Abstract
Aims/hypothesis
The development of an orally active insulin formulation will offer great advantages over conventional injectable insulin therapy in the treatment of patients with diabetes mellitus. Since insulin absorption in the intestine is restricted by the natural physiological characteristics of insulin, we developed a small synthetic compound, N α-deoxycholyl-l-lysyl-methylester (DCK), as an insulin carrier to enhance oral delivery.
Methods
Streptozotocin-induced diabetic rats orally received single doses of insulin (42 U/kg) or insulin/DCK formulation (10, 21, 30 and 42 U/kg) under fasting conditions. Blood glucose levels and plasma insulin concentrations were measured for 6 h following the administration of the agents. An OGTT was also performed immediately after the administration of the oral insulin/DCK formulation.
Results
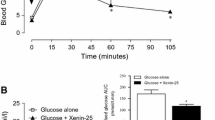
The administration of 21, 30 and 42 U/kg (based on insulin activity) of insulin/DCK formulation reduced plasma glucose levels by up to 33.0% (median; range 30.6–70.2%), 78.5% (39.4–86.8%) and 75.2% (67.0–87.4%), respectively, compared with baseline levels. Furthermore, plasma insulin concentrations were observed to rapidly increase. In the OGTT, the insulin/DCK formulation reduced the AUC0–240 for glucose by 30.8% (22.3–54.9%) (p<0.01), and stabilized glycaemia for up to 4 h.
Conclusions/interpretation
The results of this study demonstrate that the insulin/DCK formulation can be absorbed in the intestine and that it is biologically efficacious. We therefore suggest that this oral formulation could be used as an alternative to injectable insulin with enhanced clinical effects.
Similar content being viewed by others
Introduction
The goal of oral insulin therapy is to mimic the effects of pancreas-secreted insulin in order to control postprandial hyperglycaemia and to prevent hypoglycaemia between meals. Although conventional injectable insulin therapy meets this goal, it is associated with several therapeutic disadvantages, such as hyperinsulinaemia, pain and inconvenience [1–3]. Many attempts have been made to find alternative methods of insulin delivery via non-invasive routes, including peroral, buccal, transdermal, intranasal and pulmonary routes [4–6]. Of the alternative routes available for insulin delivery, peroral administration is the most preferable as it offers significant advantages in terms of therapeutic efficacy and patient acceptability. Since orally delivered insulin undergoes a hepatic pass before entering the circulation, it has the potential to mimic the effects of pancreas-secreted insulin in terms of inhibition of hepatic gluconeogenesis [7–9].
However, the intestinal absorption of many therapeutic proteins, including insulin, is greatly restricted by their specific physicochemical characteristics, such as physical instability, large molecular weight and limited ability to traverse biological barriers [10, 11]. In order to achieve successful oral delivery, enzymatic degradation must be prevented and epithelial permeability must be increased. To this end, permeation enhancers [12, 13], protease inhibitors [14], microspheres [15], nanoparticles [16], polymeric carriers [17] and different modes of chemical modification [18, 19] have been used in attempts to exploit the oral route.
The results of our previous study demonstrated that deoxycholic acid (DOCA)-conjugated heparin is highly absorbed in the intestine and does not damage the tissue structure of the mucous membrane [20, 21]. These findings suggest that the absorption of therapeutic macromolecules in the intestine could be increased in association with bile acids. Based on this, using DOCA and lysine, we developed an oral drug carrier called N α-deoxycholyl-l-lysyl-methylester (DCK) (Fig. 1) that is able to physically associate with therapeutic proteins by ion-pair interactions without altering the structure of native proteins. The aim of this study was to evaluate the efficacy of the new oral insulin formulation (insulin/DCK) in streptozotocin (STZ)-induced diabetic rats.
Materials and methods
Materials
Human zinc insulin (28 U/mg) was obtained from Serologicals (Norcross, GA, USA) and used without further purification. N α-tBOC-Lys-OCH3 was purchased from Bachem (Bubendorf, Switzerland). All other chemicals used in this study were obtained from Sigma-Aldrich (St. Louis, MO, USA) and were of analytic grade.
