the three different groups of mice studied. In contrast, RPT Agt mRNA and AGT protein levels, and urinary AGT and ANG II levels were significantly higher in Akita mice than in WT controls. Insulin treatment normalised RPT Agt mRNA and AGT protein expression and urinary AGT and ANG II levels. It is worth noting that urinary AGT levels in insulin-treated Akita mice appeared to be slightly higher than in WT controls without reaching statistical significance. These observations point to tissue-specific regulation of hepatic and renal Agt expression and indicate that urinary AGT is derived predominantly from RPTCs and to a lesser degree from extrarenal source(s) in diabetic mice. Indeed, recent studies [44–46] have shown that AGT filtered through the glomerulus in non-diabetic animals constitutes only a small portion of AGT detected in the urine.
We also detected significantly lower renal ACE-2 expression in the RPTCs of Akita mice, and this was normalised with insulin treatment. Consistent with these observations, our ex vivo studies employing freshly isolated RPTs from non-Akita and Akita mice showed insulin stimulation of Ace2 mRNA expression in normal-glucose and high-glucose conditions. These data imply a novel role for insulin in upregulation of intrarenal ACE-2 expression in preventing hypertension and renal injury in diabetes.
Our studies with pharmacological inhibitors indicate that the action of insulin on Agt, Hnrnpf and Hnrnpk transcription is mediated via the p44/42 MAPK signalling pathway, confirming our earlier report [18]. Insulin has previously been reported to stimulate hnRNP K phosphorylation via p44/42 MAPK signalling and to enhance its cytoplasmic translocation [47, 48]. Consistently, we also observed increased cytoplasmic and nuclear hnRNP F and hnRNP K in RPTCs of Akita mice treated with insulin as well as in RPTCs treated by insulin in vitro (ESM Fig. 3).
We have also shown that knock-down of hnRNP F and hnRNP K by their respective siRNAs prevented insulin inhibition of Agt transcription in RPTCs in high-glucose medium. These findings clearly indicate involvement of hnRNP F and hnRNP K in mediating insulin inhibition of Agt expression in the diabetic mouse kidney. Nevertheless, additional studies employing RPTC-specific hnRNP F and hnRNP K knockout mice are needed to firmly establish this pathway.
The molecular mechanisms by which hnRNP F and hnRNP K inhibit Agt expression remain to be investigated. Overexpression of CREB augmented Agt transcription [25] and high glucose enhanced CREB expression in RPTCs [49]. We found that overexpression of hnRNP F and/or hnRNP K attenuated the stimulatory effect of CREB on Agt transcription. These data imply that the beneficial actions of hnRNP F and hnRNP K are mediated, at least in part, via competition with CREB for binding to TBP and RNA Poly II, subsequently attenuating Agt transcription. Additional studies are needed to confirm this mechanism.
In summary, our data demonstrate that hnRNP F and hnRNP K mediate insulin inhibition of renal Agt expression, prevention of hypertension and amelioration of kidney and cardiac hypertrophy in mouse models of type 1 diabetes. These observations imply that dysregulation of hnRNP F and hnRNP K expression in vivo may directly alter activation of intrarenal RAS and, therefore, contribute to hypertension and renal injury in diabetes. Thus, hnRNP F and hnRNP K may be potential targets in the treatment of hypertension and kidney injury in diabetes.
