Abstract
Purpose
There is no consensus on the optimal operative technique for humeral shaft fractures. This meta-analysis aims to compare minimal-invasive plate osteosynthesis (MIPO) with nail fixation for humeral shaft fractures regarding healing, complications and functional results.
Methods
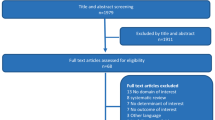
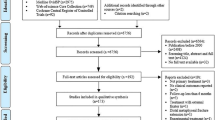
PubMed/Medline/Embase/CENTRAL/CINAHL were searched for randomized clinical trials (RCT) and observational studies comparing MIPO with nailing for humeral shaft fractures. Effect estimates were pooled across studies using random effects models and presented as weighted odds ratio (OR), risk difference (RD), mean difference (MD) and standardized mean difference (SMD) with corresponding 95% confidence interval (95%CI). Analyses were repeated stratified by study design (RCTs and observational studies).
Results
A total of 2 RCTs (87 patients) and 5 observational studies (595 patients) were included. The effects estimated in observational studies and RCTs were similar in direction and magnitude for all outcomes except operation duration. MIPO has a lower risk for non-union (RD 7%; OR 0.2, 95% CI 0.1–0.5) and re-intervention (RD 13%; OR 0.3, 95% CI 0.1–0.8). Functional shoulder (SMD 1.0, 95% CI 0.2–1.8) and elbow scores (SMD 0.4, 95% CI 0–0.8) were better among patients treated with MIPO. The risk for radial nerve palsy following surgery was equal (RD 2%; OR 0.6, 95% CI 0.3–1.2) and nerve function recovered spontaneously in all patients in both groups. No difference was detected with regard to infection, time to union and operation duration.
Conclusion
MIPO has a considerable lower risk for non-union and re-intervention, leads to better shoulder function and, to a lesser extent, better elbow function compared to nailing. Although nailing appears to be a viable option, the evidence suggests that MIPO should be the preferred treatment of choice. The learning curve of minimal-invasive plating should, however, be taken into account when interpreting these results.










Similar content being viewed by others
References
Schoch BS, et al. Humeral shaft fractures: national trends in management. J Orthop Traumatol. 2017;18(3):259–63.
van de Wall BJM, et al. Conservative vs operative treatment for humeral shaft fractures: a meta-analysis and systematic review of randomized clinical trials and observational studies. J Shoulder Elbow Surg. 2020;29:1493–504.
Xue Z, et al. Effects of different surgical techniques on mid-distal humeral shaft vascularity: open reduction and internal fixation versus minimally invasive plate osteosynthesis. BMC Musculoskelet Disord. 2016;17:370.
Wen H, et al. Antegrade intramedullary nail versus plate fixation in the treatment of humeral shaft fractures: an update meta-analysis. Medicine (Baltimore). 2019;98(46):e17952.
Yu BF, et al. Comparison of minimally invasive plate osteosynthesis and conventional plate osteosynthesis for humeral shaft fracture: a meta-analysis. Medicine (Baltimore). 2016;95(39):e4955.
Moher D, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg. 2010;8(5):336–41.
Stroup DF, et al. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283(15):2008–12.
Meinberg EG, et al. Fracture and dislocation classification compendium-2018. J Orthop Trauma. 2018;32(Suppl 1):S1–170.
Slim K, et al. Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg. 2003;73(9):712–6.
Whelan DB, et al. Interobserver and intraobserver variation in the assessment of the healing of tibial fractures after intramedullary fixation. J Bone Jt Surg Br. 2002;84(1):15–8.
Wilson J. Surveillance of surgical site infection in orthopaedic surgery is useful in tackling hospital-acquired infections in England. Euro Surveill. 2005;10(11):E0511173.
Higgins JP, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928.
An Z, et al. Comparison of effectiveness between minimally invasive plating osteosynthesis and expandable intramedullary nailing technique in treatment of middle third humeral shaft fractures. Zhongguo Xiu Fu Chong Jian Wai Ke Za Zhi. 2010;24(12):1413–5.
