Abstract
Aims/hypothesis
Rosiglitazone and metformin are two oral antihyperglycaemic drugs used to treat type 2 diabetes. While both drugs have been shown to improve insulin-sensitive glucose uptake, the direct effects of these drugs on pancreatic beta cells is only now beginning to be clarified. The aim of the present study was to determine the direct effects of these agents on beta cell gene expression.
Methods
We used reporter gene analysis to examine the effects of rosiglitazone and metformin on the activity of the proinsulin and insulin promoter factor 1 (IPF1) gene promoters in the glucose-responsive mouse beta cell line Min6. Western blot and gel retardation analyses were used to examine the effects of both drugs on the regulation of IPF1 protein production, nuclear accumulation and DNA binding activity in both Min6 cells and isolated rat islets of Langerhans.
Results
Over 24 h, rosiglitazone promoted the nuclear accumulation of IPF1 and forkhead homeobox A2 (FOXA2), independently of glucose concentration, and stimulated a two-fold increase in the activity of the Ipf1 gene promoter (p<0.01). Stimulation of the Ipf1 promoter by rosiglitazone was unaffected by the presence of the peroxisome proliferator activated receptor γ antagonist GW9662. No effect of either rosiglitazone or metformin was observed on proinsulin promoter activity. Metformin stimulated IPF1 nuclear accumulation and DNA binding activity in a time-dependent manner, with maximal effects observed after 2 h.
Conclusions/interpretation
Metformin and rosiglitazone have direct effects on beta cell gene expression, suggesting that these agents may play a previously unrecognised role in the direct regulation of pancreatic beta cell function.
Similar content being viewed by others
Introduction
Rosiglitazone and metformin are oral antihyperglycaemic drugs used in the management of type 2 diabetes. Rosiglitazone is a member of the thiazolidinedione class of drugs and acts largely through agonist action on the nuclear receptor peroxisome proliferator-activated receptor γ (PPARγ) [1], through which it has been shown to increase insulin-dependent peripheral glucose disposal, decrease hepatic glucose output and alter adipocyte metabolism [2]. Metformin is of the biguanide class of drugs, and also largely targets tissues of glucose storage and metabolism, predominantly the liver [3].
While both drugs improve insulin-sensitive glucose uptake [4, 5], their direct effects on pancreatic beta cells has not been fully clarified. Metformin has been shown to restore insulin secretion following chronic exposure of rat islets to non-esterified fatty acids or high glucose [6], an effect mediated through direct effects on beta cell glucose and fatty acid metabolism. The effects of metformin on glucose-induced insulin secretion have been linked to the activation of AMP-dependent protein kinase (AMPK) [7, 8]. Although not analysed in beta cells to date, in muscle cells rosiglitazone has also been shown to activate AMPK [9]. The pathways involved in the activation of AMPK by metformin and rosiglitazone in muscle cells are reportedly distinct [9]. The aim of the present study was to investigate the direct effects of rosiglitazone and metformin on pancreatic beta cell gene expression and the activity of the key beta cell regulatory transcription factors insulin promoter factor (IPF1) and forkhead homeobox A2 (FOXA2).
Regulation of the proinsulin gene in response to glucose is dependent in part on the activity of the beta cell transcription factor IPF1 (also known as pancreatic duodenal homeobox 1 [PDX1]) [10], which is central to the regulation of a complement of beta cell glucose-sensing genes [11, 12]. IPF1 accumulates in the beta cell nucleus in response to elevated glucose concentrations, events mediated by post-translational modification of the protein [13–15]. Expression of the Ipf1 gene is also regulated in response to glucose [16]. The complex 4.5 kb Ipf1 gene promoter contains binding sites for many beta cell transcription factors, including hepatocyte nuclear factor 1α (HNF1α), IPF1 and FOXA2 [17–20]. FOXA2 is a member of the forkhead/winged helix family and has been identified as a key regulator of Ipf1 gene expression. FOXA2 is produced at the onset of pancreatic development in the foregut endoderm. Its expression pattern is similar to that of IPF1, and it has been shown to bind key regulatory elements within the Ipf1 gene promoter, regulating expression both during pancreas development and in adult islets [19, 20]. Although the key role of FOXA2 in regulating Ipf1 gene expression is becoming clear, at present little is known about the stimuli regulating FOXA2 production itself in adult beta cells.
In the present study, we used the glucose-responsive beta cell line Min6 and a series of reporter gene constructs containing sections of the proinsulin and Ipf1 gene promoters to analyse the direct effects of rosiglitazone and metformin on the regulation of these key beta cell genes. We also used Western blotting and electrophoretic mobility shift assay (EMSA) analysis to evaluate the production, nuclear accumulation and DNA binding activity of the key beta cell transcription factors IPF1, FOXA2 and HNF1α. Our data indicate that the established effects of rosiglitazone and metformin on beta cell functional activity may occur in part through direct effects on beta cell transcriptional regulation.
Materials and methods
Materials
Cell culture materials, LipofectAMINE and OptiMem were purchased from Invitrogen (Paisley, UK). Rosiglitazone (purity >99.5%) was provided by GlaxoSmithKline (Harlow, UK). Metformin (purity >98%) was purchased from Sigma-Aldrich (Dorset, UK). Luciferin was from Perbio (Newcastle, UK). Protein assay reagent was from Bio-Rad (Hemel Hempstead, UK). All other chemicals and materials were purchased from Sigma-Aldrich.
