Abstract
Purpose
Midlife adults (50–64 y) are at risk for falls and subsequent injury; yet current guidance on fall screening only pertains to older adults (> 65 y). Herein, we evaluated whether frailty was predictive of readmission for falls in midlife trauma patients.
Study design
This was a retrospective cohort study of trauma midlife patients admitted for traumatic injuries from 2010 to 2015. Demographics, injury data, fall history, and post-index readmission for falls were collected from medical records. Frailty scores were calculated retrospectively using the Canadian Study of Health and Aging Clinical Frailty Scale (CSHA-CFS). The association between frailty and outcomes was assessed. p < 0.05 was considered significant.
Results
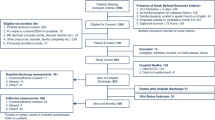
A total of 326 midlife patients were included, 54% were considered fit, 33.7% pre-frail, and 12.3% frail. Compared to their fit and pre-frail counterparts, frail patients were more likely to be female (67.5% vs. 46.3% vs. 36.3%, p < 0.001), have a history of fall (22.5% vs. 15.5% vs. 6.2%, p < 0.001), and to have suffered a ground level fall on index admission (52.5% vs. 20% vs. 5.7%, p < 0.001). Controlling for age, BMI, gender, race, and fall history, frailty was associated with readmission of midlife adults for falls (OR = 1.82 [1.23–2.69]; p = 0.003) and discharge to skilled nursing facilities (OR = 26.86 [8.03–89.81], p < 0.001).
Conclusions
Pre-injury frailty may be an effective tool to predict risk of readmission for fall and discharge disposition in midlife trauma patients.



Similar content being viewed by others
References
Center for Disease Control and Prevention. Web-based injury statistics query and reporting system (WISQARS) www.cdc.gov/ncipc/wisqars2002. www.cdc.gov/ncipc/wisqars. Accessed 15 Jan 2022.
Ylitalo KR, Karvonen-Gutierrez CA. Body mass index, falls, and injurious falls among US adults: findings from the 2014 Behavioral Risk Factor Surveillance System. Prev Med. 2016;91:217–23. https://doi.org/10.1016/j.ypmed.2016.08.044.
Caban-Martinez AJ, Courtney TK, Chang WR, Lombardi DA, Huang YH, Brennan MJ, et al. Leisure-time physical activity, falls, and fall injuries in middle-aged adults. Am J Prev Med. 2015;49(6):888–901. https://doi.org/10.1016/j.amepre.2015.05.022.
Lee R. The CDC’s STEADI initiative: promoting older adult health and independence through fall prevention. Am Fam Physician. 2017;96(4):220–1.
Talbot LA, Musiol RJ, Witham EK, Metter EJ. Falls in young, middle-aged and older community dwelling adults: perceived cause, environmental factors and injury. BMC Public Health. 2005;5:86. https://doi.org/10.1186/1471-2458-5-86.
Nwagwu VC, Cigolle C, Suh T. Reducing frailty to promote healthy aging. Clin Geriatr Med. 2020;36(4):613–30. https://doi.org/10.1016/j.cger.2020.06.005.
Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, et al. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173(5):489–95. https://doi.org/10.1503/cmaj.050051.
Morley JE, Vellas B, van Kan GA, Anker SD, Bauer JM, Bernabei R, et al. Frailty consensus: a call to action. J Am Med Dir Assoc. 2013;14(6):392–7. https://doi.org/10.1016/j.jamda.2013.03.022.
Hoogendijk EO, Afilalo J, Ensrud KE, Kowal P, Onder G, Fried LP. Frailty: implications for clinical practice and public health. Lancet. 2019;394(10206):1365–75. https://doi.org/10.1016/S0140-6736(19)31786-6.
Rockwood K, Abeysundera MJ, Mitnitski A. How should we grade frailty in nursing home patients? J Am Med Dir Assoc. 2007;8(9):595–603. https://doi.org/10.1016/j.jamda.2007.07.012.
Curtis E, Romanowski K, Sen S, Hill A, Cocanour C. Frailty score on admission predicts mortality and discharge disposition in elderly trauma patients over the age of 65 y. J Surg Res. 2018;230:13–9. https://doi.org/10.1016/j.jss.2018.04.017.
Romanowski KS, Curtis E, Palmieri TL, Greenhalgh DG, Sen S. Frailty is associated with mortality in patients aged 50 years and older. J Burn Care Res. 2018;39(5):703–7. https://doi.org/10.1093/jbcr/irx024.
Artiles-Armas M, Roque-Castellano C, Conde-Martel A, Marchena-Gomez J. The comprehensive complication index is related to frailty in elderly surgical patients. J Surg Res. 2019;244:218–24. https://doi.org/10.1016/j.jss.2019.06.011.
Parmar KL, Law J, Carter B, Hewitt J, Boyle JM, Casey P, et al. Frailty in older patients undergoing emergency laparotomy: results from the UK observational emergency laparotomy and frailty (ELF) STUDY. Ann Surg. 2021;273(4):709–18. https://doi.org/10.1097/SLA.0000000000003402.