Synthesis of DCK
Deoxycholic acid (200 mg, 0.5 mmol) and N-hydroxysuccinimide (76 mg, 0.67 mmol) were dissolved in anhydrous terahydrofuran (20 ml). Following the addition of 1,3-dicyclohexylcarbodiimide (136 mg, 0.67 mmol), the solution was stirred at 4°C for 6 h. The urea derivatives produced were filtered, the filtrate was poured into cold n-hexane (120 ml), and then the precipitates were dried under vacuum. Prepared succinimido deoxycholate (230 mg, 0.48 mmol) was then reacted with primary amine group of N α-tBOC-Lys-OCH3 (150 mg, 0.58 mmol) in dimethylformamide (10 ml) containing triethylamine (200 μl, 1.7 mmol) for 12 h at room temperature. After the completion of the reaction, the mixture was diluted with ethylacetate (30 ml) and then successively washed with 10 ml of 0.5 mol/l HCl, distilled water, 0.5 mol/l NaOH and distilled water. The organic phase was dried over magnesium sulphate and evaporated. The protected amine group of lysine was deprotected by mixing in trifluoroacetic acid/dichloromethane (1:1 v/v) for 2 h at room temperature. The reaction volume was minimised by evaporation under reduced pressure, cold diethyl ether was added to induce precipitation, and the mixture was subsequently dried under vacuum. The dried product was dissolved in distilled water and then purified by passing the solution through a Sep-Pak C18 column (Waters, Milford, MA, USA). Finally, purified DCK was lyophilised and obtained as a white powder.
Enzymatic degradation studies
Insulin (100 μl, 17.2 μmol/l) and equivalent amount of insulin/DCK (1:1 w/w) mixture were prepared in HEPES buffer (50 mmol/l, pH 7.4). Following the addition of α-chymotrypsin (10 μl, 1.5 μg), the solutions were incubated at 37°C. At the time points indicated, aliquots of the solutions were acidified by the addition of 890 μl of 0.1% trifluoroacetic acid. Each sample was analysed by reversed-phase HPLC using a Shimadzu HPLC system (Tokyo, Japan) and a C18 Bondapak column (Waters) with a linear gradient of 5–60% solvent B (solvent A: 0.1% trifluoroacetic acid; solvent B: 0.1% trifluoroacetic acid in 95% acetonitrile) over 55 min.
Animals
We followed the National Institutes of Health (NIH) guidelines for the care and use of laboratory animals (NIH Publication No. 85-23, revised 1985). After an initial 3-day acclimation period, male Sprague–Dawley rats (weight 230–250 g) were fasted for 12 h before inducing diabetes mellitus. Diabetes was induced by a single i.p. injection of 60 mg/kg STZ (in a citrate buffer at pH 4.5). Five days after the STZ treatment, rats with fasting blood glucose above 15 mmol/l were selected as diabetic rats for further investigations.
Oral administration of insulin/DCK formulation
The oral insulin/DCK formulation was prepared by making a complex of insulin with DCK. Insulin was dissolved in a small volume of 5 mmol/l HCl and the resultant solution was diluted with PBS (10 mmol/l, pH 7.4) to a final concentration of 42 U/ml. A predetermined dose of DCK in PBS was added to the insulin solution while mixing by vortex.
After being fasted for 12 h, diabetic rats were orally administered either insulin alone or insulin/DCK using a gavage needle. Both groups of rats were randomized based on their average body weights and fasting blood glucose levels. The dose of oral insulin administered ranged from 10 to 42 U/kg. We initially used a fixed amount of insulin (42 U/kg) with increasing amounts of DCK (dose range 0–3 mg/kg). After determination of the optimum ratio of insulin : DCK, we fixed the ratio and evaluated the dose dependency of oral insulin between 10 and 42 U/kg. In order to determine the efficiency of oral insulin compared with parental administration, diabetic rats received an i.v. injection of 1 U/kg of insulin in PBS via the tail vein. All rats were kept in metabolic cages and had free access to water only. Blood samples were collected from the ocular orbital at predetermined time points (0, 30, 60, 120, 180, 240, 300 and 360 min). The blood glucose levels of fresh samples were determined immediately after collection using a one-touch blood glucose monitoring system (Glucocard II; Arkray, Kyoto, Japan). Plasma insulin concentrations were measured using a RIA kit (Insulin Kit; ICN Pharmaceuticals, Orangeburg, NY, USA).
Protocol for the OGTT
Fasted diabetic rats randomly received either placebo or oral insulin. At 0 min, placebo (PBS) and oral insulin (42 U/kg of insulin associated with 1.5 mg/kg of DCK) were orally administered using a gavage needle. At 20 min, 1.5 g/kg of glucose solution in PBS was given orally to each group. Blood samples were collected and blood glucose levels determined at 0, 40, 60, 90, 120, 180 and 240 min as described above.