Plasmids
The construct pGL-Luc200 is derived from the pGL2 vector (Promega, Southampton, UK) and contains 200 bp of the human proinsulin gene promoter upstream of the firefly luciferase reporter gene, as previously described [13]. The control construct Luc lacks the proinsulin gene promoter fragment. The construct pGL-IPF1 is based on the pGL3 vector (Promega) and contains a 4,531 bp fragment of the mouse Ipf1 promoter upstream of the firefly luciferase reporter gene, as previously described [16]. Plasmid DNA was prepared using an endotoxin-free Maxiprep kit (Qiagen, Crawley, UK).
Cell culture
Min6 cells, a beta cell line derived from transgenic mice expressing the SV40 large T antigen under the control of the rat proinsulin gene promoter [21], were cultured in DMEM containing 5 mmol/l glucose, supplemented with 15% heat-inactivated fetal calf serum, 100 U/ml penicillin, 100 mg/ml streptomycin and 50 μmol/l β-mercaptoethanol. All of the present studies were performed using cells between passage numbers 28 and 32.
Transfection studies
Cells at 80% confluence were transfected using LipofectAMINE (Invitrogen) as previously described [16]. Forty-eight hours after transfection (including preincubation for 12 h in 0.5 mmol/l glucose prior to stimulation) the cells were incubated with either 10 μmol/l rosiglitazone (2 μl of 1,000× stock in DMSO added to each 2 ml well) or 15 μmol/l metformin (2 μl of 1,000× stock in the same media added to each 2 ml well) for the indicated time periods. Cells were harvested and lysates prepared as previously described [16]. Luciferase reporter gene assays were performed and luciferase activity was normalised to protein content as previously described [16].
Islet isolation
Islets were isolated from male Wistar rats, weighing 250–300 g, as previously described [22], aliquoted into batches of 150 in RPMI containing 5 mmol/l glucose, supplemented with 10% fetal calf serum, and maintained in a humidified 37°C incubator with 5% CO2.
Western blotting
Whole cell or nuclear extracts were prepared, and fractionated by SDS-PAGE. Western blotting was carried out as previously described [23]. Protein concentrations were measured using Bio-Rad Protein Assay Kit reagent, titrated against known concentrations of bovine serum albumin. Whole-cell extract (10 μg) or 5 μg of nuclear extract was added per well. Equal loading of protein to each well was additionally confirmed by blotting with a specific HNF1α antibody. Levels of HNF1α remained constant under all experimental conditions tested (not shown). The IPF1 antibody was a kind gift from C. V. Wright (Vanderbilt University, Nashville, TN, USA). FOXA2 and HNF1α antibodies were purchased from Santa Cruz (Calne, UK). Secondary horseradish peroxidase (HRP)-conjugated antibodies were purchased from Amersham (UK).
Electrophoretic mobility shift assays
EMSA analysis was performed using the DIG Gel Shift Kit (Roche Molecular Biochemicals, Mannheim, Germany) using Probe B, containing the A3 site of the human proinsulin gene promoter [13]. Five micrograms of each nuclear extract, 0.4 ng of digoxigenin-labelled probe, 1× binding buffer, 1 μg (poly-deoxy-inosinic-deoxy-cytidylic acid) and 0.1 μg poly-l-lysine were incubated at room temperature for 20 min, fractionated on 6% polyacrylamide gels, and blotted onto nylon membrane, blocked for 30 min. Chemiluminescent detection reaction was carried out all according to the manufacturer’s protocol.
Statistics and densitometry
The data are expressed as mean±SD. Data were compared using two-tailed Student’s t-test for paired data. Densitometry was performed using the Tina v2.09 g software (Raytest, Straubenhardt, Germany). A p value of less than 0.05 was considered significant.
Results
Rosiglitazone stimulates Ipf1 gene promoter activity in a concentration-dependent manner
To analyse the effects of rosiglitazone on Ipf1 gene promoter activity, Min6 cells were transfected with the construct pGL-IPF1, which contains the full-length mouse Ipf1 gene promoter upstream of the firefly luciferase reporter gene, or with the control construct pGL3, which lacks the promoter fragment. Forty-eight hours after transfection, cells were stimulated for 24 h with 5 mmol/l glucose alone (containing DMSO as a control for rosiglitazone/DMSO addition) or with 5 mmol/l glucose containing 0.1, 1.0, 10 or 100 μmol/l rosiglitazone, respectively (Fig. 1). Incubation in 5 mmol/l glucose resulted in a two-fold increase in Ipf1 promoter activity compared with that observed in 0.5 mmol/l glucose, consistent with previous studies [16]. Addition of 1–100 μmol/l rosiglitazone produced a further concentration-dependent increase in the activity of the Ipf1 gene promoter, which was maximal at 10 μmol/l rosiglitazone. No effect of glucose or rosiglitazone was observed on the expression of control construct pGL3 (data not shown). A comparable concentration-dependent increase in Ipf1 promoter activity was observed when the same experiment was performed at 25 mmol/l glucose (not shown). These results are the first to indicate that rosiglitazone directly stimulates the activity of the Ipf1 gene promoter in pancreatic beta cells.