Abbreviations
- ACE:
-
Angiotensin-converting enzyme
- ACE-2:
-
Angiotensin-converting enzyme-2
- ACR:
-
Albumin–creatinine ratio
- AGT:
-
Angiotensinogen
- ANG II:
-
Angiotensin II
- BW:
-
Body weight
- CREB:
-
cAMP-responsive element binding protein
- hnRNP F:
-
Heterogeneous nuclear ribonucleoprotein F
- hnRNP K:
-
Heterogeneous nuclear ribonucleoprotein K
- HW:
-
Heart weight
- KW:
-
Kidney weight
- MAPK:
-
Mitogen-activated protein kinase
- PAS:
-
Periodic acid Schiff
- Poly II:
-
Polymerase II
- RAS:
-
Renin–angiotensin system
- RPTs:
-
Renal proximal tubules
- RPTCs:
-
Renal proximal tubular cells
- RT-qPCR:
-
Real time-quantitative polymerase chain reaction
- SBP:
-
Systolic BP
- siRNA:
-
Small interfering RNA
- TBP:
-
TATA-binding protein
- Tg:
-
Transgenic
- TGF-β1:
-
Transforming growth factor-beta 1
- WT:
-
Wild type
References
The Diabetes Control and Complications Trial Research Group (1993) The effect of intensive treatment of diabetes on the development and progression of long term complications in insulin-dependent diabetic mellitus. N Engl J Med 329:977–986
Reichard P, Nilsson BY, Rosenqvist U (1993) The effect of long-term intensified insulin treatment on the development of microvascular complications of diabetes mellitus. New Engl J Med 329:304–309
de Boer IH, Kestenbaum B, Rue TC et al (2008) Insulin therapy, hyperglycemia, and hypertension in type 1 diabetes mellitus. Arch Intern Med 168:1867–1873
Dzau VJ, Ingelfinger JR (1989) Molecular biology and pathophysiology of the intrarenal renin-angiotensin system. J Hypertens Suppl 7:S3–S8
Wolf G, Neilson EG (1993) Angiotensin II as a hypertrophogenic cytokine for proximal tubular cells. Kidney Int Suppl 39:S100–S107
Tang SS, Jung F, Diamant D et al (1995) Temperature-sensitive SV40 immortalized rat proximal tubule cell line has functional renin-angiotensin system. Am J Physiol Renal Physiol 268:F435–F446
Loghman-Adham M, Rohrwasser A, Helin C et al (1997) A conditionally immortalized cell line from murine proximal tubule. Kidney Int 52:229–239
Anderson S, Jung FF, Ingelfinger JR (1993) Renal renin-angiotensin system in diabetes: functional, immunohistochemical, and molecular biological correlations. Am J Physiol 265:F477–F486
Lai KN, Leung JC, Lai KB, To WY, Yeung VT, Lai FM (1998) Gene expression of the renin-angiotensin system in human kidney. J Hypertens 16:91–102
Saito T, Urushihara M, Kotani Y, Kagami S, Kobori H (2009) Increased urinary angiotensinogen is precedent to increased urinary albumin in patients with type 1 diabetes. Am J Med Sci 338:478–480
Kobori H, Urushihara M, Xu JH, Berenson GS, Navar LG (2010) Urinary angiotensinogen is correlated with blood pressure in men (Bogalusa Heart Study). J Hypertens 28:1422–1428
Sawaguchi M, Araki SI, Kobori H et al (2012) Association between urinary angiotensinogen levels and renal and cardiovascular prognoses in patients with type 2 diabetes mellitus. J Diabetes Invest 3:318–324
Sachetelli S, Liu F, Zhang SL et al (2006) RAS blockade decreases blood pressure and proteinuria in transgenic mice overexpressing rat angiotensinogen gene in the kidney. Kidney Int 69:1016–1023
Godin N, Liu F, Lau GJ et al (2010) Catalase overexpression prevents hypertension and tubular apoptosis in angiotensinogen transgenic mice. Kidney Int 77:1086–1097
Ying J, Stuart D, Hillas E et al (2012) Overexpression of mouse angiotensinogen in renal proximal tubule causes salt-sensitive hypertension in mice. Am J Hypertens 25:684–689
Liu F, Brezniceanu ML, Wei CC et al (2008) Overexpression of angiotensinogen increases tubular apoptosis in diabetes. J Am Soc Nephrol 19:269–280
Lo CS, Liu F, Shi Y et al (2012) Dual RAS blockade normalizes angiotensin-converting enzyme-2 expression and prevents hypertension and tubular apoptosis in Akita angiotensinogen-transgenic mice. Am J Physiol Renal Physiol 302:F840–F852