Data analysis
Basal glycaemia was defined as the blood glucose concentration at time 0 min, measured immediately after injection. The glucodynamic and pharmacokinetic parameters were calculated using the blood glucose or plasma insulin concentrations measured after administration of the agents. The areas under the time curves were calculated using the linear trapezoidal method. Half-life (t 1/2) was estimated as the time (in min) taken for the degradation of 50% of the insulin administered. Standard statistical methods were performed using Sigmaplot statistical software (SPSS, Chicago, IL, USA). Data are expressed as medians and ranges (minimum and maximum values) in the text and tables, and are expressed as medians and interquartile ranges (75th and 25th percentiles) in the figures. The Mann–Whitney non-parametric test was used to assess the degree of statistical significance of differences. A p value less than 0.05 was considered statistically significant.
Results
The cationic deoxycholic acid derivative DCK was synthesised from lysine and deoxycholic acid precursors. DCK is composed of the hydrophobic part of deoxycholic acid and the positive charge of lysine, thereby facilitating ion-pairing interactions with anionic drugs. As a positively charged drug carrier, DCK readily induced microparticulate complexes with insulin by electrostatic interaction in PBS (pH 7.4). The complex formation was reversible and dependent on the molar of DCK : insulin. If allowed to stand, the complexes would invariably form a precipitate; however, they returned to the dispersed state with gentle shaking. This is important for uniform dosing.
On incubation with α-chymotrypsin, native insulin was degraded with a t 1/2 value of 62.3 min (Fig. 2). In contrast, insulin/DCK complexes were resistant to proteolysis, exhibiting a t 1/2 value of 114.4 min, thereby indicating the increased stability of the formulated insulin against proteolysis compared with the native insulin.
Stability of insulin/DCK against enzymatic degradation compared with native insulin. Insulin/DCK (○) formulation and native insulin (●) were incubated with α-chymotrypsin at 37°C. At the indicated time points, aliquots were subjected to analytical HPLC. The quantity of the insulin (peak area) at t=0 was assigned to 100%
Oral administration of insulin alone (42 U/kg), did not appreciably lower the blood glucose levels of the animals. Conversely, the administration of insulin/DCK produced a significant reduction in blood glucose concentrations and an increase in plasma insulin concentrations. When administered alone, DCK did not alter the blood glucose and insulin levels (Fig. 3). Figure 3a shows blood glucose levels following the oral administration of insulin (42 U/kg) in combination with increasing doses of DCK at 0.75, 1.5 and 3 mg/kg. The glucose levels observed following the administration of the 0.75-mg/kg dose were similar to those seen with insulin alone. However, the oral administration of higher concentrations of DCK (1.5 and 3 mg/kg) in combination with insulin significantly reduced glucose levels [75.2% (67.0–87.4%) and 75.0% (36.2–78.3%), respectively, compared with basal glycaemia] and the glucose AUC0–360 [54.0% (27.5–59.9%), p<0.02 and 37.7% (2.8–59.9%), p<0.03, respectively, compared with insulin alone] (Table 1). Glucose levels returned to baseline values at 6 h after administration. Glucose levels were rapidly decreased following insulin/DCK administration, with minimum levels reached 2 h after administration. Figure 3b shows the concentrations of circulating insulin following the oral administration of each formulation. The oral administration of insulin/DCK (1.5 and 3 mg/kg) increased the insulin AUC0–360 by more than 7-fold compared with the equivalent dose of insulin alone. When associated with DCK, insulin produced a statistically significant difference in plasma insulin levels at 30 min.
Effect of a single administration of oral insulin, alone (42 U/kg, ○) and in combination with DCK (0.75 mg/kg, ●; 1.5 mg/kg, □; 3 mg/kg, ▪), on blood glucose (a) and insulin plasma concentration (b) in STZ-induced diabetic rats fasted overnight. DCK was administered alone (3 mg/kg, △) as a control. Results are medians and interquartile ranges (n=4–5). *p<0.05 vs insulin alone
Figure 4 shows the dose–response relationship of orally administered insulin/DCK. At a fixed ratio of insulin/DCK (1:1 w/w), we studied four different doses of insulin (10, 21, 30 and 42 U/kg) in combination with appropriate amounts of DCK (0.37, 0.75, 1 and 1.5 mg/kg, respectively). The higher amounts of orally administered insulin formulation reduced blood glucose levels and increased plasma insulin concentrations in a dose-dependent manner (Table 2). At a dose of 10 U/kg, the administration of insulin alone neither appreciably lowered blood glucose nor increased insulin levels. However, at insulin doses of 21, 30 and 42 U/kg, the insulin/DCK formulation reduced glucose levels [33.0% (30.6–70.2%), 78.5% (39.4–86.8%) and 75.2% (67.0–87.4%), respectively, compared with basal glycaemia) and the glucose AUC0–360 [22.9% (8.6–43.6%), p<0.03; 55.9% (14.2–69.5%), p<0.02; and 54.0% (27.5–59.9%), p<0.02, respectively, compared with insulin alone]. The glucose AUC0–360 values observed at doses of 30 and 42 U/kg were comparable to the value obtained following the i.v. injection of 1 U/kg of insulin. All concentrations of the formulation showed a rapid action within 30 min of administration.
