Abstract
Purpose
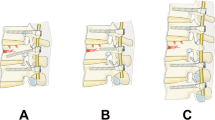
It was aimed to compare the results of long segment posterior instrumentation with intermediate pedicular screw + fusion at the level of the fractured segment including one vertebra above and one below the fractured vertebra (LSPI) and short segment posterior instrumentation with intermediate pedicular screw + fusion at the level of the fractured segment including one vertebra above and one below the fractured vertebra (SSPI) in the surgical treatment of thoracolumbar vertebral fractures.
Methods
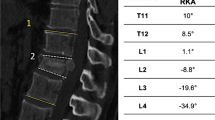
Ninety patients with thoracolumbar vertebral (T11-L2) fractures operated between March 2015 and February 2022 were included in this retrospective study. The patients were divided into two groups as those who underwent LSPI (n, 54; age, 40.3) and those who underwent SSPI (n, 36; age, 39.7). Radiological evaluations like vertebral compression angle (VCA), vertebral corpus heights (VCH), intraoperative parameters, and complications were compared between the groups.
Results
Correction in early postoperative VCA was statistically significantly better in LSPI (p = 0.003). At 1-year follow-up, postoperative VCA correction was significantly more successful in LSPI (p = 0.001). There was no difference between the two groups in terms of correction loss in VCA measured at 1-year follow-up. There was no statistically significant difference between the two groups in terms of postoperative VCH, VCH at 1-year follow-up, and correction loss in VCH.
Conclusion
LSPI provides better postoperative kyphosis correction of the fractured vertebra than SSPI. Regarding the segment level of posterior instrumentation, there was no difference between the two groups in terms of the loss of achieved correction of VCA, ABH, and PBH at 1-year follow-up. Operating a thoracolumbar fracture with LSPI will lengthen the operation and increase the number of intraoperative fluoroscopies compared to SSPI.




Similar content being viewed by others
Data availability
No datasets were generated or analysed during the current study.
References
Gertzbein SD, Scoliosis Research Society. Multicenter spine fracture study. Spine (Phila Pa 1976). 1992;17(5):528–40. https://doi.org/10.1097/00007632-199205000-00010.
Thurman DJ, Burnett CL, Jeppson L, Beaudoin DE, Sniezek JE. Surveillance of spinal cord injuries in Utah, USA. Paraplegia. 1994;32(10):665–9. https://doi.org/10.1038/sc.1994.107.
Hughes H, Carthy AM, Sheridan GA, Donnell JM, Doyle F, Butler J. Thoracolumbar burst fractures: a systematic review and meta-analysis comparing posterior-only instrumentation versus combined anterior-posterior instrumentation. Spine (Phila Pa 1976). 2021;46(15):E840–9. https://doi.org/10.1097/BRS.0000000000003934.
Alvine GF, Swain JM, Asher MA, Burton DC. Treatment of thoracolumbar burst fractures with variable screw placement or Isola instrumentation and arthrodesis: case series and literature review. J Spinal Disord Tech. 2004;17(4):251–64. https://doi.org/10.1097/01.bsd.0000095827.98982.88.
Mittal S, Ifthekar S, Ahuja K, Sarkar B, Singh G, Rana A, et al. Outcomes of thoracolumbar fracture-dislocation managed by short-segment and long-segment posterior fixation: a single-center retrospective study. Int J Spine Surg. 2021;15(1):55–61. https://doi.org/10.14444/8006.
Basaran R, Efendioglu M, Kaksi M, Celik T, Mutlu İ, Ucar M. Finite element analysis of short- versus long-segment posterior fixation for thoracolumbar burst fracture. World Neurosurg. 2019;128:e1109–17. https://doi.org/10.1016/j.wneu.2019.05.077.
Kapoen C, Liu Y, Bloemers FW, Deunk J. Pedicle screw fixation of thoracolumbar fractures: conventional short segment versus short segment with intermediate screws at the fracture level-a systematic review and meta-analysis. Eur Spine J. 2020;29(10):2491–504. https://doi.org/10.1007/s00586-020-06479-4.
