Abstract
Purpose
To review the management of patients >16 years with blunt splenic injury in a single, UK, major trauma centre and identify whether the following are associated with success or failure of non-operative management with selective use of arterial embolization (NOM ± AE): age, Injury Severity Score (ISS), head injury, haemodynamic instability, massive transfusion, radiological hard signs [contrast extravasation or pseudoaneurysm on the initial computed tomography (CT) scan], grade, and presence of intraparenchymal haematoma or splenic laceration.
Methods
Retrospective, cross-sectional study undertaken between April 2012 and October 2015. Paediatric patients, penetrating splenic trauma, and iatrogenic injuries were excluded. Follow-up was for at least 30 days.
Results
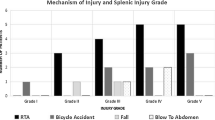
154 patients were included. Median age was 38 years, 77.3% were male, and median ISS was 22. 14/87 (16.1%) patients re-bled following NOM in a median of 2.3 days (IQR 0.8–3.6 days). 8/28 (28.6%) patients re-bled following AE in a median of 2.0 days (IQR 1.3–3.7 days). Grade III–V injuries are a significant predictor of the failure of NOM ± AE (OR 15.6, 95% CI 3.1–78.9, p = 0.001). No grade I injuries and only 3.3% grade II injuries re-bled following NOM ± AE. Age ≥55 years, ISS, radiological hard signs, and haemodynamic instability are not significant predictors of the failure of NOM ± AE, but an intraparenchymal or subcapsular haematoma increases the likelihood of failure 11-fold (OR 10.9, 95% CI 2.2–55.1, p = 0.004).
Conclusions
Higher grade injuries (III–V) and intraparenchymal or subcapsular haematomas are associated with a higher failure rate of NOM ± AE and should be managed more aggressively. Grade I and II injuries can be discharged after 24 h with appropriate advice.

Similar content being viewed by others
References
Costa GI, Tierno SM, Tomassini F, Venturini L, Frezza B, et al. The epidemiology and clinical evaluation of abdominal trauma. An analysis of a multidisciplinary trauma registry. Ann Ital Chir. 2010;81(2):95–102.
Moore EE, Cogbill TH, Malangoni M, Jurkovich GJ, Champion HR. Organ injury scaling: spleen and liver (1994 revision). J Trauma. 1995;38(3):323–4.
Shapiro MJ, Krausz C, Durham RM, Mazuski J, Battistella FD, et al. Overuse of splenic scoring and computed tomographic scans. J Trauma. 1999;47:651–8.
Scarborough JE, Ingraham AM, Liepert AE, Jung HS, O’Rourke AP, et al. Non-operative management is as effective as immediate splenectomy for adult patients with high-grade blunt splenic injury. J Am Coll Surg. 2016;223(2):249–58.
Velmahos GC, Zacharias N, Emhoff TA, Feeney JM, Hurst JM, et al. Management of the most severely injured spleen: a multicenter study of the research consortium of new england centers for trauma (ReCONECT). Arch Surg. 2010;145(5):456–60.
McIntyre LK, Schiff M, Jurkovich GJ. Failure of nonoperative management of splenic injuries: causes and consequences. Arch Surg. 2005;140:563–9.
Requarth JA, D’Agostino RB, Miller PR. Nonoperative management of adult blunt splenic injury with and without splenic artery embolotherapy: a meta-analysis. J Trauma. 2011;71(4):898–903.
Haan JM, Bochicchio GV, Kramer N, Scalea TM. Non-operative management of blunt splenic injury: a 5 year experience. J Trauma. 2005;58:492–8.
Konstantakos AK, Barnoski AL, Plaisier BR, Yowler CJ, Fallon WF Jr, et al. Optimizing the management of blunt splenic injury in adults and children. Surgery. 1999;126:805–12.
Fu CY, Wu SC, Chen RJ, Chen YF, Wang YC, et al. Evaluation of need for operative intervention in blunt splenic injury: intraperitoneal contrast extravasation has an increased probability of requiring operative intervention. World J Surg. 2010;34(11):2745–51.
Zarzaur BL, Kozar R, Myers JG, Claridge JA, Scalea TM, et al. The splenic injury outcomes trial: an american association for the surgery of trauma multi-institutional study. J Trauma Acute Care Surg. 2015;79(3):335–42.
Lopez JM Jr, McGonagill PW, Gross JL, Hoth JJ, Chang MC, et al. Subcapsular hematoma in blunt splenic injury: a significant predictor of failure of nonoperative management. J Trauma Acute Care Surg. 2015;79(6):957–60.
Olthof DC, Joosse P, van der Vlies CH, de Haan RJ, Goslings JC. Prognostic factors for the failure of non-operative management in adults with blunt splenic injury. J Trauma. 2013;74(2):546–57.
Stassen NA, Bhullar I, Cheng JD, Crandall ML, Friese RS, et al. Selective nonoperative management of blunt splenic injury: an eastern association for the surgery of trauma practice management guideline. J Trauma. 2012;73(5):S294–300.
Lecky Fiona. Twenty-five years of the trauma audit and research network: a continuing evolution to drive improvement. Emerg Med J. 2015;32:906–8.
The national confidential enquiry into patient outcome and death (NCEPOD) report. Trauma: who cares? London. 2007. http://www.ncepod.org.uk/2007t.html. Accessed 4 Oct 2016.