Effect of a single administration of oral insulin/DCK on blood glucose (a) and plasma insulin (b) in STZ-induced diabetic rats fasted overnight. Insulin/DCK was administered at the following doses: 10 U/0.37 mg/kg (○), 21 U/0.75 mg/kg (●), 30 U/1 mg/kg (□) and 42 U/1.5 mg/kg (▪). An i.v. injection of 1 U/kg of insulin in PBS via the tail vein (Δ) served as a control. Results are medians and interquartile ranges (n=4–5). *p<0.05 vs insulin alone
When glucose (1.5 g/kg) was orally administered to the control rats at 20 min after PBS administration (placebo), their blood glucose levels immediately rose above 34 mmol/l and then slowly returned to the baseline (Fig. 5). In contrast, the blood glucose levels of rats treated with the oral insulin/DCK formulation did not increase above the fasting level and were statistically lower than those of the control group at all time points measured. The oral insulin/DCK formulation reduced basal glycaemia by 31.2% (11.9–59.6%) at 60 min and stabilized glycaemia for up to 4 h. The glucose AUC0–240 was also significantly reduced in insulin/DCK-treated rats compared with PBS-treated rats [−30.8% (−22.3 to −54.9%), p<0.01].
Effect of a single administration of oral insulin/DCK (42 U/1.5 mg/kg) in STZ-induced diabetic rats fasted overnight. Insulin/DCK (○) and PBS (●, control) were administered at dose time 0 min. Each group received an oral glucose load of 1.5 g/kg at dose time 20 min. Results are medians and interquartile ranges (n=6). *p<0.05 vs control; **p<0.01 vs control. The insert shows the glucose AUC0–240 for the glycaemic responses of PBS-treated (shaded bar) and oral insulin/DCK-treated (white bar) rats compared with basal glycaemia
Discussion
Bile acids are biological compounds that consist of a facially amphiphilic steroid nucleus with a hydrophobic α-side and a hydrophilic β-side. They are synthesized from cholesterol in the liver, from where they are carried via the bile duct to the small intestine, and return to the liver by absorption through the bile acid transporter [22, 23]. The natural physicochemical properties and enterohepatic circulation of the bile acids suggest that these compounds could be used in the preparation of new drugs and formulations [24–27]. Using bile acid-based molecules, we developed a novel delivery agent that physically interacts with macromolecules to enable their oral absorption. DCK is a positively charged DOCA derivative that readily forms complexes by electrostatic interaction when mixed with insulin in aqueous conditions. We hypothesized that the accessibility of proteases to insulin is reduced when insulin is physically associated with DCK, due to the hydrophobic interactions of DCK. Furthermore, since the chemical structure of DCK is based on the bile acid DOCA, it is recognized by bile acid transporters in intestinal membranes, which may increase the retention time of the peptide in the intestine. Increased lipophilicity, stability and retention time in the gastrointestinal tract are known to be the key factors required for increasing peptide permeability across cell membranes. In this respect, the DCK/insulin formulation was found to be more successful than the conventional enhancers, including bile salts [28, 29].
The results of this study clearly show that an oral formulation of insulin associated with a new carrier, DCK, produced the desired biological effects of insulin in diabetic rats. Consistent dose and time dependencies were observed, with good reproducibility of glucodynamic and pharmacokinetic profiles. The administration of insulin/DCK rapidly decreased plasma glucose to levels significantly lower than those observed following the administration of and equivalent dose of insulin alone. A rapid action is essential for the stabilization of postprandial glycaemia. Insulin absorption usually occurs slowly and erratically following the administration of the injectable insulin against food intake [30]. This mismatch between insulin availability and glucose absorption after a meal might result in a hyperglycaemic or hypoglycaemic condition with potentially serious side effects [1]. Due to its rapid action profile, we propose that our oral insulin/DCK formulation better mimics the first phase insulin release after meals.