Norton RP, Milne EL, Kaimrajh DN, Eismont FJ, Latta LL, Williams SK. Biomechanical analysis of four- versus six-screw constructs for short-segment pedicle screw and rod instrumentation of unstable thoracolumbar fractures. Spine J. 2014;14(8):1734–9. https://doi.org/10.1016/j.spinee.2014.01.035.
Keynan O, Fisher CG, Vaccaro A, Fehlings MG, Oner FC, Dietz J, et al. Radiographic measurement parameters in thoracolumbar fractures: a systematic review and consensus statement of the spine trauma study group. Spine (Phila Pa 1976). 2006;31(5):E156-165. https://doi.org/10.1097/01.brs.0000201261.94907.0d.
Roy-Camille R, Saillant G, Berteaux D, Salgado V. Osteosynthesis of thoraco-lumbar spine fractures with metal plates screwed through the vertebral pedicles. Reconstr Surg Traumatol. 1976;15:2–16.
Roy-Camille R, Saillant G, Mazel C. Internal fixation of the lumbar spine with pedicle screw plating. Clin Orthop Relat Res. 1986;203:7–17.
Kanna RM, Shetty AP, Rajashekhran S. Posterior fixation including the fractured vertebra for severe unstable thoracolumbar fractures. Spine J 15:256–264. https://doi.org/10.1016/j.spinee.2014.09.004.
Jindal R, Jasani V, Sandal D, Garg SK. Current status of short segment fixation in thoracolumbar spine injuries. J Clin Orthop Trauma. 2020;11(5):770–7. https://doi.org/10.1016/j.jcot.2020.06.008.
Lin H, Chang M, Wang S, Liu C, Chou P. The fates of pedicle screws and functional outcomes in a geriatric population following polymethylmethacrylate augmentation fixation for the osteoporotic thoracolumbar and lumbar burst fractures with mean ninety five month follow-up. Int Orthop. 2018;42(6):1313–20. https://doi.org/10.1007/s00264-018-3812-3.
Kim H, Park S, Joy H, Ryu J, Kim S, Ju C. Bone cement augmentation of short segment fixation for unstable burst fracture in severe osteoporosis. J Korean Neurosurg Soc. 2008;44(1):8–14. https://doi.org/10.3340/jkns.2008.44.1.8.
Kasliwal MK, Shaffrey CI, Lenke LG, et al. Frequency, risk factors, and treatment of distal adjacent segment pathology after long thoracolumbar fusion: a systematic review. Spine (Phila Pa 1976). 2012;37(22 Suppl):165–79. https://doi.org/10.1097/BRS.0b013e31826d62c9.
Modi HN, Chung KJ, Seo IW, Yoon HS, Hwang JH, Kim HK, et al. Two levels above and one level below pedicle screw fixation for the treatment of unstable thoracolumbar fracture with partial or intact neurology. J Orthop Surg Res. 2009;4:28. https://doi.org/10.1186/1749-799X-4-28.10.1186/1749-799X-4-28.
Ökten Aİ, Gezercan Y, Özsoy KM, Ateş T, Menekşe G, Aslan A, et al. Results of treatment of unstable thoracolumbar burst fractures using pedicle instrumentation with and without fracture-level screws. Acta Neurochir (Wien). 2015;157(5):831–6. https://doi.org/10.1007/s00701-015-2383-y.
Gurwitz GS, Dawson JM, McNamara MJ, Federspiel CF, Spengler DM. Biomechanical analysis of three surgical approaches for lumbar burst fractures using short-segment instrumentation. Spine (Phila Pa 1976). 1993;18(8):977–82. https://doi.org/10.1097/00007632-199306150-00005.
Kramer DL, Rodgers WB, Mansfield FL. Transpedicular instrumentation and short-segment fusion of thoracolumbar fractures: a prospective study using a single instrumentation system. J Orthop Trauma. 1995;9(6):499–506. https://doi.org/10.1097/00005131-199509060-00007.