Cesari M, Calvani R, Marzetti E. Frailty in older persons. Clin Geriatr Med. 2017;33(3):293–303. https://doi.org/10.1016/j.cger.2017.02.002.
Walston J, Buta B, Xue QL. Frailty screening and interventions considerations for clinical practice. Clin Geriatr Med. 2018;34(1):25–38. https://doi.org/10.1016/j.cger.2017.09.004.
Church S, Rogers E, Rockwood K, Theou O. A scoping review of the Clinical Frailty Scale. BMC Geriatr. 2020;20(1):393. https://doi.org/10.1186/s12877-020-01801-7.
Romanowski KS, Barsun A, Pamlieri TL, Greenhalgh DG, Sen S. Frailty score on admission predicts outcomes in elderly burn injury. J Burn Care Res. 2015;36(1):1–6. https://doi.org/10.1097/BCR.0000000000000190.
Bryant EA, Tulebaev S, Castillo-Angeles M, Moberg E, Senglaub SS, O’Mara L, et al. Frailty identification and care pathway: an interdisciplinary approach to care for older trauma patients. J Am Coll Surg. 2019;228(6):852-9 e1. https://doi.org/10.1016/j.jamcollsurg.2019.02.052.
Chua XY, Toh S, Wei K, Teo N, Tang T, Wee SL. Evaluation of clinical frailty screening in geriatric acute care. J Eval Clin Pract. 2020;26(1):35–41. https://doi.org/10.1111/jep.13096.
Tejiram S, Cartwright J, Taylor SL, Hatcher VH, Galet C, Skeete DA, et al. A prospective comparison of frailty scores and fall prediction in acutely injured older adults. J Surg Res. 2021;257:326–32. https://doi.org/10.1016/j.jss.2020.08.007.
Maxwell CA, Patel MB, Suarez-Rodriguez LC, Miller RS. Frailty and prognostication in geriatric surgery and trauma. Clin Geriatr Med. 2019;35(1):13–26. https://doi.org/10.1016/j.cger.2018.08.002.
Hatcher VH, Galet C, Lilienthal M, Skeete DA, Romanowski KS. Association of clinical frailty scores with hospital readmission for falls after index admission for trauma-related injury. JAMA Netw Open. 2019;2(10): e1912409. https://doi.org/10.1001/jamanetworkopen.2019.12409.
Segaux L, Broussier A, Oubaya N, Leissing-Desprez C, Laurent M, Naga H, et al. Several frailty parameters highly prevalent in middle age (50–65) are independent predictors of adverse events. Sci Rep. 2021;11(1):8774. https://doi.org/10.1038/s41598-021-88410-5.
Li X, Ploner A, Karlsson IK, Liu XR, Magnusson PKE, Pedersen NL, et al. The frailty index is a predictor of cause-specific mortality independent of familial effects from midlife onwards: a large cohort study. BMC Med. 2019;17(1):94. https://doi.org/10.1186/s12916-019-1331-8.
Vandenbroucke JP, von Elm E, Altman DG, Gotzsche PC, Mulrow CD, Pocock SJ, et al. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): explanation and elaboration. Epidemiology. 2007;18(6):805–35. https://doi.org/10.1097/EDE.0b013e3181577511.
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP, et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Epidemiology. 2007;18(6):800–4. https://doi.org/10.1097/EDE.0b013e3181577654.
Demidenko E. Sample size determination for logistic regression revisited. Stat Med. 2007;26(18):3385–97. https://doi.org/10.1002/sim.2771.
Phelan EA, Ritchey K. Fall prevention in community-dwelling older adults. Ann Intern Med. 2018;169(11):Itc81–96. https://doi.org/10.7326/Aitc201812040.
Havermans RJM, de Jongh MAC, de Munter L, Lansink KWW. Longitudinal analysis of health status the first year after trauma in severely injured patients. Scand J Trauma Resusc Emerg Med. 2020;28(1):29. https://doi.org/10.1186/s13049-020-00719-8.
Martino C, Russo E, Santonastaso DP, Gamberini E, Bertoni S, Padovani E, et al. Long-term outcomes in major trauma patients and correlations with the acute phase. World J Emerg Surg. 2020;15(1):6. https://doi.org/10.1186/s13017-020-0289-3.
Cheng MH, Chang SF. Frailty as a risk factor for falls among community dwelling people: evidence from a meta-analysis. J Nurs Scholarship. 2017;49(5):529–36. https://doi.org/10.1111/jnu.12322.
Robertson MC, Gillespie LD. Fall prevention in community-dwelling older adults. JAMA. 2013;309(13):1406–7. https://doi.org/10.1001/jama.2013.3130.
Acknowledgements
We thank Michele Lilienthal for her help in retrieving data from our institution’s trauma registry.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Slagel, I.C., Hatcher, V., Romanowski, K.S. et al. Frailty in mid-life predicts outcome following trauma. Eur J Trauma Emerg Surg 49, 1071–1078 (2023). https://doi.org/10.1007/s00068-022-02145-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-022-02145-0