Kulkarni VS, et al. Comparison between antegrade intramedullary nailing (IMN), open reduction plate osteosynthesis (ORPO) and minimally invasive plate osteosynthesis (MIPO) in treatment of humerus diaphyseal fractures. Injury. 2017;48(Suppl 2):S8–13.
Goncalves FF, et al. Evaluation of the surgical treatment of humeral shaft fractures and comparison between surgical fixation methods. Rev Bras Ortop. 2018;53(2):136–41.
Davies G, et al. Case-match controlled comparison of minimally invasive plate osteosynthesis and intramedullary nailing for the stabilization of humeral shaft fractures. J Orthop Trauma. 2016;30(11):612–7.
Yuan H, et al. Comparison between intramedullary nailing and minimally invasive percutaneous plate osteosynthesis in treatment of humeral shaft fractures. J Coll Physicians Surg Pak. 2019;29(10):942–5.
Lian K, et al. Minimally invasive plating osteosynthesis for mid-distal third humeral shaft fractures. Orthopedics. 2013;36(8):e1025–32.
Benegas E, et al. Shoulder function after surgical treatment of displaced fractures of the humeral shaft: a randomized trial comparing antegrade intramedullary nailing with minimally invasive plate osteosynthesis. J Shoulder Elbow Surg. 2014;23(6):767–74.
Hohmann E, Glatt V, Tetsworth K. Minimally invasive plating versus either open reduction and plate fixation or intramedullary nailing of humeral shaft fractures: a systematic review and meta-analysis of randomized controlled trials. J Shoulder Elbow Surg. 2016;25(10):1634–42.
Zhang Q, et al. Minimally invasive plating osteosynthesis in the treatment of humeral shaft fractures: a meta-analysis. J Invest Surg. 2017;30(2):133–42.
Qiu H, et al. A Bayesian network meta-analysis of three different surgical procedures for the treatment of humeral shaft fractures. Medicine (Baltimore). 2016;95(51):e5464.
Zhao Y, et al. Interventions for humeral shaft fractures: mixed treatment comparisons of clinical trials. Osteoporos Int. 2017;28(11):3229–37.
Farivar SS, Liu H, Hays RD. Half standard deviation estimate of the minimally important difference in HRQOL scores? Expert Rev Pharmacoecon Outcomes Res. 2004;4(5):515–23.
Cheng HR, Lin J. Prospective randomized comparative study of antegrade and retrograde locked nailing for middle humeral shaft fracture. J Trauma. 2008;65(1):94–102.
Lopiz Y, et al. Proximal humerus nailing: a randomized clinical trial between curvilinear and straight nails. J Shoulder Elbow Surg. 2014;23(3):369–76.
Da Silva, T et al. Comparing iatrogenic radial nerve lesions in humeral shaft fractures treated with helical or straight PHILOS plates: a 10-year retrospective cohort study of 62 cases. Arch Orthop Trauma Surg 2020.
Canada-Oya H, et al. New, minimally invasive, anteromedial-distal approach for plate osteosynthesis of distal-third humeral shaft fractures: an anatomical study. JB JS Open Access. 2020;5(1):e0056.
Beeres FJP, et al. Plate fixation of the proximal humerus: an international multicentre comparative study of postoperative complications. Arch Orthop Trauma Surg. 2017;137(12):1685–92.
Beeres, FJP et al. ORIF versus MIPO for humeral shaft fractures: a meta-analysis and systematic review of randomized clinical trials and observational studies. Injury. 2020 6:S0020-1383(20)30939-6.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
van de Wall, B.J.M., Baumgärtner, R., Houwert, R.M. et al. MIPO versus nailing for humeral shaft fractures: a meta-analysis and systematic review of randomised clinical trials and observational studies. Eur J Trauma Emerg Surg 48, 47–59 (2022). https://doi.org/10.1007/s00068-020-01585-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01585-w