Abstract
Purpose
The routine use of thromboprophylaxis during cast immobilisation for lower leg trauma is controversial. The concern involves the perceived increased risk of deep vein thrombosis (DVT) and its sequelae following leg immobilisation. However, immobilisation is used for a spectrum of trauma and for varying duration. This heterogenicity in management is reflected in the current evidence and coupled with the risks of thromboprophylaxis; no clear consensus has been made.
Methods
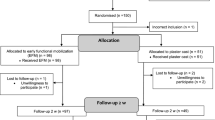
In this retrospective study, we report the incidence of DVT and pulmonary embolism (PE) observed following cast immobilisation and early functional management of patients with Tendo Achilles rupture. Over 12 years, 945 consecutive patients (949 tendons) were treated without additional thromboprophylaxis.
Results
The incidence of DVT was 1.05 % and PE was 0.32 %. Females were significantly more likely to develop a DVT but not a PE. When compared to the incidence of DVT and PE observed in the general population, DVT rate was statistically significantly higher than that observed in the general population. There was no significant difference in PE rates. The number needed to treat to reduce the DVT incidence is 106. The number needed to treat to reduce the PE incidence is 475.
Conclusions
Although we can conclude that conservative treatment for Tendo Achilles does increase the incidence of symptomatic DVT from the general population, we feel that large randomised control trials are required to evaluate the efficacy, compliance and cost effectiveness of routine DVT thromboprophylaxis in the outpatient setting.
Similar content being viewed by others
References
Ho WK, Hankey GJ, Eikelboom JW. The incidence of venous thromboembolism: a prospective, community-based study in Perth, Western Australia. MJA. 2008;189(3):144–7.
The epidemiology of venous thromboembolism: implications for prevention and management. In: Surgeon General’s Workshop on Deep Vein Thrombosis. The office of the surgeon general. US department of health and social sciences.
Venous thromboembolism: reducing the risk of venous thromboembolism (deep vein thrombosis and pulmonary embolism) in patients admitted to hospital. Methods evidence and guidance. National clinical guidance centre acute and chronic conditions 2010. http://www.nice.org.uk.
Reilmann H, Weinberg AM, Forster EE, et al. Prevention of thrombosis in ambulatory patients. Orthopade. 1993;22(2):117–20.
Kujath P, Spannagel U, Habscheid W. Incidence and prophylaxis of deep venous thrombosis in outpatients with injury of the lower limb. Haemostasis. 1993;23(suppl 1):20–6.
Kock HJ, Schmit-Neuerburg KP, Hanke J, et al. Thromboprophylaxis with low-molecular-weight heparin in outpatients with plaster-cast immobilisation of the leg. Lancet. 1995;346(8973):459–61.
Healy B, Beasley R, Weatherall M. Venous thromboembolism following prolonged cast immobilisation for injury to the Tendo Achillis. J Bone Joint Surg Br. 2010;92-B:646–50.
Jameson SS, Augustine A, James P, et al. Venous 116 thromboembolic events following foot and ankle surgery in the English National Health Service. J Bone Joint Surg Br. 2011;93-B:490–7.
Jorgensen PS, Warming T, Hansen K, et al. Low molecular weight heparin (Innohep) as thromboprophylaxis in outpatients with a plaster cast: a venografic controlled study. Thromb Res. 2002;105:477–80.
Lassen MR, Borris LC, Nakov RL. Use of the low-molecular-weight heparin reviparin to prevent deep-vein thrombosis after leg injury requiring immobilization. N Engl J Med. 2002;347:726–30.
Biant LC, Hill G, Singh D. Antithrombotic prophylaxis in foot and ankle surgery in the UK. British Orthopaedic Foot Surgery Society. J Bone Joint Surg Br. 2005;87-B(SUPP_III):375.
Geerts WH, Pineo GF, Heit JA, et al. Prevention of venous thromboembolism: the seventh ACCP conference on antithrombotic and thrombolytic therapy. Chest. 2004;126(3):338S–400S.
Douketis JD, Eikelboom JW, Quinlan DJ, et al. Short duration prophylaxis against venous thromboembolism after total hip or knee replacement: a meta-analysis of prospective studies investigating symptomatic outcomes. Arch Intern Med. 2002;162:1465–71.
Eikelboom JW, Quinlan DJ, Douketis JD. Extended-duration prophylaxis against venous thromboembolism after total hip or knee replacement: a meta-analysis of the randomised trials. Lancet. 2001;358:9–15.
Cohen AT, Bailey CS, Alikhan R, et al. Extended thromboprophylaxis with low molecular weight heparin reduces symptomatic venous thromboembolism following lower limb arthroplasty: 140 a meta-analysis. Thromb Haemost. 2001;85:940–1.
Testroote M, Stigter WAH, de Visser DC, et al. Low molecular weight heparin for prevention of venous thromboembolism in patients with lower-leg immobilization (Review). The Cochrane Collaboration. 2011; The Cochrane Library, issue 3.
Patel A, Ogawa B, Charlton T, et al. Incidence of deep vein thrombosis and pulmonary embolism after achilles tendon rupture. Clin Orthop Relat Res. 2012;470:270–4.
Lapidus LJ, Rosfors S, Ponzer S, et al. Prolonged thromboprophylaxis with Dalteparin after surgical treatment of achilles tendon rupture: a randomized, placebo controlled study. J Orthop Trauma. 2007;21(1):52–7.
Lapidus LJ, Ponzer S, Elvin A, et al. Prolonged thromboprophylaxis with Dalteparin during immobilization after ankle fracture surgery: a randomized, placebocontrolled, double-blind study. Acta Orthop. 2007;78(4):528–35.
Soohoo NF, Krenek L, Eagan MJ, et al. Complication rates following open reduction and internal fixation of ankle fractures. J Bone Joint Surg Am. 2009;91:1042–9.
Wukich DK, Waters DH. Thromboembolism following foot and ankle surgery: a case series and literature review. J Foot Ankle Surg. 2008;47:243–9.
Nordstrom M, Linblad B, Bergqvist D, et al. A prospective study of the incidence of deep-vein thrombosis within a defined urban population. Arch Intern Med. 1992;326:155–60.
Naess IAC. Incidence and mortality of venous thrombosis: a population-based study. J Thromb Haemost. 2007;5:692–9.
Struijk-Mulder MC, Ettema HB, Verheyen CC, et al. Comparing consensus guidelines on thromboprophylaxis in orthopedic surgery. J Thromb Haemost. 2010;8(678–683):2010.
Conflict of interest
Gavin Heyes, Adam Tucker, Richard GH Wallace and Anthony LR Michael declare that they have no conflict of interest.
Compliance with ethics guidelines
Gavin Heyes, Adam Tucker, Richard GH Wallace and Anthony LR Michael confirm that there was no experimental treatment of patients, and that treatment was in accordance with the ethical standards expected by the hospital and in accordance with the Helsinki Declaration of 1975, as revised in 2008. Gavin Heyes, Adam Tucker, Richard GH Wallace and Anthony LR Michael confirm that informed consent was taken from all patients included in the study at time of clinical review. No identifying patient information was used in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Heyes, G.J., Tucker, A., Michael, A.L.R. et al. The incidence of deep vein thrombosis and pulmonary embolism following cast immobilisation and early functional bracing of Tendo Achilles rupture without thromboprophylaxis. Eur J Trauma Emerg Surg 41, 273–276 (2015). https://doi.org/10.1007/s00068-014-0408-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-014-0408-5