The trauma audit and research network (TARN). Press release on major trauma. 2015. https://www.tarn.ac.uk/Content.aspx?c=3477. Accessed 4 Oct 2016.
Yiannoullou P, Hall C, Newton K, Pearce L, Bouamra O, et al. A review of the management of blunt splenic trauma in England and Wales: have regional trauma networks influenced management strategies and outcomes? Ann R Coll Surg Engl. 2017;99:63–9.
Moore FA, Davis JW, Moore EE, Cocanour CS, West MA, et al. Western trauma association (WTA) critical decisions in trauma: management of adult blunt splenic injury. J Trauma. 2008;65:1007–11.
Tugnoli G, Bianchi E, Biscardi A, Coniglio C, Isceri S, et al. Nonoperative management of blunt splenic injury in adults: there is (still) a long way to go. The results of the Bologna-Maggiore hospital trauma center experience and development of a clinical algorithm. Surg Today. 2015;45(10):1210–7.
Bhullar I, Frykberg ER, Tepas JJ III, Siragusa D, Loper T, et al. At first blush: absence of computed tomography contrast extravasation in Grade IV or V adult blunt splenic trauma should not preclude angioembolization. J Trauma Acute Care Surg. 2013;74(1):105–12.
Banerjee A, Duane TM, Wilson SP, Haney S, O’Neill PJ, et al. Trauma center variation in splenic artery embolization and spleen salvage: a multicenter analysis. EAST plenary paper. J Trauma Acute Care Surg. 2013;75(1):69–75.
Sabe AA, Claridge JA, Rosenblum DI, Lie K, Malangoni MA. The effects of splenic artery embolization on nonoperative management of blunt splenic injury: a 16-year experience. J Trauma. 2009;67(3):565–72.
Falimirski ME, Provost D. Nonsurgical management of solid abdominal organ injury in patients over 55 years of age. Am Surg. 2000;66(7):631–5.
Sharma OP, Oswanski MF, Singer D, Raj SS, Daoud YA. Assessment of nonoperative management of blunt spleen and liver trauma. Am Surg. 2005;71(5):379–86.
Alabbasi T, Nathens AB, Tien H. Blunt splenic injury and severe brain injury: a decision analysis and implications for care. J can chir. 2015;58(3):S108–17.
Watson GA, Rosengart MR, Zenati MS, Tsung A, Forsythe RM, et al. Nonoperative management of severe blunt splenic injury: are we getting better? J Trauma. 2006;61(5):1113–8.
Peitzman A, Heil B, Rivera L, Federle MB, Harbrecht BG, et al. Blunt splenic injury in adults: multi-institutional study of the eastern association for the surgery of trauma. J Trauma. 2000;49(2):177–87.
Smith J, Armen S, Cook CH, Martin LC. Blunt splenic injuries: have we watched long enough? J Trauma. 2008;64(3):656–63.
Velmahos GC, Chan LS, Kamel E, Murray JA, Yassa N, et al. Non-operative management of splenic injuries—have we gone too far? Arch Surg. 2000;135:674–9.
Sartorelli KH, Frumiento C, Rogers FB, Osler TM. Nonoperative management of hepatic, splenic, and renal injuries in adults with multiple injuries. J Trauma. 2000;49(1):56–61.
London JA, Parry L, Galante J, Battistella F. Safety of early mobilization of patients with blunt solid organ injuries. Arch Surg. 2008;143(10):972–6.
Duchesne JC, Simmons JD, Schmieg RE Jr, McSwain NE Jr, Bellows CF. Proximal splenic angioembolization does not improve outcomes in treating blunt splenic injuries compared with splenectomy: a cohort analysis. J Trauma. 2008;65(6):1346–51.
Peitzman AB, Harbrecht BG, Rivera L, Heil B. Eastern association for the surgery of trauma multiinstitutional trials workgroup. Failure of observation of blunt splenic injury in adults: variability in practice and adverse consequences. J Am Coll Surg. 2005;201:179–87.
Zarzaur BL, Vashi S, Magnotti LJ, Croce MA, Fabian TC. The real risk of splenectomy after discharge home following nonoperative management of blunt splenic injury. J Trauma. 2009;66(6):1531–6.
Fata P, Robinson L, Fakhry SM. A survey of EAST member practices in blunt splenic injury: a description of current trends and opportunities for improvement. J Trauma. 2005;59(4):836–41.
Alarhayem AQ, Myers JG, Dent D, Lamus D, Lopera J, et al. Blush at first sight: significance of computed tomographic and angiographic discrepancy in patients with blunt abdominal trauma. Am J Surg. 2015;210(6):1104–10.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
For this type of study, formal consent is not required.
Previous presentation of this work
European Society of Trauma and Emergency Surgery Congress, Vienna 2016 oral presentation. Reference 0197: Management of Blunt Splenic Injury: a retrospective review of practice and outcomes at a UK major trauma centre.
Rights and permissions
About this article
Cite this article
Smith, S.R., Morris, L., Spreadborough, S. et al. Management of blunt splenic injury in a UK major trauma centre and predicting the failure of non-operative management: a retrospective, cross-sectional study. Eur J Trauma Emerg Surg 44, 397–406 (2018). https://doi.org/10.1007/s00068-017-0807-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-017-0807-5