The present studies indicated that DCK significantly affected the glucodynamic and pharmacokinetic parameters for orally administered insulin in a fashion that is dependent on the doses of insulin and DCK. When a fixed dose of insulin (42 U/kg) was associated with 1.5 and 3 mg/kg of DCK, similar results were obtained for these parameters (Table 1). This indicates that 42 U/kg of insulin is saturated with 1.5 mg/kg of DCK, and that DCK in its free state may not affect the absorption of insulin in the intestine. Therefore, ratio of insulin/DCK is important for the optimization of the oral formulation. In dose dependency studies, the 30- and 42-U/kg doses of oral insulin produced similar glucose AUC0–360 values (Table 2).
The absolute bioavailability of orally delivered insulin compared with parental insulin was not assessed in the current study. The hepatic extraction of insulin on its first pass through the liver is approximately 50% [8]; thus, the amount of orally delivered insulin is not directly reflected in peripheral blood concentrations [9]. For this reason, the plasma levels of insulin in the peripheral circulation were used as an indicator of insulin absorption, and insulin concentrations in the portal vein were not measured directly. By comparing the glucose AUC following the oral administration of insulin/DCK with that obtained following the i.v. injection of insulin we obtained an indirect estimate of glucose control efficiency of approximately 3%.
An OGTT was performed to investigate whether our formulation could stabilize postprandial glycaemia. Compared with placebo treatment (PBS), a single dose of insulin/DCK administered 20 min prior to an oral glucose load reduced glucose levels and stabilized glycaemia for 4 h. The glucose AUC was also significantly reduced in rats treated with oral insulin compared with control rats. These results provide further evidence that our oral formulation is rapid acting, and support its use clinically in the stabilization of postprandial glycaemia.
Although the mechanism by which DCK enhances insulin absorption is not clear, it may be partly explained by the physicochemical structure of insulin/DCK. DCK possesses the natural characteristics of a bile acid and has the ability to form electrostatic interactions with insulin. When associated with insulin, the amphiphilic steroid nucleus and reactive side groups DCK may increase the lipophilicity and stability of the native hormone. Increased lipophilicity would improve the permeability of the peptide across the mucosal membrane, and increased stability would prolong the therapeutic activity of insulin in the gastrointestinal region. These characteristics are probably responsible for the enhanced oral absorption profiles of insulin when associated with DCK. Further investigations into the physicochemical relationship between insulin and DCK should focus on the mechanism of absorption and long-term toxicity of DCK.
In conclusion, the results of this study demonstrate that a new delivery carrier, DCK, increases the bioavailability and improves the pharmacokinetic effect of insulin when orally delivered. In addition, that the rapid action of our formulation has a stabilizing effect on glycaemia. We anticipate that this formulation may provide an alternative to injectable insulin, resulting in significantly improved patient acceptability and therapeutic effects.
Abbreviations
- DCK:
-
N α-deoxycholyl-l-lysyl-methylester
- DOCA:
-
Deoxycholic acid
- G nadir :
-
Nadir blood glucose concentration
- Insulin C max :
-
Maximum plasma insulin concentration
- STZ:
-
Streptozotocin
- Insulin T max :
-
Time to maximum plasma insulin concentration
- T nadir :
-
Time to nadir blood glucose concentration
References
Skyler JS (1986) Lessons from studies of insulin pharmacokinetics. Diabetes Care 9:666–668
Lauritzen T, Faber OK, Binder C (1979) Variation in 125I-insulin absorption and blood glucose concentration. Diabetologia 17:977–986
Binder C, Lauritzen T, Faber O, Pramming S (1984) Insulin pharmacokinetics. Diabetes Care 7:188–199
Owens DR (2002) New horizons—alternative routes for insulin therapy. Nat Rev Drug Discov 1:529–540
Cefalu WT (2004) Concept, strategies, and feasibility of noninvasive insulin delivery. Diabetes Care 27:239–246