Rosiglitazone increases Ipf1 gene promoter activity in a concentration-dependent manner. Min6 cells were transfected with the construct pGL-IPF1, which contains the full-length mouse Ipf1 gene promoter upstream of the firefly luciferase reporter gene, or with the control construct pGL3, which lacks the promoter fragment. Thirty-six hours after transfection, cells were preincubated in 0.5 mmol/l glucose for 12 h, and were then maintained in 0.5 mmol/l glucose (white bar) and stimulated with 5 mmol/l glucose alone (black bars) (containing DMSO as a control for rosiglitazone/DMSO addition) or with 5 mmol/l glucose containing 0.1, 1.0, 10 or 100 μmol/l rosiglitazone, respectively. Cells were harvested 24 h after addition of rosiglitazone, lysed, and extracts assayed for luciferase reporter gene activity. Luciferase values were standardised against protein concentration. n=3 for each value; error bars represent the SD. These results were reproduced in at least three separate experiments. **p<0.01 compared with 5 mmol/l glucose alone
Metformin has no effect on the activity of either the Ipf1 or the proinsulin gene promoter in Min6 beta cells
To compare the effects of rosiglitazone and metformin on Ipf1 promoter activity, Min6 cells were transfected with the constructs pGL-IPF1 and pGL3 as above. Forty-eight hours after transfection, cells were incubated for 24 h with 5 mmol/l glucose, or with 5 mmol/l glucose containing DMSO, 15 μmol/l metformin, 10 μmol/l rosiglitazone, or a combination of rosiglitazone and metformin as indicated (Fig. 2a). Metformin at 15 μmol/l has previously been shown to have direct effects on beta cell function [6]. As before, addition of rosiglitazone stimulated a two-fold increase in Ipf1 promoter activity compared with 5 mmol/l glucose alone. Addition of metformin had no effect on Ipf1 promoter activity. A combination of rosiglitazone and metformin resulted in no greater increase in Ipf1 promoter activity than was observed with rosiglitazone alone. No effect of either drug was observed on the control construct pGL3 (not shown).
Combined effect of rosiglitazone and metformin on the Ipf1 and proinsulin gene promoters. Min6 cells were transfected with: (a) the construct pGL-IPF1, which contains the full-length mouse Ipf1 gene promoter upstream of the firefly luciferase reporter gene, or with the control construct pGL3, which lacks the promoter fragment; or (b) with construct Luc200, containing a 200 bp section of the human proinsulin gene promoter upstream of the firefly luciferase gene, or the control construct Luc, which lacks the proinsulin gene promoter fragment. Thirty-six hours after transfection, cells were preincubated in 0.5 mmol/l glucose for 12 h, and were then maintained in 0.5 mmol/l glucose (white bars). They were stimulated with 5 mmol/l glucose alone (black bars); 5 mmol/l glucose containing DMSO; 5 mmol/l glucose containing 10 μmol/l rosiglitazone (ROSI); 5 mmol/l glucose containing 15 μmol/l metformin (MET); or 5 mmol/l glucose containing both 10 μmol/l rosiglitazone and 15 μmol/l metformin (ROSI+MET). Twenty-four hours after these additions, cells were harvested and luciferase reporter gene activity was measured. Luciferase values were standardised against protein concentration. n=3 for each value; error bars represent the SD. These results were reproduced in at least three separate experiments. *p<0.05 compared with 5 mmol/l glucose alone
To investigate the effects of rosiglitazone and metformin on proinsulin promoter activity, the same experiment was performed using the construct Luc200, containing a 200 bp section of the human proinsulin gene promoter upstream of the firefly luciferase gene, or the control construct Luc, which lacks the proinsulin gene promoter fragment (Fig. 2b). Incubation in 5 mmol/l glucose resulted in a two-fold increase in Luc200 activity compared with that observed in 0.5 mmol/l glucose. However, no effect of rosiglitazone or metformin was observed on Luc200 activity, or on the activity of the control construct Luc (not shown).
Rosiglitazone stimulation of the Ipf1 promoter is unaffected by the presence of GW9662
To investigate the potential role of PPARγ in the observed effects of rosiglitazone on Ipf1 promoter activity, Min6 cells were transfected with the constructs pGL-IPF1 and pGL3 as above. Forty-eight hours after transfection, cells were preincubated for 30 min in the presence of 30 μmol/l GW9662, followed by incubation for 24 h with 5 mmol/l glucose, or with 5 mmol/l glucose containing 10 μmol/l rosiglitazone (Fig. 3). As before, the addition of rosiglitazone resulted in a two-fold increase in Ipf1 promoter activity compared with 5 mmol/l glucose alone. The observed effects of rosiglitazone were unaffected by the addition of GW9662.
GW9662 does not affect rosiglitazone stimulation of the Ipf1 gene promoter. Min6 cells were transfected with the construct pGL-IPF1, which contains the full-length mouse Ipf1 gene promoter upstream of the firefly luciferase reporter gene, or with the control construct pGL3, which lacks the promoter fragment. Forty-eight hours after transfection, cells were maintained in 5 mmol/l glucose (white bar) or stimulated with 10 μmol/l rosiglitazone alone (ROSI) or with rosiglitazone in the presence of 30 μmol/l GW9662 (ROSI+GW) (black bars). GW9662 was added 30 min before rosiglitazone addition. Cells were harvested 24 h after addition of rosiglitazone, and lysed; extracts were assayed for luciferase reporter gene activity. Luciferase values were standardised against protein concentration. n=3 for each value; error bars represent the SD. These results were reproduced in at least three separate experiments
Metformin and rosiglitazone both stimulate IPF1 protein levels at 5 and 25 mmol/l glucose
To determine the effects of rosiglitazone and metformin on the levels of the IPF1 protein, Min6 cells were stimulated with 15 μmol/l metformin or 10 μmol/l rosiglitazone in the presence of 0.5, 5 or 25 mmol/l glucose for 24 h. Whole-cell extracts were then analysed by Western blotting using a specific IPF1 antibody. Metformin stimulated a significant increase in IPF1 protein levels at all glucose concentrations tested (Fig. 4a) (12% at 0.5 mmol/l glucose, 20% at 5 mmol/l glucose and 17% at 25 mmol/l glucose). The percentage values given are based on densitometric analysis of blots from three separate experiments. All increases were statistically significant (p<0.05). In 0.5 mmol/l glucose, the addition of rosiglitazone had no detectable effect on the levels of the IPF1 protein (Fig. 4b). In contrast, however, the addition of rosiglitazone in the presence of 5 or 25 mmol/l glucose resulted in a marked increase (25%) in the levels of the IPF1 protein. These results indicate that rosiglitazone stimulation of IPF1 protein levels occurs only in the presence of 5 or 25 mmol/l glucose, with no effect at a minimal (0.5 mmol/l) glucose concentration. At both 5 and 25 mmol/l glucose concentrations, the addition of metformin and rosiglitazone together produced no further increase in the IPF1 protein level over that observed with rosiglitazone alone (not shown). Similar results were observed using isolated rat islets of Langerhans (Fig. 5), where the combined effects of metformin and rosiglitazone on whole-cell IPF1 protein levels at 5 mmol/l glucose were no greater than the effects of metformin or rosiglitazone alone.
