Abstract
Background
Acute superior mesenteric artery (SMA) occlusion is an uncommon condition associated with high mortality. If extensive bowel resection is performed for patients with acute SMA occlusion and the patient survives, long-term total parenteral nutrition (TPN) may be needed due to short bowel syndrome. This study examined factors associated with the need for long-term TPN after the treatment of acute SMA occlusion.
Methods
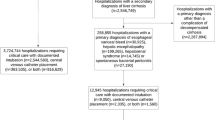
We retrospectively analyzed 78 patients with acute SMA occlusion. Patients were abstracted from a Japanese database from institutions with at least 10 patients with acute SMA occlusive disease from January 2015 through December 2020
Results
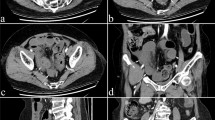
Among the initial cohort there were 41/78 survivors. Of these, 14/41 (34%) required permanent TPN who were compared with those who did not require long-term TPN (27/41, 66%). Compared to patients in the non-TPN group, those in the TPN group had significantly shorter remaining small intestine (90.7 cm vs. 218 cm, P<0.01), more patients with time from onset to intervention >6 hours (P=0.02), pneumatosis intestinalis on enhanced computed tomography scan (P=0.04), ascites (Odds Ratio 11.6, P<0.01), and a positive smaller superior mesenteric vein sign (P= 0.03). These were considered significant risk factors for needing long-term TPN. Age, gender, underlying disease, presence of peritoneal sign, presence of shock requiring vasopressors, site of obstruction (proximal vs. distal), and initial treatment (surgery vs. interventional radiology vs. thrombolytic therapy) were not significantly different between the two groups. Long-term TPN was significantly associated with longer hospital stay (52 vs. 35 days, P=0.04). Multivariate analysis identified the presence of ascites as an independent risk factor for needing long-term TPN.
Conclusion
The need for permanent TPN after treatment of acute SMA occlusion is significantly associated with longer hospital stay, longer time to intervention, and characteristic imaging findings (pneumatosis intestinalis, ascites, Smaller SMV sign). Ascites is an independent risk factor.
Level of evidence
III.
Similar content being viewed by others
References
Bala M, Kashuk J, Moore EE, Kluger Y, Biffl W, Gomes CA, et al. Acute mesenteric ischemia: guidelines of the world society of emergency surgery. World J Emerg Surg. 2017;12:38. https://doi.org/10.1186/s13017-017-0150-5.
Cohran VC, Prozialeck JD, Cole CR. Redefining short bowel syndrome in the 21st century. Pediatr Res. 2017;81(4):540–9. https://doi.org/10.1038/pr.2016.265.
Ekema G, Milianti S, Boroni G. Total parenteral nutrition in patients with short bowel syndrome. Minerva Pediatr 2009;61 (3): 283–91. (https://www.ncbi.nlm.nih.gov/pubmed/19461572).
Kougias P, Lau D, El Sayed HF, Zhou W, Huynh TT, Lin PH. Determinants of mortality and treatment outcome following surgical interventions for acute mesenteric ischemia. J Vasc Surg. 2007;46(3):467–74. https://doi.org/10.1016/j.jvs.2007.04.045.
Nuzzo A, Maggiori L, Ronot M, Becq A, Plessier A, Gault N, et al. Predictive factors of intestinal necrosis in acute mesenteric ischemia: prospective study from an intestinal stroke center. Am J Gastroenterol. 2017;112(4):597–605. https://doi.org/10.1038/ajg.2017.38.
Kirkpatrick ID, Kroeker MA, Greenberg HM. Biphasic CT with mesenteric CT angiography in the evaluation of acute mesenteric ischemia: initial experience. Radiology. 2003;229(1):91–8. https://doi.org/10.1148/radiol.2291020991.
Hagspiel KD, Flors L, Hanley M, Norton PT. Computed tomography angiography and magnetic resonance angiography imaging of the mesenteric vasculature. Tech Vasc Interv Radiol. 2015;18(1):2–13. https://doi.org/10.1053/j.tvir.2014.12.002.
Ginsburg M, Obara P, Lambert DL, Hanley M, Steigner ML, Camacho MA, et al. ACR appropriateness criteria ((R)) imaging of mesenteric ischemia. J Am Coll Radiol. 2018;15(11S):S332–40. https://doi.org/10.1016/j.jacr.2018.09.018.
Wyers MC. Acute mesenteric ischemia: diagnostic approach and surgical treatment. Semin Vasc Surg. 2010;23(1):9–20. https://doi.org/10.1053/j.semvascsurg.2009.12.002.
Beaulieu RJ, Arnaoutakis KD, Abularrage CJ, Efron DT, Schneider E, Black JH 3rd. Comparison of open and endovascular treatment of acute mesenteric ischemia. J Vasc Surg. 2014;59(1):159–64. https://doi.org/10.1016/j.jvs.2013.06.084.
Acosta S. Surgical management of peritonitis secondary to acute superior mesenteric artery occlusion. World J Gastroenterol. 2014;20(29):9936–41. https://doi.org/10.3748/wjg.v20.i29.9936.
Godat L, Kobayashi L, Costantini T, Coimbra R. Abdominal damage control surgery and reconstruction: world society of emergency surgery position paper. World J Emerg Surg. 2013;8(1):53. https://doi.org/10.1186/1749-7922-8-53.
Weber DG, Bendinelli C, Balogh ZJ. Damage control surgery for abdominal emergencies. Br J Surg. 2014;101(1):e109–18. https://doi.org/10.1002/bjs.9360.
Funding
This work was supported by the Japan Society of Abdominal Emergency Medicine [grant numbers 21–2].
Author information
Authors and Affiliations
Contributions
YN was involved in literature search, data collection, study design, data analysis, data interpretation, writing; HS helped in study design, data interpretation, writing critical revision; NS contributed to data interpretation, critical revision; NT, KM, TM, and FK were involved in data collection; ET helped in writing, critical revision, AL contributed to data interpretation, writing, critical revision.
Corresponding author
Ethics declarations
Conflict of interest
We have no conflicts of interest to disclose.
Ethical approval and consent to participate
The institutional review board of the study hospital provided a waiver for retrospective data collection.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nakao, Y., Sasanuma, H., Sata, N. et al. Factors associated with the need for long-term total parenteral nutrition in survivors of acute superior mesenteric artery occlusion. Eur J Trauma Emerg Surg 49, 2025–2030 (2023). https://doi.org/10.1007/s00068-023-02281-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-023-02281-1