Abstract
Introduction
Blood donation from healthy donors is used experimental model that surrogates for class 1 hemorrhage in humans. We examined changes in the perfusion index (PI) and plethysmographic variability index (PVI) in healthy blood donors after donating a unit of blood, and we evaluated the usability of these indices in detecting blood loss volumes of less than 750 mL (class 1 hemorrhagic shock trauma patients).
Materials and methods
This study is a prospective, cross-sectional study. 180 healthy volunteers aged 18 and over, who donated blood at the local blood bank, were included in the study consecutively. The age, gender, and body mass index of the volunteers were recorded and, before and after the blood donation, the vital signs and perfusion indices were measured.
Results
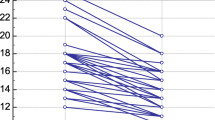
Of the donors, 61.7% were men (n = 111), and the median age of all donors was 32 (IQR: 21–39). A statistically significant difference was found between the hemodynamic parameters and PIs before and after the blood donation (p < 0.01 for all parameters; median difference of PI [− 1.45, 95% CI: (− 0.9)–( − 2)], median difference of PVI [6, 95% CI: 7.77–4.23].
Conclusion
We evaluated the perfusion indices in the early diagnosis of blood volume loss in patients admitted to the emergency department due to trauma. After the participants donated one unit of blood, we found that their PI decreased and PVI increased compared to the measurements before the blood donation. Considering that major bleeding starts in the very early stage as minor bleeding, it is essential for emergency physicians to recognize class 1 hemorrhagic shock patients. Further, non-invasive and straightforward procedures, such as measuring PI and PVI, can be particularly useful in identifying blood loss volumes of less than 750 mL.


Similar content being viewed by others
Availability of data and materials
The dataset generated and/or analyzed during the current study are available from corresponding author.
References
Krug EG, Mercy JA, Dahlberg LL, Zwi AB. World report on violence and health. Biomedica. 2002;22(2):327–36.
Wo CC, Shoemaker WC, Appel PL, Bishop MH, Kram HB, Hardin E. Unreliability of blood pressure and heart rate to evaluate cardiac output in emergency resuscitation and critical illness. Crit Care Med. 1993;21:218–23.
Birkhahn RH, Gaeta TJ, Terry D, Bove JJ, Tloczkowski J. Shock index in diagnosing early acute hypovolemia. Am J Emerg Med. 2005;23:323–6.
Victorino GP, Battistella FD, Wisner DH. Does tachycardia correlate with hypotension after trauma? J Am Coll Surg. 2003;196:679–84.
Akilli B, Bayir A, Kara F, Ak A, Cander B. Inferior vena cava diameter as a marker of early hemorrhagic shock: comparative study. Ulus Travma Acil Cerrahi Derg. 2010;16:113–8.
Gundersen KM, Nyborg C, Heiberg S, Hisdal J. The effects of sympathetic activity induced by ice water on blood flow and brachial artery flow-mediated dilatation response in healthy volunteers. PLoS ONE. 2019;14(9):e0219814.
Silva Lopes B, Craveiro N, Firmino-Machado J, Ribeiro P, Castelo-Branco M. Hemodynamic differences among hypertensive patients with and without heart failure using impedance cardiography. Ther Adv Cardiovasc Dis. 2019. https://doi.org/10.1177/1753944719876517.
Feissel M, Kalakhy R, Banwarth P, Badie J, Pavon A, Faller JP, Quenot JP. Plethysmographic variation index predicts fluid responsiveness in ventilated patients in the early phase of septic shock in the emergency department: a pilot study. J Crit Care. 2013. https://doi.org/10.1016/j.jcrc.2013.03.011.
Brandwein A, Patel K, Kline M, Silver P, Gangadharan S. Using pleth variability as a triage tool for children with obstructive airway disease in a pediatric emergency department. Pediatr Emerg Care. 2016. https://doi.org/10.1097/PEC.0000000000000887.
Zdolsek J, Li Y, Hahn RG. Detection of dehydration by using volume kinetics. Anesth Analg. 2012;115:814–22.