Western blot analysis of the effects of rosiglitazone and metformin on Min6 whole-cell IPF1 protein levels. Min6 cells were stimulated (black bars+sign) with (a) 15 μmol/l metformin or (b) 10 μmol/l rosiglitazone in 0.5 mmol/l glucose, 5 or 25 mmol/l glucose, as indicated. Twenty-four hours after addition of the drugs, cells were harvested, whole-cell extracts were prepared, and the levels of IPF1 protein were analysed by Western blotting using a specific IPF1 antibody and a horseradish peroxidase-conjugated secondary antibody. These results were reproduced in at least three separate experiments. Densitometric analysis of blots from three separate experiments was performed using the Tina v2.09g software, with values shown in the lower panels. *p<0.05 compared with unstimulated samples (white bars−sign) at the same glucose concentration
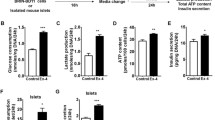
Western blot analysis of the effects of rosiglitazone and metformin on whole-cell IPF1 protein levels in isolated rat islets of Langerhans. Freshly isolated rat islets of Langerhans were separated into batches of 150 and incubated in 5 mmol/l glucose overnight. Batches were then incubated for 24 h in 5 mmol/l glucose; 5 mmol/l glucose containing DMSO; 5 mmol/l glucose containing 10 μmol/l rosiglitazone (ROSI); 5 mmol/l glucose containing 15 μmol/l metformin (MET); or 5 mmol/l glucose containing both 10 μmol/l rosiglitazone and 15 μmol/l metformin (ROSI+MET). Twenty-four hours after addition of the drugs, cells were harvested, whole-cell extracts were prepared and the levels of IPF1 protein were analysed by Western blotting using a specific IPF1 antibody and an horseradish peroxide-conjugated secondary antibody (a). These results were reproduced in at least three separate experiments. Densitometric analysis (b) of blots from three separate experiments was performed using the Tina v2.09g software; values are shown in. *p<0.05 compared with unstimulated samples (white bars)
Metformin promotes the nuclear accumulation of IPF1 and FOXA2 in a glucose-dependent manner over 24 h
To analyse the effects of metformin on nuclear abundance of IPF1 and FOXA2, Min6 cells were stimulated with 15 μmol/l metformin in the presence of 0.5, 5 or 25 mmol/l glucose for 24 h. Nuclear extracts were then subjected to Western blotting using the appropriate specific antibody. The addition of metformin had no effect on nuclear levels of IPF1 in 0.5 or 5 mmol/l glucose, but did induce a significant (30%) increase in nuclear IPF1 in 25 mmol/l glucose (Fig. 6a). At 25 mmol/l glucose, the addition of metformin also resulted in an increase in the nuclear level of FOXA2 (15%). No effect of metformin on FOXA2 nuclear accumulation was observed at 0.5 or 5 mmol/l glucose (Fig. 6b). These results indicate that metformin stimulates the nuclear accumulation of both IPF1 and FOXA2 over a 24-h period in the presence of 25 mmol/l glucose. No effect of metformin was observed on the nuclear levels of HNF1α at 0.5, 5 or 25 mmol/l glucose (data not shown).
Western blot analysis of the effects of metformin on nuclear IPF1 and FOXA2 protein levels at 24 h. Min6 cells were stimulated (+ sign) with 15 μmol/l metformin (black bars) in the presence of 0.5, 5 or 25 mmol/l glucose, as indicated. Twenty-four hours after addition of metformin, cells were harvested and nuclear extracts were then prepared; Western blotting was performed using specific antibodies for IPF1 (a) and FOXA2 (b), in combination with horseradish peroxide-conjugated secondary antibody. These results were reproduced in at least three separate experiments. Graphs represent densitometric analysis of blots from three separate experiments, performed using the Tina v2.09g software. *p<0.05 compared with unstimulated samples (white bars) at the same glucose concentration
Rosiglitazone promotes the nuclear accumulation of IPF1 and FOXA2 in a glucose-independent manner over 24 h
A similar analysis was performed to determine the effects of rosiglitazone on the nuclear accumulation of IPF1 and FOXA2. Min6 cells were stimulated with 10 μmol/l rosiglitazone in the presence of 0.5, 5 or 25 mmol/l glucose for 24 h. Nuclear extracts were then subjected to Western blotting using the appropriate specific antibody (Fig. 7). The effects of rosiglitazone on both transcription factors were marked at all glucose concentrations. The addition of rosiglitazone resulted in nuclear accumulation of IPF1 at 0.5 mmol/l glucose (16%), 5 mmol/l glucose (28%) and 25 mmol/l glucose (23%) (p<0.01). It also resulted in the stimulation of nuclear accumulation of FOXA2 (32% at 0.5 mmol/l glucose, 25% at 5 mmol/l glucose and 52% at 25 mmol/l glucose; p<0.05). No effect of rosiglitazone was observed on the nuclear levels of HNF1α at 0.5, 5 or 25 mmol/l glucose (not shown). These results indicate that rosiglitazone has profound effects on the nuclear accumulation of both IPF1 and FOXA2, over a 24-h incubation period, at all glucose concentrations tested.