Tezeren G, Kuru I. Posterior fixation of thoracolumbar burst fracture: short-segment pedicle fixation versus long-segment instrumentation. J Spinal Disord Tech. 2005;18(6):485–8. https://doi.org/10.1097/01.bsd.0000149874.61397.38.
Aly TA. Short segment versus long segment pedicle screws fixation in management of thoracolumbar burst fractures: meta-analysis. Asian Spine J. 2017;11(1):150–60. https://doi.org/10.4184/asj.2017.11.1.150.
Baaj AA, Reyes PM, Yaqoobi AS, Uribe JS, Vale FL, Theodore N, et al. Biomechanical advantage of the index-level pedicle screw in unstable thoracolumbar junction fractures. J Neurosurg Spine. 2011;14(2):192–7. https://doi.org/10.3171/2010.10.SPINE10222.
Wang H, Li C, Liu T, Zhao WD, Zhou Y. Biomechanical efficacy of monoaxial or polyaxial pedicle screw and additional screw insertion at the level of fracture, in lumbar burst fracture: an experimental study. Indian J Orthop. 2012;46(4):395–401. https://doi.org/10.4103/0019-5413.98827.
Bolesta MJ, Caron T, Chinthakunta SR, Vazifeh PN, Khalil S. Pedicle screw instrumentation of thoracolumbar burst fractures: biomechanical evaluation of screw configuration with pedicle screws at the level of the fracture. Int J Spine Surg. 2012;6:200–5. https://doi.org/10.1016/j.ijsp.2012.09.002.
Mahar A, Kim C, Wedemeyer M, Mitsunaga L, Odell T, Johnson B, et al. Short-segment fixation of lumbar burst fractures using pedicle fixation at the level of the fracture. Spine (Phila Pa 1976). 2007;32(14):1503–7. https://doi.org/10.1097/BRS.0b013e318067dd24.
Dobran M, Nasi D, Brunozzi D, di Somma L, Gladi M, Iacoangeli M, et al. Treatment of unstable thoracolumbar junction fractures: short-segment pedicle fixation with inclusion of the fracture level versus long-segment instrumentation. Acta Neurochir (Wien). 2016;158(10):1883–9. https://doi.org/10.1007/s00701-016-2907-0.
El Behairy HF, Abdelaziz AM, Saleh AK, Elsherief FAH, Abuomira IEA, Elkawary AI, et al. Short-segment fixation of thoracolumbar fractures with ıncorporated screws at the level of fracture. Orthop Surg. 2020;12(1):170–6. https://doi.org/10.1111/os.12590.
Guven O, Kocaoglu B, Bezer M, Aydin N, Nalbantoglu U. The use of screw at the fracture level in the treatment of thoracolumbar burst fractures. J Spinal Disord Tech. 2009;22(6):417–21. https://doi.org/10.1097/BSD.0b013e3181870385.
Wang X, Wu X-D, Zhang Y, Zhu Z, Jiang J, Li G, Liu J, Shao J, Sun Y. The necessity of ımplant removal after fixation of thoracolumbar burst fractures—a systematic review. J Clin Med. 2023;12(6):2213. https://doi.org/10.3390/jcm12062213.
Lee JH, Lee JH, Park JW, Shin YH. The insertional torque of a pedicle screw has a positive correlation with bone mineral density in posterior lumbar pedicle screw fixation. J Bone Joint Surg Br. 2012;94(1):93–7. https://doi.org/10.1302/0301-620X.94B1.27032.
Farrokhi MR, Razmkon A, Maghami Z, Nikoo Z. Inclusion of the fracture level in short segment fixation of thoracolumbar fractures. Eur Spine J. 2010;19(10):1651–6. https://doi.org/10.1007/s00586-010-1449-z.
Altay M, Ozkurt B, Aktekin CN, Ozturk AM, Dogan O, Tabak AY. Treatment of unstable thoracolumbar junction burst fractures with short- or long-segment posterior fixation in magerl type a fractures. Eur Spine J. 2007;16(8):1145–55. https://doi.org/10.1007/s00586-007-0310-5.