Landesberg G, Shamir M, Avidan A. Early noninvasive detection of hypovolemia in trauma patients-are we there yet? Crit Care Med. 2015;43:907–8.
Tanaka H, Katsuragi S, Tanaka K, Kawamura T, Nii M, Kubo M, Osato K, Sasaki Y, Ikeda T. Application of the perfusion index in obstetric bleeding. J Matern-Fetal Neonatal Med. 2016;29:3812–4.
Schoonjans A, Forget P, Labriola L, Deneys V, Jadoul M, Pingaut I, De Kock M. Pleth variability index combined with passive leg raising-induced pulse pressure variation to detect hypovolemia in spontaneously breathing patients. Acta Anaesthesiol Belg. 2010;61:147–50.
Bonett DG, Price RM. Statistical inference for a linear function of medians: confidence intervals, hypothesis testing and sample size requirements. Psychol Methods. 2002;7(3):370–83.
American College of Surgeons Committee on Trauma. Advanced Trauma Life Support for Doctors (ATLS), student course manual. 10th ed. Chicago: The American College of Surgeons; 2018.
Sauaia A, Moore FA, Moore EE, Moser KS, Brennan R, Read RA, Pons PT. Epidemiology of trauma deaths: a reassessment. J Trauma. 1995;38:185–93.
Rossaint R, Bouillon B, Cerny V, Coats TJ, Duranteau J, Fernández-Mondéjar E, Filipescu D, Hunt BJ, Komadina R, Nardi G, Neugebauer EAM, Ozier Y, Riddez L, Schultz A, Vincent JL, Spahn DR. The European guideline on management of major bleeding and coagulopathy following trauma. Crit Care. 2016;20:100.
Guly HR, Bouamra O, Spiers M, Dark P, Coats T, Lecky FE. Trauma audit and research network: vital signs and estimated blood loss in patients with major trauma: testing the validity of the ATLS classification of hypovolemic shock. Resuscitation. 2011;82:556–9.
Lima A, Bakker J. Noninvasive monitoring of peripheral perfusion. Intensive Care Med. 2005;31:1316–26.
Cannesson M, Delannoy B, Morand A, Rosamel P, Attof Y, Bastien O, Lehot JJ. Does the Pleth variability index indicate the respiratory-induced variation in the plethysmogram and arterial pressure waveforms? Anesth Analg. 2008;106(4):1189–94.
Hoiseth L, Hisdal J, Hoff IE, Hagen OA, Landsverk SA, Kirkeboen KA. Tissue oxygen saturation and finger perfusion index in central hypovolemia: influence of pain. Crit Care Med. 2015;43(4):747–56.
Bartels SA, Bezemer R, De Vries FJ, Milstein DM, Lima A, Cherpanath TG, Van Den Meiracker AH, Van Bommel J, Heger M, Karemaker JM, Ince C. Multi-site and multi-depth near-infrared spectroscopy in a model of simulated (central) hypovolemia: lower body negative pressure. Intensive Care Med. 2011;37:671–7.
Haberthur C, Schachinger H, Seeberger M, Gysi CS. Effect of non-hypotensive haemorrhage on plasma catecholamine levels and cardiovascular variability in man. Clin Physiol Funct Imaging. 2003. https://doi.org/10.1046/j.1475-097x.2003.00490.x.
Triedman JK, Cohen RJ, Saul JP. Mild hypovolemic stress alters autonomic modulation of heart rate. Hypertension. 1993. https://doi.org/10.1161/01.hyp.21.2.236.
Acknowledgements
None
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
Ethical approval for this study was obtained from Kecioren Training and Research Hospital Ethics Committee. The study protocol conforms to the ethical guidelines of the 1975 Declaration of Helsinki.
Informed consent
Written informed consent was obtained from patients.
Rights and permissions
About this article
Cite this article
Öztekin, Ö., Emektar, E., Selvi, H. et al. Perfusion indices can predict early volume depletion in a blood donor model. Eur J Trauma Emerg Surg 48, 553–557 (2022). https://doi.org/10.1007/s00068-020-01463-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01463-5