Western blot analysis of the effects of rosiglitazone on nuclear IPF1 and FOXA2 protein levels at 24 h. Min6 cells were stimulated (+) with 10 μmol/l rosiglitazone (black bars) in the presence of 0.5, 5 or 25 mmol/l glucose as indicated. Twenty-four hours after addition of rosiglitazone, cells were harvested and nuclear extracts were then prepared; Western blotting was performed using specific antibodies for IPF1 (a) and FOXA2 (b), in combination with horseradish peroxide-conjugated secondary antibody. These results were reproduced in at least three separate experiments. Graphs represent densitometric analysis of blots from three separate experiments, performed using the Tina v2.09g software. **p<0.01, *p<0.05 compared with unstimulated samples (white bars) at the same glucose concentration
Metformin rapidly (2 h) stimulates IPF1 nuclear accumulation and DNA binding activity
Since post-translational modification and nuclear accumulation of IPF1 can occur rapidly in pancreatic beta cells, we next examined the nuclear accumulation and DNA binding activity of IPF1 over the shorter period of 2 h. Min6 cells were incubated in 5 mmol/l glucose containing 15 μmol/l metformin, 10 μmol/l rosiglitazone, or both metformin and rosiglitazone. Following a 2-h incubation period, nuclear extracts were prepared and EMSA analysis was performed using a probe containing a consensus IPF1 binding site (Fig. 8a). The addition of metformin resulted in a marked increase in IPF1 binding activity over the 2-h period. Addition of rosiglitazone had no effect on IPF1 binding activity. Adding metformin and rosiglitazone together resulted in stimulation of binding activity comparable with that produced by the addition of metformin alone. These data indicate that metformin rapidly stimulates an increase in IPF1 DNA binding activity in pancreatic beta cells, and that rosiglitazone has no effect over this shorter period. Probe specificity was confirmed by mutant oligonucleotide competition and antibody competition EMSA analysis (not shown) as in previous studies [13, 23]. Using the same nuclear extracts, Western blotting analysis was performed to determine the level of nuclear IPF1 (Fig. 8b). Consistent with the EMSA analysis, elevated levels of nuclear IPF1 were observed in cells stimulated with 15 μmol/l metformin and in cells stimulated with both metformin and rosiglitazone together. As with the EMSA analysis, the effect of rosiglitazone and metformin together was comparable to the stimulation observed with metformin alone. The results of these experiments indicate that metformin alone can promote the short-term (2 h) accumulation of IPF1 in the beta cell nucleus, and that this accumulation is associated with a marked increase in IPF1 DNA binding activity.
Metformin stimulates IPF1 nuclear accumulation and DNA binding activity over 2 h. Min6 cells were incubated in 5 mmol/l glucose containing: 15 μmol/l metformin (MET); 10 μmol/l rosiglitazone (ROSI); or both metformin and rosiglitazone (MET+ROSI) as indicated (black bars). Following a 2-h incubation period, cells were harvested and nuclear extracts prepared. (a) EMSA analysis of 5 μg of each nuclear extract using a 23-mer oligonucleotide probe containing a consensus IPF1 binding site. (b) Western blot analysis of 3 μg of the same extracts, using a specific IPF1 antibody in combination with an horseradish peroxidase-conjugated secondary antibody. These results were reproduced in at least three separate experiments. Graphs (a,b) represent densitometric analysis of corresponding blots from three separate experiments, performed using the TINA v2.09g software. *p<0.05 compared with the unstimulated control (white bars)
Since an increase in nuclear IPF1 levels and DNA binding activity was observed at 2 h but no effect on nuclear IPF1 levels was evident at 24 h (Fig. 6a), our last experiment analysed the time course of the effect of metformin addition on nuclear levels of IPF1 (Fig. 9). Min6 cells were incubated in 5 mmol/l glucose or in 5 mmol/l glucose containing 15 μmol/l metformin for 1, 2, 6, 9 or 24 h, nuclear extracts prepared, and IPF1 protein levels analysed by Western blotting using a specific IPF1 antibody. IPF1 nuclear accumulation occurred rapidly, with a significant increase in nuclear IPF1 after 1 and 2 h. However, at later time points nuclear levels of IPF1 declined, and by 24 h the levels of IPF1 had returned to those observed in 5 mmol/l glucose alone. These data indicate that the effect of metformin on nuclear IPF1 protein levels occurs rapidly in Min6 beta cells, but is not prolonged over a 24-h incubation period.
Time-course analysis of the effects of metformin on nuclear IPF1 protein levels. Min6 cells were incubated in 5 mmol/l glucose for 24 h. Following addition of 15 μmol/l metformin, samples were harvested at 0, 1, 2, 6, 9 and 24 h as indicated and nuclear extracts were then prepared; Western blotting (a) was performed using a specific IPF1 antibody. These results were reproduced in at least three separate experiments. Densitometric analysis (b) of blots from three separate experiments was performed using the Tina v2.09g software. *p<0.05 compared with the 0 h time point
Discussion
The results of the present study show that both metformin and rosiglitazone have marked effects on transcriptional regulation in the pancreatic beta cell line Min6 and in freshly isolated rat islets of Langerhans. Our initial concentration-response analysis indicates that rosiglitazone has maximal effects on the Ipf1 gene promoter over 24 h at a concentration of 10 μmol/l. In agreement with our previous studies, increased glucose concentrations (0.5–5 mmol/l) stimulated a marked increase in the activity of the Ipf1 promoter [16]. A further two-fold increase was observed upon addition of 10 μmol/l rosiglitazone, indicating that glucose and rosiglitazone have an additive effect on Ipf1 promoter activity. Comparable results were observed at 25 mmol/l glucose.