Gordberg M, Gomez-Orellana I (2003) Challenges for the oral delivery of macromolecules. Nat Rev Drug Discov 4:289–295
Lewis GF, Zinman B, Groenewound Y, Vranic M, Giacca A (1996) Hepatic glucose production is regulated both by direct hepatic and extrahepatic effects of insulin in humans. Diabetes 45:454–462
Eaton RP, Allen RC, Schade DS, Standefer JC (1980) ‘Normal’ insulin secretion: the goal of artificial insulin delivery systems? Diabetes Care 3:270–273
Clement S, Still G, Kosutic G, McAllister RG (2002) Oral insulin product hexyl-insulin monoconjugate 2 (HIM2) in type 1 diabetes mellitus: the glucose stabilization effects of HIM2. Diabetes Technol Ther 4:459–466
Shah RB, Ahsan F, Khan MA (2002) Oral delivery of proteins: progress and prognostication. Crit Rev Ther Drug Carr Syst 19:135–169
Sood A, Panchagnula R (2001) Peroral route: an opportunity for protein and peptide drug delivery. Chem Rev 101:3275–3303
Ziv E, Kidron M, Raz I et al (1994) Oral administration of insulin in solid form to nondiabetic and diabetic dogs. J Pharm Sci 83:792–794
Fasano A, Uzzau S (1997) Modulation of intestinal tight junctions by zonula occludens toxin permits enteral administration of insulin and other macromolecules in an animal model. J Clin Invest 99:1158–1164
Carino GP, Mathiowitz E (1999) Oral insulin delivery. Adv Drug Deliv Rev 35:249–257
Mathiowitz E, Jacob JS, Jong YS et al (1997) Biologically erodable microspheres as potential oral drug delivery systems. Nature 386:410–414
Chung H, Kim J, Um JY, Kwon IC, Jeong SY (2002) Self-assembled ‘nanocubicle’ as a carrier for peroral insulin delivery. Diabetologia 45:448–451
Damge C, Michel C, Aprahamian M, Couvreur P (1998) New approach for oral administration of insulin with polyalkylcyanoacrylate nanocapsules as drug carrier. Diabetes 37:246–251
Still JG (2002) Development of oral insulin: progress and current status. Diabetes Metab Res Rev 18:S29–S37
Xia CQ, Wang J, Shen WC (2000) Hypoglycemic effect of insulin–transferrin conjugate in streptozotocin-induced diabetic rats. J Pharmacol Exp Ther 295:594–600
Lee Y, Nam JH, Shin HC, Byun Y (2001) Conjugation of low-molecular-weight heparin and deoxycholic acid for the development of a new oral anticoagulant agent. Circulation 104:3116–3120
Lee Y, Kim SH, Byun Y (2000) Oral delivery of new heparin derivatives in rats. Pharm Res 17:1259–1264
Matern S, Gerok W (1979) Pathophysiology of the enterohepatic circulation of bile acids. Rev Physiol Biochem Pharmacol 85:125–204
Danilson H, Sjovall J (1985) Steroids and bile acids. Elsevier, Amsterdam
Kramer W, Wess G, Neckermann G et al (1994) Intestinal absorption of peptides by coupling to bile acids. J Biol Chem 269:10621–10627
Bowe CL, Mokhtarzadeh L, Venkatesan P et al (1997) Design of compounds that increase the absorption of polar molecules. Proc Natl Acad Sci U S A 94:12218–12223
Zhu XX, Nichifor M (2002) Polymeric materials containing bile acids. Acc Chem Res 35:539–546
Michael S, Thole M, Dillmann R, Fahr A, Drewe J, Fricker G (2000) Improvement of intestinal peptide absorption by a synthetic bile acid derivative, cholylsarcosine. Eur J Pharm Sci 10:133–140
Scott-Moncrieff JC, Shao Z, Mitra AK (1994) Enhancement of intestinal insulin absorption by bile salt-fatty acid mixed micelles in dogs. J Pharm Sci 83:1465–1469
Mesiha MS, Ponnapula S, Plakogiannis F (2002) Oral absorption of insulin encapsulated in artificial chyles of bile salts, palmitic acid and alpha-tocopherol dispersions. Int J Pharm 249:1–5
Mosekilde E, Jensen K, Binder C, Pramming S, Thorsteinsson B (1989) Modeling absorption kinetics of subcutaneous injected soluble insulin. J Pharmacokinet Biopharm 17:67–87
Acknowledgements
This study was supported by the National Research Laboratory (NRL) Project of the Korean Ministry of Science and Technology. The authors affirm that there are no conflicts of interest and no patents pending.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lee, S., Lee, J., Lee, D.Y. et al. A new drug carrier, N α-deoxycholyl-l-lysyl-methylester, for enhancing insulin absorption in the intestine. Diabetologia 48, 405–411 (2005). https://doi.org/10.1007/s00125-004-1658-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-004-1658-2