Shin SR, Lee SS, Kim JH, et al. Thoracolumbar burst fractures in patients with neurological deficit: anterior approach versus posterior percutaneous fixation with laminotomy. J Clin Neurosci. 2020;75:11–8. https://doi.org/10.1016/j.jocn.2020.03.046.
Sasso RC, Renkens K, Hanson D, Reilly T, McGuire RA Jr, Best NM. Unstable thoracolumbar burst fractures: anterior-only versus short-segment posterior fixation. J Spinal Disord Tech. 2006;19(4):242–8. https://doi.org/10.1097/01.bsd.0000211298.59884.24.
Xu GJ, Li ZJ, Ma JX, Zhang T, Fu X, Ma XL. Anterior versus posterior approach for treatment of thoracolumbar burst fractures: a meta-analysis. Eur Spine J. 2013;22(10):2176–83. https://doi.org/10.1007/s00586-013-2987-y.
Wang J, Liu P. Analysis of surgical approaches for unstable thoracolumbar burst fracture: minimum of five-year follow-up. J Pak Med Assoc. 2015;65(2):201–5.
Hinojosa-Gonzalez DE, Estrada-Mendizabal RJ, Bueno-Gutierrez LC, et al. A network meta-analysis on the surgical management of thoracolumbar burst fractures: anterior, posterior, and combined. Spine Surg Relat Res. 2023;7(3):211–8. https://doi.org/10.22603/ssrr.2022-0196. (Published 2023 Mar 13).
Öztürk AM, Süer O, Aydemir S, Kılıçlı B, Akçalı Ö. The effect of the size of pedicle screw on the long-term radiological and clinical results of short-segment posterior instrumentation in the management of thoracolumbar vertebral fractures. Acta Orthop Traumatol Turc. 2024;58(1):20–6.
Dai LY, Jiang LS, Jiang SD. Posterior short-segment fixation with or without fusion for thoracolumbar burst fractures a five to seven-year prospective randomized study. J Bone Joint Surg Am. 2009;91(5):1033–41.
Wang ST, Ma HL, Liu CL, Yu WK, Chang MC, Chen TH. Is fusion necessary for surgically treated burst fractures of the thoracolumbar and lumbar spine?: a prospective, randomized study. Spine. 2006;31(23):1724–31.
Yang H, Shi JH, Ebraheim M, Liu X, Konrad J, Husain I, Tang TS, Liu J. Outcome of thoracolumbar burst fractures treated with indirect reduction and fixation without fusion. Eur Spine J. 2011;20(3):380–6.
Parker JW, Lane JR, Karaikovic EE, Gaines RW. Successful short-segment instrumentation and fusion for thoracolumbar spine fractures: a consecutive 41/2-year series. Spine. 2000;25(9):1157–70.
Yung AW, Thng PL. Radiological outcome of short segment posterior stabilisation and fusion in thoracolumbar spine acute fracture. Ann Acad Med Singap. 2011;40(3):140–4.
Hwang JH, Modi HN, Yang JH, Kim SJ, Lee SH. Short segment pedicle screw fixation for unstable T11–L2 fractures: with or without fusion? A three-year follow-up study. Acta Orthop Belg. 2009;75(6):822–7.
Lan T, Chen Y, Hu SY, Li AL, Yang XJ. Is fusion superior to non-fusion for the treatment of thoracolumbar burst fracture? A systematic review and meta-analysis. J Orthop Sci. 2017;22(5):828–33. https://doi.org/10.1016/j.jos.2017.05.014.
Zhang W, Li H, Zhou Y, et al. Minimally invasive posterior decompression combined with percutaneous pedicle screw fixation for the treatment of thoracolumbar fractures with neurological deficits: a prospective randomized study versus traditional open posterior surgery. Spine (Phila Pa 1976). 2016;41 Suppl 19:23–9.