Zhang SL, Chen X, Filep JG, Tang SS, Ingelfinger JR, Chan JS (1999) Insulin inhibits angiotensinogen gene expression via the mitogen-activated protein kinase pathway in rat kidney proximal tubular cells. Endocrinology 140:5285–5292
Zhang SL, Chen X, Wei CC et al (2002) Insulin inhibits dexamethasone effect on angiotensinogen gene expression and induction of hypertrophy in rat kidney proximal tubular cells in high glucose. Endocrinology 143:4627–4635
Chen X, Zhang SL, Pang L et al (2001) Characterization of a putative insulin-responsive element and its binding protein(s) in rat angiotensinogen gene promoter: regulation by glucose and insulin. Endocrinology 142:2577–2585
Wei CC, Guo DF, Zhang SL, Ingelfinger JR, Chan JS (2005) Heterogenous nuclear ribonucleoprotein F modulates angiotensinogen gene expression in rat kidney proximal tubular cells. J Am Soc Nephrol 16:616–628
Wei CC, Zhang SL, Chen YW et al (2006) Heterogeneous nuclear ribonucleoprotein K modulates angiotensinogen gene expression in kidney cells. J Biol Chem 281:25344–25355
Lo CS, Chang SY, Chenier I et al (2012) Heterogeneous nuclear ribonucleoprotein f suppresses angiotensinogen gene expression and attenuates hypertension and kidney injury in diabetic mice. Diabetes 61:2597–2608
Chan JS, Chan AH, Jiang Q, Nie ZR, LaChance S, Carriere S (1990) Molecular cloning and expression of the rat angiotensinogen gene. Pediatr Nephrol 4:429–435
Qian J-F, Wang T-T, Wu X-H et al (1997) Angiotensinogen gene expression is stimulated by the cAMP-responsive element binding protein in opposum kidney cells. J Am Soc Nephrol 8:1072–1079
Wang L, Lei C, Zhang SL et al (1998) Synergistic effect of dexamethasone and isoproterenol on the expression of angiotensinogen in immortalized rat proximal tubular cells. Kidney Int 53:287–295
Qi Z, Fujita H, Jin J et al (2005) Characterization of susceptibility of inbred mouse strains to diabetic nephropathy. Diabetes 54:2628–2637
Chang SY, Chen YW, Chenier I, Tran Sle M, Zhang SL (2011) Angiotensin II type II receptor deficiency accelerates the development of nephropathy in type I diabetes via oxidative stress and ACE2. Exp Diabetes Res 2011:521076
Zhang SL, To C, Chen X et al (2002) Essential role(s) of the intrarenal renin-angiotensin system in transforming growth factor-beta1 gene expression and induction of hypertrophy of rat kidney proximal tubular cells in high glucose. J Am Soc Nephrol 13:302–312
Han SP, Tang YH, Smith R (2010) Functional diversity of the hnRNPs: past, present and perspectives. Biochem J 430:379–392
Decorsiere A, Cayrel A, Vagner S, Millevoi S (2011) Essential role for the interaction between hnRNP H/F and a G quadruplex in maintaining p53 pre-mRNA 3'-end processing and function during DNA damage. Genes Dev 25:220–225
Talukdar I, Sen S, Urbano R, Thompson J, Yates JR 3rd, Webster NJ (2011) hnRNP A1 and hnRNP F modulate the alternative splicing of exon 11 of the insulin receptor gene. PLoS One 6:e27869
Stains JP, Lecanda F, Towler DA, Civitelli R (2005) Heterogeneous nuclear ribonucleoprotein K represses transcription from a cytosine/thymidine-rich element in the osteocalcin promoter. Biochem J 385:613–623
Revil T, Pelletier J, Toutant J, Cloutier A, Chabot B (2009) Heterogeneous nuclear ribonucleoprotein K represses the production of pro-apoptotic Bcl-xS splice isoform. J Biol Chem 284:21458–21467
Yoshida T, Makino Y, Tamura T (1999) Association of the rat heterogeneous nuclear RNA-ribonucleoprotein F with TATA-binding protein. FEBS Lett 457:251–254
Gamberi C, Izaurralde E, Beisel C, Mattaj IW (1997) Interaction between the human nuclear cap-binding protein complex and hnRNP F. Mol Cell Biol 17:2587–2597
Shnyreva M, Schullery DS, Suzuki H, Higaki Y, Bomsztyk K (2000) Interaction of two multifunctional proteins. Heterogeneous nuclear ribonucleoprotein K and Y-box-binding protein. J Biol Chem 275:15498–15503
Wang J, Takeuchi T, Tanaka S et al (1999) A mutation in the insulin 2 gene induces diabetes with severe pancreatic beta-cell dysfunction in the Mody mouse. J Clin Invest 103:27–37
