Abstract
Background
Distal tibia fractures are known to be difficult to stabilize and nonunions often occur because of a relative instability of the fragments. Therefore, it was of interest to ascertain how different locking plates behave regarding stiffness and interfragmentary movement in comminuted distal tibia fractures.
Methods
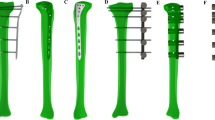
A locked medial plate (AxSOS) for the medial distal tibia and a locked medial plate (LCP) for the distal medial tibia were compared biomechanically under compression and torsional load. The tibiae were osteotomized in distal intersection between 4/5 and 5/5, with a gap of 10 mm after instrumentation. For compression force, a load of 350 N was applied and for torsion, a torque of 0–10 Nm and back to 0 over −5-Nm intervals was performed. Stiffness was calculated from the machine data and interfragmentary movement was measured with an optoelectronic measurement device.
Results
Under compression load, the stiffness showed no significant differences between the AxSOS plate compared to the LCP. Significant differences were seen in the interfragmentary movement, where the LCP showed 1.03 mm compared to 0.6 mm for the AxSOS plate. In torsional testing, the AxSOS plate showed significantly higher stiffness than the LCP. The AxSOS plate and the LCP showed similar values for interfragmentary movement under torsional load.
Conclusion
The treatment of distal tibia fractures with angle-stable medial AxSOS plate showed less interfragmentary movement and higher stiffness than fracture fixation with a locked medial LCP. Even if there are no significant differences in torsional testing, plating of the distal tibia should be performed with a steel plate from the biomechanical view.


Similar content being viewed by others
References
Hazarika S, Chakravarthy J, Cooper J. Minimally invasive locking plate osteosynthesis for fractures of the distal tibia—results in 20 patients. Injury. 2006;37(9):877–87.
Dai JP, Yan YQ, Yu YF, Zhou X. Curative effect comparison of two methods of treatment for distal tibial fractures. Zhongguo Gu Shang. 2009;22(5):361–3.
Bahari S, Lenehan B, Khan H, McElwain JP. Minimally invasive percutaneous plate fixation of distal tibia fractures. Acta Orthop Belg. 2007;73(5):635–40.
Yamaji T, Ando K, Wolf S, Augat P, Claes L. The effect of micromovement on callus formation. J Orthop Sci. 2001;6:571–5.
Augat P, Burger J, Schorlemmer S, Henke T, Peraus M, Claes L. Shear movement at the fracture site delays healing in a diaphyseal fracture model. J Orthop Res. 2003;21:1011–7.
Bhandari M, Guyatt GH, Swiontkowski MF, Schemitsch EH. Treatment of open fractures of the shaft of the tibia. J Bone Joint Surg Br. 2001;83:62–8.
Kuner EH, Berwarth H, Lücke SV. Behandlungsprinzipien bei aseptischen Pseudarthrosen. Orthopäde. 1996;25:394–404.
Cui Y, Wang YJ, Hua QK, Cai SQ, Yan LM, Chen KJ. Biomechanical research in treating unstable Pilon fracture with anatomic plate of distal tibia. Zhongguo Gu Shang. 2009;22(7):519–21.
Lau TW, Leung F, Chan CF, Chow SP. Wound complication of minimally invasive plate osteosynthesis in distal tibia fractures. Int Orthop. 2008;32(5):697–703.
AnyBody Technology. http://www.anybodytech.com.
Morrison JB. The mechanics of the knee joint in relation to normal walking. J Biomech. 1970;3:51–61.
Bergmann G, Deuretzbacher G, Heller M, Graichen F, Rohlmann A, Strauss J, Duda GN. Hip contact forces and gait patterns from routine activities. J Biomech. 2001;34:859–71.
Andriacchi TP, Alexander EJ, Toney MK, Dyrby C, Sum J. A point cluster method for in vivo motion analysis: applied to a study of knee kinematics. J Biomech Eng. 1998;120:743–9.
Mehler D, Hansen M, Rommens PM. Biomechanische Untersuchungen Verschiedener Osteosynthesen an der proximalen Tibia: Vorstellung einer neuartigen meßgeometrischen Anordnung. Biomedizinische Technik. 2003;48:319–24.
Gaebler C, Stanzl-Tschegg S, Laube W, Vécsei V. The fatigue strength of small diameter tibial nails. Injury. 2000;32:401–5.
Hansen M, Mehler D, Hessmann MH, Blum J, Rommens PM. Intramedullary stabilization of extraarticular proximal tibial fractures: a biomechanical comparison of intramedullary and extramedullary implants including a new proximal tibia nail (PTN). J Orthop Trauma. 2007;21:701–9.
Heller MO, Bergmann G, Deuretzbacher G, Dürselen L, Pohl M, Claes L, Haas NP, Duda GN. Musculo-skeletal loading conditions at the hip during walking and stair climbing. J Biomech. 2001;34:883–93.
Jöllenbeck T, Schönle C. Die Teilbelastung nach Knie- oder Hüft-totalendoprothese: Unmöglichkeit der Einhaltung, ihre Ursachen und Abhilfen. Z Orthop Ihre Grenzgeb. 2005;143:124–8.
Hoenig M, Gao F, Kinder J, Zhang LQ, Collinge C, Merk BR. Extra-articular distal tibia fractures: a mechanical evaluation of 4 different treatment methods. J Orthop Trauma. 2010;24(1):30–5.
Augat P, Margevicius K, Simon J, Wolf S, Suger G, Claes L. Local tissue properties in bone healing: influence of size and stability of the osteotomy gap. J Orthop Res. 1998;16:475–81.
Claes L, Augat P, Suger G, Wilke HJ. Influence of size and stability of the osteotomy gap on the success of fracture healing. J Orthop Res. 1997;15:577–84.
Claes LE, Heigele CA, Neidlinger-Wilke C, Kaspar D, Seidl W, Margevicius KJ, Augat P. Effects of mechanical factors on the fracture healing process. Clin Orthop Relat Res. 1998;355:S132–47.
Aro HT, Chao EY. Bone-healing patterns affected by loading, fracture fragment stability, fracture type, and fracture site compression. Clin Orthop Relat Res. 1993;293:8–17.
Goodship AE, Watkins PE, Rigby HS, Kenwright J. The role of fixator frame stiffness in the control of fracture healing. An experimental study. J Biomech. 1993;26:1027–35.
Kenwright J, Goodship AE. Controlled mechanical stimulation in the treatment of tibial fractures. Clin Orthop Relat Res. 1989;241:36–47.
Schildhauer TA, Robie B, Muhr G, Köller M. Bacterial adherence to tantalum versus commonly used orthopedic metallic implant materials. J Orthop Trauma. 2006;20(7):476–84.
Soong M, van Leerdam R, Guitton TG, Got C, Katarincic J, Ring D. Fracture of the distal radius: risk factors for complications after locked volar plate fixation. J Hand Surg Am. 2011;36(1):3–9.
Rozental TD, Blazar PE. Functional outcome and complications after volar plating for dorsally displaced, unstable fractures of the distal radius. J Hand Surg Am. 2006;31(3):359–65.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Högel, F., Hoffmann, S., Weninger, P. et al. Biomechanical comparison of two locking plate systems for the distal tibia. Eur J Trauma Emerg Surg 38, 53–58 (2012). https://doi.org/10.1007/s00068-011-0123-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-011-0123-4