Khoo LT, Palmer S, Laich DT, Fessler RG. Minimally invasive percutaneous posterior lumbar interbody fusion. Neurosurgery. 2002;51(5):166–81.
Hong SH, Suh SP, Yeom J, Kim JY, Lee SG, Han JW. Minimally invasive spine surgery versus open posterior instrumentation surgery for unstable thoracolumbar burst fracture. Asian Spine J. 2021;15(6):761–8. https://doi.org/10.31616/asj.2020.0572.
Deckey JE, Bradford DS. Loss of sagittal plane correction after removal of spinal implants. Spine (Phila Pa 1976). 2000;25(19):2453–60.
Alpert HW, Farley FA, Caird MS, Hensinger RN, Li Y, Vanderhave KL. Outcomes following removal of instrumentation after posterior spinal fusion. J Pediatr Orthop Part B. 2014;34(6):613–7.
Kim H-J, Kang K-T, Moon S-H, Chun H-J, et al. The quantitative assessment of risk factors to overstress at adjacent segments after lumbar fusion: removal of posterior ligaments and pedicle screws. Spine (Phila Pa 1976). 2011;36(17):1367–73.
Singh V, Shorez JP, Mali SA, Hallab NJ, Gilbert JL. Material dependent fretting corrosion in spinal fusion devices: evaluation of onset and long-term response. J Biomed Mater Res B Appl Biomater. 2018;106(8):2858–68. https://doi.org/10.1002/jbm.b.34067.
Oh HS, Seo HY. Percutaneous pedicle screw fixation in thoracolumbar fractures: comparison of results according to implant removal time. Clin Orthop Surg. 2019;11(3):291–6.
Charles YP, Walter A, Schuller S, Steib JP. Temporary percutaneous instrumentation and selective anterior fusion for thoracolumbar fractures. Spine (Phila Pa 1976). 2017;42(9):E523–31.
Jug M, Al Mawed S, Brilej D, Dobravec M, Herman S, Kalacun D, KidričSivec U, Kokalj J, Košar J, Movrin I, Tominc U, Vesel M, Komadina R. Recommendations for treatment of thoracolumbar fractures by the Slovenian Spine Society. Zdrav Vestn. 2021;90:336–59. https://doi.org/10.6016/ZdravVestn.3140.
Kweh BTS, Tan T, Lee HQ, Hunn M, Liew S, Tee JW. Implant removal versus implant retention following posterior surgical stabilization of thoracolumbar burst fractures: a systematic review and meta-analysis. Glob Spine J. 2022;12(4):700–18. https://doi.org/10.1177/21925682211005411.
Author information
Authors and Affiliations
Contributions
Concept: O.S., O.A., A.M.O.
Design: O.S., S.A., B.K., A.M.O.
Supervision: O.S., O.A., A.M.O.
Materials: O.S., S.A., B.K., A.M.O.
Data Collection and/or Processing: O.S., S.A., B.K., A.M.O.
Analysis and/or Interpretation: O.S, O.A., A.M.O.
Literature Search: All authors.
Writing: All Authors.
Critical Review: O.S., O.A., A.M.O.
Corresponding author
Ethics declarations
Our study was accepted as an oral presentation at the 31st National Turkish Orthopedics and Traumatology Congress (25–30 October 2022, Antalya, Turkey) and was published in the congress book. This internet address belongs to the congress oral presentation book (https://www.totbid.org.tr/uploads/31.totbid_kongre_program.pdf). This study has not been published in any journal.
IRB approval
This study was approved by Medical Research Ethics Committee of Ege University (23-1T12).
Competing interests
The authors declare no competing interests.
Additional information
Level of clinical evidence: 3
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Suer, O., Aydemir, S., Kilicli, B. et al. Should the level of the posterior instrumentation combined with the intermediate screw be a short segment or a long segment in thoracolumbar fractures with fusion to the fractured segment?. Eur J Trauma Emerg Surg (2024). https://doi.org/10.1007/s00068-024-02518-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00068-024-02518-7