Yoshioka M, Kayo T, Ikeda T, Koizumi A (1997) A novel locus, Mody4, distal to D7Mit189 on chromosome 7 determines early-onset NIDDM in nonobese C57BL/6 (Akita) mutant mice. Diabetes 46:887–894
Haseyama T, Fujita T, Hirasawa F et al (2002) Complications of IgA nephropathy in a non-insulin-dependent diabetes model, the Akita mouse. Tohoku J Exp Med 198:233–244
Hong EG, Jung DY, Ko HJ et al (2007) Nonobese, insulin-deficient Ins2Akita mice develop type 2 diabetes phenotypes including insulin resistance and cardiac remodeling. Am J Physiol Endocrinol Metab 293:E1687–E1696
Oudit GY, Liu GC, Zhong J et al (2010) Human recombinant ACE2 reduces the progression of diabetic nephropathy. Diabetes 59:529–538
Chang JH, Paik SY, Mao L et al (2012) Diabetic kidney disease in FVB/NJ Akita mice: temporal pattern of kidney injury and urinary nephrin excretion. PLoS One 7:e33942
Pohl M, Kaminski H, Castrop H et al (2010) Intrarenal renin angiotensin system revisited: role of megalin-dependent endocytosis along the proximal nephron. J Biol Chem 285:41935–41946
Matsusaka T, Niimura F, Shimizu A et al (2012) Liver angiotensinogen is the primary source of renal angiotensin II. J Am Soc Nephrol 23:1181–1189
Nakano D, Kobori H, Burford JL et al (2012) Multiphoton imaging of the glomerular permeability of angiotensinogen. J Am Soc Nephrol 23:1847–1856
Habelhah H, Shah K, Huang L et al (2001) ERK phosphorylation drives cytoplasmic accumulation of hnRNP-K and inhibition of mRNA translation. Nat Cell Biol 3:325–330
Ostrowski J, Kawata Y, Schullery DS et al (2001) Insulin alters heterogeneous nuclear ribonucleoprotein K protein binding to DNA and RNA. Proc Natl Acad Sci USA 98:9044–9049
Hsieh TJ, Fustier P, Zhang SL et al (2003) High glucose stimulates angiotensinogen gene expression and cell hypertrophy via activation of the hexosamine biosynthesis pathway in rat kidney proximal tubular cells. Endocrinology 144:4338–4349
Acknowledgements
This manuscript or any significant part of it is not under consideration for publication elsewhere. The data, however, were presented, in part, as a poster communication at the 44th Annual Meeting of the American Society of Nephrology, San Diego, CA, USA, October 30–November 4, 2012.
Funding
The study was supported by grants from the Canadian Institutes of Health Research (CIHR, MOP-93650, MOP-84363 and MOP-16088 to J. S. D. Chan; MOP-86450 to S.-L. Zhang; and MOP-64283 to J. G. Filep), the Heart and Stroke Foundation of Quebec (HSFQ to J. S. D. Chan), and the National Institutes of Health (HL-48455 to J. R. Ingelfinger). Editorial assistance was provided by the CRCHUM Research Support Office.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Contribution statement
JSDC is the guarantor of this work, had full access to all study data and takes responsibility for data integrity and the accuracy of data analysis. JSDC is the principal investigator and was responsible for the study conception and design. JSDC drafted the manuscript and reviewed/edited manuscript. SA, CSL, IC, AS and SLZ contributed to the in vivo and ex vivo experiments and collection of data. JGF and JRI contributed to the discussion and reviewed/edited the manuscript. All authors were involved in analysis and interpretation of data and contributed to the critical revision of the manuscript. All authors provided final approval of the version to be published.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM Fig. 1
(PDF 250 kb)
ESM Fig. 2
(PDF 193 kb)
ESM Fig. 3
(PDF 223 kb)
Rights and permissions
About this article
Cite this article
Abdo, S., Lo, CS., Chenier, I. et al. Heterogeneous nuclear ribonucleoproteins F and K mediate insulin inhibition of renal angiotensinogen gene expression and prevention of hypertension and kidney injury in diabetic mice. Diabetologia 56, 1649–1660 (2013). https://doi.org/10.1007/s00125-013-2910-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-013-2910-4