In the present study, rosiglitazone had no effect on the 200 bp section of the human proinsulin gene promoter analysed. This section of the promoter has been shown in previous studies to contain key regulatory elements essential for the control of proinsulin gene transcription [10, 13, 23]. Although our data do not exclude the possibility that further elements which may respond to rosiglitazone lie outside this region, our findings are consistent with previous studies which show 100 μmol/l rosiglitazone has no effect on proinsulin mRNA levels in INS1 cells over a 24-h period [24]. In contrast to the marked effects of rosiglitazone, metformin had no effect on the activity of either the Ipf1 or the proinsulin promoter over the same 24-h incubation period. The effects of rosiglitazone and metformin on Ipf1 promoter activity have not been reported previously. It is intriguing that metformin did not affect Ipf1 promoter activity, but did stimulate IPF1 protein levels over 24 h. This suggests that the observed effects of metformin on IPF1 production occur post-transcriptionally.
Since metformin and rosiglitazone are often prescribed in combination for the treatment of insulin-resistance in type 2 diabetes [25, 26], we tested the combined effect of these agents on our selected targets, both in Min6 cells and in freshly isolated rat islets. No additive effect of rosiglitazone and metformin was observed. Several recent studies indicate that these agents stimulate distinct intracellular signalling pathways [27, 28]. Recent studies in muscle cells indicate that although both agents are able to activate AMP kinase, even activation of the same target may occur through distinct signalling pathways [9]. These pathways remain to be fully elucidated; however, phosphatidylinositol 3-kinase, mitogen-activated protein kinase and p38 do not appear to be involved [9].
In the present study, rosiglitazone had a marked effect on the expression level and nuclear accumulation of the IPF1 protein. This is consistent with the observed effects on Ipf1 promoter activity. Nuclear accumulation of IPF1 was independent of glucose concentration and was evident at each of the 0.5, 5 and 25 mmol/l glucose conditions tested over 24 h. We and others have previously shown that stimuli such as glucose and glucagon-like peptide-1 (GLP-1) can promote the translocation of IPF1 from the cytoplasm to the nucleus in pancreatic beta cells [23, 29, 30]. Further studies have shown that nuclear export of IPF1 in response to oxidative stress is dependent on signalling events regulated through the activity of c-JNK [31]. Interestingly, thiazolidinediones have previously been shown to decrease oxidative stress [32] and to suppress c-fos/c-Jun [33]. Further investigation is required to determine the intracellular signalling events regulating the effects of rosiglitazone in the present study.
Although the effects of rosiglitazone on insulin target tissues have been largely attributed to selective activation of PPARγ, recent studies have begun to reveal that members of the thiazolidinedione family of drugs can also have marked effects on cell function through PPARγ-independent mechanisms [34, 35]. In the present study, addition of GW9662 had no effect on rosiglitazone stimulation of the Ipf1 gene promoter, indicating that these events are not dependent on the activity of PPARγ. This is consistent with bioinformatic analysis of the Ipf1 promoter sequence, which does not reveal the presence of any consensus PPARγ response elements. The transcription factor targets mediating the effects of rosiglitazone on the Ipf1 promoter remain to be delineated.
We have shown that rosiglitazone promotes elevated nuclear levels of FOXA2 over 24 h. FOXA2 is a known regulator of the Ipf1 gene promoter and plays a key role in Ipf1 gene expression both during pancreas development and in adult islets [19, 20]. Nuclear/cytosolic localisation of FOXA2 in hepatocytes is regulated through Akt-mediated phosphorylation events [36]. This study is the first to describe changes in the nuclear accumulation of FOXA2 in response to a specific stimulus in pancreatic beta cells. The exact role of FOXA2 in mediating the effects of rosiglitazone on the Ipf1 promoter has yet to be more fully explored.
The effects of metformin on protein levels, nuclear accumulation and the binding activity of IPF1 appear to be time- and glucose-dependent. The effects of stimuli such as glucose and GLP1 on IPF1 binding activity are known to occur through post-translational modification of the protein over relatively short periods [23, 30]. In the final part of the current analyses, we examined the temporal activation of IPF1 binding activity. EMSA analysis indicates that metformin rapidly activates IPF1 DNA binding activity. Consistent with this observation, nuclear accumulation of IPF1 was observed after 2 h. However, time course analysis of nuclear accumulation confirmed that this effect is not prolonged, with nuclear IPF1 returning to basal levels within 24 h. EMSA analysis of nuclear extracts at 24 h confirms that IPF1 binding activity is unaffected by metformin at this later time point (not shown).
It is perhaps surprising that metformin stimulates IPF1 DNA binding activity but has no effect on the activity of the Luc200 construct, containing the proinsulin gene promoter section. However, two key factors may have contributed to these observations: firstly, the promoter experiments were performed over 24 h, by which time nuclear IPF1 levels have dropped and DNA binding activity has decreased. Secondly, it has become increasingly clear that regulation of the proinsulin promoter is controlled through the synergistic activities of a number of beta cell transcription factors [37–39]. Hence, activation of IPF1 alone may not be sufficient to effect proinsulin gene transcription in this case. Further studies would be necessary to clarify this.
The effects of rosiglitazone in the present study are of particular importance since they add to a growing body of evidence suggesting that thiazolidinediones can have a direct positive impact on beta cell function. Along with improved glycaemic control and improvements in insulin resistance, beta cell ‘rejuvenation’ and improvements in beta cell function have been reported in several recent thiazolidinedione trials [40]. In parallel with in vitro data indicating that thiazolidinediones can protect beta cells not only from apoptosis but also from loss of function [41], the role of thiazolidinediones in directly targeting and preserving beta cell function is only now becoming clear [42].
In summary, the present study indicates that both metformin and rosiglitazone have profound effects on transcriptional regulation in pancreatic beta cells, these effects being dependent on both exposure time and glucose concentration. These data are the first to indicate that both metformin and rosiglitazone have direct effects on beta-cell gene expression, and suggest that these widely prescribed antidiabetic drugs may play a previously unrecognised role in the direct regulation of pancreatic beta cell function. Further studies are now required to fully delineate the cell signalling mechanisms regulating these events.
Abbreviations
- AMPK:
-
AMP-dependent protein kinase
- EMSA:
-
electrophoretic mobility shift assay
- FOXA2:
-
forkhead homeobox A2
- GLP-1:
-
glucagon-like peptide-1
- HNF1α:
-
hepatocyte nuclear factor 1α
- IPF1:
-
insulin promoter factor 1
- PPARγ:
-
peroxisome proliferator-activated receptor γ
References
Stumvoll M (2003) Thiazolidinediones—some recent developments. Expert Opin Investig Drugs 12:1179–1187
Furnsinn C, Waldhausl W (2002) Thiazolidinediones: metabolic actions in vitro. Diabetologia 45:1211–1223
Bailey CJ (1992) Biguanides and NIDDM. Diabetes Care 15:755–772
Stumvoll M, Nurjhan N, Perriello G et al (1995) Metabolic effects of metformin in non-insulin-dependent diabetes mellitus. N Engl J Med 333:550–554
Ovalle F, Bell DS (2004) Effect of rosiglitazone versus insulin on the pancreatic beta-cell function of subjects with type 2 diabetes. Diabetes Care 27:2585–2589
Patane G, Piro S, Rabuazzo AM et al (2000) Metformin restores insulin secretion altered by chronic exposure to free fatty acids or high glucose: a direct metformin effect on pancreatic beta-cells. Diabetes 49:735–740
Leclerc I, Woltersdorf WW, da Silva Xavier G et al (2004) Metformin, but not leptin, regulates AMP-activated protein kinase in pancreatic islets: impact on glucose-stimulated insulin secretion. Am J Physiol Endocrinol Metab 286:E1023–E1031
Kefas BA, Cai Y, Kerckhofs K et al (2004) Metformin-induced stimulation of AMP-activated protein kinase in beta-cells impairs their glucose responsiveness and can lead to apoptosis. Biochem Pharmacol 68:409–416
Fryer LG, Parbu-Patel A, Carling D (2002) The anti-diabetic drugs rosiglitazone and metformin stimulate AMP-activated protein kinase through distinct signaling pathways. J Biol Chem 277:25226–25232
Macfarlane WM, Shepherd RM, Cosgrove KE et al (2000) Glucose modulation of insulin mRNA levels is dependent on PDX1, and occurs independently of changes in intracellular Ca2+. Diabetes 49:418–423
Waeber W, Thomson N, Nicod P et al (1996) Transcriptional activation of the GLUT-2 gene by the IPF1/STF1/IDX1 homeobox factor. Mol Endocrinol 10:1327–1334
German MS (1993) Glucose sensing in pancreatic islet β-cells: the key role of glucokinase and the glycolytic intermediates. Proc Natl Acad Sci USA 90:1781–1785
Macfarlane WM, Smith SB, James RFL et al (1997) The p38/reactivating kinase mitogen activated protein kinase cascade mediates the activation of the transcription factor insulin upstream factor 1 and insulin gene transcription by high glucose in pancreatic β-cells. J Biol Chem 272:20936–20944
Guillemain G, da Silva Xavier G, Rafiq I et al (2004) Importin beta1 mediates the glucose-stimulated nuclear import of pancreatic and duodenal homeobox-1 in pancreatic islet beat-cells (MIN6). Biochem J 15:219–227
Kishi A, Nakamura T, Nishio Y et al (2003) Related sumoylation of Pdx1 is associated with its nuclear localization and insulin gene activation. Am J Physiol Endocrinol Metab 284:830–840
Campbell SC, Macfarlane WM (2002) Regulation of the pdx1 gene promoter in pancreatic β-cells. Biochem Biophys Res Commun 299:277–284
Wu K-L, Gannon M, Peshavaria MM et al (1997) Hepatocyte nuclear factor 3β is involved in pancreatic β-cell-specific transcription of the pdx-1 gene. Mol Cell Biol 17:6002–6013
Gerrish K, Gannon M, Shih D et al (2000) Pancreatic β cell-specific transcription of the pdx-1 gene: the role of conserved upstream control regions and their hepatic nuclear factor 3β sites. J Biol Chem 275:3485–3492
Marshak S, Benshushan E, Shoshkes M et al (2000) Functional conservation of regulatory elements in the pdx-1 gene: PDX-1 and hepatocyte nuclear factor 3β transcription factors mediate β-cell-specific expression. Mol Cell Biol 20:7583–7590
Ben-Shushan E, Marshak S, Shoshkes M et al (2001) A pancreatic β-cell-specific enhancer in the human PDX-1 gene is regulated by hepatocyte nuclear factor 3β (HNF-3 β), HNF-1α, and SPs transcription factors. J Biol Chem 276:17533–17540
Miyazaki J, Araki K, Yamato E et al (1990) Establishment of a pancreatic beta cell line that retains glucose-inducible insulin secretion: special reference to expression of glucose transporter isoforms. Endocrinology 127:126–132
Shepherd LA, Campbell SC, Macfarlane WM (2004) Transcriptional regulation of the IAPP gene in pancreatic β-cells. Biochim Biophys Acta 1681:28–37
Macfarlane WM, McKinnon CM, Felton-Edkins ZM et al (1999) Glucose stimulates translocation of the homeodomain transcription factor PDX1 from the cytoplasm to the nucleus in pancreatic β-cells. J Biol Chem 274:1011–1016
Blumentrath J, Neye H, Verspohl EJ (2001) Effects of retinoids and thiazolidinediones on proliferation, insulin release, insulin mRNA, GLUT 2 transporter protein and mRNA of INS-1 cells. Cell Biochem Funct 19:159–169
Bailey CJ, Day C (2004) Avandamet: combined metformin-rosiglitazone treatment for insulin resistance in type 2 diabetes. Int J Clin Pract 58:867–876
Jones TA, Sautter M, Van Gaal LF et al (2003) Addition of rosiglitazone to metformin is most effective in obese, insulin-resistant patients with type 2 diabetes. Diabetes Obes Metab 5:163–170
Lenhard JM, Kliewer SA, Paulik MA et al (1997) Effects of troglitazone and metformin on glucose and lipid metabolism: alterations of two distinct molecular pathways. Biochem Pharmacol 54:801–808
Lupi R, Del Guerra S, Marselli L et al (2004) Rosiglitazone prevents the impairment of human islet function induced by fatty acids: evidence for a role of PPARgamma2 in the modulation of insulin secretion. Am J Physiol Endocrinol Metab 286:E560–E567
Rafiq I, da Silva Xavier G, Hooper S et al (2000) Glucose-stimulated preproinsulin gene expression and nuclear trans-location of pancreatic duodenum homeobox-1 require activation of phosphatidylinositol 3-kinase but not p38 MAPK/SAPK2. J Biol Chem 275:15977–15984
Wang X, Cahill CM, Pineyro MA et al (1999) Glucagon-like peptide-1 regulates the beta cell transcription factor, PDX-1, in insulinoma cells. Endocrinology 140:4904–4970
Kaneto H, Xu G, Fujii N et al (2002) Involvement of c-Jun N-terminal kinase in oxidative stress-mediated suppression of insulin gene expression. J Biol Chem 277:30010–30018
Ishida H, Takizawa M, Ozawa S et al (2004) Pioglitazone improves insulin secretory capacity and prevents the loss of beta-cell mass in obese diabetic db/db mice: possible protection of beta cells from oxidative stress. Metabolism 53:488–494
Masamune A, Satoh K, Sakai Y et al (2002) Ligands of peroxisome proliferator-activated receptor-gamma induce apoptosis in AR42J cells. Pancreas 24:130–138
Brunmair B, Gras F, Neschen S et al (2001) Direct thiazolidinedione action on isolated rat skeletal muscle fuel handling is independent of peroxisome proliferator-activated receptor-gamma-mediated changes in gene expression. Diabetes 50:2309–2315
Iwata M, Haruta T, Usui I et al (2001) Pioglitazone ameliorates tumor necrosis factor-alpha-induced insulin resistance by a mechanism independent of adipogenic activity of peroxisome proliferator-activated receptor-gamma. Diabetes 50:1083–1092
Wolfrum C, Besser D, Luca E et al (2003) Insulin regulates the activity of forkhead transcription factor Hnf-3beta/Foxa-2 by Akt-mediated phosphorylation and nuclear/cytosolic localization. Proc Natl Acad Sci USA 100:11624–11629
Nishimura W, Salameh T, Kondo T et al (2005) Regulation of insulin gene expression by overlapping DNA binding elements. Biochem J 392:181–189
Aramata S, Han SI, Yasuda K et al (2005) Synergistic activation of the insulin gene promoter by the beta-cell enriched transcription factors MafA, Beta2, and Pdx1. Biochim Biophys Acta 1730:41–46
Zhao L, Guo M, Matsuoka TA et al (2005) The islet beta cell-enriched MafA activator is a key regulator of insulin gene transcription. J Biol Chem 280:11887–11894
Bell DS (2003) Beta-cell rejuvenation with thiazolidinediones. Am J Med 115 Suppl 8A:20S–23S
Zeender E, Maedler K, Bosco D et al (2004) Pioglitazone and sodium salicylate protect human beta-cells against apoptosis and impaired function induced by glucose and interleukin-1beta. J Clin Endocrinol Metab 89:5059–5066
Walter H, Lubben G (2005) Potential role of oral thiazolidinedione therapy in preserving beta-cell function in type 2 diabetes mellitus. Drugs 65:1–13
Acknowledgements
H. Richardson was supported by a Biotechnology and Biological Sciences Research Council CASE studentship with GlaxoSmithKline. W. M. Macfarlane was supported by a Career Development Award from the Juvenile Diabetes Research Foundation. S. C. Campbell was supported by Diabetes UK.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Richardson, H., Campbell, S.C., Smith, S.A. et al. Effects of rosiglitazone and metformin on pancreatic beta cell gene expression. Diabetologia 49, 685–696 (2006). https://doi.org/10.1007/s00125-006-0155-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-006-0155-1